Abstract
Purpose
We aimed to systematically identify and characterize existing digital health tools for pain monitoring in children with cancer, and to assess common barriers and facilitators of implementation.
Methods
A comprehensive literature search (PubMed, Cochrane, Embase, and PsycINFO) was carried out to identify published research on mobile apps and wearable devices focusing on acute and/or chronic pain in children (0–18 years) with cancer (all diagnoses) during active treatment. Tools had to at least include a monitoring feature for one or more pain characteristic(s) (e.g., presence, severity, perceived cause interference with daily life). Project leaders of identified tools were invited for an interview on barriers and facilitators.
Results
Of 121 potential publications, 33 met inclusion criteria, describing 14 tools. Two methods of delivery were used: apps (n=13), and a wearable wristband (n=1). Most publications focused on feasibility and acceptability. Results of interviews with project leaders (100% response rate), reveal that most barriers to implementation were identified in the organizational context (47% of barriers), with financial resources and insufficient time available mentioned most often. Most factors that facilitated implementation related to end users (56% of facilitators), with end-user cooperation and end-user satisfaction mentioned most often.
Conclusions
Existing digital tools for pain in children with cancer were mostly apps directed at pain severity monitoring and little is still known about their effectiveness. Paying attention to common barriers and facilitators, especially taking into account realistic funding expectations and involving end users during early stages of new projects, might prevent evidence based interventions from ending up unused.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Children with cancer experience a wide range of symptoms as a result of their illness and/or treatment [1]. These symptoms include pain, nausea, and fatigue [2]. As survival rates of pediatric cancer improve [3, 4], the focus on supportive care (i.e., the management and prevention of adverse symptoms of the illness and its treatment) has increased [5]. Pain is one of the most common adverse symptoms during childhood cancer treatment with prevalence rates varying between 40 and 78% [2, 6,7,8,9,10,11]. It is also the symptom most feared by children [12]. Cancer-related pain is often caused by the treatment (chemotherapy, surgery, or radiation), by procedures (lumbar punctures, blood draws, or bone marrow aspirations), or by the illness itself (tumor infiltration in tissues or organs) [10, 13].
A previous study on pain in children receiving chemotherapy at the outpatient clinic showed that the majority (78%) experienced clinically significant pain (score ≥ 4), some even more than half of the time (30%) [9]. In one-third (33%) of the clinically significant pain incidences reported in this study, no interventions were used to reduce the pain. This might be due to parental misconceptions (e.g., pain in cancer is inevitable) [10] or concerns regarding analgesic use in children (e.g., pain medication is addictive and works best when used as little as possible) [14]. Despite existing evidence for a variety of effective pain prevention and pain management strategies [15], the management of pain in the home setting is still suboptimal [9]. Digital health provides healthcare organizations with an opportunity to bridge the distance between the hospital and home setting, and to offer support remotely. Digital health includes electronic health (eHealth) and mobile health (mHealth) [16] and has many potential benefits such as accessibility and availability to a wider public (anywhere, anytime), the ability to provide real-time strategies in everyday settings, and to fine-tune interventions to end users’ individual needs [17].
Over the years, the amount of digital health tools for pain management has grown rapidly [18,19,20,21]. The range of features used in existing digital tools for pain seems to vary widely, from more basic tools providing information about pain(management) or using symptom diary tracking, to more advanced tools including real-time feedback from healthcare professionals (HCPs) and game elements (i.e., gamification) such as personalized avatars or in-app rewards to increase user engagement and motivation to symptom reporting [22, 23]. The literature shows growing evidence for the feasibility, acceptability, and effectiveness of digital tools in adult cancer patients and survivors [19, 24]. In the pediatric oncology population, the feasibility and acceptability of some digital tools for cancer-related symptoms, including pain, have been assessed as well [25], yet results on their effectiveness are scarce. One systematic review looked at the effectiveness and efficacy of digital health tools for children and young adults undergoing cancer treatment and survivors [25]. The results of the two identified studies examining the impact on pain were mixed: one study using virtual reality did not demonstrate a significant change in self-reported pain intensity [26], and one study using an app did [27], yet this was a pilot study with preliminary results.
The rapid development and rise of these, often very costly, tools raise the urgency of implementation science [18]. It generally takes approximately 15–20 years to successfully implement a new evidence-based intervention in healthcare settings [28, 29], and only 14% of interventions are successfully adopted in routine care [29], resulting in a large amount of “research waste.” Implementation science uses strategies to adopt and integrate evidence-based health interventions into a clinical setting and describes “the effects of deliberate and purposive actions to implement new treatments, practices, and services” [29]. In order to prevent evidence-based interventions from ending up unused, it is imperative to assess and address determinants that are slowing down (i.e., barriers) and/or facilitating (i.e., facilitators) implementation [30]. In order to make optimal use of this knowledge and focus on areas that need more attention, barriers, and facilitators need to be identified at an early stage. A review on the availability of pain-related eHealth interventions in routine pediatric care found researchers’ intrinsic motivation (i.e., personal beliefs in the importance of making their tools available to end users) to be the most endorsed facilitator, whereas system-level issues (e.g., lack of time and infrastructure to support intervention availability) were common barriers [30]. Including end users in the design phase (user-centered design) was associated with intervention availability in routine care [30]. This is consistent with other reviews on digital tools stressing the importance of involving key stakeholders throughout the entire process to attain buy-in from these parties [25, 31,32,33]. Stakeholders are defined as all people and/or organizations that affect or are affected by the outcomes of a project [34].
In children with cancer, pain has been identified as one of the most common symptoms during all phases of cancer treatment (acute as well as follow-up). Relative to other pediatric diagnoses, their treatment is particularly intense and toxic. Moreover, with new treatment regimens allowing patients to spend more time at home, the responsibility of managing pain lies with families themselves more than ever [35, 36]. Therefore, there is a need to identify digital health tools aimed at the pediatric population specifically, as these might help parents and children cope better. Two systematic reviews (2020) reported on the availability of digital health tools for cancer-related symptoms in pediatric patients [20, 25], yet in both studies, only a limited number (n=2) of tools aimed at pain were identified. As the field of digital health is still rapidly evolving, we expect that an update on the subject will yield more results.
Moreover, this review will focus on mobile applications (“apps”) and wearable devices specifically. The reasoning behind this is that we want to include digital health tools that are always at hand and enable real-time (i.e., prospective) pain assessments, in order to avoid recall bias [37]. Thus, we aim to identify and characterize existing digital health tools (i.e., mobile apps and wearable devices) for pain in children with cancer. For each tool, we aim to provide an overview of research findings (e.g., feasibility, acceptability, effectiveness), and to assess common barriers and facilitators (i.e., lessons learned). By doing so, we hope to gain insight into existing digital tools for pain in pediatric oncology specifically, and secondly to compile valuable lessons for future digital health developers and researchers, not only in pediatric oncology but in a broader range of pediatric healthcare settings.
Methods
Design and reporting
We used Arksey and O’Malley’s methodological framework for scoping reviews to examine the extent, range, and nature of research activity, and to summarize and disseminate our research findings [38]. The framework consists of (step 1) identifying an aim, (step 2) identifying relevant studies (i.e., carry out a literature search), (step 3) selecting studies based on inclusion and exclusion criteria, (step 4) charting the data, and (step 5) collating, summarizing, and reporting the results and is in accordance with the extended PRISMA guideline for Scoping Reviews [39]. No review protocol exists for the current review.
Search strategy and eligibility criteria
A search strategy was created with a medical librarian and carried out on February 9th 2022. Eligible publications were identified through searches of PubMed, Cochrane, Embase, and PsycINFO. The search consisted of four main search terms (ehealth/mhealth, pain, children, and cancer), each consisting of multiple keywords. A detailed overview of the included keywords and search string used for PubMed can be found in Appendix 1. Medical Subject Headings (MeSH), or equivalent terms, were used. No date range was used to limit the search and only English publications were considered. Additional publications were manually searched by scanning reference lists of identified publications.
We included publications (a) concerning mobile apps and wearable devices aimed at pain (b) with (at least) a monitoring feature for one or more pain characteristic(s) (e.g., presence, severity, perceived cause, interference with daily life), (c) for children with a cancer diagnosis (all diagnoses) (d) aged between 0 and 18 years old (or their parents) (e) during active treatment.
The literature management program EndNote was used to remove duplicates, after which the remaining publications were transported into Rayyan [40], which was used to remove the remaining duplicates and to enable multiple authors to screen the publications independently. Two reviewers (JDHPS and ISH) screened the publications independently for eligibility based on abstract and title. Disagreements were resolved by discussion and consensus. A final review of full-text versions of the selected publications was carried out by JDHPS and ISH to determine eligibility.
Semi-structured interviews
The second objective was to assess the determinants of implementation of the identified tools. For this purpose, the corresponding authors of these tools were approached for a semi-structured interview about their tool via a live video communication platform (Zoom). The interviews were audio-recorded after obtaining permission from the interviewees and consisted of three sections: (1) current project phase and parties involved (i.e., professionals who contributed to the project and key stakeholders), (2) use of implementation theory/model/framework, (3) and key barriers and facilitators encountered during the project. Finally, demographic information and working experience of interviewees were collected.
The Measurement Instrument for Determinants of Innovations (MIDI) was used to guide section 3 of the interview (key barriers and facilitators encountered during the project) [41]. The MIDI categorizes barriers and facilitators into 4 main themes and 29 subthemes. The main themes are a tool (e.g., complexity, compatibility), end user (e.g., personal benefits/drawbacks, satisfaction), organization (e.g., formal ratification by management, replacement when staff leave), and socio-political context (e.g., legislation and regulations). We added an additional sub-theme to socio-political context (collaborating with external stakeholders, i.e., other disciplines/hospitals/cultures) since external collaboration barriers/facilitators were not included in the MIDI. An overview of the MIDI (sub)themes was sent to the interviewees prior to the interview and was displayed during the interview when barriers and facilitators were discussed [41]. After a barrier/facilitator was mentioned by an interviewee, the interviewer and interviewee collaboratively categorized it into a corresponding MIDI theme and subtheme. The interview guide, including the overview of MIDI (sub)themes, can be found in Appendix 2.
Data charting and synthesis of results
The data from the publications identified in the literature search was charted by giving an overview of tool characteristics based on published research, namely method of delivery, features, end users, and published research (including outcome measures and main findings) in table form. Published studies were categorized by study design based on what was reported in articles. During interviews, aspects that remained unclear based on published research were verified with the project leaders. Finally, all project leaders were requested to verify the data in the table via email (Table 1).
The outcomes of the interviews on barriers and facilitators were summarized based on audio recordings and represented in table form and visualized in graphs. Each interviewee was requested to verify the data in the table (Appendix 3).
Results
Publication selection process
We identified 122 publications across databases, and 11 additional publications through alternative routes (Fig. 1). After duplicates had been removed, 120 publications were screened based on titles and abstracts, and 33 full-text publications were reviewed. Finally, 32 publications were included. In total, 14 tools for pain in pediatric oncology were identified.
Results scoping review
An overview of included studies and characteristics of the digital tools can be found in Table 1.
Method of delivery
Two methods of delivery were used: apps (n=13, 92.9%), and a wearable wristband (n=1, 7.1%).
Features
Tool features were grouped into four main themes: (1) monitoring feature for one or more pain characteristic(s) (e.g., presence, severity, perceived cause, interference with daily life, bothersomeness), (2) information about pain(management), (3) communication, and (4) game elements. In 13/14 tools, the pain characteristic “severity” was monitored (n=14, 92.9%), of which 12 tools used self and/or parent reports with several rating scales (details in Table 1), and one wearable tool used heart rate, skin temperature, and electrodermal activity to monitor pain [42]. One tool just assessed the pain characteristic “bothersomeness” (mouth sores, headache, hurt of pain other than headache) [43]. Information about pain(management) was provided in six tools (42.9%), and nine tools (64.3%) included a communication feature, of which n=3 provided real-time feedback from healthcare professionals, n=2 provided real-time algorithm-informed feedback, n=3 included a web-interface for healthcare professionals to evaluate and give feedback on data, n=1 included a community forum for peers, and n=1 provided pain reports for healthcare professionals during clinic appointments. One tool had two communication features and thus was counted twice [43]. Gamification elements were used in four tools (24.6%) and included users picking their own avatar (n=2), playing the role of a superhero or law-enforcer (n=2), having a sketch pad available (n=1), and reward systems for adherence to pain diary completion (n=2).
End users
All tools were developed for children during cancer treatment, yet one was also available during follow-up after treatment, and one was available for children with sickle cell disease as well. Age groups of children varied, with one tool (7.1%) solely focusing on young children (ages 0–12), three tools (21.4%) on adolescents and young adults (AYAs) (ages 13–32), and ten tools (71.4%) on both young children and AYAs. With regard to setting, one tool (7.1%) could be used solely in the hospital (i.e., inpatients), five tools were meant for an outpatient setting (i.e., not during hospitalization) (35.7%), and eight tools were available for in- as well as outpatients (57.1%).
Included studies
The research was published between 2012 and 2022. An overview can be found in Fig. 2. The majority of studies focused on the development and usability/feasibility/acceptability testing. For two tools (Pain Squad+ and Pain Buddy [44, 45]), preliminary data on their effectiveness in reducing pain has been published, yet no definitive results are available. For another tool (C-SCAT [46]), an effectiveness study was published. However, this study focused on the tool’s effectiveness in increasing AYA self-efficacy for symptom management, rather than pain reduction.
Results semi-structured interviews
Thirteen project leaders were invited for a semi-structured interview on barriers and facilitators to (future) implementation of their tools (100% response rate). Table 2 describes the interviewee characteristics. For the RESPONSE app [43], no interview was conducted as this tool was added during the review process.
With regard to professional input, 60.3% of the professionals were healthcare professionals (e.g., physicians,nurses,physiotherapists, psychologists, pain experts, child life specialists), 27.9% were digital technique specialists (e.g., computer scientists, engineers, software developers, applied IT specialists), and 11.8% were other professionals (e.g., lawyers, patient organization members, communication experts, measurements experts, health economists).
With regard to key stakeholders, 41.4% of all mentioned stakeholders were families (e.g., patients, parents, and extended families), 37.9% were healthcare professionals (includes the hospital as an organization), 10.3% were cancer aid organizations, 6.9% were research funders, and 3.4% were IT companies.
Five interviewees (38.5%) reported having used or using a theoretical model for implementation, namely the Consolidated Framework for Implementation Research (CFIR) (n=2), the Knowledge-to-Action (KTA) Framework (n=1), the Reach, Effectiveness, Adoption, Implementation, and Maintenance (RE-AIM) Framework (n=1), and the MRC (Medical Research Council) Framework for Development and Evaluation of Complex Tools (n=1).
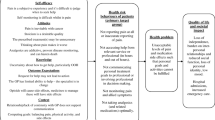
The key barriers and facilitators can be found in Fig. 3. Most barriers related to the organization (i.e., financial resources: “During effectiveness testing, a nurse is paid from research funding. But how will we fund this down the road, when we want to implement/scale up?”) and the socio-political context (i.e., legislation/regulations: “When you work with different hospitals and institutions they may have different juridical regulations”). Most facilitators related to the end users (i.e., client/patient cooperation: “Children are more likely to accept new technology and to incorporate new technology into their house”) and the tool itself (i.e., complexity: “It was really easy and clear how to use the app”).
Discussion
This review identified fourteen unique digital tools for pain monitoring, with the ultimate goal of improving pain management and reducing pain in children and/or AYAs with cancer. Identified tools in this study were mostly mobile apps that can be used in both in- and outpatient settings, by young children as well as AYAs, and were directed at pain severity monitoring using self- and/or proxy reporting rating scales. The feasibility and/or acceptability of all but one tool (RESPONSE [43]) has been established, yet very little is still known about their effectiveness in accurately monitoring and/or reducing pain [47]. Moreover, little is also known about their (future) chances of successful implementation in care. During the interviews, project leaders mostly mentioned organizational barriers and end-user facilitators in the process of implementation.
In addition to pain severity monitoring, another commonly used feature was “communication.” Seven tools included a communication feature with healthcare professionals (50% of all tools), and one tool included a community forum for communication with peers (7.1%). Communication options with healthcare professionals ranged from real-time feedback on reported pain scores, to feedback on pain scores during clinic visits (i.e., delayed feedback). A previous review on the benefits of mobile apps for cancer pain management in (mostly) adults revealed evidence for improved quality of life and decreased pain catastrophizing for digital tools with a real-time communication functionality between patients and healthcare professionals [19]. This shows promise for the future effectiveness of tools which included real-time feedback from healthcare professionals.
Most included publications focused on the development and user experiences. The biggest knowledge gap lies in these tools’ effectiveness in successfully monitoring and/or reducing pain. One effectiveness study found a significant effect on self-efficacy for symptom management in AYAs, yet no results on symptom (i.e., pain) reduction were included [46]. Two preliminary effectiveness studies on pain reduction were published and found a significant effect on pain severity (decreased) [27, 48], pain interference (decreased), and Health-Related Quality of Life (HRQOL) (increased) [27]. The tools described in these two studies (Pain Buddy and Pain Squad+) both included real-time feedback (from healthcare professionals or algorithm informed based on healthcare professionals’ input) and game elements. Game elements and in-app incentives have previously been found to increase medication adherence [49] and thus might also be useful to improve symptom reporting adherence of digital tools. However, since both studies were preliminary with small sample sizes (N=40/48), no definitive recommendations can be made.
A strength of this scoping review lies in the added value of the semi-structured interviews aimed at identifying key barriers and facilitators. This mixed-method design informs readers on the state of the field based on published literature but also incorporates project leaders’ experiences that may form valuable lessons for future researchers. The high response rate (100%) for interview participation in this study reflects the project leaders’ willingness to share experiences with colleagues to contribute to implementation awareness. Digital tools have the potential of being more cost-effective than regular face-to-face care [50], that is, when successfully implemented in care. A key pillar of implementation science lies in the involvement of stakeholders, and user-centered designs have previously been associated with successful implementation in care [30]. In this review, only five out of 12 interviewees reported using a theoretical model for implementation. However, all interviewees did report getting input from a diverse group of professionals (i.e., healthcare professionals, specialists in digital technique, lawyers, patient organizations) and stakeholders (i.e., families, healthcare professionals, cancer aid organizations, research funders, IT companies) throughout their projects. Healthcare professionals were by far the most involved professionals, and they were also the second most commonly mentioned key stakeholders, after families. Thus, despite the sparse use of formal theoretical models for implementation, end users’ input was highly valued as they were involved in the majority of projects. Based on the literature, this increases the chance of successful future implementation of these tools in care. The close involvement of project leaders globally in this review might lead to more international collaborations, larger sample sizes, and higher cost-effectiveness in the future. At the same time, international collaborations might cause barriers in the socio-political spectrum of the MIDI [41], such as legislation and regulations and collaborating with external stakeholders (i.e., other disciplines/hospitals/cultures).
The importance of including end users is also reflected in the results of the interviews with project leaders on barriers and facilitators. The most common facilitators were often connected to end users (56% of all mentioned facilitators), with end-user cooperation and end-user satisfaction mentioned most often. This is in line with several reviews stressing the importance of user-centered designs to accomplish successful use in routine care [25, 31,32,33]. In contrast to previous findings in which researchers’ intrinsic motivation (personal beliefs in the importance of making their tools available to end users) was mentioned as an important facilitator [30], this was not found in the current study. The most common barriers were identified in the organizational context (47% of all mentioned barriers), with financial resources and time available being the most common. This is in line with a previous review on digital health tools for pediatric pain (not cancer-specific) in which lack of time and infrastructure to support tool availability were identified as barriers as well [30]. The overarching aim of assessing barriers and facilitators is to identify and understand factors that influence implementation [51]. However, solely assessment of barriers and facilitators does not suffice. It is also important to act on this knowledge and focus on areas that need more attention. For this purpose, Nilsen et al. have described several models which guide the process of translating research into practice and provide more practical planning and execution of implementation endeavors [51]. Future digital health researchers should incorporate such models in their projects in order to increase implementation success.
A limitation of this study lies in the fact that the RESPONSE tool [43] did not come up in our initial literature search and was brought to our attention during the review process. As a result, we were unable to carry out the interview about barriers and facilitators. We did include this tool in Table 1 (overview tool characteristics based on published research).
This review provides an update on digital tools for acute and/or chronic pain in children with cancer that have been developed in research settings. Thirteen unique digital tools were identified, and these are mostly apps directed at pain severity monitoring. Feasibility and acceptability were established for all tools, yet definitive data on their effectiveness in accurately monitoring and/or reducing pain is lacking. Qualitative assessment of common determinants (barriers and facilitators) of successful implementation yielded valuable findings that can inform and guide future digital health researchers and implementers, not only in pediatric oncology, but also in a wide variety of both pediatric and adult healthcare populations.
References
Ramsey WA, Heidelberg RE, Gilbert AM, Heneghan MB, Badawy SM, Alberts NM (2020) Health and mHealth interventions in pediatric cancer: a systematic review of interventions across the cancer continuum. Psycho-oncology 29(1):17–37
Miller E, Jacob E, Hockenberry MJ (2011) Nausea, pain, fatigue, and multiple symptoms in hospitalized children with cancer. Oncol Nurs Forum 38(5):E382–E393
Schulpen M et al (2021) Significant improvement in survival of advanced stage childhood and young adolescent cancer in the Netherlands since the 1990s. Eur. J. Cancer 157:81–93. https://doi.org/10.1016/j.ejca.2021.08.001
Smith MA, Altekruse SF, Adamson PC, Reaman GH, Seibel NL (2014) Declining childhood and adolescent cancer mortality. Cancer 120(16):2497–2506. https://doi.org/10.1002/cncr.28748
M. A. o. S. C. i. C. (MASCC). "Strategic plan, consensus on the core ideology of MASCC." http://www.mascc.org/index.php?option=com_ content&view=article&id=493:mascc-strategic-plan&catid=30: navigation. (Accessed 21 April 2022).
Alberts NM, Gagnon MM, Stinson JN (2018) Chronic pain in survivors of childhood cancer: a developmental model of pain across the cancer trajectory. Pain 159(10):1916–1927
Fortier MA, Wahi A, Bruce C, Maurer EL, Stevenson R (2014) Pain management at home in children with cancer: a daily diary study. Pediatr. Blood Cancer 61(6):1029–1033. https://doi.org/10.1002/pbc.24907
Bult MK et al (2019) Health-Related quality of life of adolescents with cancer during the first year of treatment. J Adolesc Young Adult Oncol 8(5):616–622. https://doi.org/10.1089/jayao.2019.0017
Simon JDHP et al (2020) Pain at home during childhood cancer treatment: severity, prevalence, analgesic use, and interference with daily life. Pediatr. Blood Cancer 67(12):e28699. https://doi.org/10.1002/pbc.28699
Ljungman G, Gordh T, Sorensen S, Kreuger A (2000) Pain variations during cancer treatment in children: a descriptive survey. Pediatr. Hematol. Oncol 17(3):211–221. https://doi.org/10.1080/088800100276389
Tutelman PR et al (2018) Pain in children with cancer: prevalence, characteristics, and parent management. Clin. J. Pain 34(3):198–206. https://doi.org/10.1097/ajp.0000000000000531
Enskar K, Carlsson M, Golsater M, Hamrin E, Kreuger A (1997) Life situation and problems as reported by children with cancer and their parents. J. Pediatr. Oncol. Nurs 14(1):18–26. https://doi.org/10.1177/104345429701400104
Ljungman G, Gordh T, Sorensen S, Kreuger A (1999) Pain in paedeatric oncology: interviews with children, adolescents and their parents. Acta Paediatr 88(6):623–630. https://doi.org/10.1080/08035259950169279
Fortier MA, Maurer EL, Tan ET, Senders LS, Kain ZN (2012) Attitudes regarding analgesic use and pain expression in parents of children with cancer. J. Pediatr. Hematol. Oncol 34(4):257–262. https://doi.org/10.1097/MPH.0b013e318241fd07
Loeffen E et al (2020) Reducing pain and distress related to needle procedures in children with cancer: a clinical practice guideline. Eur. J. Cancer 131:53–67. https://doi.org/10.1016/j.ejca.2020.02.039
Hallberg D, Salimi N (2020) Qualitative and quantitative analysis of definitions of e-Health and m-Health. Healthc Inform Res 26(2):119–128. https://doi.org/10.4258/hir.2020.26.2.119
Kaplan RM, Stone AA (2013) Bringing the laboratory and clinic to the community: mobile technologies for health promotion and disease prevention. Annu. Rev. Psychol 64:471–498. https://doi.org/10.1146/annurev-psych-113011-143736
Higgins KS et al (2018) Availability of researcher-led eHealth tools for pain assessment and management: barriers, facilitators, costs, and design. PAIN Reports 3(7):e686. https://doi.org/10.1097/pr9.0000000000000686
Zheng C et al (2020) Benefits of mobile apps for cancer pain management: systematic review. JMIR Mhealth Uhealth 8(1):e17055. https://doi.org/10.2196/17055
Lopez-Rodriguez MM, Fernández-Millan A, Ruiz-Fernández MD, Dobarrio-Sanz I, Fernández-Medina IM (2020) New technologies to improve pain, anxiety and depression in children and adolescents with cancer: a systematic review. Int. J. Environ. Res. Public Health 17(10):3563. https://doi.org/10.3390/ijerph17103563
Rosser BA, Eccleston C (2011) Smartphone applications for pain management. J. Telemed. Telecare 17(6):308–312. https://doi.org/10.1258/jtt.2011.101102
Cugelman B (2013) Gamification: what it is and why it matters to digital health behavior change developers. JMIR Serious Games 1(1):e3. https://doi.org/10.2196/games.3139
Hoffmann A, Faust-Christmann CA, Zolynski G, Bleser G (2020) Toward gamified pain management apps: mobile application rating scale-based quality assessment of pain-mentor's first prototype through an expert study. JMIR Form Res 4(5):e13170. https://doi.org/10.2196/13170
Hernandez Silva E, Lawler S, Langbecker D (2019) The effectiveness of mHealth for self-management in improving pain, psychological distress, fatigue, and sleep in cancer survivors: a systematic review. J. Cancer Surviv 13(1):97–107. https://doi.org/10.1007/s11764-018-0730-8
Ramsey WA, Heidelberg RE, Gilbert AM, Heneghan MB, Badawy SM, Alberts NM (2020) eHealth and mHealth interventions in pediatric cancer: a systematic review of interventions across the cancer continuum. Psychooncology 29(1):17–37. https://doi.org/10.1002/pon.5280
Gershon J, Zimand E, Pickering M, Rothbaum BO, Hodges L (2004) A pilot and feasibility study of virtual reality as a distraction for children with cancer. J. Am. Acad. Child Adolesc. Psychiatry 43(10):1243–1249. https://doi.org/10.1097/01.chi.0000135621.23145.05
Jibb LA et al (2017) Implementation and preliminary effectiveness of a real-time pain management smartphone app for adolescents with cancer: a multicenter pilot clinical study. Pediatr. Blood Cancer 64(10):e26554. https://doi.org/10.1002/pbc.26554
Proctor EK, Landsverk J, Aarons G, Chambers D, Glisson C, Mittman B (2009) Implementation Research in mental health services: an emerging science with conceptual, methodological, and training challenges. Adm Policy Ment Health 36(1):24–34. https://doi.org/10.1007/s10488-008-0197-4
Balas EA, Boren SA (2000) Managing clinical knowledge for health care improvement. Yearb. Med. Inform 09(01):65–70. https://doi.org/10.1055/s-0038-1637943
Higgins KS et al (2018) Availability of researcher-led eHealth tools for pain assessment and management: barriers, facilitators, costs, and design. Pain Rep 3(Suppl 1):e686. https://doi.org/10.1097/PR9.0000000000000686
Cheng L, Duan M, Mao X, Ge Y, Wang Y, Huang H (2021) The effect of digital health technologies on managing symptoms across pediatric cancer continuum: a systematic review. Int J Nurs Sci 8(1):22–29
McGuire BE, Henderson EM, McGrath PJ (2017) Translating e-pain research into patient care. Pain 158(2):190–193. https://doi.org/10.1097/j.pain.0000000000000686
Lalloo C, Jibb LA, Rivera J, Agarwal A, Stinson JN (2015) There’s a pain app for that: Review of Patient-targeted Smartphone Applications for Pain Management. Clin. J. Pain 31(6):557–563. https://doi.org/10.1097/ajp.0000000000000171
Deverka PA et al (2012) Stakeholder participation in comparative effectiveness research: defining a framework for effective engagement. J Comp Eff Res 1(2):181–194. https://doi.org/10.2217/cer.12.7
Flury M, Caflisch U, Ullmann-Bremi A, Spichiger E (2011) Experiences of parents with caring for their child after a cancer diagnosis. J. Pediatr. Oncol. Nurs 28(3):143–153. https://doi.org/10.1177/1043454210378015
Henderschot E, Murphy C, Doyle S, Van-Clieaf J, Lowry J, Honeyford L (2005) Outpatient chemotherapy administration: decreasing wait times for patients and families. J. Pediatr. Oncol. Nurs 22(1):31–37. https://doi.org/10.1177/1043454204272539
van den Brink M, Bandell-Hoekstra EN, Abu-Saad HH (2001) The occurrence of recall bias in pediatric headache: a comparison of questionnaire and diary data. Headache 41(1):11–20 [Online]. Available: https://onlinelibrary.wiley.com/doi/pdf/10.1046/j.1526-4610.2001.111006011.x
Arksey H, O'Malley L (2005) Scoping studies: towards a methodological framework. Int. J. Soc. Res 8(1):19–32. https://doi.org/10.1080/1364557032000119616
Tricco AC et al (2018) PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann.Intern.Med 169(7):467–473. https://doi.org/10.7326/m18-0850
Ouzzani M, Hammady H, Fedorowicz Z, Elmagarmid A (2016) Rayyan — a web and mobile app for systematic reviews. Syst Rev 5(1):210. https://doi.org/10.1186/s13643-016-0384-4
Fleuren MA, Paulussen TG, Van Dommelen P, Van Buuren S (2014) Towards a measurement instrument for determinants of innovations. Int. J. Qual. Health Care 26(5):501–510. https://doi.org/10.1093/intqhc/mzu060
Ajayi TA, Salongo L, Zang Y, Wineinger N, Steinhubl S (2021) Mobile health-collected biophysical markers in children with serious illness-related pain. J. Palliat. Med 24(4):580–588. https://doi.org/10.1089/jpm.2020.0234
Bradford N, Condon P, Pitt E, Tyack Z, Alexander K (2021) Optimising symptom management in children with cancer using a novel mobile phone application: protocol for a controlled hybrid effectiveness implementation trial (RESPONSE). BMC Health Serv. Res 21(1):942. https://doi.org/10.1186/s12913-021-06943-x
Jibb LA et al (2017) Implementation and preliminary effectiveness of a real-time pain management smartphone app for adolescents with cancer: a multicenter pilot clinical study. Pediatric blood & cancer 64(10):e26554
Hunter JF et al (2020) A pilot study of the preliminary efficacy of Pain Buddy: a novel intervention for the management of children's cancer-related pain. Pediatric Blood & Cancer 67(10):e28278. https://doi.org/10.1002/pbc.28278
Erickson JM et al (2019) Using a heuristic app to improve symptom self-management in adolescents and young adults with cancer. J Adolesc Young Adult Oncol 8(2):131–141. https://doi.org/10.1089/jayao.2018.0103
Gartlehner G, Hansen RA, Nissman D, Lohr KN, Carey TS (2006) AHRQ technical reviews. In: Criteria for Distinguishing Effectiveness From Efficacy Trials in Systematic Reviews. Agency for Healthcare Research and Quality (US), Rockville (MD)
Hunter JF et al (2020) A pilot study of the preliminary efficacy of Pain Buddy: a novel intervention for the management of children’s cancer-related pain. Pediatr Blood Cancer 67(10):e28278. https://doi.org/10.1002/pbc.28278
Tran S, Smith L, El-Den S, Carter S (2022) The use of gamification and incentives in mobile health apps to improve medication adherence: scoping review. JMIR Mhealth Uhealth 10(2):e30671. https://doi.org/10.2196/30671
Borrelli B, Ritterband LM (2015) Special issue on eHealth and mHealth: challenges and future directions for assessment, treatment, and dissemination. Health Psychol 34s:1205–1208. https://doi.org/10.1037/hea0000323
Nilsen P (2015) Making sense of implementation theories, models and frameworks. Implement Sci 10(1):53. https://doi.org/10.1186/s13012-015-0242-0
Acknowledgements
We would like to thank all project leaders for participating in the interviews.
Availability of data
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Code availability
SPSS version 26.0 was used for all analyses.
Funding
This work was supported by the ZonMw under Grant Agreement No 844001505.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study’s conception and design. Material preparation, data collection, and analysis were performed by Julia D.H.P. Simon and Isabel S. Hooijman. The first draft of the manuscript was written by Julia D. H. P. Simon, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
Approval for the study was obtained from the Internal Review Board of the Princess Máxima Center for Pediatric Oncology and was performed in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki and its later amendments.
Consent to participate and for publication
Informed consent was obtained from all individual participants (i.e., project leaders) included in the study. The authors affirm that all participants consented to the publication of their data.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
APPENDIX 1.
PubMed search string
APPENDIX 2.
Interview guide
APPENDIX 3.
Summary semi-structured interviews
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Simon, J.D.H.P., Hooijman, I.S., Van Gorp, M. et al. Digital health tools for pain monitoring in pediatric oncology: a scoping review and qualitative assessment of barriers and facilitators of implementation. Support Care Cancer 31, 175 (2023). https://doi.org/10.1007/s00520-023-07629-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-023-07629-2