Abstract
Purpose
The most appropriate criteria and timing for palliative care referral remain a critical issue, especially in patients with metastatic breast cancer for whom long-term chemosensibility and survival are observed. We aimed to compare the impact of early palliative care including formal concertation with oncologists on decision for an additional line of chemotherapy compared with usual oncology care.
Methods
This randomized prospective study enrolled adult women with metastatic breast cancer and visceral metastases with a 3rd- or 4th-line chemotherapy (CT). Patients received usual oncology care with a palliative care consultation only upon patient or oncologist request (standard group, S) or were referred to systematic palliative care consultation including a regular concertation between palliative care team and oncologists (early palliative care group, EPC). The primary endpoint was the rate of an additional CT (4th or 5th line) decision. Quality of life, symptoms, social support and satisfaction were self-evaluated at 6 and 12 months, at treatment discontinuation or 3 months after discontinuation.
Results
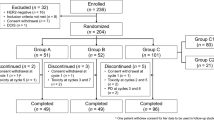
From January 2009 to November 2012, two authorized cancer centers included 98 women (EPC: 50; S: 48). Thirty-seven (77.1%, 95%CI 62.7–88%) patients in the EPC group had a subsequent chemotherapy prescribed and 36 (72.0%, 95%CI 57.5–83.8%) in the S group (p = 0.646). No differences in symptom control and global quality of life were observed, but less deterioration in physical functioning was reported in EPC (EPC: 0 [− 53–40]; S: − 6; 7 [− 60 to − 20]; p = 0.027). Information exchange and communication were significant improved in EPC (exchange, EPC: − 8.3 [− 30 to + 7]; S: 0.0 [− 17 to + 23]; p = 0.024; communication, EPC: 12.5 [− 8 to − 37]; S: 0.0 [− 21 to + 17]; p = 0.004).
Conclusion
EPC in metastatic breast cancer patients did not impact the prescription rate of additional chemotherapy in patients a 3rd- or 4th-line chemotherapy for metastatic breast cancer; however, EPC may contribute to alleviate deterioration in physical functioning, while facilitating communication.
Trial registration
ClinicalTrial.gov identifier: NCT00905281, May 20, 2009.


Similar content being viewed by others
Data availability
Data supporting the findings of this study is available within the article, and from the corresponding author upon reasonable request.
Code availability
Not applicable.
References
Molinié F, Tretarre B, Arveux P, Woronoff AM, Lecoffre C, Lafay L, et al. (2020) Survie des personnes atteintes de cancer en France métropolitaine 1989 2018. https://www.e-cancerfr 2020.
Siegel RL, Miller KD, Fuchs HE, Jemal A (2021) Cancer Statistics CA: A Cancer Journal for Clinicians 71:7–33
DeSantis CE, Ma J, Gaudet MM, Newman LA, Miller KD, Goding Sauer A et al (2019) Breast cancer statistics 2019. Cancer J Clin 69:438–51
Dufresne A, Pivot X, Tournigand C, Facchini T, Altweegg T, Chaigneau L et al (2008) Impact of chemotherapy beyond the first line in patients with metastatic breast cancer. Breast Cancer Res Treat 107:275–9. https://doi.org/10.1007/s10549-007-9550-7
Edman Kessler L, Sigfridsson J, Hatzidaki D, Bergh J, Foukakis T, Georgoulias V et al (2020) Chemotherapy use near the end-of-life in patients with metastatic breast cancer. Breast Cancer Res Treat 181:645–51. https://doi.org/10.1007/s10549-020-05663-w
Mathew A, Achkar T, Abberbock S, Sandhu GS, Jacob ME, Das Villgran V et al (2017) (2017) Prevalence and determinants of end-of-life chemotherapy use in patients with metastatic breast cancer. Breast J 23:718–22. https://doi.org/10.1111/tbj.12905
Shin JA, Parkes A, El-Jawahri A, Traeger L, Knight H, Gallagher ER et al (2016) Retrospective evaluation of palliative care and hospice utilization in hospitalized patients with metastatic breast cancer. Palliat Med 30:854–61. https://doi.org/10.1177/0269216316637238
Chen Y, Lin S, Zhu Y, Xu R, Lan X, Xiang F et al (2020) Prevalence, trend and disparities of palliative care utilization among hospitalized metastatic breast cancer patients who received critical care therapies. The Breast 54:264–71. https://doi.org/10.1016/j.breast.2020.11.001
Ferrell BR, Temel JS, Temin S, Alesi ER, Balboni TA, Basch EM et al (2017) Integration of palliative care into standard oncology care: American Society of Clinical Oncology Clinical Practice Guideline Update. J Clin Oncol 35:96–112. https://doi.org/10.1200/JCO.2016.70.1474
Jordan K, Aapro M, Kaasa S, Ripamonti CI, Scotté F, Strasser F et al (2018) European Society for Medical Oncology (ESMO) position paper on supportive and palliative care. Ann Oncol 29:36–43. https://doi.org/10.1093/annonc/mdx757
Zimmermann C, Swami N, Krzyzanowska M, Hannon B, Leighl N, Oza A et al (2014) Early palliative care for patients with advanced cancer: a cluster-randomised controlled trial. The Lancet 383:1721–30. https://doi.org/10.1016/S0140-6736(13)62416-2
Lu Z, Fang Y, Liu C, Zhang X, Xin X, He Y et al (2021) Early interdisciplinary supportive care in patients with previously untreated metastatic esophagogastric cancer: a phase iii randomized controlled trial. J Clin Oncol 39:748–56. https://doi.org/10.1200/JCO.20.01254
Temel JS, Greer JA, Admane S, Gallagher ER, Jackson VA, Lynch TJ et al (2011) Longitudinal perceptions of prognosis and goals of therapy in patients with metastatic non–small-cell lung cancer: results of a randomized study of early palliative care. J Clin Oncol 29:2319–26. https://doi.org/10.1200/JCO.2010.32.4459
Greer JA, Pirl WF, Jackson VA, Muzikansky A, Lennes IT, Heist RS et al (2012) Effect of early palliative care on chemotherapy use and end-of-life care in patients with metastatic non–small-cell lung cancer. J Clin Oncol 30:394–400. https://doi.org/10.1200/JCO.2011.35.7996
Earle CC, Landrum MB, Souza JM, Neville BA, Weeks JC, Ayanian JZ (2008) Aggressiveness of cancer care near the end of life: is it a quality-of-care issue? J Clin Oncol 26:3860–6. https://doi.org/10.1200/JCO.2007.15.8253
Haun MW, Estel S, Rücker G, Friederich H-C, Villalobos M, Thomas M, et al. (2017) Early palliative care for adults with advanced cancer. Cochrane Database of Systematic Reviews 2017;. https://doi.org/10.1002/14651858.CD011129.pub2.
Kavalieratos D, Corbelli J, Zhang D, Dionne-Odom JN, Ernecoff NC, Hanmer J et al (2016) Association between palliative care and patient and caregiver outcomes. JAMA 316:2104. https://doi.org/10.1001/jama.2016.16840
Jäger EM, Filipits M, Glechner A, Zwickl-Traxler E, Schmoranzer G, Pecherstorfer M et al (2020) Retrospective analysis of the prevalence of specialised palliative care services for patients with metastatic breast cancer. ESMO Open 5:e000905. https://doi.org/10.1136/esmoopen-2020-000905
Rabow M, Small R, Jow A, Majure M, Chien A, Melisko M et al (2018) The value of embedding: integrated palliative care for patients with metastatic breast cancer. Breast Cancer Res Treat 167:703–8. https://doi.org/10.1007/s10549-017-4556-2
Bakitas MA, Tosteson TD, Li Z, Lyons KD, Hull JG, Li Z et al (2015) Early versus delayed initiation of concurrent palliative oncology care: patient outcomes in the ENABLE III randomized controlled trial. J Clin Oncol 33:1438–45. https://doi.org/10.1200/JCO.2014.58.6362
McLachlan S-A, Allenby A, Matthews J, Wirth A, Kissane D, Bishop M et al (2001) Randomized trial of coordinated psychosocial interventions based on patient self-assessments versus standard care to improve the psychosocial functioning of patients with cancer. J Clin Oncol 19:4117–25. https://doi.org/10.1200/JCO.2001.19.21.4117
Aaronson NK, Ahmedzai S, Bergman B, Bullinger M, Cull A, Duez NJ et al (1993) The European Organization for Research and Treatment of Cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology. J Natl Cancer Inst 85:365–76. https://doi.org/10.1093/jnci/85.5.365
Cousson-Gélie F, Irachabal S, Bruchon-Schweitzer M, Dilhuydy JM, Lakdja F (2005) Dimensions of cancer locus of control scale as predictors of psychological adjustment and survival in breast cancer patients. Psychol Rep 97:699–711. https://doi.org/10.2466/pr0.97.3.699-711
Bolognini M, Bettschart W, Zehnder-Gubler M, Rossier L (1989) The validity of the French version of the GHQ-28 and PSYDIS in a community sample of 20 year olds in Switzerland. Eur Arch Psychiatry Neurol Sci 238:161–8. https://doi.org/10.1007/BF00451005
Barlési F, Chabert-Greillier L, Loundou A, Siméoni M-C, Greillier L, Doddoli C et al (2006) Validation de la version française du Princess Margaret Hospital Patient Satisfaction with Doctor Questionnaire (PMH/PSQ-MD): le F-PMH/PSQ-MD. Revue Des Maladies Respir 23:227–36. https://doi.org/10.1016/S0761-8425(06)71572-8
Greer JA, Moy B, El-Jawahri A, Jackson VA, Kamdar M, Jacobsen J et al (2022) Randomized trial of a palliative care intervention to improve end-of-life care discussions in patients with metastatic breast cancer. J Natl Compr Cancer Network 20:136–43. https://doi.org/10.6004/jnccn.2021.7040
Janah A, Gauthier LR, Morin L, Bousquet PJ, le Bihan-Benjamin C, Tuppin P et al (2019) Access to palliative care for cancer patients between diagnosis and death: a national cohort study. Clin Epidemiol 11:443–55. https://doi.org/10.2147/CLEP.S198499
Smith TJ, Temin S, Alesi ER, Abernethy AP, Balboni TA, Basch EM et al (2012) American Society of Clinical Oncology Provisional Clinical Opinion: The Integration of Palliative Care Into Standard Oncology Care. J Clin Oncol 30:880–7. https://doi.org/10.1200/JCO.2011.38.5161
Rochigneux P, Raoul JL, Beaussant Y, Aubry R, Goldwasser F, Tournigand C et al (2017) Use of chemotherapy near the end of life: what factors matter? Ann Oncol 28:809–17. https://doi.org/10.1093/annonc/mdw654
Gilligan T, Coyle N, Frankel RM, Berry DL, Bohlke K, Epstein RM et al (2017) Patient-clinician communication: American Society of Clinical Oncology Consensus Guideline. J Clin Oncol 35:3618–32. https://doi.org/10.1200/JCO.2017.75.2311
Chosich B, Burgess M, Earnest A, Franco M, Runacres F, William L et al (2020) Cancer patients’ perceptions of palliative care. Support Care Cancer 28:1207–14. https://doi.org/10.1007/s00520-019-04917-8
Fox JA, Rosenberg J, Ekberg S, Langbecker D (2020) Palliative care in the context of immune and targeted therapies: a qualitative study of bereaved carers’ experiences in metastatic melanoma. Palliat Med 34:1351–60. https://doi.org/10.1177/0269216320916154
LeBlanc TW (2020) Hoping for the best and preparing for the worst: a forgotten maxim in the immunotherapy era? Palliat Med 34:1289–90. https://doi.org/10.1177/0269216320954621
Hui D, Mori M, Watanabe SM, Caraceni A, Strasser F, Saarto T et al (2016) Referral criteria for outpatient specialty palliative cancer care: an international consensus. Lancet Oncol 17:e552-9. https://doi.org/10.1016/S1470-2045(16)30577-0
Molin Y, Gallay C, Gautier J, Lardy-Cleaud A, Mayet R, Grach M et al (2019) PALLIA-10, a screening tool to identify patients needing palliative care referral in comprehensive cancer centers: a prospective multicentric study (PREPA-10). Cancer Med 8:2950–61. https://doi.org/10.1002/cam4.2118
Acknowledgements
The authors thank Sophie DARNIS PhD (Centre Léon Bérard) for helpful comments and valuable help for medical editorial assistance.
Funding
Partial financial support was received from the French general direction of health care (PHRQ-2007), and Ligue contre le cancer (SHS 2010).
Author information
Authors and Affiliations
Contributions
G. C., P. S., J. P. G., O. T., P. R. and D. P. contributed to the study conception and design. Data collection was performed by G. C., C. B., P. S., V. D., J. P. G., O. T., P. R., S. P., I. R-C, P-YP, L. M., V. L. and T. B. Data curation was performed by V. B. B., A. L-C. and M. M. did the data analysis and contributed together with G. C. to the interpretation. The first draft of the manuscript was written by G. C. G. C. and C. B. closely revised the manuscript, with all authors contributing to the final review and approval of the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
This study was conducted with the ethical standards as laid down in the Declaration of Helsinki and its last amendments or comparable ethical standards, the International Conference on Harmonization on Good Medical Practices after local approvals from the ethics committee (Lyon Sud-Est IV), the French advisory committee on information in health research (CCTITS) and the French data protection authority (Commission Nationale de l’Informatique et des Libertés, CNIL). All patients provided written informed consent before enrolment. This study was registered with ClinicalTrial.gov, number NCT00905281, registered on May 20, 2009.
Conflict of interest
The authors declare no competing interests.
Disclaimer
The funders had no role in the design, conduct, analysis or reporting of the trial.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chvetzoff, G., Bouleuc, C., Lardy-Cléaud, A. et al. Impact of early palliative care on additional line of chemotherapy in metastatic breast cancer patients: results from the randomized study OSS. Support Care Cancer 31, 82 (2023). https://doi.org/10.1007/s00520-022-07561-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-022-07561-x