Abstract
Objective
To assess the effect of physical therapy on cancer-related fatigue (CRF) during cytotoxic anticancer treatment.
Methods
Systematic review with meta-analysis of randomized clinical trials published from 2010 to 2021 (EMBASE, MEDLINE, PEDro; SciELO, and LILACS). Studies assessing the effect of supervised physical therapy (IG) for the management of CRF on adults undergoing anticancer treatment compared with a control group (CG) covering usual care or any uncontrolled practice, such as recommendations about exercise and health education, were included in this review.
Results
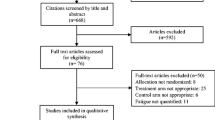
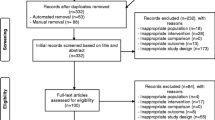
A total of 22 studies were included in the SR and 21 in the meta-analysis, resulting in 1.992 individuals (CG = 973 and IG = 1.019). There was a reduction in general fatigue [SMD = − 0.69; 95%CI (− 1.15, − 0.22) p < 0.01; I2 = 87%; NNT = 3], with greater weight attributed to combined exercise (44%). Physical fatigue also reduced [SMD = − 0.76; 95%CI (− 1.13, − 0.39) p < 0.01; I2 = 90%; NNT = 2], with greater weight for resistance exercise (50%) and greater effect with combined exercise [SMD = − 1.90; 95%CI (− 3.04, − 0.76) p < 0.01; I 2 = 96%]. There was reduction in general fatigue with moderate intensity (74%) [SMD = − 0.89; 95%CI (− 1.61, − 0.17) p < 0.02; I2 = 90%] and physical fatigue [SMD = − 1.00; 95%CI (− 1.54, − 0.46) p < 0.01; I2 = 92%], while high intensity reduced only general fatigue [SMD = − 0.35; 95%CI (− 0.51, − 0.20) p < 0.01; I2 = 0%]. The number of overall and weekly sessions has been shown to contribute to the reduction of CRF.
Conclusion
Physical rehabilitation with moderate intensity promoted greater relief of general and physical fatigue. Even after controlling for high heterogeneity, the quality of evidence, summarized in GRADE, was considered moderate for general fatigue and low for physical fatigue.




Similar content being viewed by others
Data availability
This study did not generate any new data.
References
Mattiuzzi C, Lippi G (2019) Current cancer epidemiology. J Epidemiol Glob Health 9(4):217–222. https://doi.org/10.2991/jegh.k.191008.001
O’Higgins CM, Brady B, O’Connor B et al (2018) The pathophysiology of cancer-related fatigue: current controversies. Supp Care Cancer 26:3353–3364. https://doi.org/10.1007/s00520-018-4318-7
Bower JE et al (2014) Cancer-related fatigue-mechanisms, risk factors, and treatments. Nat Rev Clin Oncol 11(10):597–609. https://doi.org/10.1038/nrclinonc.2014.127
Beaver CC, Magnan MA (2016) Managing chemotherapy side effects: achieving reliable and equitable outcomes. Clin J Oncol Nurs. 20(6):589–591. https://doi.org/10.1188/16.CJON.589-591
Strebkova R (2020) Cancer-related fatigue in patients with oncological diseases: causes, prevalence, guidelines for assessment and management. Folia Med (Plovdiv) 62(4):679–689. https://doi.org/10.3897/folmed.62.e50517
Fabi A, Bhargava R, Fatigoni S, Guglielmo M, Horneber M, Roila F, Weis J, Jordan K, Ripamonti, (2020) Cancer-related fatigue: ESMO Clinical Practice Guidelines for diagnosis and treatment. Ann Oncol. 31(6):713–723. https://doi.org/10.1016/j.annonc.2020.02.016
Bo Y, Jiansheng W (2017) Effects of exercise on cancer-related fatigue and quality of life in prostate cancer patients undergoing androgen deprivation therapy: a meta-analysis of randomized clinical trials. Chinese medical sciences jornal 32(1):13–21. https://doi.org/10.24920/J1001-9242.2007.002
Wu C, Zheng Y, Duan Y, Lai X, Cui S, Xu N, Tang C, Lu L (2019) Nonpharmacological interventions for cancer-related fatigue: a systematic review and Bayesian network meta-analysis. Worldviews Evid Based Nurs 16(2):102–110. https://doi.org/10.1111/wvn.12352
Arring M, Barton L, Brooks T, Zick M (2019) Integrative therapies for cancer-related fatigue. Cancer J 25(5):349–356. https://doi.org/10.1097/PPO.0000000000000396
Mehl A, Reif M, Zerm R, Pranga D, Friemel D, Berger B, Brinkhaus B, Gutenbrunner C, Büssing A, Kröz M (2020) Impact of a multimodal and combination therapy on self-regulation and internal coherence in German breast cancer survivors with chronic cancer-related fatigue: a mixed-method comprehensive cohort design study. Integr Cancer Ther 19:1534735420935618. https://doi.org/10.1177/1534735420935618
Wagoner CW, Lee JT, Battaglini CL (2021) Community-based exercise programs and cancer-related fatigue: a systematic review and meta-analysis. Support Care Cancer 29(9):4921–4929. https://doi.org/10.1007/s00520-021-06135-7
Thong Y, Van Noorden F, Steindorf K, Arndt V (2020) Cancer-related fatigue: causes and current treatment options. Curr Treat Options Oncol. 21(2):17. https://doi.org/10.1007/s11864-020-0707-5
Hilfiker R, Meichtry A, Eicher M, Nilsson Balfe L, Knols RH, Verra ML, Taeymans J (2018) Exercise and other non-pharmaceutical interventions for cancer-related fatigue in patients during or after cancer treatment: a systematic review incorporating an indirect-comparisons meta-analysis. Br J Sports Med 52(10):651–658. https://doi.org/10.1136/bjsports-2016-096422
Kuchinski M, Reading M, Lash A (2009) Treatment-related fatigue and exercise in patients with cancer: a systematic review. Medsurg Nurs 18(3):174–180
Van Vulpen K, Peeters H, Velthuis J, Van der Wall E, May M (2016) Effects of physical exercise during adjuvant breast cancer treatment on physical and psychosocial dimensions of cancer-related fatigue: a meta-analysis. Maturitas 85:104–111. https://doi.org/10.1016/j.maturitas.2015.12.007
Ashcraft A, Warner B, Jones W, Dewhirst W (2019) Exercise as adjunct therapy in cancer. Semin Radiat Oncol 29(1):16–24. https://doi.org/10.1016/j.semradonc.2018.10.001
Pyszora A, Budzyński J, Wójcik A, Prokop A, Krajnik M (2017) Physiotherapy programme reduces fatigue in patients with advanced cancer receiving palliative care: randomized controlled trial. Support Care Cancer 25(9):2899–2908. https://doi.org/10.1007/s00520-017-3742-4
Mijwel S et al (2018) Exercise training during chemotherapy preservesskeletal muscle fiber area, capillarization, andmitochondrial content in patients with breast cancer. FASEB J. 32:5495–5505
Cramp F, Daniel J (2008) Exercise for the management of cancer-related fatigue in adults. Cochrane Database of Systematic Reviews. Issue 2. https://doi.org/10.1002/14651858.CD006145.pub2
Higgins J, Green S. (2011) Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0. The Cochrane Collaboration: The Cochrane Collaboration
Furukawa TA, Leucht S (2011) How to obtain NNT from Cohen’s d: comparison of two methods. PLoS One 6(4):e19070. https://doi.org/10.1371/journal.pone.0019070
Hacker D, Larson J, Kujath A, Peace D, Rondelli D, Gaston L (2011) Strength training following hematopoietic stem cell transplantation. Cancer Nurs 34(3):238–249. https://doi.org/10.1097/NCC.0b013e3181fb3686
Schmidt E, Wiskemann J, Armbrust P, Schneeweiss A, Ulrich M, Steindorf K (2015) Effects of resistance exercise on fatigue and quality of life in breast cancer patients undergoing adjuvant chemotherapy: a randomized controlled trial. Int J Cancer 137(2):471–480. https://doi.org/10.1002/ijc.29383
Steindorf K, Schmidt ME, Klassen O, Ulrich CM, Oelmann J et al (2014) Randomized, controlled trial of resistance training in breast cancer patients receiving adjuvant radiotherapy: results on cancer-related fatigue and quality of life. Ann Oncol 25(11):2237–2243. https://doi.org/10.1093/annonc/mdu374
Andersen C, Rørth M, Ejlertsen B, Stage M, Møller T, Midtgaard J, Quist M, Bloomquist K, Adamsen L (2013) The effects of a six-week supervised multimodal exercise intervention during chemotherapy on cancer-related fatigue. Eur J Oncol Nurs 17(3):331–339. https://doi.org/10.1016/j.ejon.2012.09.003
Cormie P, Galvão A, Spry N, Joseph D, Chee R, Taaffe R, Chambers K, Newton RU (2015) Can supervised exercise prevent treatment toxicity in patients with prostate cancer initiating androgen-deprivation therapy: a randomised controlled trial. BJU Int 115(2):256–266. https://doi.org/10.1111/bju.12646
Hojan K, Kwiatkowska-Borowczyk E, Leporowska E, Milecki P (2017) Inflammation, cardiometabolic markers, and functional changes in men with prostate cancer A randomized controlled trial of a 12-month exercise program. Pol Arch Intern Med 127(1):25–35. https://doi.org/10.20452/pamw.3888
Hojan K, Kwiatkowska-Borowczyk E, Leporowska E, Górecki M, Ozga-Majchrzak O, Milecki T, Milecki P (2016) Physical exercise for functional capacity, blood immune function, fatigue, and quality of life in high-risk prostate cancer patients during radiotherapy: a prospective, randomized clinical study. Eur J Phys Rehabil Med 52(4):489–501
Cooper HM, Hedges LV, Valentine JC (2019) Handbook of research synthesis and meta-analysis, 3rd edn. Russell Sage Foundation, New York NY
Faraone SV (2008) Interpreting estimates of treatment effects: implications for managed care. P T. 33(12):700–11
Guyatt H, Oxman D, Vist E, Kunz R, Falck-Ytter Y, Alonso-Coello P (2008) GRADE Working Group GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ. 336(7650):924–926
Al-Majid S, Wilson D, Rakovski C, Coburn W (2015) Effects of exercise on biobehavioral outcomes of fatigue during cancer treatment: results of a feasibility study. Biol Res Nurs 17(1):40–48. https://doi.org/10.1177/1099800414523489
Bolam A, Mijwel S, Rundqvist H, Wengström Y (2019) Two-year follow-up of the OptiTrain randomised controlled exercise trial. Breast Cancer Res Treat 175(3):637–648. https://doi.org/10.1007/s10549-019-05204-0
Dhillon M, Bell L, van der Ploeg HP, Turner D et al (2017) Impact of physical activity on fatigue and quality of life in people with advanced lung cancer: a randomized controlled trial. Ann Oncol. 28(8):1889–1897. https://doi.org/10.1093/annonc/mdx205
Mijwel S, Backman M, Bolam A, Jervaeus A, Sundberg J, Margolin S, Browall M, Rundqvist H, Wengström Y (2018) Adding high-intensity interval training to conventional training modalities: optimizing health-related outcomes during chemotherapy for breast cancer: the OptiTrain randomized controlled trial. Breast Cancer Res Treat 168(1):79–93. https://doi.org/10.1007/s10549-017-4571-3
Cešeiko R, Eglītis J, Srebnijs A, Timofejevs M, Purmalis E, Erts R, Vētra A, Tomsone S (2019) The impact of maximal strength training on quality of life among women with breast cancer undergoing treatment. Exp Oncol 41(2):166–172. https://doi.org/10.32471/exp-oncology.2312-8852.vol-41-no-2.13249
Grote M, Maihöfer C, Weigl M, Davies-Knorr P, Belka C (2018) Progressive resistance training in cachectic head and neck cancer patients undergoing radiotherapy: a randomized controlled pilot feasibility trial. Radiat Oncol. 13(1):215. https://doi.org/10.1186/s13014-018-1157-0
Hacker D, Collins E, Park C, Peters T, Patel P, Rondelli D (2017) Strength training to enhance early recovery after hematopoietic stem cell transplantation. Biol Blood Marrow Transplant 23(4):659–669. https://doi.org/10.1016/j.bbmt.2016.12.637
Rogers Q, Anton M, Fogleman A, Hopkins-Price P et al (2013) Pilot, randomized trial of resistance exercise during radiation therapy for head and neck cancer. Head Neck 35(8):1178–1188. https://doi.org/10.1002/hed.23118
Baumann T, Zopf M, Nykamp E, Kraut L, Schüle K, Elter T, Fauser AA, Bloch W (2011) Physical activity for patients undergoing an allogeneic hematopoietic stem cell transplantation: benefits of a moderate exercise intervention. Eur J Haematol. 87(2):148–56. https://doi.org/10.1111/j.1600-0609.2011.01640.x
Rogers Q, Vicari S, Trammell R, Hopkins-Price P, Fogleman A et al (2014) Biobehavioral factors mediate exercise effects on fatigue in breast cancer survivors. Med Sci Sports Exerc 46(6):1077–1088. https://doi.org/10.1249/MSS.0000000000000210
Samuel R, Maiya G, Fernandes J, Guddattu V, Saxena P, Kurian R, Lin J, Mustian M (2019) Effectiveness of exercise-based rehabilitation on functional capacity and quality of life in head and neck cancer patients receiving chemo-radiotherapy. Support Care Cancer 27(10):3913–3920. https://doi.org/10.1007/s00520-019-04750-z
Travier N, Velthuis J, Steins Bisschop N, van den BuijsMonninkhof EM et al (2015) Effects of an 18-week exercise programme started early during breast cancer treatment: a randomised controlled trial. BMC Med. 13:121. https://doi.org/10.1186/s12916-015-0362-z
Van Vulpen K, Velthuis J, Steins Bisschop N, Travier N, Van Den J et al (2016) Effects of an exercise program in colon cancer patients undergoing chemotherapy. Med Sci Sports Exerc 48(5):767–775. https://doi.org/10.1249/MSS.0000000000000855
Van Waart H, Stuiver M, van Harten H, Geleijn E, Kieffer M et al (2015) Effect of low-intensity physical activity and moderate- to high-intensity physical exercise during adjuvant chemotherapy on physical fitness, fatigue, and chemotherapy completion rates: results of the PACES randomized clinical trial. J Clin Oncol. 33(17):1918–27. https://doi.org/10.1200/JCO.2014.59.1081
Oechsle K, Aslan Z, Suesse Y, Jensen W, Bokemeyer C, de Wit M (2014) Multimodal exercise training during myeloablative chemotherapy: a prospective randomized pilot trial. Support Care Cancer 22(1):63–69. https://doi.org/10.1007/s00520-013-1927-z
Echávez M, Jiménez G, Vélez R (2015) Effects of supervised multimodal exercise interventions on cancer-related fatigue: systematic review and meta-analysis of randomized controlled trials. Biomed Res Int. https://doi.org/10.1155/2015/328636
George A, Kelley A, Kelley S (2017) Exercise and cancer-related fatigue in adults: a systematic review of previous systematic reviews with meta-analyses. BMC Cancer 17:693
Pearson M, Morris E, Di Stefano M, Mckintry E (2016) Interventions for cancer-related fatigue: a scoping review. European Journal of Cancer Care
Arpin D et al (2005) Early variations of circulating interleukin-6 and interleukin-10 levels during thoracic radiotherapy are predictive for radiation pneumonitis. J Clin Oncol 23:8748–8756
Bower E et al (2011) Inflammation and behavioural symptoms after breast cancer treatment: do fatigue, depression, and sleep disturbance share a common underlying mechanism? J Clin Oncol 29:3517–3522
Yuxia Ma et. al (2020) Prevalence and risk factors of cancer-related fatigue: a systematic review and meta-analysis. International Journal of Nursing Studies 2020; Volume 111
Yang S, Chu S, Gao Y, Ai Q, Liu Y, Li X, Chen N (2019) A narrative review of cancer-related fatigue (CRF) and its possible pathogenesis. Cells 8(7):738. https://doi.org/10.3390/cells8070738
Mustian M, Alfano M, Heckler C, Kleckner S, Kleckner R et al (2017) Comparison of pharmaceutical, psychological, and exercise treatments for cancer-related fatigue: a meta-analysis. JAMA Oncol 3(7):961–968. https://doi.org/10.1001/jamaoncol.2016.6914
Sasso JP et al (2015) A framework for prescription in exercise-oncology research. J Cachexia Sarcopenia Muscle 6:115–124. https://doi.org/10.1002/jcsm.12042
Brown C, Huedo-Medina B, Pescatello S, Pescatello M, Ferrer A, Johnson T (2011) Efficacy of exercise interventions in modulating cancer-related fatigue among adult cancer survivors: a meta-analysis. Cancer Epidemiol Biomarkers Prev 20(1):123–133. https://doi.org/10.1158/1055-9965.EPI-10-0988
Lahart M, Metsios S, Nevill M, Carmichael R (2018) Physical activity for women with breast cancer after adjuvant therapy. Cochrane Database Syst Rev. 1(1):CD011292. https://doi.org/10.1002/14651858.CD011292
Stout L, Baima J, Swisher K, Winters-Stone M, Welsh J (2017) A systematic review of exercise systematic reviews in the cancer literature (2005–2017). PM R 9(9S2):S347–S384. https://doi.org/10.1016/j.pmrj.2017.07.074
Author information
Authors and Affiliations
Contributions
All authors planned the search strategy; Giana Penna, Tassiana da Silva, and Douglas Maquart Otto performed the searches and extracted the data into tables and endnote which were checked by Fabricio Macagnan. Anderson Pedroni synthesised the findings. Giana Penna, Douglas Maquart Otto, and Tassiana da Silva drafted the paper; Fabricio Macagnan and Anderson Pedroni critically revised the work. All authors contributed to the writing and editing of the final draft and have approved the submitted version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Penna, G.B., Otto, D.M., da Silva, T.C. et al. Physical rehabilitation for the management of cancer-related fatigue during cytotoxic treatment: a systematic review with meta-analysis. Support Care Cancer 31, 129 (2023). https://doi.org/10.1007/s00520-022-07549-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-022-07549-7