Abstract
Purpose
Patients with primary malignant brain tumors have high symptom burden and commonly rely on family caregivers for practical and emotional support. This can lead to negative mental and physical consequences for caregivers. We investigated effectiveness of an 8-week nurse-led online needs-based support program (SmartCare©) with and without online self-guided cognitive behavioral therapy (CBT) for depression compared to enhanced care as usual (ECAU) on depressive symptoms, caregiving-specific distress, anxiety, mastery, and burden.
Methods
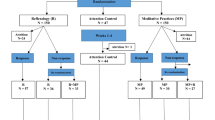
Family caregivers scoring ≥ 6 on a depressive symptoms inventory were randomized to three groups: ECAU plus self-guided CBT and SmartCare©; ECAU plus SmartCare©; ECAU only. Primary outcomes (depressive symptoms; caregiving-specific distress) and secondary outcomes (anxiety, caregiver mastery, and caregiver burden) were assessed online. Intention to treat (ITT) and per protocol (PP) analyses of covariance corrected for baseline scores were performed for outcomes at 4 months.
Results
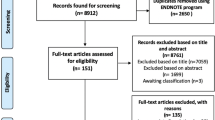
In total, 120 family caregivers participated. Accrual and CBT engagement were lower than expected, therefore intervention groups were combined (n = 80) and compared to ECAU (n = 40). For depressive symptoms, no statistically significant group differences were found. Caregiving-specific distress decreased in the intervention group compared with ECAU (ITT: p = 0.01, partial ɳ2 = 0.08; PP: p = 0.02, partial ɳ2 = 0.08). A trend towards improvement in mastery for the intervention group compared with ECAU was identified (ITT: p = 0.08, partial ɳ2 = 0.04; PP: p = 0.07, partial ɳ2 = 0.05).
Conclusions
SmartCare©, with or without self-guided CBT, reduced caregiving-specific distress with a trend towards improving mastery. SmartCare© has the potential to improve the lives of families coping with a brain tumor diagnosis.
Trial registration number
NCT02058745; 10 February 2014


Similar content being viewed by others
Data availability
All raw data is held securely by the research team and access can be requested if required.
Change history
24 May 2022
A Correction to this paper has been published: https://doi.org/10.1007/s00520-022-07146-8
References
Louis DN, Perry A, Reifenberger G et al (2016) The 2016 World Health Organization classification of tumors of the central nervous system: a summary. Acta Neuropathol 131:803–820
IJzerman-Korevaar M, Snijders TJ, de Graeff A, Teunissen SC, de Vos FY (2018) Prevalence of symptoms in glioma patients throughout the disease trajectory: a systematic review. J Neuro-oncol 140:485–496
Sherwood PR, Cwiklik M, Donovan HS (2016) Neuro-oncology family caregiving: review and directions for future research. CNS Oncol 5:41–48
Choi CW, Stone RA, Kim KH et al (2012) Group-based trajectory modeling of caregiver psychological distress over time. Ann Behav Med 44:73–84
Bayen E, Laigle-Donadey F, Prouté M, Hoang-Xuan K, Joël M-E, Delattre J-Y (2017) The multidimensional burden of informal caregivers in primary malignant brain tumor. Support Care Cancer 25:245–253
Sherwood PR, Donovan H. SmartCare: Innovations in Caregiving Interventions: National Cancer Institute 2012–2015
Grunfeld E, Coyle D, Whelan T et al (2004) Family caregiver burden: results of a longitudinal study of breast cancer patients and their principal caregivers. Can Med Assoc J 170:1795–1801
Boele F, Given C, Given B et al (2017) Family caregivers’ level of mastery predicts survival of glioblastoma patients: a preliminary report. Cancer 123:832–840
Boele FW, Rooney AG, Bulbeck H, Sherwood PR (2019) Interventions to help support caregivers of people with a brain or spinal cord tumour. Cochrane Database Syst Rev 7:CD012582
Boele F, van Uden-Kraan C, Hilverda K et al (2016) Attitudes and preferences towards monitoring supportive care needs in glioma patients and their informal caregivers. Support Care Cancer 24:3011–3022
Boele FW, van Uden-Kraan CF, Hilverda K et al (2017) Neuro-oncology family caregivers’ view on keeping track of care issues using eHealth systems: it’s a question of time. J Neurooncol 134:157–167
Chi N-C, Demiris G (2015) A systematic review of telehealth tools and interventions to support family caregivers. J Telemed Telecare 21:37–44
Ownsworth T, Chan RJ, Jones S, Robertson J, Pinkham MB (2021) Use of telehealth platforms for delivering supportive care to adults with primary brain tumors and their family caregivers: a systematic review. Psychooncology 30:16–26
Proudfoot J, Ryden C, Everitt B et al (2004) Clinical efficacy of computerised cognitive-behavioural therapy for anxiety and depression in primary care: randomised controlled trial. Br J Psychiatry 185:46–54
Arida JA, Sherwood PR, Flannery M, Donovan HS (2016) Representational approach: a conceptual framework to guide patient education research and practice. Oncol Nurs Forum 46:781–783
Foroushani PS, Schneider J, Assareh N (2011) Meta-review of the effectiveness of computerised CBT in treating depression. BMC Psychiatry 11:131
Andresen EM, Malmgren JA, Carter WB, Patrick DL (1994) Screening for depression in well older adults: Evaluation of a short form of the CES-D. Am J Prev Med 10:77–84
Boele FW, Terhorst L, Prince J, Donovan HS, Weimer J, Lieberman FS, Drappatz J, Sherwood PR (2019) Psychometric evaluation of the Caregiver Needs Screen in neuro-oncology family caregivers. J Nurs Meas 27:162–176
Usala PD, Hertzog C (1989) Measurement of affective states in adults evaluation of an adjective rating scale instrument. Res Aging 11:403–426
Pearlin LI, Schooler C (1978) The structure of coping. J Health Soc Behav 19(1):2–21
Given C, Given B, Stommel M, Collins C, King S, Franklin S (1992) The caregiver reaction assessment (CRA) for caregivers to persons with chronic physical and mental impairments. Res Nurs Health 15:271–283
Sherwood PR, Given BA, Donovan H et al (2008) Guiding research in family care: a new approach to oncology caregiving. Psychooncology 17:986–996
Karyotaki E, Efthimiou O, Miguel C et al (2021) Internet-based cognitive behavioral therapy for depression: A systematic review and individual patient data network meta-analysis. JAMA Psychiatry 78(4):361–371
Melville K, Casey L, Kavanagh D (2010) Dropout from internet-based treatment for psychological disorders. Br J Clin Psychol 49:455–471
Christensen H, Griffiths K, Farrer L (2009) Adherence in internet interventions for anxiety and depression: systematic review. J Med Intern Res 11:e13
Acknowledgements
We would like to thank the research nurses and staff involved: Judy Knapp RN, Anna Fisher RN, Sue Hughes RN, Mary Roberge RN, Sue Misko RN, A. Blair Powell BS. We also thank participating caregivers and patients, and the clinical teams that have supported recruitment.
Funding
This work was funded by the National Institute for Nursing Research R01 NR013170. Florien Boele was supported by a Yorkshire Cancer Research Fellowship (L389FB).
Author information
Authors and Affiliations
Contributions
Florien Boele: data curation, formal analysis, writing (original draft), writing (review and editing). Jason Weimer: investigation, data curation, project administration, writing (review and editing). Judith Proudfoot: conceptualization, writing (review and editing). Anna Marsland, Charles Given: conceptualization, methodology, writing (review and editing). Terri Armstrong: investigation, data curation, writing (review and editing). Jan Drappatz: data curation, resources, writing (review and editing). Heidi Donovan: conceptualization, investigation, methodology, supervision, funding acquisition, writing (review and editing). Paula Sherwood: conceptualization, investigation, methodology, data curation, supervision, funding acquisition, writing (review and editing).
Corresponding authors
Ethics declarations
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Consent to participate
All participants provided written informed consent.
Consent for publication
All participants provided consent for publication.
Competing interests
Jan Drappatz: equity from Gilead and Pfizer, consulting fees from Agios. Judith Proudfoot: involved in development of Beating the Blues, and consultancy to the company formerly distributing the program. All other authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Heidi S Donovan and Paula R Sherwood are co-senior authors.
This article has already been printed but the online version is revised. Judith Proudfoot wanted to be removed in the authorgroup.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Boele, F.W., Weimer, J.M., Marsland, A.L. et al. The effects of SmartCare© on neuro-oncology family caregivers’ distress: a randomized controlled trial. Support Care Cancer 30, 2059–2068 (2022). https://doi.org/10.1007/s00520-021-06555-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-021-06555-5