Abstract
Purpose
Cardiovascular disease, often secondary to chemotherapy, is the leading cause of death in BC survivors. Increased aerobic capacity improves post-rehabilitation survival; however, many cancer rehabilitation programs are limited to lower intensity training. High-intensity interval training (HIIT) is associated with the largest improvements in aerobic capacity; therefore, this study aimed to determine whether HIIT would cause a greater increase in VO2peak than continuous moderate-intensity (MICT) exercise in previously trained BC survivors.
Methods
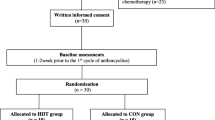
Twenty BC survivors who had completed a low/moderate-intensity exercise rehabilitation program performed a VO2peak test and received a dual-energy X-ray absorptiometry (DXA) scan at baseline and after randomization into a 12-week HIIT or MICT program. ANOVA with repeated measures determined the effects of the different training programs on aerobic capacity and body composition.
Results
Both groups began the training program near or above age- and sex-matched VO2peak norms. Pre- to post-intervention improvements in VO2peak (P = 0.006) and waist circumference (P = 0.007) were found in both groups; however, there were no between-group differences. Minute ventilation and peak workload increased in the HIIT group (P < 0.05) but not the MICT group. Body composition was not different after either training program.
Conclusions
These data suggest that transitioning from low/moderate-intensity exercise to moderate/high-intensity exercise causes further clinically relevant increases in VO2peak in previously trained BC survivors. HIIT did not cause a significantly greater improvement in VO2peak than MICT; however, future studies with greater intensity and frequency of training are encouraged.
Similar content being viewed by others
Data availability
Not applicable.
Code availability
Not applicable.
References
Ministry of Health. Cancer: Historical Summary 1948–2015 (2018) Ministry of Health: Wellington, New Zealand
Patnaik JL, Byers T, DiGuiseppi C, Dabelea D, Denberg TD (2011) Cardiovascular disease competes with breast cancer as the leading cause of death for older females diagnosed with breast cancer: a retrospective cohort study. Breast Cancer Res 3:R64
Gernaat SAM, Ho PJ, Rijnberg N, Emaus MJ, Baak LM, Hartman M, Grobbee DE, Verkooijen HM (2017) Risk of death from cardiovascular disease following breast cancer: a systematic review. Breast Cancer Res Treat 164:537–535
Ramin C, Schaeffer ML, Zheng Z, Connor AE, Hoffman-Bolton J, Lau B, Visvanathan K (2020) All-cause and cardiovascular disease mortality among breast cancer survivors in CLUE II, a long-standing community-based cohort. J Natl Cancer Inst. https://doi.org/10.1093/jnci/djaa096
Kirkham AA, Ian Paterson D, Prado CM, Mackey JR, Courneya KS, Pituskin E, Thompson RB (2019) Curing breast cancer and killing the heart: a novel model to explain elevated cardiovascular disease and mortality risk among women with early stage breast cancer. Prog Cardiovasc Dis 62:116–126
Schmid D, Leitzmann MF (2015) Cardiorespiratory fitness as predictor of cancer mortality: a systematic review and meta-analysis. Ann Oncol 26:272–278
Brawner CA, Al-Mallah MH, Ehrman JK, Qureshi WT, Blaha MJ, Keteyian SJ (2017) Change in maximal exercise capacity is associated with survival in men and women. Mayo Clin Proc 92:383–390
Sheean PM, Hoskins K, Stolley M (2012) Body composition changes in females treated for breast cancer: a review of the evidence. Breast Cancer Res Treat 135:663–680
Villasenor A, Ballard-Barbash R, Baumgartner K, Baumgartner R, Bernstein L, McTiernan A, Neuhouser ML (2012) Prevalence and prognostic effect of sarcopenia in breast cancer survivors: the HEAL Study. J Cancer Surviv 6:398–406
Soares Falcetta F, de Araújo Vianna Träsel H, de Almeida FK, Rangel Ribeiro Falcetta M, Falavigna M, Dornelles Rosa D, (2018) Effects of physical exercise after treatment of early breast cancer: systematic review and meta-analysis. Breast Cancer Res Treat 170:455–476
Brown JC, Schmitz KH (2015) Weight lifting and appendicular skeletal muscle mass among breast cancer survivors: a randomized controlled trial. Breast Cancer Res Treat 151:385–392
Santos WDND, Gentil P, De Moraes RF, Júnior JBF, Campos MH, De Lira CAB, Junior RF, Bottaro M, Vieira CA (2017) Chronic effects of resistance training in breast cancer survivors. Bio Med Res Int. https://doi.org/10.1155/2017/8367803
Schmitz KH, Ahmed RL, Hannan PJ, Yee D (2005) Safety and efficacy of weight training in recent breast cancer survivors to alter body composition, insulin, and insulin-like growth factor axis proteins. Cancer Epidemiol Biomarkers Prev 14:1672
Schmitz K, Courneya K, Matthews C et al (2010) American College of Sports Medicine roundtable on exercise guidelines for cancer survivors. Med Sci Sports Exerc 42:1409–1426
McNeely ML, Campbell KL, Rowe BH, Klassen TP, Mackey JR, Courneya KS (2006) Effects of exercise on breast cancer patients and survivors: a systematic review and meta-analysis. Can Med Assoc J 175:34–41
Martland R, Mondelli V, Gaughran F, Stubbs B (2020) Can high-intensity interval training improve physical and mental health outcomes? A meta-review of 33 systematic reviews across the lifespan. J Sports Sci 38:430–446
Williams CJ, Gurd BM, Bonafiglia JT et al (2019) A multi-center comparison of VO2peak trainability between interval training and moderate intensity continuous training. Front Physiol 10:19. https://doi.org/10.3389/fphys.2019.00019
Dolan LB, Campbell K, Gelmon K, Neil-Sztramko S, Holmes D, McKenzie DC (2016) Interval versus continuous aerobic exercise training in breast cancer survivors-a pilot RCT. Support Care Cancer 24:119–127
Iellamo F, Caminiti G, Sposato B, Vitale C, Massaro M, Rosano G, Volterrani M (2014) Effect of high-intensity interval training versus moderate continuous training on 24-h blood pressure profile and insulin resistance in patients with chronic heart failure. Intern Emerg Med 9:547–552
De Groot PCE, Hjeltnes N, Heijboer AC, Stal W, Birkeland K (2003) Effect of training intensity on physical capacity, lipid profile and insulin sensitivity in early rehabilitation of spinal cord injured individuals. Spinal Cord 41:673–679
Streiner D, Geddes J (2001) Intention to treat analysis in clinical trials when there are missing data. Evid-Based Ment Health 4:70
Rapp D, Scharhag J, Wagenpfeil S, Scholl J (2018) Reference values for peak oxygen uptake: cross-sectional analysis of cycle ergometry-based cardiopulmonary exercise tests of 10090 adult German volunteers from the Prevention First Registry. BMJ Open 8:e018697
Myers J, Prakash M, Froelicher V, Do D, Partington S, Atwood JE (2002) Exercise capacity and mortality among men referred for exercise testing. N Engl J Med 346:793–801
Peel JB, Sui X, Adams SA, Hebert JR, Hardin JW, Blair SN (2009) A prospective study of cardiorespiratory fitness and BC mortality. Med Sci Sports Exerc 41:742–748
Roger VL, Jacobsen SJ, Pelikka PA, Miller TD, Bailey KR, Gersh BJ (1998) Prognostic value of treadmill exercise testing: a population-based study in Olmsted County, Minnesota. Circulation 98:2836–2841
Rognmo O, Moholdt T, Bakken H, Hole T, Mølstad P, Myhr NE, Grimsmo J, Wisløff U (2012) Cardiovascular risk of high-versus moderate-intensity aerobic exercise in coronary heart disease patients. Circulation 126:1436–1440
Wisløff U, Støylen A, Loennechen JP, Bruvold M, Rognmo O, Haram PM, Tjønna AE, Helgerud J, Slørdahl SA, Lee SJ, Videm V, Bye A, Smith GL, Najjar SM, Ellingsen O, Skjӕrpe T (2007) Superior cardiovascular effect of aerobic interval training versus moderate continuous training in heart failure patients: a randomised study. Circulation 115:3086–3094
Tjønna AE, Lee SJ, Rognmo O, Stølen TO, Bye A, Haram PM, Loennechen JP, Al-Share QY, Skogvoll E, Slørdahl SA, Kemi OJ, Najjar SM, Wisloff U (2018) Aerobic interval training versus continuous moderate exercise as a treatment for the metabolic syndrome: a pilot study. Circulation 118:346–354
Ross R, Blair SN, Arena R et al (2016) Importance of assessing cardiorespiratory fitness in clinical practice: a case for fitness as a clinical vital sign: a scientific statement from the American Heart Association. Circulation 134:e653–e699
Adams SC, DeLorey DS, Davenport MH, Stickland MK, Fairey AS, North S, Szczotka A, Courneya KS (2017) Effects of high-intensity aerobic interval training on cardiovascualr disease risk in testicular cancer survivors: a phase 2 randomized controlled trial. Cancer 123:4057–4065
Toohey K, Pumpa KL, Arnolda L, Cooke J, Yip D, Craft PS, Semple S (2016) A pilot study examining the effects of low-volume high-intensity interval training and continuous low to moderate intensity training on quality of life, functional capacity and cardiovascular risk factors in cancer survivors. PeerJ 20(4):e2613
Vainshelboim B, Lima RM, Myers J (2019) Cardiorespiratory fitness and cancer in women: a prospective pilot study. J Sport Health Sci 8:457–462
Funding
This study was funded by the Department of Medicine, Departmental Grant, University of Otago.
Author information
Authors and Affiliations
Contributions
L.M.J., J.C.B., and R.B. contributed to the study conception and design. Data collection and analysis were performed by R.B., under the supervision of L.M.J. and J.C.B. J.C.B. wrote the first draft of the manuscript. L.M.J. and R.B. provided edits and all authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
All procedures performed in this study were in accordance with and approved by the University of Otago Human Ethics committee (Health, H18/029) and in accordance with the 1964 Helsinki Declaration.
Consent to participate
All participants provided informed written consent.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bell, R.A., Baldi, J.C. & Jones, L.M. Additional cardiovascular fitness when progressing from moderate- to high-intensity exercise training in previously trained breast cancer survivors. Support Care Cancer 29, 6645–6650 (2021). https://doi.org/10.1007/s00520-021-06259-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-021-06259-w