Abstract
Cancer-related fatigue (CRF) is one of the most prolonged discomforts suffered by people who have had cancer. Seventy-eight to ninety-six percent of cancer patients experience fatigue, especially while undergoing treatment. CRF is related to insomnia, anxiety, depression, and also varies depending on age. However, little is known about the factors contributing to CRF and better understanding of determinants of CRF makes it easier to identify early patients at risk and in designing intervention planning. The aim of this study was to assess the influence of precipitating factors (diagnosis of breast cancer and other clinical aspects) and perpetuating factors (social network, quality of life, mental disorders) on the presence of chronic fatigue in women from our cultural context, by social class each other determinants.
Methods
It was carried out a mixed cohort study (prospective and retrospective) using a convenience sample of women diagnosed with breast cancer. The information sources were data from the Brief Fatigue Inventory questionnaire and hospital medical records. The dependent variable was fatigue and the independent variables were age, social class, time since diagnoses, cohabitation, comorbidity, relapse, body mass index, mental health (anxiety and depression), social network, social support, and quality of life.
Results
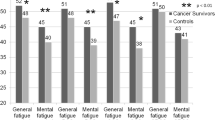
Seventy-two percent of the women in the DAMA cohort reported moderate to severe fatigue. Risk of suffering from severe fatigue was greatest among individuals with low social class, those aged under 50 years, those with chronic disorders who had relapsed, and those with symptoms of anxiety and depression. In our study, CRF did not appear to be related to the stage of the cancer at diagnosis, or to the time since diagnosis.
Conclusions
CRF is an element that the professionals responsible for the control and monitoring of women should take into account as another element to be taken into consideration.

Similar content being viewed by others
References
Berger AM, Mooney K, Alvarez-Pérez A, Breitbart WS, Carpenter KM, Cella D et al (2015) Cancer-related fatigue, versión 2.2015: clinical practice guidelines in oncology. J Natl Compr Cancer Netw 13(8):1012–1039
Lewis S, Salins N, Rao MR, Kadam A (2014) Spiritual well-being and its influence on fatigue in patients undergoing active cancer directed treatment: a correlation study. J Can Res Ther 10:676–680
Tavio M, Milan I, Tirello U (2002) Cancer-related fatigue (review). Int J Oncol 21:1093–1099
De Vries J, Van der Steeg AF, Roukema (2009) Determinants of fatigue 6 and 12 months after surgery in women with early-stage breast cáncer: a comparison with women with benign breast problems. J Psychosom Res 66:495–502
Reinersten KV, Engebraaten O, Loge JH, Cvancarova M, Naume B, Wist E, Edvarsen H, Wille E, Bjøro T, Kiserud CE (2017) Fatigue during and after breast cancer therapy. A prospective study. J Pain Symptom Manag 53(3):551–560
Hall DL, Mishel M, Germino BB (2014) Living with cáncer-related uncertainty: associations with fatigue, insomnia and affect in younger breast cáncer survivors. Support Care Cancer 22:2489–2495
Abrahams HJG, Gielissen MFM, Schmits IC, Verhagen CAHHVM, Rovers MM, Knoop H (2016) Risk factors, prevalence, anc ourse of severe fatigue after breast cáncer treatment: a meta-analysus involving 12327 breast cáncer survivors. Ann Oncol 27:965–974
Kumar NB, Fink A, Levis S, Su P, Tamura R, Krischer (2018) Thyroid function in the etiology of fatigue in breast cáncer. Oncotarget 9(39):25723–25737
Gjerset GM, Loge JH, Kiserud CE, Fosså SD, Gudbergsson SB, Oldervoll LM, Wisløff T, Thorsen L (2017) Perceived needs for different components in a rehabilitation program among cáncer survivors with chronic fatigue compared to survivors without chronic fatigue. Acta Oncol 56(2):245–253. https://doi.org/10.1080/0284186X.2016.1266091
Hall DL, Antoni MH, Lattie EG, Jutagir DR, Czaja SJ, Perdomo D, Lechner SC, Stagi JM, Bouchard LC, Gudenkauf LM, Traeger L, Fletcher MA, Klimas NG (2015) Perceived fatigue interference and depressed mood: comparison of chronic fatigue syndrome/myalgic encephalomyelitis patients with fatigued breast cancer survivors. Fatigue 3(3):142–155. https://doi.org/10.1080/21641846.2015.1039289
Crosswell AD, Lockwood KG, Ganz PA, Bower JE (2014) Low heart rate variability and cancer-related fatigue in breast cancer survivors. Psychoneuroendocrinology 45:58–66. https://doi.org/10.1016/j.psyneuen.2014.03.011
Wang XS, Woodruff JF (2015) Cancer-related and treatment-related fatigue. Gynecol Oncol 136:446–452. https://doi.org/10.1016/j.ygyno.2014.10.013
Abrahams HFG, Gielissen MFM, Goedenorp MM, Berends T, Peters MEWJ, Poort H, Verhagen CAHHVM, Knoop H (2015) A randomized controlled trial of web-based cognitive behavioral therapy for severely fatigued breast cancer survivors (CHANGE-study): study protocol. BMC Cancer 15:765. https://doi.org/10.1186/s12885-015-1787-7
Puigpinós-Riera R, Continente X, Serral G, Bargalló X, Doménech M, Espinosa-Bravo M, Grau J, Macià F, Manzanera R, Pla M, Quintant MJ, Sala M, Vidal E (2017) Influence of social determinants, lifestyle, emotional well-being and the use of unconventional therapies in breast cancer progression in a cohort of women in Barcelona: study protocol for the cohort DAMA. JMR Res Protoc 6(12):e249. http://www.researchprotocols.org2017/12/e249/
Mendoza TR, Wang XS, Cleeland CS, Morrissey M, Johnson BA, Wendt JK, Huber SL (1999) The rapid assessment of fatigue severity in cancer patients. CANCER 85(1):1186–1196
Domingo-Salvany A, Bacigalupe JM, Carrasco JM, Espelt A, Ferrando J, Borrell C, del Grupo de Determinantes Sociales de la Sociedad Española de Epidemiología (2013) Propuestas de clase social neoweberiana y neomarxista a partir de la Clasificación Nacional de Ocupaciones 2011. Gac Sanit 27(3):263–272
Schmidt ME, Chang-Claude J, Seibold P, Vrieling A, Heinz J, Flexch-Janys D, Steindorf K (2015) Determinants of long-term fatigue in breast cancer survivors: results of a prospective patient cohort study. Psycho-Oncology 24:40–46
Reinertsen KV, Cvancarova M, Loge JH, Edvardsen H, Wist E, Fossa SD (2010) Predictors and course of chronic fatigue in long-term breast cáncer survivors. J Cancer Surviv 4:405–414
Alvarez-Salgado F, Galiano-Castillo N, Arroyo-Morales M, Cruz-Fernández M, Lozano-Lozano M, Cantarero-Villanueva I (2018) Health status among long-term breast cancer survivors suffering from higher levels of fatigue: a cross-sectional study. Support Care Cancer 26:3649–3658. https://doi.org/10.1007/s00520-018-4240-z
Abrahams HJG, Gielissen MFM, Verhagen CAHHVM, Knoop H (2018) The relationship of fatigue in breast cáncer survivors with quality of life and factors to address in psychological interventions: a systematic review. Clin Psychol Rev 63:1–11
Schmidt ME, Chang-Claude J, Vrieling A, Heinz J, Flesch-Janis D, Steindorf K (2012) Fatigue and quality of life in breast cancer survivors: temporal courses and long-term pattern. J Cancer Surviv 6:11–19
Jones JM, Olson K, Catton P, Catton CN, Fleshner NE, Krzyzanowska MK, McCready DR, Wong RKS, Jiang H, Howell D (2016) Cancer-related fatigue and associated disability in post-treatment cáncer survivors. J Cancer Surv 10:51–61. https://doi.org/10.1007/s11764-015-0450-2
Frick MA, Vachani CC, Bach C, Hampshire MK, Arnold-Korzeniowski K, Metz JM, Hill-Kayser E (2017) Survivorship and the chronic cancer patient: patterns in treatment-related effects, follow-up care, and use of survivorship care plans. Cancer:4268–4276. https://doi.org/10.1002/cncr.30862
Veni T, Boyas S, Beaune B, Bourgeois H, Rahmani A, Landry S, Bochereau A, Durand S, Morel B (2018) Handgrip fatiguing exercise can provide objective assessment of cancer-related fatigue: a pilot study. Support Care Cancer. https://doi.org/10.1007/s00520-018-4321-0
Baumann FT, Bieck O, Pberste M, Kuhn R, Schmitt J, Wentrock S, Zopf E, Bloch W, Schüle K, Reuss-Borst M (2017) Sustainable impact of an individualized exercise program on physical activity level and fatigue syndrome on breast cancer patients in two German rehabilitation centers. Support Care Cancer 25:1047–1054. https://doi.org/10.1007/s00520-016-3491-x
Hagstrom AD, Marshall PWM, Lonsdale C, Cheema BS, Fiatarone Singh MA, Green S (2016) Resistance training improves fatigue and quality of life in previously sedentary breast cancer survivors: a randomised controlled trial. Eur J Cancer Care 25:784–794. https://doi.org/10.1111/ecc.12422
Meneses-Echávez JF, González-Jiménez E, Ramírez-Vélez R (2015) Effects of supervised exercise on cáncer related fatigue in breast cáncer survivors: a systematic review and meta-analysis. BMC Cancer 15:77. https://doi.org/10.1186/s12885-015-1069-4
Carter SJ, Hunter GR, McAuley E, Courneya KS, Anton PM, Rogers LQ (2016) Lower rate-pressure product during submaximal walking: a link to fatigue improvement following a physical activity intervention among breast cancer survivors. J Cancer Surviv 10(5):927–934. https://doi.org/10.1007/s11764-016-0539-2
Gielissen MFM, Verhagen S, Witjes F, Bleijenberg G (2006) Effects of cognitive behaviour therapy in severely fatigued disease-free cancer patients compared with patients waiting for cognitive behaviour therapy: a randomized controlled trial. J Clin Oncol 24(30):4882–4887. https://doi.org/10.1200/JCO.2006.06.8270
Abrahams HJG, Gielissen MFM, Donders RRT, Goedendorp MM, van der Wouw AJ, Verhagen CHHVM, Knoop H (2017) The efficacy on internet-based cognitive behavioural therapy for severely fatigued survivors of breast cancer compared with care as usual: a randomized controlled trial. CANCER:3825–3834. https://doi.org/10.1002/cnr.30815
Berntsen S, Aaronson NK, Buffart L, Börjeson S, Demmelmaier I, Hellbom M, Hojman P, Igelström H, Johansson B, Pingel R, Raastad T, Velikova G, Åsenlöf P, Nordin K (2017) Design of a randomized controlled trial of physical training and cancer (Phys-Can)- the impact of exercise intensity on cancer related fatigue, quality of life and disease outcome. BMC Cancer 17:218. https://doi.org/10.1186/s12885-017-3197-5
Kröz M, Reif M, Glinz A, Berger B, Nikolaou A, Zerm R, Brinkhaus B, Girke M, Büssing A, Gutenbrunner C, and On behalf of the CRF study group (2017) Impact of a combined multimodal-aerobic and multimodal intervention compared to standard aerobic treatment in breast cancer survivors with chronic cancer-related fatigue–results of a three-armed pragmatic trial in a comprehensive cohort design. BMC Cancer 17:166. https://doi.org/10.1186/s12885-017-3142-7
Stan DL, Croghan KA, Croghan IT, Jenkins SM, Sutherland SJ, Cheville AL, Pruthi S (2016) Randomized pilot trial of yoga versus strengthening exercises in breast cancer survivors with cancer-related fatigue. Support Care Cancer 24:4005–4015. https://doi.org/10.1007/s00520-016-3233-z
Larkey L, Huberty J, Pedersen M, Weihs K (2016) Qigons/tai chi easy for fatigue in breast cancer survivors: rationale and design of a randomized clinical trial. Contemp Clin Trials 50:222–228 https://doi.org/10.1016/j.cct.2016.08.002
Grégoire C, Bragard I, Jerusalem G, Etienne AM, Coucke P, Dupuis G, Lanctôt D, Faymonville ME (2017) Group interventions to reduce emotional distress and fatigue in breast cancer patients: a 9-month follow-up pragmatic trial. Br J Cancer 117:1442–1449. https://doi.org/10.1038/bjc.2017.326
Johns SA, Brown LF, Beck-Coon K, Talib TL, Monahan PO, Giesler RB, Tong Y, Willhelm L, Carpenter JS, Von Ah D, Wagner CD, de Groot M, Schmidt K, Miller KD, Kroenke K (2016) Randomized controlled pilot trial of mindfulness-based stress reduction compared to psychoeducational support for persistently fatigued breast and colorectal cancer survivors. Support Care Cancer 24(10):4085–4096. https://doi.org/10.1007/s00520-016-3220-4
Zick SM, Colacino J, Cornellier M, Khabir T, Surnow K, Djuric Z (2017) Fatigue reduction diet in breast cancer survivors: a pilot randomized clinical trial. Breast Cancer Res 161(2):299–310. https://doi.org/10.1007/s10549-016-4070-y
Funding
This project was funded by the Fondo de Investigación Sanitaria, Instituto de Salud Carlos III, with register number PI13/01977.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Confidentiality and anonymity of the data was ensured, in compliance with Spanish Law 15/1999 on data confidentiality.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was approved by the Parc de Salut MAR Clinical Research Ethics Committee. register number 2015/6499/I.
Informed consent
Informed consent was obtained from all participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Puigpinós-Riera, R., Serral, G., Sala, M. et al. Cancer-related fatigue and its determinants in a cohort of women with breast cancer: the DAMA Cohort. Support Care Cancer 28, 5213–5221 (2020). https://doi.org/10.1007/s00520-020-05337-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-020-05337-9