Summary
Objective
Obstructive sleep apnea (OSA) is a common medical problem with numerous comorbidities and high costs. Since the introduction of the Epworth sleepiness scale (ESS), excessive daytime sleepiness (EDS) has been considered the most common and prominent symptom of OSA. Aim of this study was to re-evaluate the ESS for detection of OSA in a population at risk compared to the gold standard overnight polysomnography (PSG).
Methods
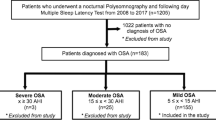
A total of 266 patients (mean age 57.9 ± 11.6 years; 189 men and 77 women), referred to our sleep laboratory for probable OSA, were given ESS followed by an overnight PSG. The ESS values were compared to PSG apnea hypopnea index (AHI) with sensitivity (SE), specificity (SP), positive predictive value (PPV), negative predictive value (NPV) and diagnostic accuracy (DA) calculated for ESS. The positive cut-off value for ESS was ≥ 10 and for AHI ≥ 5.
Results
Only 92 (34.6%) subjects had a positive ESS. An OSA was diagnosed by PSG in 213 (80.1%) subjects: 46 having mild, 37 moderate and 130 severe apnea. Most subjects with positive ESS (88.0%) were found to have OSA but most subjects with a negative ESS (75.9%) were also positive for OSA (42% with AHI ≥ 30). The area under the receiver operating characteristic (ROC) curve for ESS was 0.60 (95% confidence interval, CI 0.54–0.66; p = 0.020) with SE 38.0%, SP 79.3%, PPV 88.0%, NPV 24.1% and DA 46.2%.
Conclusion
It was found that excessive daytime sleepiness, measured by ESS, is not a valuable screening tool for OSA, especially when the test is negative. Other screening tests that involve additional parameters, beside daytime sleepiness alone, should be considered.


Similar content being viewed by others
References
American Academy of Sleep Medicine. International classification of sleep disorders. 2nd ed. Diagnostic and coding manual. Westchester, IL: American Academy of Sleep Medicine; 2005.
Schreier DR, Banks C, Mathis J. Driving simulators in the clinical assessment of fitness to drive in sleepy individuals: a systematic review. Sleep Med Rev. 2018;38:86–100. https://doi.org/10.1016/j.smrv.2017.04.004.
Sangal RB, Thomas L, Mitler MM. Disorders of excessive sleepiness. Treatment improves ability to stay awake but does not reduce sleepiness. Chest. 1992;102(3):699–703. https://doi.org/10.1378/chest.102.3.699.
Stepanski E, Zorick F, Roehrs T, Young D, Roth T. Daytime alertness in patients with chronic insomnia compared with asymptomatic control subjects. Sleep. 1988;11(1):54–60. https://doi.org/10.1093/sleep/11.1.54.
Léger D, Stepnowsky C. The economic and societal burden of excessive daytime sleepiness in patients with obstructive sleep apnea. Sleep Med Rev. 2020;51:101275. https://doi.org/10.1016/j.smrv.2020.101275.
Markowitz AJ, Rabow MW. Palliative management of fatigue at the close of life: “it feels like my body is just worn out”. JAMA. 2007;298(2):217. https://doi.org/10.1001/jama.298.2.217.
Young TB. Epidemiology of daytime sleepiness: definitions, symptomatology, and prevalence. J Clin Psychiatry. 2004;65(16):12–6.
Chervin RD. Sleepiness, fatigue, tiredness, and lack of energy in obstructive sleep apnea. Chest. 2000;118(2):372–9. https://doi.org/10.1378/chest.118.2.372.
Patel SR, White DP, Malhotra A, Stanchina ML, Ayas NT. Continuous positive airway pressure therapy for treating sleepiness in a diverse population with obstructive sleep apnea: results of a meta-analysis. Arch Intern Med. 2003;163(5):565–71. https://doi.org/10.1001/archinte.163.5.565.
Dempsey JA, Veasey SC, Morgan BJ, O’Donnell CP. Pathophysiology of sleep apnea. Physiol Rev. 2010;90(1):47–112. https://doi.org/10.1152/physrev.00043.2008. Erratum in: Physiol Rev.2010;90(2):797–8.
Chervin RD. Use of clinical tools and tests in sleep medicine. In: Kryger MH, Roth T, Dement WC, editors. Principles and practice of sleep medicine. St Louis: Elsevier Saunders; 2011. p. 666.
Littner MR, Kushida C, Wise M, et al. Standards of practice committee of the American academy of sleep medicine. Practice parameters for clinical use of the multiple sleep latency test and the maintenance of wakefulness test. Sleep. 2005;28(1):113–21. https://doi.org/10.1093/sleep/28.1.113.
Kushida CA, Littner MR, Morgenthaler T, et al. Practice parameters for the indications for polysomnography and related procedures: an update for 2005. Sleep. 2005;28(4):499–521. https://doi.org/10.1093/sleep/28.4.499.
Iber C, Ancoli-Israel S, Chesson AL Jr., Quan SF. The AASM manual for the scoring of sleep and associated events: rules, terminology, and technical specification. Westchester, IL: American Academy of Sleep Medicine; 2007.
Berry RB, Budhiraja R, Gottlieb DJ, American Academy of Sleep Medicine, et al. Rules for scoring respiratory events in sleep: update of the 2007 AASM manual for the scoring of sleep and associated events. Deliberations of the sleep apnea definitions task force of the American academy of sleep medicine. J Clin Sleep Med. 2012;8(5):597–619. https://doi.org/10.5664/jcsm.2172.
Johns MW. A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep. 1991;14(6):540–5. https://doi.org/10.1093/sleep/14.6.540.
Johns MW. Daytime sleepiness, snoring, and obstructive sleep apnea. The Epworth sleepiness scale. Chest. 1993;103(1):30–6. https://doi.org/10.1378/chest.103.1.30.
Johns M. Rethinking the assessment of sleepiness. Sleep Med Rev. 1998;2(1):3–15. https://doi.org/10.1016/s1087-0792(98)90050-8.
Smolley LA, Ivey C, Farkas M, Faucette E, Murphy S. Epworth sleepiness scale is useful for monitoring daytime sleepiness. J Sleep Res. 1993;22:389.
Manni R, Politini L, Ratti MT, Tartara A. Sleepiness in obstructive sleep apnea syndrome and simple snoring evaluated by the Epworth sleepiness scale. J Sleep Res. 1999;8(4):319–20. https://doi.org/10.1046/j.1365-2869.1999.00166.x.
Kendzerska TB, Smith PM, Brignardello-Petersen R, Leung RS, Tomlinson GA. Evaluation of the measurement properties of the Epworth sleepiness scale: a systematic review. Sleep Med Rev. 2014;18(4):321–31. https://doi.org/10.1016/j.smrv.2013.08.002.
Kapur VK, Baldwin CM, Resnick HE, Gottlieb DJ, Nieto FJ. Sleepiness in patients with moderate to severe sleep-disordered breathing. Sleep. 2005;28(4):472–7. https://doi.org/10.1093/sleep/28.4.472.
El-Sayed IH. Comparison of four sleep questionnaires for screening obstructive sleep apnea. Egypt J Chest Dis Tuberc. 2012;61(4):433–41.
Silva GE, Vana KD, Goodwin JL, Sherrill DL, Quan SF. Identification of patients with sleep disordered breathing: comparing the four-variable screening tool, STOP, STOP-bang, and Epworth sleepiness scales. J Clin Sleep Med. 2011;7(5):467–72. https://doi.org/10.5664/JCSM.1308.
Pecotic R, Dodig IP, Valic M, Ivkovic N, Dogas Z. The evaluation of the Croatian version of the Epworth sleepiness scale and STOP questionnaire as screening tools for obstructive sleep apnea syndrome. Sleep Breath. 2012;16(3):793–802. https://doi.org/10.1007/s11325-011-0578-x.
Mazzotti DR, Keenan BT, Thorarinsdottir EH, Gislason T, Pack AI, Sleep Apnea Global Interdisciplinary Consortium. Is the Epworth sleepiness scale sufficient to identify the excessively sleepy subtype of OSA? Chest. 2022;161(2):557–61. https://doi.org/10.1016/j.chest.2021.10.027.
Basille D, Baud ME, Andrejak C, Basille-Fantinato A, Jounieaux V. Correlation between the Epworth sleepiness scale and the maintenance of wakefulness test in obstructive sleep apnea patients treated with positive airway pressure. Respir Med Res. 2020;78:100787. https://doi.org/10.1016/j.resmer.2020.100787.
Young T, Finn L, Peppard PE, et al. Sleep disordered breathing and mortality: eighteen-year follow-up of the Wisconsin sleep cohort. Sleep. 2008;31(8):1071–8.
Gami AS, Olson EJ, Shen WK, et al. Obstructive sleep apnea and the risk of sudden cardiac death: a longitudinal study of 10,701 adults. J Am Coll Cardiol. 2013;62(7):610–6. https://doi.org/10.1016/j.jacc.2013.04.080.
Marshall NS, Wong KK, Liu PY, Cullen SR, Knuiman MW, Grunstein RR. Sleep apnea as an independent risk factor for all-cause mortality: the Busselton health study. Sleep. 2008;31(8):1079–85.
Marin JM, Agusti A, Villar I, et al. Association between treated and untreated obstructive sleep apnea and risk of hypertension. JAMA. 2012;307(20):2169–76. https://doi.org/10.1001/jama.2012.3418.
Shahar E, Whitney CW, Redline S, et al. Sleep-disordered breathing and cardiovascular disease: cross-sectional results of the sleep heart health study. Am J Respir Crit Care Med. 2001; https://doi.org/10.1164/ajrccm.163.1.2001008.
Barbé PJ, Muñoz A, Findley L, Antó JM, Agustí AG. Automobile accidents in patients with sleep apnea syndrome. An epidemiological and mechanistic study. Am J Respir Crit Care Med. 1998;158(1):18–22. https://doi.org/10.1164/ajrccm.158.1.9709135.
Finkel KJ, Searleman AC, Tymkew H, et al. Prevalence of undiagnosed obstructive sleep apnea among adult surgical patients in an academic medical center. Sleep Med. 2009;10(7):753–8. https://doi.org/10.1016/j.sleep.2008.08.007.
Kapur V, Strohl KP, Redline S, Iber C, O’Connor G, Nieto J. Underdiagnosis of sleep apnea syndrome in U.S. communities. Sleep Breath. 2002;6(2):49–54. https://doi.org/10.1007/s11325-002-0049-5.
Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, Hla KM. Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol. 2013;177(9):1006–14. https://doi.org/10.1093/aje/kws342.
Kribbs N, Getsy J, Dinges D. Investigation and management of daytime sleepiness in sleep apnea. In: Saunders N, Sullivan C, editors. Sleeping and Breathing. New York: Marcel Dekker; 1993. p. 575.
Netzer NC, Stoohs RA, Netzer CM, Clark K, Strohl KP. Using the Berlin questionnaire to identify patients at risk for the sleep apnea syndrome. Ann Intern Med. 1999;131(7):485–91. https://doi.org/10.7326/0003-4819-131-7-199910050-00002.
Chung F, Yegneswaran B, Liao P, et al. STOP questionnaire: a tool to screen patients for obstructive sleep apnea. Anesthesiology. 2008;108(5):812–21. https://doi.org/10.1097/ALN.0b013e31816d83e4.
Chung F, Subramanyam R, Liao P, Sasaki E, Shapiro C, Sun Y. High STOP-Bang score indicates a high probability of obstructive sleep apnoea. Br J Anaesth. 2012;108(5):768–75. https://doi.org/10.1093/bja/aes022.
Johns M, Hocking B. Daytime sleepiness and sleep habits of Australian workers. Sleep. 1997;20(10):844–9. https://doi.org/10.1093/sleep/20.10.844.
Hara C, Lopes Rocha F, Lima-Costa MF. Prevalence of excessive daytime sleepiness and associated factors in a Brazilian community: the Bambuí study. Sleep Med. 2004;5(1):31–6. https://doi.org/10.1016/j.sleep.2003.09.009.
Johns MW. Sleep propensity varies with behaviour and the situation in which it is measured: the concept of somnificity. J Sleep Res. 2002;11(1):61–7. https://doi.org/10.1046/j.1365-2869.2002.00274.x.
Johns MW. Sleepiness in different situations measured by the Epworth sleepiness scale. Sleep. 1994;17(8):703–10. https://doi.org/10.1093/sleep/17.8.703.
Baldwin CM, Kapur VK, Holberg CJ, Rosen C, Nieto FJ, Sleep Heart Health Study Group. Associations between gender and measures of daytime somnolence in the sleep heart health study. Sleep. 2004;27(2):305–11. https://doi.org/10.1093/sleep/27.2.305.
Theorell-Haglöw J, Åkerstedt T, Schwarz J, Lindberg E. Predictors for development of excessive daytime sleepiness in women: a population-based 10-year follow-up. Sleep. 2015;38(12):1995–2003. https://doi.org/10.5665/sleep.5258.
Lok R, Zeitzer JM. Physiological correlates of the Epworth sleepiness scale reveal different dimensions of daytime sleepiness. Sleep Adv. 2021;2(1):zpab8. https://doi.org/10.1093/sleepadvances/zpab008.
Mazzotti DR, Keenan BT, Lim DC, Gottlieb DJ, Kim J, Pack AI. Symptom subtypes of obstructive sleep apnea predict incidence of cardiovascular outcomes. Am J Respir Crit Care Med. 2019;200(4):493–506. https://doi.org/10.1164/rccm.201808-1509OC.
Société de Pneumologie de Langue Française, Société Française d’Anesthésie Réanimation, Société Française de Cardiologie, Société Française de Médecine du Travail, Société Française d’ORL, Société de Physiologie, Société Française de Recherche et de Médecine du Sommeil. Recommandations pour la pratique clinique syndrome d’apnées hypopnées obstructives du sommeil de l’adulte. Rev Mal Respir. 2010;27(7):806–33. https://doi.org/10.1016/j.rmr.2010.05.011.
Abrishami A, Khajehdehi A, Chung F. A systematic review of screening questionnaires for obstructive sleep apnea. Can J Anaesth. 2010;57(5):423–38. https://doi.org/10.1007/s12630-010-9280-x.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
H. Puretić, M. Bosnar Puretić, G. Pavliša and M. Jakopović declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Puretić, H., Bosnar Puretić, M., Pavliša, G. et al. Revisiting the Epworth sleepiness scale. Wien Klin Wochenschr (2023). https://doi.org/10.1007/s00508-023-02213-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00508-023-02213-4