Summary
Background and aim
Sarcoidosis is a multisystem disease of unknown origin. Determining the involvement and the response to the treatment is important. The aim of this study was to identify the effects of methylprednisolone and indomethacine on metabolic activity and pulmonary function test parameters in patients with sarcoidosis.
Material and methods
A total of 24 pulmonary sarcoidosis patients were enrolled in the study. All the patients underwent spirometry and [18F]fluorodeoxyglucose positron emission tomography–computed tomography (FDG PET-CT) scan before treatment and were divided into two groups according to the necessity of corticosteroid treatment or not. Patients who did not have corticosteroid indication were treated with indomethacine. Symptomatic patients and patients who did not respond to indomethacine treatment received methylprednisolone. Patients were followed up on a monthly basis to determine the response. FDG uptakes as the disease activity were re-evaluated before ending the treatment at the sixth month.
Results
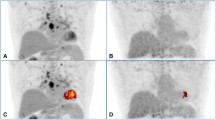
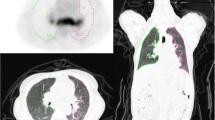
Mean age of patients (16 male, 8 female) was 39.79 (9.3) years. Besides mediastinum and pulmonary parenchyma, extrapulmonary sites were also involved in patients with pulmonary sarcoidosis (distant lymph nodes (upper abdominal, supraclavicular, inguinal, and axillary), liver, and spleen). Although maximum standard uptake values of methylprednisolone group regressed significantly (p < 0.001) after treatment, indomethacine group did not have significant regression (p = 0.345). Despite metabolic regressions, spirometry values of patients did not significantly increase (p > 0.005).
Conclusion
FDG PET-CT may be useful for determining activity and the efficacy of treatments. Methylprednisolone is effective in reducing metabolic activity but does not lead to improvement in functional parameters.
Zusammenfassung
Hintergrund und Ziel
Die Sarkoidose ist eine Multisystemerkrankung unbekannten Ursprungs. Die Bestimmung des Ausmaßes der Erkrankung und des Ansprechen auf Therapie ist wichtig. Das Ziel dieser Studie war es, die Wirkung von Methylprednisolon und Indomethacin auf die Stoffwechselaktivität und auf Lungenfunktionsparameter bei Patienten mit Sarkoidose zu erfassen.
Material und Methoden
Es wurden 24 Patienten mit Sarkoidose in die Studie aufgenommen. Bei allen Patienten wurde eine Spirometrie und ein FDG PET-CT vor der Therapie durchgeführt. Die Patienten wurden in zwei Gruppen je nach der Notwendigkeit einer Cortisontherapie geteilt. Die Patienten, bei denen keine Indikation für eine Cortisontherapie bestand, wurden mit Indomethacin behandelt. Patienten mit Symptomen und Patienten, die nicht auf die Indomethacin-Therapie ansprachen, erhielten Cortison. Die Patienten wurden zur Erfassung des Ansprechens auf die Therapie monatlich kontrolliert. Als Parameter der Aktivität der Erkrankung wurden FDG-Uptakes vor Ende der 6-monatigen Therapie neuerlich erhoben.
Ergebnisse
Das mittlere Alter der Patienten (16 Männer, 8 Frauen) lag bei 39,79 (9,3) Jahren. Neben dem Mediastinum und Lungenparenchym waren auch extrapulmonale Organe befallen (Lymphknoten im Bereich des oberen Abdomens, der Supraclaviculargruben, der Leisten und der Axillae; Leber und Milz). Obwohl die SUV max Werte in der Gruppe mit Methylprednisolon signifikant (p < 0,001) nach der Behandlung abfielen, blieben die Werte der Gruppe mit Indomethacin unverändert (p = 0,345). Trotz des Abfalls in der Stoffwechselaktivität kam es zu keiner Besserung der Spirometriewerte.
Schlussfolgerung
FDG PET-CT kann zur Erfassung der Aktivität der Sarkoidose und der Wirksamkeit einer Behandlung nützlich sein. Methylprednisolon ist wirksam im Bezug auf eine Reduktion der Stoffwechselaktivität, führt aber nicht zu einer Besserung der Lungenfunktionsparameter.






Similar content being viewed by others
References
Statement on sarcoidosis. Joint Statement of the American Thoracic Society (ATS), the European Respiratory Society (ERS) and the World Association of Sarcoidosis and Other Granulomatous Disorders (WASOG) adopted by the ATS Board of Directors and by the ERS Executive Committee, February 1999. Am J Respir Crit Care Med. 1999;160(2):736–55.
Beaumont D, Herry JY, Sapene M, Bourguet P, Larzul JJ, de Labarthe B. Gallium-67 in the evaluation of sarcoidosis: correlations with serum angiotensin-converting enzyme and bronchoalveolar lavage. Thorax. 1982;37(1):11–8.
Israel HL, Albertine KH, Park CH, Patrick H. Whole-body gallium 67 scans. Role in diagnosis of sarcoidosis. Am Rev Respir Dis. 1991;144(5):1182–6.
Klech H, Kohn H, Kummer F, Mostbeck A. Assessment of activity in sarcoidosis. Sensitivity and specificity of 67Gallium scintigraphy, serum ACE levels, chest roentgenography, and blood lymphocyte subpopulations. Chest. 1982;82(6):732–8.
Line BR, Hunninghake GW, Keogh BA, Jones AE, Johnston GS, Crystal RG. Gallium-67 scanning to stage the alveolitis of sarcoidosis: correlation with clinical studies, pulmonary function studies, and bronchoalveolar lavage. Am Rev Respir Dis. 1981;123(4 Pt. 1):440–6.
Niden AH, Mishkin FS, Salem F, Thomas AV, Jr., Kamdar V. Prognostic significance of gallium lung scans in sarcoidosis. Ann N Y Acad Sci. 1986;465:435–43.
Nosal A, Schleissner LA, Mishkin FS, Lieberman J. Angiotensin-I-converting enzyme and gallium scan in noninvasive evaluation of sarcoidosis. Ann Intern Med. 1979;90(3):328–31.
Braun JJ, Kessler R, Constantinesco A, Imperiale A. 18F-FDG PET/CT in sarcoidosis management: review and report of 20 cases. Eur J Nucl Med Mol Imaging. 2008;35(8):1537–43.
Glaudemans AW, de Vries EF, Galli F, Dierckx RA, Slart RH, Signore A. The use of (18)F-FDG-PET/CT for diagnosis and treatment monitoring of inflammatory and infectious diseases. Clin Dev Immunol. 2013;2013:623036.
Morgenthau AS, Iannuzzi MC. Recent advances in sarcoidosis. Chest. 2011;139(1):174–82.
Gottlieb JE, Israel HL, Steiner RM, Triolo J, Patrick H. Outcome in sarcoidosis. The relationship of relapse to corticosteroid therapy. Chest. 1997;111(3):623–31.
Baughman RP, Lower EE. Treatment of sarcoidosis with corticosteroids: who is going to relapse and why? Sarcoidosis Vasc Diffuse Lung Dis. 1998;15(1):19–20.
Hunninghake GW, Gilbert S, Pueringer R, Dayton C, Floerchinger C, Helmers R, et al. Outcome of the treatment for sarcoidosis. Am J Respir Crit Care Med. 1994;149(4 Pt. 1):893–8.
Baughman RP, Nunes H, Sweiss NJ, Lower EE. Established and experimental medical therapy of pulmonary sarcoidosis. Eur Respir J. 2013;41(6):1424–38.
Cottin V, Muller-Quernheim J. Sarcoidosis from bench to bedside: a state-of-the-art series for the clinician. Eur Respir J. 2012;40(1):14–6.
Tabak L. Sarkoidoz olgularında uzun dönem izlem sonuçları. Solunum. 2001;3:86–90.
Zabel P, Entzian P, Dalhoff K, Schlaak M. Pentoxifylline in treatment of sarcoidosis. Am J Respir Crit Care Med. 1997;155(5):1665–9.
Türktaş H, Oğuzülgen İ, Gürsel G. Effects of pentoxifylline and methylprednisolone combined therapy on sarcoidosis. Turkish Respir J. 2000;1:15–20.
James DG, Carstairs LS, Trowell J, Sharma OP. Treatment of sarcoidosis. Report of a controlled therapeutic trial. Lancet. 1967;2(7515):526–8.
Milman N, Mortensen J, Sloth C. Fluorodeoxyglucose PET scan in pulmonary sarcoidosis during treatment with inhaled and oral corticosteroids. Respiration. 2003;70(4):408–13.
Kaira K, Ishizuka T, Yanagitani N, Sunaga N, Hisada T, Mori M. Value of FDG positron emission tomography in monitoring the effects of therapy in progressive pulmonary sarcoidosis. Clin Nucl Med. 2007;32(2):114–6.
Teirstein AS, Machac J, Almeida O, Lu P, Padilla ML, Iannuzzi MC. Results of 188 whole-body fluorodeoxyglucose positron emission tomography scans in 137 patients with sarcoidosis. Chest. 2007;132(6):1949–53.
Brudin LH, Valind SO, Rhodes CG, Pantin CF, Sweatman M, Jones T, et al. Fluorine-18 deoxyglucose uptake in sarcoidosis measured with positron emission tomography. Eur J Nucl Med. 1994;21(4):297–305.
Miller MR, Crapo R, Hankinson J, Brusasco V, Burgos F, Casaburi R, et al. General considerations for lung function testing. Eur Respir J. 2005;26(1):153–61.
Acknowledgments
The English in this document has been checked by at least two professional editors, both native speakers of English. For a certificate, please see: http://www.textcheck.com/certificate/DxY8pE.
Conflict of interest
None of the authors declares any conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yakar, A., Yakar, F., Sezer, M. et al. Use of PET-CT for the assessment of treatment results in patients with sarcoidosis. Wien Klin Wochenschr 127, 274–282 (2015). https://doi.org/10.1007/s00508-014-0647-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00508-014-0647-9