Abstract
Background
The objective of this study was to explore the frequency of occurrence of extra-renal manifestations associated with monogenic nephrolithiasis.
Methods
A literature review was conducted to identify genes that are monogenic causes of nephrolithiasis. The Online Mendelian Inheritance in Man (OMIM) database was used to identify associated diseases and their properties. Disease phenotypes were ascertained using OMIM clinical synopses and sorted into 24 different phenotype categories as classified in OMIM. Disease phenotypes caused by the same gene were merged into a phenotypic profile of a gene (PPG) such that one PPG encompasses all related disease phenotypes for a specific gene. The total number of PPGs involving each phenotype category was measured, and the median phenotype category was determined. Phenotype categories were classified as overrepresented or underrepresented if the number of PPGs involving them was higher or lower than the median, respectively. Chi-square test was conducted to determine whether the number of PPGs affecting a given category significantly deviated from the median.
Results
Fifty-five genes were identified as monogenic causes of nephrolithiasis. A total of six significantly overrepresented and three significantly underrepresented phenotype categories were identified (p < 0.05). Four phenotypic categories (growth, neurological, skeletal, and abdomen/gastrointestinal) are significantly overrepresented after Bonferroni correction for multiple comparisons (p < 0.002). Among all phenotypes, impaired growth is the most common manifestation.
Conclusion
Recognizing the extra-renal manifestations associated with monogenic causes of kidney stones is critical for earlier diagnosis and optimal care in patients.
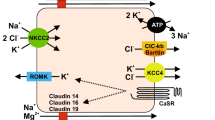
Graphical abstract

A higher resolution version of the Graphical abstract is available as Supplementary information


Similar content being viewed by others
Data availability
The datasets analyzed during the current study is available at OMIM (https://www.omim.org/search/advanced/clinicalSynopsis) and the Human Protein Atlas database (https://www.proteinatlas.org/).
References
Alelign T, Petros B (2018) Kidney stone disease: an update on current concepts. Adv Urol 2018:3068365. https://doi.org/10.1155/2018/3068365
Scales CD, Smith AC, Hanley JM, Saigal CS (2012) Prevalence of kidney stones in the United States. Eur Urol 62:160–165. https://doi.org/10.1016/j.eururo.2012.03.052
Tundo G, Vollstedt A, Meeks W, Pais V (2021) Beyond prevalence: annual cumulative incidence of kidney stones in the United States. J Urol 205:1704–1709. https://doi.org/10.1097/JU.0000000000001629
Dwyer ME, Krambeck AE, Bergstralh EJ et al (2012) Temporal trends in incidence of kidney stones among children: a 25-year population based study. J Urol 188:247–252. https://doi.org/10.1016/j.juro.2012.03.021
Ward JB, Feinstein L, Pierce C et al (2019) Pediatric urinary stone disease in the United States: the urologic diseases in America project. Urology 129:180–187. https://doi.org/10.1016/j.urology.2019.04.012
Moe OW (2006) Kidney stones: pathophysiology and medical management. Lancet 367:333–344. https://doi.org/10.1016/S0140-6736(06)68071-9
Goldfarb DS, Avery AR, Beara-Lasic L et al (2018) A twin study of genetic influences on nephrolithiasis in women and men. Kidney Int Rep 4:535–540. https://doi.org/10.1016/j.ekir.2018.11.017
Lieske JC, Wang X (2019) Heritable traits that contribute to nephrolithiasis. Urolithiasis 47:5–10. https://doi.org/10.1007/s00240-018-1095-1
Howles SA, Thakker RV (2020) Genetics of kidney stone disease. Nat Rev Urol 17:407–421. https://doi.org/10.1038/s41585-020-0332-x
Daga A, Majmundar AJ, Braun DA et al (2018) Whole exome sequencing frequently detects a monogenic cause in early onset nephrolithiasis and nephrocalcinosis. Kidney Int 93:204–213. https://doi.org/10.1016/j.kint.2017.06.025
Huang L, Qi C, Zhu G et al (2022) Genetic testing enables a precision medicine approach for nephrolithiasis and nephrocalcinosis in pediatrics: a single-center cohort. Mol Genet Genomics 297:1049–1061. https://doi.org/10.1007/s00438-022-01897-z
Schwaderer AL, Kusumi K, Ayoob RM (2014) Pediatric nephrolithiasis and the link to bone metabolism. Curr Opin Pediatr 26:207–214. https://doi.org/10.1097/MOP.0000000000000069
Ferraro PM, Bargagli M, Trinchieri A, Gambaro G (2020) Risk of kidney stones: influence of dietary factors, dietary patterns, and vegetarian-vegan diets. Nutrients 12:E779. https://doi.org/10.3390/nu12030779
Alexander RT, Hemmelgarn BR, Wiebe N et al (2012) Kidney stones and kidney function loss: a cohort study. BMJ 345:e5287. https://doi.org/10.1136/bmj.e5287
Amberger JS, Bocchini CA, Schiettecatte F et al (2015) OMIM.org: Online Mendelian Inheritance in Man (OMIM®), an online catalog of human genes and genetic disorders. Nucleic Acids Res 43:D789-798. https://doi.org/10.1093/nar/gku1205
Vasudevan V, Samson P, Smith AD, Okeke Z (2017) The genetic framework for development of nephrolithiasis. Asian J Urol 4:18–26. https://doi.org/10.1016/j.ajur.2016.11.003
Bhojani N, Bjazevic J, Wallace B et al (2022) UPDATE – Canadian Urological Association guideline: evaluation and medical management of kidney stones. Can Urol Assoc J 16:175–188. https://doi.org/10.5489/cuaj.7872
Maalouf NM, Tondapu P, Guth ES et al (2010) Hypocitraturia and hyperoxaluria after Roux-en-Y gastric bypass surgery. J Urol 183:1026–1030. https://doi.org/10.1016/j.juro.2009.11.022
Curhan GC, Willett WC, Rimm EB, Stampfer MJ (1997) Family history and risk of kidney stones. J Am Soc Nephrol 8:1568–1573. https://doi.org/10.1681/ASN.V8101568
Jungers P, Joly D, Blanchard A et al (2008) Inherited monogenic kidney stone diseases: recent diagnostic and therapeutic advances. Nephrol Ther 4:231–255. https://doi.org/10.1016/j.nephro.2007.12.005
Ferraro PM, Taylor EN, Eisner BH et al (2013) History of kidney stones and the risk of coronary heart disease. JAMA 310:408–415. https://doi.org/10.1001/jama.2013.8780
Jaeger P, Lippuner K, Casez JP et al (1994) Low bone mass in idiopathic renal stone formers: magnitude and significance. J Bone Miner Res 9:1525–1532. https://doi.org/10.1002/jbmr.5650091004
Krieger NS, Bushinsky DA (2013) The relation between bone and stone formation. Calcif Tissue Int 93:374–381. https://doi.org/10.1007/s00223-012-9686-2
Pietschmann F, Breslau NA, Pak CY (1992) Reduced vertebral bone density in hypercalciuric nephrolithiasis. J Bone Miner Res 7:1383–1388. https://doi.org/10.1002/jbmr.5650071205
Sella S, Cattelan C, Realdi G, Giannini S (2008) Bone disease in primary hypercalciuria. Clin Cases Miner Bone Metab 5:118–126
Schott C, Pourtousi A, Connaughton DM (2022) Monogenic causation of pediatric nephrolithiasis. Front Urol 2:1075711. https://doi.org/10.3389/fruro.2022.1075711
Bhowmick SS, Lang AE (2020) Movement disorders and renal diseases. Mov Disord Clin Pract 7:763–779. https://doi.org/10.1002/mdc3.13005
Attree O, Olivos IM, Okabe I et al (1992) The Lowe’s oculocerebrorenal syndrome gene encodes a protein highly homologous to inositol polyphosphate-5-phosphatase. Nature 358:239–242. https://doi.org/10.1038/358239a0
Romani M, Micalizzi A, Valente EM (2013) Joubert syndrome: congenital cerebellar ataxia with the molar tooth. Lancet Neurol 12:894–905. https://doi.org/10.1016/S1474-4422(13)70136-4
Bockenhauer D, Feather S, Stanescu HC et al (2009) Epilepsy, ataxia, sensorineural deafness, tubulopathy, and KCNJ10 mutations. N Engl J Med 360:1960–1970. https://doi.org/10.1056/NEJMoa0810276
Rumsby G (2016) Genetic defects underlying renal stone disease. Int J Surg 36:590–595. https://doi.org/10.1016/j.ijsu.2016.11.015
Paolella G, Santamaria R, Buono P, Salvatore F (1987) Mapping of a restriction fragment length polymorphism within the human aldolase B gene. Hum Genet 77:115–117. https://doi.org/10.1007/BF00272375
Hendy GN, D’Souza-Li L, Yang B et al (2000) Mutations of the calcium-sensing receptor (CASR) in familial hypocalciuric hypercalcemia, neonatal severe hyperparathyroidism, and autosomal dominant hypocalcemia. Hum Mutat 16:281–296. https://doi.org/10.1002/1098-1004(200010)16:4<281::AID-HUMU1>3.0.CO;2-A
Madore F, Stampfer MJ, Rimm EB, Curhan GC (1998) Nephrolithiasis and risk of hypertension. Am J Hypertens 11:46–53. https://doi.org/10.1016/s0895-7061(97)00371-3
Assimos D, Krambeck A, Miller NL et al (2016) Surgical management of stones: American Urological Association/Endourological Society Guideline, PART I. J Urol 196:1153–1160. https://doi.org/10.1016/j.juro.2016.05.090
Skolarikos A, Straub M, Knoll T et al (2015) Metabolic evaluation and recurrence prevention for urinary stone patients: EAU guidelines. Eur Urol 67:750–763. https://doi.org/10.1016/j.eururo.2014.10.029
Bonzo JR, Tasian GE (2017) The emergence of kidney stone disease during childhood-impact on adults. Curr Urol Rep 18:44. https://doi.org/10.1007/s11934-017-0691-x
Hopp K, Cogal AG, Bergstralh EJ et al (2015) Phenotype-genotype correlations and estimated carrier frequencies of primary hyperoxaluria. J Am Soc Nephrol 26:2559–2570. https://doi.org/10.1681/ASN.2014070698
Wu C-HW, Badreddine J, Chang J et al (2023) Population genetics analysis of SLC3A1 and SLC7A9 revealed the etiology of cystine stone may be more than what our current genetic knowledge can explain. Urolithiasis 51:101. https://doi.org/10.1007/s00240-023-01473-z
Sas DJ, Enders FT, Mehta RA et al (2020) Clinical features of genetically confirmed patients with primary hyperoxaluria identified by clinical indication versus familial screening. Kidney Int 97:786–792. https://doi.org/10.1016/j.kint.2019.11.023
Author information
Authors and Affiliations
Contributions
All listed authors contributed to this manuscript through data collection, analysis, interpretation, writing, and reviewing the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Donald Bodner owns stock shares in Fortec Litho Inc. The other authors report no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wu, CH.W., Badreddine, J., Su, E. et al. Beyond the kidney: extra-renal manifestations of monogenic nephrolithiasis and their significance. Pediatr Nephrol 39, 1429–1434 (2024). https://doi.org/10.1007/s00467-023-06242-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-023-06242-z