Abstract
Background
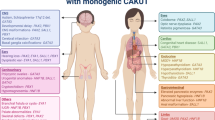
Kabuki syndrome (KS) is a genetic disorder caused mainly by de novo pathogenic variants in KMT2D or KDM6A, characterized by recognizable facial features, intellectual disability, and multi-systemic involvement, including short stature, microcephaly, hearing loss, cardiac defects, and additional congenital anomalies. While congenital anomalies of the kidneys and urinary tract (CAKUT) are known manifestations of this disorder, studies focused solely on kidney involvement are scarce, and its prevalence is most likely underestimated. This study aimed to describe the prevalence and nature of CAKUT and other renal manifestations, in a cohort of KS patients followed at a single tertiary center.
Methods
All patients who were evaluated at the Sheba Medical Center and received a clinical and/or molecular diagnosis of KS, over a 16-year period (2004–2020), were included. Digital medical records, including ultrasound studies, were reviewed by a team of pediatric nephrologists.
Results
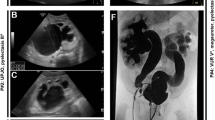
Thirteen patients were included in the study, at ages ranging from the neonatal period to 20 years. In eight patients, a pathogenic variant in KMT2D was established. CAKUT were detected in 8/13 (61.5%) of patients and varied from hypospadias, hydronephrosis, or double collecting systems to pelvic kidney, kidney asymmetry, horseshoe kidney, or kidney agenesis. One patient experienced kidney failure necessitating transplantation at 20 years of age.
Conclusions
Our findings underscore the high prevalence of CAKUT and genitourinary involvement in patients with KS and suggest that assessment by pediatric nephrology specialists is warranted as part of the routine multidisciplinary evaluation of newly diagnosed patients.
Graphical abstract
A higher resolution version of the Graphical abstract is available as Supplementary information


reproduced from STRING (https://string-db.org), version 11.0, for Homo-sapiens. Network nodes represent proteins and edges represent protein–protein interactions in different types of evidence for association
Similar content being viewed by others
Data Availability
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
Code availability
Not applicable.
References
Adam MP, Banka S, Bjornsson HT, Bodamer O, Chudley AE, Harris J, Kawame H, Lanpher BC, Lindsley AW, Merla G, Miyake N, Okamoto N, Stumpel CT, Niikawa N, Kabuki Syndrome Medical Advisory Board (2019) Kabuki syndrome: international consensus diagnostic criteria. J Med Genet 56:89–95
Matsumoto N, Niikawa N (2003) Kabuki make-up syndrome: a review. Am J Med Genet C Semin Med Genet 117C:57–65
Banka S, Veeramachaneni R, Reardon W, Howard E, Bunstone S, Ragge N et al (2012) How genetically heterogeneous is Kabuki syndrome?: MLL2 testing in 116 patients, review and analyses of mutation and phenotypic spectrum. Eur J Hum Genet 20:381–388
Makrythanasis P, van Bon BW, Steehouwer M, Rodríguez-Santiago B, Simpson M, Dias P et al (2013) MLL2 mutation detection in 86 patients with Kabuki syndrome: a genotype-phenotype study. Clin Genet 84:539–545
Paděrová J, Holubová A, Simandlová M, Puchmajerová A, Vlčková M, Malíková M, Pourová R, Vejvalková S, Havlovicová M, Šenkeříková M, Ptáková N, Drábová J, Geryk J, Maver A, Křepelová A, Macek M Jr (2016) Molecular genetic analysis in 14 Czech Kabuki syndrome patients is confirming the utility of phenotypic scoring. Clin Genet 90:230–237
Courcet J-B, Faivre L, Michot C, Burguet A, Perez-Martin S, Alix E et al (2013) Clinical and molecular spectrum of renal malformations in Kabuki syndrome. J Pediatr 163:742–746
Ewart-Toland A, Enns GM, Cox VA, Mohan GC, Rosenthal P, Golabi M (1998) Severe congenital anomalies requiring transplantation in children with Kabuki syndrome. Am J Med Genet 80:362–367
Hamdi Kamel M, Gilmartin B, Mohan P, Hickey DP (2006) Successful long-term outcome of kidney transplantation in a child with Kabuki syndrome. Pediatr Transplant 10:105–107
Kohei N, Takada H, Hishiki K, Nakashima Y, Yoshimura K, Nishio Y, Ito K, Matsuo K, Mori N (2016) Spontaneous Infection of an atrophic ureter with an ectopic ureteral opening after living-donor renal transplantation in a patient with Kabuki syndrome. Hinyokika Kiyo 62:455–458
Armstrong L, Abd El Moneim A, Aleck K, Aughton DJ, Baumann C, Braddock SR et al (2005) Further delineation of Kabuki syndrome in 48 well-defined new individuals. Am J Med Genet A 132A:265–272
Rosenblum S, Pal A, Reidy K (2017) Renal development in the fetus and premature infant. Semin Fetal Neonatal Med 22:58–66
Vivante A, Kohl S, Hwang D-Y, Dworschak GC, Hildebrandt F (2014) Single-gene causes of congenital anomalies of the kidney and urinary tract (CAKUT) in humans. Pediatr Nephrol 29:695–704
Shpargel KB, Mangini CL, Xie G, Ge K, Magnuson T (2020) The KMT2D Kabuki syndrome histone methylase controls neural crest cell differentiation and facial morphology. Development 147:dev187997
Pacelli C, Adipietro I, Malerba N, Squeo GM, Piccoli C, Amoresano A, Pinto G, Pucci P, Lee JE, Ge K, Capitanio N, Merla G (2020) Loss of function of the gene encoding the histone methyltransferase KMT2D leads to deregulation of mitochondrial respiration. Cells 9:1685
Wanner N, Vornweg J, Combes A, Wilson S, Plappert J, Rafflenbeul G et al (2019) DNA methyltransferase 1 controls nephron progenitor cell renewal and differentiation. J Am Soc Nephrol 30:63–78
Acknowledgements
The authors wish to thank the patients and their families for their kind cooperation and assistance.
Author information
Authors and Affiliations
Contributions
R.M.-R., B.P.-S., and A.R.-R. initiated the study and substantially contributed to its conception and design, acquisition, analysis, and interpretation of the data and wrote the manuscript. A.V., E.L., M.K., O.C. and R.S. contributed to the recruitment of patients and acquisition of data. In addition, all authors critically reviewed the manuscript and approved the submitted version.
Corresponding author
Ethics declarations
Ethics approval
The described research adhered to the tenets of the Declaration of Helsinki. The study was approved by the local Institutional Review Board (IRB).
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Supplementary data associated with this article can be found, in the online version, at http://dx.doi.org/
Rights and permissions
About this article
Cite this article
Merdler-Rabinowicz, R., Pode-Shakked, B., Vivante, A. et al. Kidney and urinary tract findings among patients with Kabuki (make-up) syndrome. Pediatr Nephrol 36, 4009–4012 (2021). https://doi.org/10.1007/s00467-021-05216-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-021-05216-3