Abstract
Background
Atypical hemolytic uremic syndrome (aHUS) is frequently associated with gene mutations in complement-regulatory proteins and activators. Different complement C3 gene mutations have been associated with different outcomes in aHUS.
Case-Diagnosis/Treatment
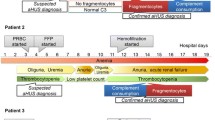
We report the case of a 21-year-old male with a C3 heterozygous gene mutation (p.Ile1157Thr) who developed aHUS at the age of 10 months and had six relapses, the last at the age of 14.5 years. Each relapse was characterized by an apparent predominance of hematological manifestations with milder renal involvement and was followed by complete recovery, with creatinine values and hematological parameters usually recovering after the 3rd to 6th day of hospitalization. The patient was treated with plasma infusion, apart from the initial and the last episode, when dialysis was needed. Twenty years after the onset, he retains normal renal function, with no proteinuria or hypertension. One similar case of highly recurrent aHUS carrying the same C3 mutation as our patient with recovery of renal function has been previously reported.
Conclusions
We further support that aHUS associated with the p.Ile1157Thr C3 mutation may be highly recurrent, but with recovered renal function. The prevalent p.Ile1157Thr C3 gene mutation has variable disease manifestations and both severe and milder renal phenotypes have been found.

Similar content being viewed by others
Abbreviations
- aHUS:
-
Atypical hemolytic uremic syndrome
- FH:
-
Factor H
- FI:
-
Factor I
- MCP:
-
Membrane cofactor protein
- FB:
-
Factor B
- ESRD:
-
End-stage renal disease
- CFHR:
-
Complement factor H-related proteins
- FFP:
-
Fresh frozen plasma
- RBC:
-
Red blood cell
References
Nester CM, Barbour T, de Cordoba SR, Dragon-Durey MA, Frémeaux-Bacchi V, Goodship TH, Kavanagh D, Noris M, Pickering M, Sanchez-Corral P, Skerka C, Zipfel P, Smith RJ (2015) Atypical aHUS: state of the art. Mol Immunol 67:31–42
Dragon-Durey MA, Loirat C, Cloarec S, Macher MA, Blouin J, Nivet H, Weiss L, Fridman WH, Frémeaux-Bacchi V (2005) Anti-Factor H autoantibodies associated with atypical hemolytic uremic syndrome. J Am Soc Nephrol 16:555–563
Sinha A, Gulati A, Saini S, Blanc C, Gupta A, Gurjar BS, Saini H, Kotresh ST, Ali U, Bhatia D, Ohri A, Kumar M, Agarwal I, Gulati S, Anand K, Vijayakumar M, Sinha R, Sethi S, Salmona M, George A, Bal V, Singh G, Dinda AK, Hari P, Rath S, Dragon-Durey MA, Bagga A, Indian HUS Registry (2014) Prompt plasma exchanges and immunosuppressive treatment improves the outcomes of anti-factor H autoantibody-associated hemolytic uremic syndrome in children. Kidney Int 85:1151–1160
Józsi M, Licht C, Strobel S, Zipfel SL, Richter H, Heinen S, Zipfel PF, Skerka C (2008) Factor H autoantibodies in atypical hemolytic uremic syndrome correlate with CFHR1/CFHR3 deficiency. Blood 111:1512–1514
Frémeaux-Bacchi V, Miller EC, Liszewski MK, Strain L, Blouin J, Brown AL, Moghal N, Kaplan BS, Weiss RA, Lhotta K, Kapur G, Mattoo T, Nivet H, Wong W, Gie S, Hurault de Ligny B, Fischbach M, Gupta R, Hauhart R, Meunier V, Loirat C, Dragon-Durey MA, Fridman WH, Janssen BJ, Goodship TH, Atkinson JP (2008) Mutations in complement C3 predispose to development of atypical hemolytic uremic syndrome. Blood 112:4948–4952
Schramm EC, Roumenina LT, Rybkine T, Chauvet S, Vieira-Martins P, Hue C, Maga T, Valoti E, Wilson V, Jokiranta S, Smith RJ, Noris M, Goodship T, Atkinson JP, Frémeaux-Bacchi V (2015) Mapping interactions between complement C3 and regulators using mutations in atypical hemolytic uremic syndrome. Blood 125:2359–2369
Fremeaux-Bacchi V, Fakhouri F, Garnier A, Bienaimé F, Dragon-Durey MA, Ngo S, Moulin B, Servais A, Provot F, Rostaing L, Burtey S, Niaudet P, Deschênes G, Lebranchu Y, Zuber J, Loirat C (2013) Genetics and outcome of atypical hemolytic uremic syndrome: a nationwide French series comparing children and adults. Clin J Am Soc Nephrol 8:554–562
Noris M, Caprioli J, Bresin E, Mossali C, Pianetti G, Gamba S, Daina E, Fenili C, Castelletti F, Sorosina A, Piras R, Donadelli R, Maranta R, van der Meer I, Conway EM, Zipfel PF, Goodship TH, Remuzzi G (2010) Relative role of genetic complement abnormalities in sporadic and familial aHUS and their impact on clinical phenotype. Clin J Am Soc Nephrol 5:1844–1859
Martínez-Barricarte R, Heurich M, López-Perrote A, Tortajada A, Pinto S, López-Trascasa M, Sánchez-Corral P, Morgan BP, Llorca O, Harris CL, Rodríguez de Córdoba S (2015) The molecular and structural bases for the association of complement C3 mutations with atypical hemolytic uremic syndrome. Mol Immunol 66:263–273
Volokhina E, Westra D, Xue X, Gros P, van de Kar N, van den Heuvel L (2012) Novel C3 mutation p.Lys65Gln in aHUS affects complement factor H binding. Pediatr Nephrol 27:1519–1524
Maga TK, Nishimura CJ, Weaver AE, Frees KL, Smith RJ (2010) Mutations in alternative pathway complement proteins in American patients with atypical hemolytic uremic syndrome. Hum Mutat 31:E1445–1460
Fan X, Yoshida Y, Honda S, Matsumoto M, Sawada Y, Hattori M, Hisanaga S, Hiwa R, Nakamura F, Tomomori M, Miyagawa S, Fujimaru R, Yamada H, Sawai T, Ikeda Y, Iwata N, Uemura O, Matsukuma E, Aizawa Y, Harada H, Wada H, Ishikawa E, Ashida A, Nangaku M, Miyata T, Fujimura Y (2013) Analysis of genetic and predisposing factors in Japanese patients with atypical hemolytic uremic syndrome. Mol Immunol 54:238–246
Matsumoto T, Fan X, Ishikawa E, Ito M, Amano K, Toyoda H, Komada Y, Ohishi K, Katayama N, Yoshida Y, Matsumoto M, Fujimura Y, Ikejiri M, Wada H, Miyata T (2014) Analysis of patients with atypical hemolytic uremic syndrome treated at the Mie University Hospital: concentration of C3 p.I1157T mutation. Int J Hematol 100:437–442
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
VFB has received fees from Alexion Pharmaceuticals for invited lectures and is member of an expert board supported by Alexion Pharmaceuticals.
Rights and permissions
About this article
Cite this article
Siomou, E., Gkoutsias, A., Serbis, A. et al. aHUS associated with C3 gene mutation: a case with numerous relapses and favorable 20-year outcome. Pediatr Nephrol 31, 513–517 (2016). https://doi.org/10.1007/s00467-015-3267-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-015-3267-3