Abstract
Background
Female sex has been associated with worse outcomes after groin hernia repair (GHR), including a higher rate of chronic pain and recurrence. Most of the studies in GHR are performed in males, and the recommendations for females extrapolate from these studies, even though females have anatomy intricacies. The round ligament of the uterus (RLU) is associated with pelvic stabilization and plays a role in sensory function. Transection of the RLU during GHR is controversial as it can allow easier mesh placement but can favor genitourinary complications and chronic pain. As no previous meta-analysis compared preserving versus transecting the RLU during minimally invasive (MIS) GHR, we aim to perform a systematic review and meta-analysis evaluating surgical outcomes comparing the approaches.
Methods
Cochrane Central, Embase, and PubMed databases were systematically searched for studies comparing transection versus preservation of the RLU in MIS groin hernia surgeries. Outcomes assessed were operative time, bleeding, surgical site events, hospital stay, chronic pain, paresthesia, recurrence rates, and genital prolapse rates. Statistical analysis was performed using RevMan 5.4.1. Heterogeneity was assessed with I2 statistics. A review protocol for this meta-analysis was registered at PROSPERO (CRD 42023467146).
Results
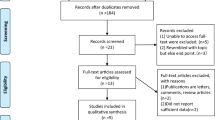
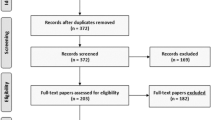
1738 studies were screened. A total of six studies, comprising 1131 women, were included, of whom 652 (57.6%) had preservation of the RLU during MIS groin hernia repair. We found no statistical difference regarding chronic pain, paresthesia, recurrence rates, and postoperative complications. We found a longer operative time for the preservation group (MD 6.84 min; 95% CI 3.0–10.68; P = 0.0005; I2 = 74%).
Conclusion
Transecting the RLU reduces the operative time during MIS GHR with no difference regarding postoperative complication rates. Although transection appears safe, further prospective randomized studies with long-term follow-up and patient-reported outcomes are necessary to define the optimal management of RLU during MIS GHR.




Similar content being viewed by others
References
Tolver MA, Strandfelt P, Rosenberg J, Bisgaard T (2013) Female gender is a risk factor for pain, discomfort, and fatigue after laparoscopic groin hernia repair. Hernia 17(3):321–327
Nilsson H, Holmberg H, Nordin P (2018) Groin hernia repair in women—a nationwide register study. Am J Surg 216(2):274–279
Köckerling F, Koch A, Lorenz R (2019) Groin hernias in women—a review of the literature. Front Surg 6(February):1–8
Bittner R, Arregui ME, Bisgaard T, Dudai M, Ferzli GS, Fitzgibbons RJ et al (2011) Guidelines for laparoscopic (TAPP) and endoscopic (TEP) treatment of inguinal hernia [International Endohernia Society (IEHS)]. Surg Endosc 25(9):2773–2843
HerniaSurge Group (2018) International guidelines for groin hernia management. Hernia 22(1):1–165. https://doi.org/10.1007/s10029-017-1668-x
Lin R, Lin X, Yang Y, Wang C, Fang H, Chen Y et al (2023) Laparoscopic transabdominal preperitoneal repair for female patients with groin hernias. BMC Womens Health 23(1):422
Liu Y, Liu J, Xu Q, Zhang B, Wang M, Zhang G et al (2022) Objective follow-up after transection of uterine round ligament during laparoscopic repair of inguinal hernias in women: assessment of safety and long-term outcomes. Surg Endosc 36(6):3798–3804. https://doi.org/10.1007/s00464-021-08696-4
Luk Y, Chau PL, Law TT, Ng L, Wong KY (2021) Laparoscopic total extraperitoneal groin hernia repair in females: comparison of outcomes between preservation or division of the uterine round ligament. J Laparoendosc Adv Surg Tech 31(1):6–10
Gopal SV, Warrier A (2013) Recurrence after groin hernia repair-revisited. Int J Surg 11(5):374–377
Fauconnier A, Dubuisson JB, Foulot H, Deyrolles C, Sarrot F, Laveyssière MN et al (2006) Mobile uterine retroversion is associated with dyspareunia and dysmenorrhea in an unselected population of women. Eur J Obstet Gynecol Reprod Biol 127(2):252–256
Guo M, Chen D, Zhang H, Lu C (2019) Safety and efficiency of laparoscopic femoral hernia repair with preserved uterine round ligament. J Coll Phys Surg Pak 29(10):932–936
Onwude JL (2012) Genital prolapse in women. BMJ Clin Evid 2012:0817
Sterne JAC, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I et al (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366:l4898
Sterne JA, Hernán MA, Reeves BC, Savović J, Berkman ND, Viswanathan M et al (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919
Balshem H, Helfand M, Schünemann HJ, Oxman AD, Kunz R, Brozek J et al (2011) GRADE guidelines: 3. Rating the quality of evidence. J Clin Epidemiol 64(4):401–406
Kark AE, Kurzer M (2008) Groin hernias in women. Hernia 12(3):267–270
Tuma F, Lopez RA, Varacallo M (2023) Anatomy, abdomen and pelvis: inguinal region (inguinal canal). StatPearls Publishing, Treasure Island
Muavha DA, Ras L, Jeffery S (2019) Laparoscopic surgical anatomy for pelvic floor surgery. Best Pract Res Clin Obstet Gynaecol 54:89–102
Burcharth J, Andresen K, Pommergaard H-C, Bisgaard T, Rosenberg J (2014) Direct inguinal hernias and anterior surgical approach are risk factors for female inguinal hernia recurrences. Langenbeck’s Arch Surg 399(1):71–76
Ilonzo N, Gribben J, Neifert S, Pettke E, Leitman IM (2019) Laparoscopic inguinal hernia repair in women: trends, disparities, and postoperative outcomes. Am J Surg 218(4):726–729
Białecki J, Pyda P, Antkowiak R, Domosławski P (2021) Unsuspected femoral hernias diagnosed during endoscopic inguinal hernia repair. Adv Clin Exp Med 30(2):135–138
Schouten N, Burgmans JPJ, van Dalen T, Smakman N, Clevers GJ, Davids PHP et al (2012) Female “groin” hernia: totally extraperitoneal (TEP) endoscopic repair seems the most appropriate treatment modality. Hernia 16(4):387–392
Schmidt L, Andresen K, Öberg S, Rosenberg J (2018) Dealing with the round ligament of uterus in laparoscopic groin hernia repair: a nationwide survey among experienced surgeons. Hernia 22(5):849–855. https://doi.org/10.1007/s10029-018-1802-4
Martins P, Silva-Filho AL, Fonseca AMRM, Santos A, Santos L, Mascarenhas T et al (2013) Strength of round and uterosacral ligaments: a biomechanical study. Arch Gynecol Obstet 287(2):313–318
Yen C-F, Wang C-J, Lin S-L, Lee C-L, Soong Y-K (2002) Combined laparoscopic uterosacral and round ligament procedures for treatment of symptomatic uterine retroversion and mild uterine decensus. J Am Assoc Gynecol Laparosc 9(3):359–366
Zhou Z, Tong C, Tian L, Zhang X, Li Y, Xiao Y et al (2023) Retrospective study of preservation and transection of the round ligament of uterus during laparoscopic transabdominal preperitoneal inguinal hernia repair in adult women. Hernia 27:1627
Yang XF, Liu JL (2016) Laparoscopic repair of inguinal hernia in adults. Ann Transl Med 4(20):1–19
Abolmasov A, Bashankaev B (2019) Laparoscopic round ligament preserving repair for groin hernia in women: a critical appraisal. Int J Abdom Wall Hernia Surg 2:130
He Z, Hao X, Feng B, Li J, Sun J, Xue P, Yue F, Yan X, Wang J, Zheng M (2019) Laparoscopic repair for groin hernias in female patients: a single-center experience in 15 years. J Laparoendosc Adv Surg Tech A 29(1):55–59. https://doi.org/10.1089/lap.2018.0287
Funding
The authors have no sources of funding to declare for this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Richard Lu received payment from Intuitive Surgical for lectures unrelated to this work. Carlos Silveira, Dr. Sergio Mazzola Poli de Figueiredo, Ana Rasador, Miguel Fernandez, Dr. Rafael Martin, Dr. Yasmin Dias have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Silveira, C.A.B., de Figueiredo, S.M.P., Rasador, A.C.D. et al. Round ligament management during minimally invasive groin hernia repair in women: a systematic review and meta-analysis. Surg Endosc 38, 1731–1739 (2024). https://doi.org/10.1007/s00464-024-10721-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-024-10721-1