Abstract
Background
Obesity is a public health concern among adolescents and young adults. Bariatric surgery is the most effective treatment for morbid obesity and has been increasingly utilized in young patients. Long-term outcomes data for bariatric surgery in this age group are limited.
Methods
This is a single-institution, prospective analysis of 167 patients aged 15–24 years who underwent one of three laparoscopic bariatric procedures between 2001 and 2019: Roux-en-Y gastric bypass (LRYGB, n = 71), adjustable gastric banding (LAGB, n = 22), and sleeve gastrectomy (LSG, n = 74). Longitudinal weight and body mass index (BMI) measurements were compared to evaluate patterns of weight loss.
Results
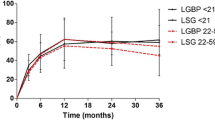
All operations were completed laparoscopically using the same clinical pathways. Patients were predominantly female (82.6%), had a median age of 22.0 [Q1-Q3 20.0–23.0] years, and had a mean presurgical BMI of 48.5 ± 6.5 kg/m2 (range 38.4–68.1 kg/m2). All procedures produced significant weight loss by 1 year, peak weight loss by 2 years, and modest weight regain after 5 years. Mean percent weight/BMI losses at 5 years for LRYGB, LAGB, and LSG were − 36.7 ± 10.8%, − 14.5 ± 15.3%, and − 25.1 ± 13.4%, respectively (p < 0.001). LRYGB patients were most likely to achieve ≥ 25% weight loss at 1, 3, and 5 years and maintained significant average weight loss for more than 15 years after surgery. Reoperations were procedure-specific, with LAGB, LRYGB, and LSG having the highest, middle, and lowest reoperation rates, respectively (40.9% vs. 16.9% vs. 5.4%, p < 0.001).
Conclusion
All procedures provided significant and durable weight loss. LRYGB patients achieved the best and most sustained weight loss. LSG patients experienced second-best weight loss between 1 and 5 years, with lowest chance of reoperation. LAGB patients had the least weight loss and the highest reoperation rate. Compared to other factors, type of bariatric procedure was independently predictive of successful weight loss over time. More studies with long-term follow-up are needed.
Graphical abstract





Similar content being viewed by others
Change history
24 August 2022
A Correction to this paper has been published: https://doi.org/10.1007/s00464-022-09574-3
References
Sanyaolu A, Okorie C, Qi X, Locke J, Rehman S (2019) Childhood and adolescent obesity in the united states: a public health concern. Glob Pediatr Health. https://doi.org/10.1177/2333794X19891305
Fryar CD, Carroll MD, Afful J (2021) Prevalence of Overweight, Obesity, and Severe Obesity among Children and Adolescents Aged 2–19 Years: United States, 1963–1965 through 2017–2018. NCHS Health E-Stats: 1–7
Barnett SJ (2013) Bariatric surgical management of adolescents with morbid obesity. Curr Opin Pediatr 25(4):515–520. https://doi.org/10.1097/MOP.0b013e328362cd96
Kelly AS, Barlow SE, Rao G, Inge TH, Hayman LL, Steinberger J, Urbina EM, Ewing LJ, Daniels SR (2013) Severe obesity in children and adolescents: identification, associated health risks, and treatment approaches: a scientific statement from the American heart association. Circulation 128(15):1689–1712. https://doi.org/10.1161/CIR.0b013e3182a5cfb3
Freedman DS, Mei Z, Srinivasan SR, Berenson GS, Dietz WH (2007) Cardiovascular risk factors and excess adiposity among overweight children and adolescents: the Bogalusa heart study. J Pediatr 150(1):12-17.e2. https://doi.org/10.1016/j.jpeds.2006.08.042
Pratt JS, Browne A, Browne NT, Bruzoni M, Cohen M, Desai A, Inge T, Linden BC, Mattar SG, Michalsky M, Podkameni D, Reichard KW, Stanford FC, Zeller MH (2018) Zitsman J (2018) ASMBS pediatric metabolic and bariatric surgery guidelines. Surg Obes Relat Dis 14(7):882–901. https://doi.org/10.1016/j.soard.2018.03.019
Kelly AS, Ryder JR, Marlatt KL, Rudser KD, Jenkins T, Inge TH (2016) Changes in inflammation, oxidative stress and adipokines following bariatric surgery among adolescents with severe obesity. Int J Obes 40(2):275–280. https://doi.org/10.1038/ijo.2015.174
Kumar S, Kelly AS (2017) Review of childhood obesity. Mayo Clin Proc 92(2):251–265. https://doi.org/10.1016/j.mayocp.2016.09.017
Loux TJ, Haricharan RN, Clements RH, Kolotkin RL, Bledsoe SE, Haynes B, Leath T, Harmon CM (2008) Health-related quality of life before and after bariatric surgery in adolescents. J Pediatr Surg 43(7):1275–1279. https://doi.org/10.1016/j.jpedsurg.2008.02.078
Loy JJ, Youn HA, Schwack B, Kurian M, Ren Fielding C, Fielding GA (2015) Improvement in nonalcoholic fatty liver disease and metabolic syndrome in adolescents undergoing bariatric surgery. Surg Obes Relat Dis 11(2):442–449. https://doi.org/10.1016/j.soard.2014.11.010
Skinner AC, Ravanbakht SN, Skelton JA, Perrin EM, Armstrong SC (2018) Prevalence of obesity and severe obesity in us children, 1999–2016. Pediatrics 141(3):e20173459. https://doi.org/10.1542/peds.2017-3459
Steinberger AE, Youngwirth LM, Kim SE, Duke NN, Skinner A, Gordee A, Kuchibhatla M, Armstrong S, Seymour KA (2021) Adolescent bariatric surgery: racial disparities in 30-day outcomes using the mbsaqip from 2015 to 2018. Obes Surg 31(8):3776–3785. https://doi.org/10.1007/s11695-021-05500-z
Cummins CB, Nunez Lopez O, Hughes BD, Adhikari D, Guidry CA, Stubbs S, Radhakrishnan RS, Bowen-Jallow KA (2019) Adolescent bariatric surgery: effects of socioeconomic, demographic, and hospital characteristics on cost, length of stay, and type of procedure performed. Obes Surg 29(3):757–764. https://doi.org/10.1007/s11695-018-03657-8
Nunez Lopez O, Jupiter DC, Bohanon FJ, Radhakrishnan RS, Bowen-Jallow KA (2017) Health disparities in adolescent bariatric surgery: nationwide outcomes and utilization. J Adolesc Health 61(5):649–656. https://doi.org/10.1016/j.jadohealth.2017.05.028
Buchwald H, Avidor Y, Braunwald E, Jensen MD, Pories W, Fahrbach K, Schoelles K (2004) Bariatric surgery: a systematic review and meta-analysis. JAMA 292(14):15
Inge TH, Courcoulas AP, Jenkins TM, Michalsky MP, Helmrath MA, Brandt ML, Harmon CM, Zeller MH, Chen MK, Xanthakos SA, Horlick M, Buncher CR (2016) Weight loss and health status 3 years after bariatric surgery in adolescents. N Engl J Med 374(2):113–123. https://doi.org/10.1056/NEJMoa1506699
Black JA, White B, Viner RM, Simmons RK (2013) Bariatric surgery for obese children and adolescents: a systematic review and meta-analysis. Obes Rev 14(8):634–644. https://doi.org/10.1111/obr.12037
Paulus GF, de Vaan LEG, Verdam FJ, Bouvy ND, Ambergen TAW, van Heurn LWE (2015) Bariatric surgery in morbidly obese adolescents: a systematic review and meta-analysis. Obes Surg 25(5):860–878. https://doi.org/10.1007/s11695-015-1581-2
Kelly AS, Fox CK, Rudser KD, Gross AC, Ryder JR (2016) Pediatric obesity pharmacotherapy: current state of the field, review of the literature, and clinical trial considerations. Int J Obes (Lond) 40(7):1043–1050. https://doi.org/10.1038/ijo.2016.69
United Nations. Youth. United Nations. 2022. URL: https://www.un.org/en/global-issues/youth (Accessed on 13 May).
World Health Organization. Adolescent and Young Adult Health. 2021. URL: https://www.who.int/news-room/fact-sheets/detail/adolescents-health-risksand-solutions (Accessed on 13 May).
Altieri MS, Pryor A, Bates A, Docimo S, Talamini M, Spaniolas K (2018) Bariatric procedures in adolescents are safe in accredited centers. Surg Obes Relat Dis 14(9):1368–1372. https://doi.org/10.1016/j.soard.2018.04.004
Desai NK, Wulkan ML, Inge TH (2016) Update on adolescent bariatric surgery. Endocrinol Metab Clin North Am 45(3):667–676. https://doi.org/10.1016/j.ecl.2016.04.015
Olbers T, Beamish AJ, Gronowitz E, Flodmark CE, Dahlgren J, Bruze G, Ekbom K, Friberg P, Göthberg G, Järvholm K, Karlsson J, Mårild S, Neovius M, Peltonen M, Marcus C (2017) Laparoscopic roux-en-Y gastric bypass in adolescents with severe obesity (AMOS): a prospective, 5-year, Swedish nationwide study. Lancet Diabetes Endocrinol 5(3):174–183. https://doi.org/10.1016/S2213-8587(16)30424-7
Maffazioli GD, Stanford FC, Campoverde Reyes KJ, Stanley TL, Singhal V, Corey KE, Pratt JS, Bredella MA, Misra M (2016) Comparing outcomes of two types of bariatric surgery in an adolescent obese population: roux-en-y gastric bypass vs Sleeve Gastrectomy. Front Pediatr. https://doi.org/10.3389/fped.2016.00078
Salminen P, Helmiö M, Ovaska J, Juuti A, Leivonen M, Peromaa-Haavisto P, Hurme S, Soinio M, Nuutila P, Victorzon M (2018) Effect of laparoscopic sleeve gastrectomy vs laparoscopic roux-en-y gastric bypass on weight loss at 5 years among patients with morbid obesity: the SLEEVEPASS randomized clinical trial. JAMA 319(3):241. https://doi.org/10.1001/jama.2017.20313
Stanford FC, Mushannen T, Cortez P, Campoverde Reyes KJ, Lee H, Gee DW, Pratt JS, Boepple PA, Bredella MA, Misra M, Singhal V (2020) Comparison of short and long-term outcomes of metabolic and bariatric surgery in adolescents and adults. Front Endocrinol 11:1–8. https://doi.org/10.3389/fendo.2020.00157
Toolabi K, Golzarand M, Farid R (2021) Laparoscopic roux-en-Y gastric bypass and laparoscopic sleeve gastrectomy in terms of efficacy and safety: a comparative study during 11-year experience. Obes Surg 31(6):2489–2496. https://doi.org/10.1007/s11695-021-05313-0
Zeller MH, Pendery EC, Reiter-Purtill J, Hunsaker SL, Jenkins TM, Helmrath MA, Inge TH (2017) From adolescence to young adulthood: trajectories of psychosocial health following roux-en-Y gastric bypass. Surg Obes Relat Dis 13(7):1196–1203. https://doi.org/10.1016/j.soard.2017.03.008
Humayon S, Altieri MS, Yang J, Nie L, Spaniolas K, Pryor AD (2019) Recent trends of bariatric surgery in adolescent population in the state of new York. Surg Obes Relat Dis 15(8):1388–1393. https://doi.org/10.1016/j.soard.2019.04.016
Sawyer SM, Azzopardi PS, Wickremarathne D, Patton GC (2018) The age of adolescence. Lancet Child Adolesc Health 2(3):223–228. https://doi.org/10.1016/S2352-4642(18)30022-1
NIH conference (1991) Gastrointestinal surgery for severe obesity: Consensus Development Conference Panel. Ann Intern Med 115(12):956–961
Di Lorenzo N, Furbetta F, Favretti F, Segato G, De Luca M, Micheletto G, Zappa M, De Meis P, Lattuada E, Paganelli M, Lucchese M, Basso N, Capizzi FD, Di Cosmo L, Mancuso V, Civitelli S, Gardinazzi A, Giardiello C, Veneziani A, Boni M, Borrelli V, Schettino A, Forestieri P, Pilone V, Camperchioli I, Lorenzo M (2010) Laparoscopic adjustable gastric banding via pars flaccida versus perigastric positioning: technique, complications, and results in 2549 patients. Surg Endosc 24(7):1519–1523. https://doi.org/10.1007/s00464-009-0669-y
Arafat M, Norain A, Burjonrappa S (2019) Characterizing bariatric surgery utilization and complication rates in the adolescent population. J Pediatr Surg 54(2):288–292. https://doi.org/10.1016/j.jpedsurg.2018.10.089
Malhotra S, Czepiel KS, Akam EY, Shaw AY, Sivasubramanian R, Seetharaman S, Stanford FC (2021) Bariatric surgery in the treatment of adolescent obesity: current perspectives in the United States. Expert Rev Endocrinol Metab 16(3):123–134. https://doi.org/10.1080/17446651.2021.1914585
Maciejewski ML, Arterburn DE, Van Scoyoc L, Smith VA, Yancy WS, Weidenbacher HJ, Livingston EH, Olsen MK (2016) Bariatric surgery and long-term durability of weight loss. JAMA Surg 151(11):1046. https://doi.org/10.1001/jamasurg.2016.2317
Pedroso FE, Angriman F, Endo A, Dasenbrock H, Storino A, Castillo R, Watkins AA, Castillo-Angeles M, Goodman JE, Zitsman JL (2018) Weight loss after bariatric surgery in obese adolescents: a systematic review and meta-analysis. Surg Obes Relat Dis 14(3):413–422. https://doi.org/10.1016/j.soard.2017.10.003
Golzarand M, Toolabi K, Farid R (2017) The bariatric surgery and weight losing: a meta-analysis in the long- and very long-term effects of laparoscopic adjustable gastric banding, laparoscopic roux-en-Y gastric bypass and laparoscopic sleeve gastrectomy on weight loss in adults. Surg Endosc 31(11):4331–4345. https://doi.org/10.1007/s00464-017-5505-1
Puzziferri N, Roshek TB, Mayo HG, Gallagher R, Belle SH, Livingston EH (2014) Long-term follow-up after bariatric surgery: a systematic review. JAMA 312(9):934. https://doi.org/10.1001/jama.2014.10706
Halloun R, Weiss R (2021) Bariatric surgery in adolescents with obesity: long-term perspectives and potential alternatives. Horm Res Paediatr. https://doi.org/10.1159/000520810
O’Brien PE, Hindle A, Brennan L, Skinner S, Burton P, Smith A, Crosthwaite G, Brown W (2019) Long-term outcomes after bariatric surgery: a systematic review and meta-analysis of weight loss at 10 or more years for all bariatric procedures and a single-centre review of 20-year outcomes after adjustable gastric banding. Obes Surg 29(1):3–14. https://doi.org/10.1007/s11695-018-3525-0
Courcoulas AP, Yanovski SZ, Bonds D, Eggerman TL, Horlick M, Staten MA, Arterburn DE (2014) Long-term outcomes of bariatric surgery: a national institutes of health symposium. JAMA Surg 149(12):1323–1329. https://doi.org/10.1001/jamasurg.2014.2440
Gorecki P, McClelland PH, Kabata K, Khusid E, Zenilman ME (2021) weight loss dynamics following laparoscopic roux-en-Y gastric bypass. an analysis of 10-year follow-up data. Surg Endosc 35(9):5315–5321. https://doi.org/10.1007/s00464-020-08021-5
Nocca D, Nedelcu M, Nedelcu A, Noel P, Leger P, Skalli M, Lefebvre P, Coisel Y, Laurent C, Lemaitre F, Fabre JM (2014) Laparoscopic sleeve gastrectomy for late adolescent population. Obes Surg 24(6):861–865. https://doi.org/10.1007/s11695-014-1200-7
Golomb I, Ben David M, Glass A, Kolitz T, Keidar A (2015) Long-term metabolic effects of laparoscopic sleeve gastrectomy. JAMA Surg 150(11):1051–1057. https://doi.org/10.1001/jamasurg.2015.2202
Baig SJ, Priya P, Mahawar KK, Shah S, Indian Bariatric Surgery Outcome Reporting (IBSOR) Group (2019) Weight regain after bariatric surgery-a multicentre study of 9617 patients from indian bariatric surgery outcome reporting group. Obes Surg 29(5):1583–1592. https://doi.org/10.1007/s11695-019-03734-6
Sepúlveda M, Alamo M, Saba J, Astorga C, Lynch R, Guzmán H (2017) Long-term weight loss in laparoscopic sleeve gastrectomy. Surg Obes Relat Dis 13(10):1676–1681. https://doi.org/10.1016/j.soard.2017.07.017
Koh CY, Inaba CS, Sujatha-Bhaskar S, Hohmann S, Ponce J, Nguyen NT (2017) Laparoscopic adjustable gastric band explantation and implantation at academic centers. J Am Coll Surg 225(4):532–537. https://doi.org/10.1016/j.jamcollsurg.2017.06.015
Felsenreich DM, Langer FB, Bichler C, Kristo I, Jedamzik J, Eilenberg M, Arnoldner MA, Prager G (2019) Surgical therapy of weight regain after roux-en-y gastric bypass. Surg Obes Relat Dis 15(10):1719–1728. https://doi.org/10.1016/j.soard.2019.07.002
Shantavasinkul PC, Omotosho P, Corsino L, Portenier D, Torquati A (2016) Predictors of weight regain in patients who underwent roux-en-Y gastric bypass surgery. Surg Obes Relat Dis 12(9):1640–1645. https://doi.org/10.1016/j.soard.2016.08.028
Mingrone G, Panunzi S, De Gaetano A, Guidone C, Iaconelli A, Leccesi L, Nanni G, Pomp A, Castagneto M, Ghirlanda G, Rubino F (2012) Bariatric surgery versus conventional medical therapy for type 2 diabetes. N Engl J Med 366(17):1577–1585. https://doi.org/10.1056/NEJMoa1200111
Zitsman JL, DiGiorgi MF, Zhang AZ, Kopchinski JS, Sysko R, Devlin MJ, Fennoy I (2020) Adolescent gastric banding: a 5-year longitudinal study. Obes Surg 30(3):828–836. https://doi.org/10.1007/s11695-019-04321-5
Paroz A, Calmes JM, Giusti V, Suter M (2006) Internal hernia after laparoscopic roux-en-Y gastric bypass for morbid obesity: a continuous challenge in bariatric surgery. Obes Surg 16(11):1482–1487. https://doi.org/10.1381/096089206778870102
Ladak F, Dang JT, Switzer NJ, Mocanu V, Birch DW, Karmali S (2019) Rates of reoperation and nonoperative intervention within 30 days of bariatric surgery. Surg Obes Relat Dis 15(3):431–440. https://doi.org/10.1016/j.soard.2018.12.035
Mehaffey JH, LaPar DJ, Clement KC, Turrentine FE, Miller MS, Hallowell PT, Schirmer BD (2016) 10-year outcomes after roux-en-Y gastric bypass. Ann Surg 264(1):121–126. https://doi.org/10.1097/SLA.0000000000001544
Edholm D, Svensson F, Näslund I, Karlsson FA, Rask E, Sundbom M (2013) Long-term results 11 years after primary gastric bypass in 384 patients. Surg Obes Relat Dis 9(5):708–713. https://doi.org/10.1016/j.soard.2012.02.011
Ruiz-Cota P, Bacardí-Gascón M, Jiménez-Cruz A (2019) Long-Term outcomes of metabolic and bariatric surgery in adolescents with severe obesity with a follow-up of at least 5 years: a systematic review. Surg Obes Relat Dis 15(1):133–144. https://doi.org/10.1016/j.soard.2018.10.016
Acknowledgements
PHM and PG conceived the study concept and design. PG provided clinical material and data. KK and AJ verified data accuracy and performed data entry. PHM performed the data analysis. PHM and PG prepared the manuscript. WG, MEZ, and PG provided critical insight and revision of the manuscript. All authors reviewed the manuscript and gave final approval before submission.
Funding
No funding was obtained for this study. None of the authors assume any financial interest or support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Paul H. McClelland, Dr. Wojciech Gorecki, Dr. Michael E. Zenilman, and Dr. Piotr Gorecki have no conflicts of interest or financial ties to disclose. PA Krystyna Kabata and Antalya Jano also have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article was updated to correct the copyright holder.
Supplementary Information
Below is the link to the electronic supplementary material.
464_2022_9434_MOESM1_ESM.eps
Supplementary file1 (EPS 364 KB) Supplemental Figure 1a Weight loss curves for patients undergoing LRYGB, LAGB, and LSG, measured by absolute weight. Individual points represent single patient weights and diamonds/bars represent means ± SD
464_2022_9434_MOESM2_ESM.eps
Supplementary file2 (EPS 364 KB) Supplemental Figure 1b Weight loss curves for patients undergoing LRYGB, LAGB, and LSG, measured by BMI. Individual points represent single patient weights and diamonds/bars represent means ± SD.
464_2022_9434_MOESM3_ESM.eps
Supplementary file3 (EPS 365 KB) Supplemental Figure 1c Weight loss curves for patients undergoing LRYGB, LAGB, and LSG, measured by net BMI change from baseline. Individual points represent single patient weights and diamonds/bars represent means ± SD.
Rights and permissions
About this article
Cite this article
McClelland, P.H., Kabata, K., Gorecki, W. et al. Long-term weight loss after bariatric procedures for morbidly obese adolescents and youth: a single-institution analysis with up to 19-year follow-up. Surg Endosc 37, 2224–2238 (2023). https://doi.org/10.1007/s00464-022-09434-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09434-0