Abstract
Background
To comprehensively evaluate the efficacy and safety of Retzius sparing (RS) for men undergoing robot-assisted laparoscopic prostatectomy (RARP).
Methods
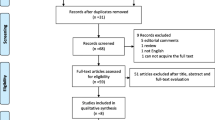
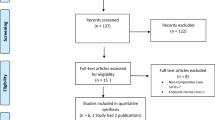
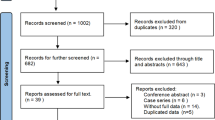
We searched four electronic databases and reference lists of relevant studies for eligible research published before March 11, 2019. After quality assessment, eligible studies were synthesized for relevant outcomes, including positive surgical margin (PSM), continence, incontinence, complication, console time, and hospital stay.
Results
Two randomized clinical trials and four observational studies were included in this study. Quantitative syntheses revealed significantly higher PSM rates in RS-RARP compared with conventional RARP (c-RARP) (odds ratio [OR] 1.68, p = 0.02). Furthermore, we found significantly higher PSM rates at the anterior site in RS-RARP compared with c-RARP (OR 4.34, p = 0.03) and significantly lower incontinence rates in RS-RARP in the first month (OR 0.30, p < 0.001) and 12th month (OR 0.25, p < 0.001).
Conclusions
Our syntheses revealed higher PSM rates in the RS-RARP group, especially in the anterior aspect. However, RS-RARP had superior functional outcome of urinary continence and lower console time than did c-RARP with equivalent complication rates. Thus, we suggest that operators pay more attention to making clear surgical margins if the lesion is in anterior prostate when performing RS-RARP.




Similar content being viewed by others
Abbreviations
- CI:
-
Confidence interval
- c-RARP:
-
Conventional robot-assisted laparoscopic radical prostatectomy
- MD:
-
Mean difference
- OR:
-
Odds ratio
- RS-RARP:
-
Retzius space-sparing robot-assisted laparoscopic prostatectomy
- SD:
-
Standard deviation
- SE:
-
Standard error
References
Jemal A, Center MM, DeSantis C, Ward EM (2010) Global patterns of cancer incidence and mortality rates and trends. Cancer Epidemiol Biomark Prev 19:1893–1907
Mottet N, Bellmunt J, Bolla M, Briers E, Cumberbatch MG, De Santis M, Fossati N, Gross T, Henry AM, Joniau S, Lam TB, Mason MD, Matveev VB, Moldovan PC, van den Bergh RCN, Van den Broeck T, van der Poel HG, van der Kwast TH, Rouviere O, Schoots IG, Wiegel T, Cornford P (2017) EAU-ESTRO-SIOG Guidelines on Prostate Cancer. Part 1: screening, diagnosis, and local treatment with curative intent. Eur Urol 71:618–629
Schuessler WW, Schulam PG, Clayman RV, Kavoussi LR (1997) Laparoscopic radical prostatectomy: initial short-term experience. Urology 50:854–857
Guillonneau B, Vallancien G (2000) Laparoscopic radical prostatectomy: the Montsouris experience. J Urol 163:418–422
Tooher R, Swindle P, Woo H, Miller J, Maddern G (2006) Laparoscopic radical prostatectomy for localized prostate cancer: a systematic review of comparative studies. J Urol 175:2011–2017
Abbou CC, Hoznek A, Salomon L, Olsson LE, Lobontiu A, Saint F, Cicco A, Antiphon P, Chopin D (2001) Laparoscopic radical prostatectomy with a remote controlled robot. J Urol 165:1964–1966
Tewari A, Peabody J, Sarle R, Balakrishnan G, Hemal A, Shrivastava A, Menon M (2002) Technique of da Vinci robot-assisted anatomic radical prostatectomy. Urology 60:569–572
Jacobs EF, Boris R, Masterson TA (2013) Advances in robotic-assisted radical prostatectomy over time. Prostate Cancer 2013:902686
Galfano A, Ascione A, Grimaldi S, Petralia G, Strada E, Bocciardi AM (2010) A new anatomic approach for robot-assisted laparoscopic prostatectomy: a feasibility study for completely intrafascial surgery. Eur Urol 58:457–461
Galfano A, Di Trapani D, Sozzi F, Strada E, Petralia G, Bramerio M, Ascione A, Gambacorta M, Bocciardi AM (2013) Beyond the learning curve of the Retzius-sparing approach for robot-assisted laparoscopic radical prostatectomy: oncologic and functional results of the first 200 patients with ≥ 1 year of follow-up. Eur Urol 64:974–980
Hemal AK, Menon M (2018) Robotics in genitourinary surgery. Springer, Berlin
Asimakopoulos AD, Topazio L, De Angelis M, Agro EF, Pastore AL, Fuschi A, Annino F (2018) Retzius-sparing versus standard robot-assisted radical prostatectomy: a prospective randomized comparison on immediate continence rates. Surg Endosc 33(7):2187–2196
Chang LW, Hung SC, Hu JC, Chiu KY (2018) Retzius-sparing robotic-assisted radical prostatectomy associated with less bladder neck descent and better early continence outcome. Anticancer Res 38:345–351
Dalela D, Jeong W, Prasad MA, Sood A, Abdollah F, Diaz M, Karabon P, Sammon J, Jamil M, Baize B, Simone A, Menon M (2017) A pragmatic randomized controlled trial examining the impact of the Retzius-sparing approach on early urinary continence recovery after robot-assisted radical prostatectomy. Eur Urol 72:677–685
Menon M, Dalela D, Jamil M, Diaz M, Tallman C, Abdollah F, Sood A, Lehtola L, Miller D, Jeong W (2018) Functional recovery, oncologic outcomes and postoperative complications after robot-assisted radical prostatectomy: an evidence-based analysis comparing the Retzius sparing and standard approaches. J Urol 199:1210–1217
Sayyid RK, Simpson WG, Lu C, Terris MK, Klaassen Z, Madi R (2017) Retzius-sparing robotic-assisted laparoscopic radical prostatectomy: a safe surgical technique with superior continence outcomes. J Endourol 31:1244–1250
Stonier T, Simson N, Davis J, Challacombe B (2019) Retzius-sparing robot-assisted radical prostatectomy (RS-RARP) vs standard RARP: it’s time for critical appraisal. BJU Int 123:5–7
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med 151(264–269):w264
Chang SH, Kang YN, Chiu HY, Chiu YH (2018) A systematic review and meta-analysis comparing pigtail catheter and chest tube as the initial treatment for pneumothorax. Chest 153:1201–1212
Kao CC, Lin YS, Chu HC, Fang TC, Wu MS, Kang YN (2018) Association of renal function and direct-acting antiviral agents for HCV: a network meta-analysis. J Clin Med 7:314
Lin EY, Kuo YK, Kang YN (2018) Effects of three common lumbar interbody fusion procedures for degenerative disc disease: a network meta-analysis of prospective studies. Int J Surg (Lond, Engl) 60:224–230
Lin TM, Chi JE, Chang CC, Kang YN (2019) Do etoricoxib and indometacin have similar effects and safety for gouty arthritis? A meta-analysis of randomized controlled trials. J Pain Res 12:83–91
Chen LS, Chen WC, Kang YN, Wu CC, Tsai LW, Liu MZ (2019) Effects of transabdominal preperitoneal and totally extraperitoneal inguinal hernia repair: an update systematic review and meta-analysis of randomized controlled trials. Surg Endosc 33:418–428
Huang YJ, Kang YN, Huang YM, Wu AT, Wang W, Wei PL (2019) Effects of laparoscopic vs robotic-assisted mesorectal excision for rectal cancer: an update systematic review and meta-analysis of randomized controlled trials. Asian J Surg 42(6):657–666
Higgins JP, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, Savovic J, Schulz KF, Weeks L, Sterne JA, Cochrane Bias Methods G, Cochrane Statistical Methods G (2011) The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ (Clin Res Ed) 343:d5928
Stang A (2010) Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25:603–605
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ (Clin Res Ed) 327:557–560
Lim SK, Kim KH, Shin TY, Han WK, Chung BH, Hong SJ, Choi YD, Rha KH (2014) Retzius-sparing robot-assisted laparoscopic radical prostatectomy: combining the best of retropubic and perineal approaches. BJU Int 114:236–244
Eden CG, Moschonas D, Soares R (2018) Urinary continence four weeks following Retzius-sparing robotic radical prostatectomy: the UK experience. J Clin Urol 11:15–20
Koutlidis N, Duperron C, de la Vega MF, Mourey E, Michel F, Cormier L (2014) Capsular incision in normal prostatic tissue during robot-assisted radical prostatectomy: a new concept or a waste of time? World J Urol 32:1235–1240
Philippou Y, Harriss E, Davies L, Jubber I, Leslie T, Bell RW, Bryant RJ, Hamdy FC, Verill C, Lamb AD (2018) Prostatic capsular incision during radical prostatectomy has important oncological implications. A systematic review and meta-analysis. BJU Int. https://doi.org/10.1111/bju.14522
Kim LHC, Santok GD, Raheem AA, Alabdulaali I, Choi YD, Rha KH (2016) Incidence and location of positive surgical margin following Retzius-Sparing Robot-Assisted Radical Prostatectomy and its significance on oncological outcome. BJU Int 118:8
Dirie NI, Pokhrel G, Guan W, Mumin MA, Yang J, Masau JF, Hu H, Wang S (2018) Is Retzius-sparing robot-assisted radical prostatectomy associated with better functional and oncological outcomes? Literature review and meta-analysis. Asian J Urol 6(2):174–182
Acknowledgement
This manuscript was edited by Wallace Academic Editing.
Funding
No funding was requested for this systematic review and meta-analysis.
Author information
Authors and Affiliations
Contributions
TET conceptualized the study, screened the full text of the included studies, extracted the data, critically appraised the studies, drafted the manuscript, and approved the final manuscript; CCW interpreted the results, supervised the study, and approved the final manuscript; YNK designed the study, systematically searched the literature, screened the citations, extracted and analyzed the data, interpreted the results, drafted and critically revised the manuscript, and approved the final manuscript. JCW screened the full text of the included studies, checked the data, supervised the study, critically revised the manuscript, and approved the final manuscript.
Corresponding authors
Ethics declarations
Disclosures
Ting-En Tai, Chien-Chih Wu, Yi-No Kang, and Jeng-Cheng Wu have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Tai, TE., Wu, CC., Kang, YN. et al. Effects of Retzius sparing on robot-assisted laparoscopic prostatectomy: a systematic review with meta-analysis. Surg Endosc 34, 4020–4029 (2020). https://doi.org/10.1007/s00464-019-07190-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-019-07190-2