Abstract
Background
The management of contralateral patent processus vaginalis (CPPV) in children with unilateral inguinal hernia is still controversial. The objective of this study was to verify the relationship between metachronous contralateral inguinal hernia (MCIH) and CPPV, and the risk factors of MCIH.
Methods
Children with unilateral inguinal hernia from three medical centers underwent either open or laparoscopic repairs. Clinical information, including demographics, morphological characteristics of CPPV, follow-up outcomes were collected.
Results
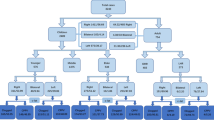
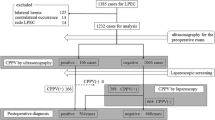
Among 2942 patients (92.2%) who received open repair with successful follow-up, 185 (6.29%) developed MCIHs [125 (10.9%) on the right side and 60 (3.3%)] on the left including 156 (7.07%) younger than 3 years old and 29 (3.94%) older than 3 years old. Patients younger than 3 years old with primary left inguinal hernias more easily develop MCIHs and the difference is statistically significant. Among 5370 patients (96.0%) who received laparoscopic repair with successful follow-up, the morphology of ipsilateral patent processus vaginalis were cavernous type in 5318 (99%) and 52 (1%) were fissure type. CPPVs were identified in 2233 (41.5%) cases [1256 (35.01%) on the left side and 977 (54.80%) on the right side, P < 0.001]; 1503 cases were cavernous type (1276 cases younger than 3 years old and 227 cases older than 3 years old) and 730 cases were fissure type (422 cases younger than 3 years old and 308 cases older than 3 years old). The probability of occurence of cavernous type and CPPV in children younger than 3 years old was higher than that in children older than 3 years old.
Conclusions
Not all CPPVS progress into an MIH, and approximate one of 15 CPPVs would progress into MIH. If patient with initial left-sided inguinal hernia is younger than 3 years old, when the morphology of CPPV is cavernous type identified by laparoscopic exploration, the contralateral repair would be recommended.

Similar content being viewed by others
References
Kokorowski PJ, Wang HHS, Routh JC, Hubert KC, Nelson CP (2014) Evaluation of the contralateral inguinal ring in clinically unilateral inguina: a systematic review and meta-analysis. Hernia 18:311–324
Nataraja RM, Mahomed AA (2011) Systematic review for paediatric metachronous contralateral inguinal hernia: a decreasing concern. Pediatr Surg Int 27:953–961
Muensterer OJ, Woller T, Metzger R, Till H (2008) The economics of contralateral laparoscopic inguinal hernia exploration. Cost calculation of herniotomy in infants. Chirurg 79:1065–1071
Wenk K, Sick B, Sasse T, Moehrlen U, Meuli M (2015) Incidence of metachronous contralateral inguinal hernias in children following unilateral repair—a meta-analysis of prospective studies. J Pediatr Surg 50:2147–2154
Ikeda H, Suzuki N, Takahashi A, Kuroiwa M, Sakai M, Tsuchida Y (2000) Risk of contralateral manifestation in children with unilateral inguinal hernia: should hernia in children be treated contralaterally? J Pediatr Surg 35:1746–1748
Tackett LD, Breuer CK, Luks FI, Caldamone AA, Breuer JG, DeLuca FG, Caesar RE, Efthemiou E, Wesselhoeft CW (1999) Incidence of contralateral inguinal: a prospective analysis. J Pediatr Surg 34:684–687
Lee DG, Lee YS, Park KH, Baek M (2015) Risk factors for contralateral patent processus vaginalis determined by transinguinal laparoscopic examination. Exp Ther Med 9:421–424
Wu CC, Chueh SC, Tsai YC (2016) Is contralateral exploration justified in endoscopic total extraperitoneal repair of clinical unilateral groin hernias—a prospective cohort study. Int J Surg 36:206–211
Lee CH, Chen Y, Cheng CF, Yao CL, Wu JC, Yin WY, Chen JH (2016) - Incidence of and risk factors for pediatric metachronous contralateral inguinal hernia: a prospective analysis of a 17-year nationwide database in Taiwan. PloS one 11:0163278
Jallouli M, Yaich S, Dhaou MB, Yengui H, Trigui D, Damak J, Mhiri R (2009) Are there any predictive factors of metachronous inguinal hernias in children with unilateral inguinal hernia. Hernia 13:613–615
Hoshino M, Sugito K, Kawashima H, Goto S, Kaneda H, Furuya T, Hosoda T, Masuko T, Ohashi K, Inoue M, Ikeda T, Tomita R, Koshinaga T (2014) Prediction of contralateral inguinal hernias in children: a prospective study of 357 unilateral inguinal hernias. Hernia 18:333–337
Rowe MI, Copelson LW, Clatworthy HW (1969) The patent processus vaginalis and the inguinal hernia. J Pediatr Surg 4:102–107
Rathauser F (1985) Historical overview of the bilateral approach to pediatric inguinal hernias. Am J Surg 150:527–532
Zhong H, Wang F (2014) Contralateral metachronous hernia following negative laparoscopic evaluation for contralateral patent processus vaginalis: a meta-analysis. J Laparoendosc Adv Surg Tech A 24:111–116
Zamakhshardy M, Ein A, Ein SH, Wales PW (2009) Predictors of metachronous inguinal hernias in children. Pediatr Surg Int 25:69–71
Funding
This project was supported by grants from the National Natural Science Foundation of China (Grants 81401606) and the Science Foundation for The Excellent Youth Scholars of Sichuan University (2015SU04A15).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Yanan Li, Yang Wu, Chuan Wang, Qi Wang, Yiyang Zhao, Yi Ji, and Bo Xiang have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Li, Y., Wu, Y., Wang, C. et al. Incidence of pediatric metachronous contralateral inguinal hernia and the relationship with contralateral patent processus vaginalis. Surg Endosc 33, 1087–1090 (2019). https://doi.org/10.1007/s00464-018-6359-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-018-6359-x