Abstract
Background
To determine whether laparoscopic surgery can be used in high-risk patients with gastric cancer.
Methods
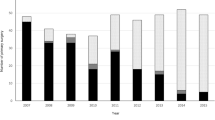
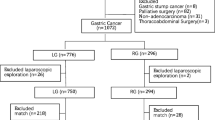
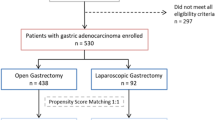
The clinicopathological data of 3743 patients with primary gastric adenocarcinoma, collected from January 2007 to December 2014, were retrospectively analyzed. Patients who had ≥ 1 of the following conditions were defined as high-risk patients: (1) age ≥ 80 years; (2) BMI ≥ 30 kg/m2; (3) ASA (American Society of Anesthesiologists) grade ≥ 3; or (4) clinical T stage 4 (cT4). Propensity score matching (PSM) was used to reduce confounding bias; then, we compared the short-term and long-term efficacy of laparoscopic gastrectomy (LG) with open gastrectomy (OG) in high-risk patients with gastric cancer.
Results
A total of 1296 patients were included in PSM. After PSM, no significant difference in clinicopathological data was observed between the LG group (n = 341) and the OG group (n = 341). The operative time (181.70 vs. 266.71 min, p < 0.001) and blood loss during the operation (68.11 vs. 225.54 ml, p < 0.001) in the LG group were significantly lower than those in the OG group. In the LG and OG groups, postoperative complications occurred in 39 (11.4%) and 63 (18.5%) patients, respectively, p = 0.010. Multivariate analysis showed that laparoscopic surgery was an independent protective factor against postoperative complications (p = 0.019). The number of risk factors was an independent risk factor for postoperative complications (p = 0.021). The 5-year overall survival rate in the LG group was comparable to that in the OG group (55.0 vs. 52.0%, p = 0.086). Hierarchical analysis further confirmed that the LG and OG groups exhibited comparable survival rates among patients with stages cI, pI, cII, pII, cIII, and pIII (all p > 0.05).
Conclusions
For high-risk patients with gastric cancer, LG not only exhibits better short-term efficacy than OG but also has a comparable 5-year survival rate to OG.



Similar content being viewed by others
References
Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A (2015) Global cancer statistics, 2012. CA Cancer J Clin 65:87–108
Kitano S, Iso Y, Moriyama M, Sugimachi K (1994) Laparoscopy-assisted Billroth I gastrectomy. Surg Laparosc Endosc 4:146–148
Kawamura H, Okada K, Isizu H, Masuko H, Yamagami H, Honma S, Ueki S, Noguchi K, Kondo Y (2008) Laparoscopic gastrectomy for early gastric cancer targeting as a less invasive procedure. Surg Endosc 22:81–85
Katai H, Mizusawa J, Katayama H, Takagi M, Yoshikawa T, Fukagawa T, Terashima M, Misawa K, Teshima S, Koeda K, Nunobe S, Fukushima N, Yasuda T, Asao Y, Fujiwara Y, Sasako M (2016) Short-term surgical outcomes from a phase III study of laparoscopy-assisted versus open distal gastrectomy with nodal dissection for clinical stage IA/IB gastric cancer: Japan Clinical Oncology Group Study JCOG0912. Gastric Cancer 20:699–708
Hu Y, Huang C, Sun Y, Su X, Cao H, Hu J, Xue Y, Suo J, Tao K, He X, Wei H, Ying M, Hu W, Du X, Chen P, Liu H, Zheng C, Liu F, Yu J, Li Z, Zhao G, Chen X, Wang K, Li P, Xing J, Li G (2016) Morbidity and mortality of laparoscopic versus open D2 distal gastrectomy for advanced gastric cancer: a randomized controlled trial. J Clin Oncol 34:1350–1357
Lee JH, Han HS, Lee JH (2005) A prospective randomized study comparing open vs laparoscopy-assisted distal gastrectomy in early gastric cancer: early results. Surg Endosc 19:168–173
Hayashi H, Ochiai T, Shimada H, Gunji Y (2005) Prospective randomized study of open versus laparoscopy-assisted distal gastrectomy with extraperigastric lymph node dissection for early gastric cancer. Surg Endosc 19:1172–1176
Kitano S, Shiraishi N, Uyama I, Sugihara K, Tanigawa N, Japanese Laparoscopic Surgery Study G (2007) A multicenter study on oncologic outcome of laparoscopic gastrectomy for early cancer in Japan. Ann Surg 245:68–72
Kim MC, Kim W, Kim HH, Ryu SW, Ryu SY, Song KY, Lee HJ, Cho GS, Han SU, Hyung WJ, Korean Laparoscopic Gastrointestinal Surgery Study G (2008) Risk factors associated with complication following laparoscopy-assisted gastrectomy for gastric cancer: a large-scale korean multicenter study. Ann Surg Oncol 15:2692–2700
Takeshita H, Ichikawa D, Komatsu S, Kubota T, Okamoto K, Shiozaki A, Fujiwara H, Otsuji E (2013) Surgical outcomes of gastrectomy for elderly patients with gastric cancer. World J Surg 37:2891–2898
Gretschel S, Estevez-Schwarz L, Hunerbein M, Schneider U, Schlag PM (2006) Gastric cancer surgery in elderly patients. World J Surg 30:1468–1474
Topal B, Leys E, Ectors N, Aerts R, Penninckx F (2007) Determinants of complications and adequacy of surgical resection in laparoscopic versus open total gastrectomy for adenocarcinoma. Surg Endosc 22:980–984
Kunisaki C, Makino H, Takagawa R, Oshima T, Nagano Y, Ono HA, Akiyama H, Shimada H (2009) Efficacy of laparoscopy-assisted distal gastrectomy for gastric cancer in the elderly. Surg Endosc 23:377–383
Pikarsky AJ, Saida Y, Yamaguchi T, Martinez S, Chen W, Weiss EG, Nogueras JJ, Wexner SD (2002) Is obesity a high-risk factor for laparoscopic colorectal surgery? Surg Endosc 16:855–858
Bittner R, Butters M, Ulrich M, Uppenbrink S, Beger HG (1996) Total gastrectomy. Updated operative mortality and long-term survival with particular reference to patients older than 70 years of age. Ann Surg 224:37–42
Huang CM, Tu RH, Lin JX, Zheng CH, Li P, Xie JW, Wang JB, Lu J, Chen QY, Cao LL, Lin M (2015) A scoring system to predict the risk of postoperative complications after laparoscopic gastrectomy for gastric cancer based on a large-scale retrospective study. Medicine 94:e812
Wu XS, Wu WG, Li ML, Yang JH, Ding QC, Zhang L, Mu JS, Gu J, Dong P, Lu JH, Liu YB (2013) Impact of being overweight on the surgical outcomes of patients with gastric cancer: a meta-analysis. World journal of gastroenterology 19:4596–4606
Fujisaki M, Shinohara T, Hanyu N, Kawano S, Tanaka Y, Watanabe A, Yanaga K (2016) Laparoscopic gastrectomy for gastric cancer in the elderly patients. Surg Endosc 30:1380–1387
Tu R-H, Huang C-M, Lin J-X, Chen Q-Y, Zheng C-H, Li P, Xie J-W, Wang J-B, Lu J, Cao L-L, Lin M (2015) A scoring system to predict the risk of organ/space surgical site infections after laparoscopic gastrectomy for gastric cancer based on a large-scale retrospective study. Surg Endosc 30:3026–3034
Frasson M, Braga M, Vignali A, Zuliani W, Di Carlo V (2008) Benefits of laparoscopic colorectal resection are more pronounced in elderly patients. Dis Colon Rectum 51:296–300
Kelly T, Yang W, Chen CS, Reynolds K, He J (2008) Global burden of obesity in 2005 and projections to 2030. Int J Obes 32:1431–1437
Hemandas AK, Abdelrahman T, Flashman KG, Skull AJ, Senapati A, O’Leary DP, Parvaiz A (2010) Laparoscopic colorectal surgery produces better outcomes for high risk cancer patients compared to open surgery. Ann Surg 252:84–89
Wang J, Zhang L, Huang Q, Wu G, Weng X, Lai Z, Lin P (2017) Monitoring the end-tidal concentration of sevoflurane for preventing awareness during anesthesia (MEETS-PANDA): a prospective clinical trial. Int J Surg 41:44–49
Washington K (2010) 7th edition of the AJCC cancer staging manual: stomach. Ann Surg Oncol 17:3077–3079
Lin JX, Huang CM, Zheng CH, Li P, Xie JW, Wang JB, Jun L, Chen QY, Cao LL, Lin M (2016) Is all advanced gastric cancer suitable for laparoscopy-assisted gastrectomy with extended lymphadenectomy? A case-control study using a propensity score method. Ann Surg Oncol 23:1252–1260
Wang JB, Zheng CH, Li P, Xie JW, Lin JX, Lu J, Chen QY, Cao LL, Lin M, Huang CM (2017) Effect of comorbidities on postoperative complications in patients with gastric cancer after laparoscopy-assisted total gastrectomy: results from an 8-year experience at a large-scale single center. Surg Endosc 31:2651–2660
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Annals of surgery 240:205–213
Kim W, Kim HH, Han SU, Kim MC, Hyung WJ, Ryu SW, Cho GS, Kim CY, Yang HK, Park DJ, Song KY, Lee SI, Ryu SY, Lee JH, Lee HJ (2016) Decreased morbidity of laparoscopic distal gastrectomy compared with open distal gastrectomy for stage I gastric cancer: short-term outcomes from a multicenter randomized controlled trial (KLASS-01). Ann Surg 263:28–35
Shinohara T, Satoh S, Kanaya S, Ishida Y, Taniguchi K, Isogaki J, Inaba K, Yanaga K, Uyama I (2013) Laparoscopic versus open D2 gastrectomy for advanced gastric cancer: a retrospective cohort study. Surg Endosc 27:286–294
Tan PY, Stephens JH, Rieger NA, Hewett PJ (2008) Laparoscopically assisted colectomy: a study of risk factors and predictors of open conversion. Surg Endosc 22:1708–1714
Gerges FJ, Kanazi GE, Jabbour-Khoury SI (2006) Anesthesia for laparoscopy: a review. J Clin Anesth 18:67–78
Poon JT, Law WL, Chow LC, Fan JK, Lo SH (2011) Outcome of laparoscopic resection for colorectal cancer in patients with high operative risk. Ann Surg Oncol 18:1884–1890
Feroci F, Baraghini M, Lenzi E, Garzi A, Vannucchi A, Cantafio S, Scatizzi M (2012) Laparoscopic surgery improves postoperative outcomes in high-risk patients with colorectal cancer. Surg Endosc 27:1130–1137
Ening G, Osterheld F, Capper D, Schmieder K, Brenke C (2015) Charlson comorbidity index: an additional prognostic parameter for preoperative glioblastoma patient stratification. J Cancer Res Clin Oncol 141:1131–1137
Dell’Oglio P, Tian Z, Leyh-Bannurah S, Trudeau V, Larcher A, Moschini M, Di Trapani E, Capitanio U, Briganti A, Montorsi F, Saad F, Karakiewicz P (2017) Short-form Charlson Comorbidity index for assessment of perioperative mortality after radical cystectomy. J Natl Compr Cancer Netw 15:327–333
Musri FY, Mutlu H, Karaagac M, Eryilmaz MK, Gunduz S, Artac M (2016) Primary tumor resection and survival in patients with stage IV gastric cancer. J Gastric Cancer 16:78–84
Claassen YHM, Hartgrink HH, Dikken JL, de Steur WO, van Sandick JW, van Grieken NCT, Cats A, Trip AK, Jansen EPM, Kranenbarg WMMK, Braak J, Putter H, van Berge Henegouwen MI, Verheij M, van de Velde CJH (2018) Surgical morbidity and mortality after neoadjuvant chemotherapy in the CRITICS gastric cancer trial. Eur J Surg Oncol 44:613–619
Jiang L, Yang KH, Guan QL, Chen Y, Zhao P, Tian JH (2015) Survival benefit of neoadjuvant chemotherapy for resectable cancer of the gastric and gastroesophageal junction: a meta-analysis. J Clin Gastroenterol 49:387–394
Hu Y, Ying M, Huang C, Wei H, Jiang Z, Peng X, Hu J, Du X, Wang B, Lin F, Xu J, Dong G, Mou T, Li G, Chinese Laparoscopic Gastrointestinal Surgery Study G (2014) Oncologic outcomes of laparoscopy-assisted gastrectomy for advanced gastric cancer: a large-scale multicenter retrospective cohort study from China. Surg Endosc 28:2048–2056
Wang D, Kong Y, Zhong B, Zhou X, Zhou Y (2010) Fast-track surgery improves postoperative recovery in patients with gastric cancer: a randomized comparison with conventional postoperative care. J Gastrointest Surg 14:620–627
Li Y-j, Huo T-t, Xing J, An J-z, Han Z-y, Liu X-n, Zhao Q-c (2014) Meta-analysis of efficacy and safety of fast-track surgery in gastrectomy for gastric cancer. World J Surg 38:3142–3151
Kim JW, Kim WS, Cheong JH, Hyung WJ, Choi SH, Noh SH (2012) Safety and efficacy of fast-track surgery in laparoscopic distal gastrectomy for gastric cancer: a randomized clinical trial. World J Surg 36:2879–2887
Acknowledgements
This work was supported by the Scientific and technological innovation joint capital projects of Fujian Province (2016Y9031). Construction Project of Fujian Province Minimally Invasive Medical Center (No. [2017]171). The second batch of special support funds for Fujian Province innovation and entrepreneurship talents (2016B013). Startup Fund for scientific research, Fujian Medical University (Grant Number: 2016QH024). Fujian province medical innovation project (2015-CXB-16). Fujian provincial health and family planning commission joint project (WKJ2016-2-27). Chinese physicians association young physician respiratory research fund.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosures
Drs. Bin-bin Xu, Jun Lu, Zhi-fang Zheng, Jian-wei Xie, Jia-bin Wang, Jian-xian Lin, Qi-yue Chen, Long–long Cao, Mi Lin, Ru-hong Tu, Ze-ning Huang, Ju-li Lin, Chao-hui Zheng, Ping Li, and Chang-ming Huang have no conflicts of interest or financial ties to disclose.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Xu, Bb., Lu, J., Zheng, Zf. et al. Comparison of short-term and long-term efficacy of laparoscopic and open gastrectomy in high-risk patients with gastric cancer: a propensity score-matching analysis. Surg Endosc 33, 58–70 (2019). https://doi.org/10.1007/s00464-018-6268-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-018-6268-z