Abstract
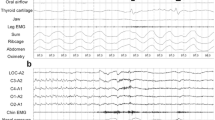
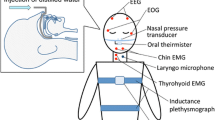
The objectives of this study are to investigate swallowing and its coordination with respiration in patients with obstructive sleep apnea (OSA). This is a prospective cohort study conducted in a tertiary referred Medical Center. A non-invasive method of assessing swallowing was used to detect the oropharyngeal swallowing parameters and the coordination with respiration during swallowing. The system used to assess swallowing detected: (1) movement of the larynx using a force-sensing resistor; (2) submental muscle activity using surface electromyography; and (3) coordination with respiration by measuring nasal airflow. Five sizes of water boluses (maximum 20 mL) were swallowed three times, and the data recorded and analyzed for each participant. Thirty-nine normal controls and 35 patients with OSA who fulfilled the inclusion criteria were recruited. The oropharyngeal swallowing parameters of the patients differed from the controls, including longer total excursion duration and shorter duration of submental muscles contraction. A longer swallowing respiratory pause (SRP), temporary coordination with respiration during swallowing, was demonstrated in the patients compared with the controls. The frequency of non-expiratory/expiratory pre- and postswallowing respiratory phase patterns of the patients was similar with the controls. There was significantly more piecemeal deglutition in OSA patients when clumping 10- and 20-mL water boluses swallowing together (p = 0.048). Oropharyngeal swallowing and coordination with respiration affected patients with OSA, and it could be detected using a non-invasive method. The results of this study may serve as a baseline for further research and help advance research methods in obstructive sleep apnea swallowing studies.




Similar content being viewed by others
References
Ferini-Strambi L, Fantini ML, Castronovo C. Epidemiology of obstructive sleep apnea syndrome. Minerva Med. 2004;95(3):187–202.
Sleep-related breathing disorders in adults: recommendations for syndrome definition and measurement techniques in clinical research. The Report of an American Academy of Sleep Medicine Task Force. Sleep. 1999;22 (5):667–9.
Chuang LP, Hsu SC, Lin SW, Ko WS, Chen NH, Tsai YH. Prevalence of snoring and witnessed apnea in Taiwanese adults. Chang Gung Med J. 2008;31(2):175–81.
Fleisher KE, Krieger AC. Current trends in the treatment of obstructive sleep apnea. J Oral Maxillofac Surg. 2007;65(10):2056–68. doi:10.1016/j.joms.2006.11.058.
Friberg D, Gazelius B, Hokfelt T, Nordlander B. Abnormal afferent nerve endings in the soft palatal mucosa of sleep apnoics and habitual snorers. Regul Pept. 1997;71(1):29–36.
Friberg D, Gazelius B, Lindblad LE, Nordlander B. Habitual snorers and sleep apnoics have abnormal vascular reactions of the soft palatal mucosa on afferent nerve stimulation. Laryngoscope. 1998;108(3):431–6.
Jobin V, Champagne V, Beauregard J, Charbonneau I, McFarland DH, Kimoff RJ. Swallowing function and upper airway sensation in obstructive sleep apnea. J Appl Physiol. 2007;102(4):1587–94. doi:10.1152/japplphysiol.00439.2006.
Valbuza JS, de Oliveira MM, Conti CF, Prado LB, Carvalho LB, do Prado GF. Oropharyngeal examination as a predictor of obstructive sleep apnea: pilot study of gag reflex and palatal reflex. Arq Neuropsiquiatr. 2011;69(5):805–8.
Teramoto S, Ishii T, Matsuse T. Relationship between swallowing function and gas exchange during day and night in patients with obstructive sleep apnea syndrome. Dysphagia. 2001;16(4):249–53.
Valbuza JS, de Oliveira MM, Zancanella E, Conti CF, Prado LB, Carvalho LB, GE Prado do. Swallowing dysfunction related to obstructive sleep apnea: a nasal fibroscopy pilot study. Sleep Breath. 2011;15(2):209–13. doi:10.1007/s11325-010-0474-9.
Hiss SG, Strauss M, Treole K, Stuart A, Boutilier S. Swallowing apnea as a function of airway closure. Dysphagia. 2003;18(4):293–300. doi:10.1007/s00455-003-0021-y.
Davenport PW, Bolser DC, Morris KF. Swallow remodeling of respiratory neural networks. Head Neck. 2011;33(Suppl 1):S8–13. doi:10.1002/hed.21845.
Broussard DL, Altschuler SM. Central integration of swallow and airway-protective reflexes. Am J Med. 2000;108(Suppl 4a):62s–7s.
Barlow SM. Oral and respiratory control for preterm feeding. Curr Opin Otolaryngol Head Neck Surg. 2009;17(3):179–86. doi:10.1097/MOO.0b013e32832b36fe.
Jafari S, Prince RA, Kim DY, Paydarfar D. Sensory regulation of swallowing and airway protection: a role for the internal superior laryngeal nerve in humans. J Physiol. 2003;550(Pt 1):287–304. doi:10.1113/jphysiol.2003.039966.
Bolser DC, Pitts TE, Morris KF. The use of multiscale systems biology approaches to facilitate understanding of complex control systems for airway protection. Curr Opin Pharmacol. 2011;11(3):272–7. doi:10.1016/j.coph.2011.06.002.
Martin-Harris B, Brodsky MB, Michel Y, Ford CL, Walters B, Heffner J. Breathing and swallowing dynamics across the adult lifespan. Arch Otolaryngol Head Neck Surg. 2005;131(9):762–70. doi:10.1001/archotol.131.9.762.
Martin-Harris B, Brodsky MB, Price CC, Michel Y, Walters B. Temporal coordination of pharyngeal and laryngeal dynamics with breathing during swallowing: single liquid swallows. J Appl Physiol. 2003;94(5):1735–43. doi:10.1152/japplphysiol.00806.2002.
Paydarfar D, Gilbert RJ, Poppel CS, Nassab PF. Respiratory phase resetting and airflow changes induced by swallowing in humans. J Physiol. 1995;483(Pt 1):273–88.
Wilson SL, Thach BT, Brouillette RT, Abu-Osba YK. Coordination of breathing and swallowing in human infants. J Appl Physiol Respir Environ Exerc Physiol. 1981;50(4):851–8.
Hiss SG, Treole K, Stuart A. Effects of age, gender, bolus volume, and trial on swallowing apnea duration and swallow/respiratory phase relationships of normal adults. Dysphagia. 2001;16(2):128–35.
Selley WG, Flack FC, Ellis RE, Brooks WA. The exeter dysphagia assessment technique. Dysphagia. 1990;4(4):227–35.
Selley WG, Ellis RE, Flack FC, Bayliss CR, Pearce VR. The synchronization of respiration and swallow sounds with videofluoroscopy during swallowing. Dysphagia. 1994;9(3):162–7.
Ertekin C, Pehlivan M, Aydogdu I, Ertas M, Uludag B, Celebi G, Colakoglu Z, Sagduyu A, Yuceyar N. An electrophysiological investigation of deglutition in man. Muscle Nerve. 1995;18(10):1177–86. doi:10.1002/mus.880181014.
Ertekin C, Aydogdu I, Yuceyar N, Tarlaci S, Kiylioglu N, Pehlivan M, Celebi G. Electrodiagnostic methods for neurogenic dysphagia. Electroencephalogr Clin Neurophysiol. 1998;109(4):331–40.
Terzi N OD, Prigent H, Denise P, Normand H, Lofaso F. Noninvasive monitoring of breathing and swallowing interaction. In: EMG Methods for evaluating muscle and nerve function. 2012. http://www.intechopencom/download/pdf/25870chap21. doi:10.5772/25779.
Wang CM, Chen JY, Chuang CC, Tseng WC, Wong AM, Pei YC. Aging-related changes in swallowing, and in the coordination of swallowing and respiration determined by novel non-invasive measurement techniques. Geriatr Gerontol Int. 2015;15(6):736–44. doi:10.1111/ggi.12343.
Li Q, Hori K, Minagi Y, Ono T, Chen YJ, Kondo J, Fujiwara S, Tamine K, Hayashi H, Inoue M, Maeda Y. Development of a system to monitor laryngeal movement during swallowing using a bend sensor. PLoS One. 2013;8(8):e70850. doi:10.1371/journal.pone.0070850.
Shieh WY, Wang CM, Chang CS. Development of a portable non-invasive swallowing and respiration assessment device. Sensors (Basel). 2015;15(6):12428–53. doi:10.3390/s150612428.
Chen NH, Johns MW, Li HY, Chu CC, Liang SC, Shu YH, Chuang ML, Wang PC. Validation of a Chinese version of the epworth sleepiness scale. Qual Life Res. 2002;11(8):817–21.
Chen NH, Li HY, Gliklich RE, Chu CC, Liang SC, Wang PC. Validation assessment of the Chinese version of the snore outcomes survey. Qual Life Res. 2002;11(6):601–7.
Wang CM, Shieh WY, Chen JY, Wu YR. Integrated non-invasive measurements reveal swallowing and respiration coordination recovery after unilateral stroke. Neurogastroenterol Motil. 2015. doi:10.1111/nmo.12634.
Aydogdu I, Tanriverdi Z, Ertekin C. Dysfunction of bulbar central pattern generator in ALS patients with dysphagia during sequential deglutition. Clin Neurophysiol. 2011;122(6):1219–28. doi:10.1016/j.clinph.2010.11.002.
Wang CMCC, Chen CPC, Tseng WC, Chen JY. Noninvasive swallowing test for young healthy adults: finding the best location to monitor thyroid cartilage movements. J Med Biol Eng. 2014;34:393–8.
Ertekin C, Celik M, Secil Y, Tarlaci S, Kiyloglu N, Aydogdu I. The electromyographic behavior of the thyroarytenoid muscle during swallowing. J Clin Gastroenterol. 2000;30(3):274–80.
Ueda N, Nohara K, Kotani Y, Tanaka N, Okuno K, Sakai T. Effects of the bolus volume on hyoid movements in normal individuals. J Oral Rehabil. 2013;40(7):491–9. doi:10.1111/joor.12060.
Nagy A, Molfenter SM, Peladeau-Pigeon M, Stokely S, Steele CM. The effect of bolus volume on hyoid kinematics in healthy swallowing. Biomed Res Int. 2014;2014:738971. doi:10.1155/2014/738971.
Steele CM, Bailey GL, Chau T, Molfenter SM, Oshalla M, Waito AA, Zoratto DC. The relationship between hyoid and laryngeal displacement and swallowing impairment. Clin Otolaryngol. 2011;36(1):30–6. doi:10.1111/j.1749-4486.2010.02219.x.
Yokoyama M, Mitomi N, Tetsuka K, Tayama N, Niimi S. Role of laryngeal movement and effect of aging on swallowing pressure in the pharynx and upper esophageal sphincter. Laryngoscope. 2000;110(3 Pt 1):434–9. doi:10.1097/00005537-200003000-00021.
Li Q, Minagi Y, Hori K, Kondoh J, Fujiwara S, Tamine K, Inoue M, Maeda Y, Chen Y, Ono T. Coordination in oro-pharyngeal biomechanics during human swallowing. Physiol Behav. 2015;147:300–5. doi:10.1016/j.physbeh.2015.05.004.
Costa MM, Lemme EM. Coordination of respiration and swallowing: functional pattern and relevance of vocal folds closure. Arq Gastroenterol. 2010;47(1):42–8.
Boden K, Cedborg AI, Eriksson LI, Hedstrom HW, Kuylenstierna R, Sundman E, Ekberg O. Swallowing and respiratory pattern in young healthy individuals recorded with high temporal resolution. Neurogastroenterol Motil. 2009;21(11):1163. doi:10.1111/j.1365-2982.2009.01352.x.
Brodsky MB, McFarland DH, Dozier TS, Blair J, Ayers C, Michel Y, Gillespie MB, Day TA, Martin-Harris B. Respiratory-swallow phase patterns and their relationship to swallowing impairment in patients treated for oropharyngeal cancer. Head Neck. 2010;32(4):481–9. doi:10.1002/hed.21209.
Charbonneau I, Lund JP, McFarland DH. Persistence of respiratory-swallowing coordination after laryngectomy. J Speech Lang Hear Res. 2005;48(1):34–44.
Hiss SG, Strauss M, Treole K, Stuart A, Boutilier S. Effects of age, gender, bolus volume, bolus viscosity, and gustation on swallowing apnea onset relative to lingual bolus propulsion onset in normal adults. J Speech Lang Hear Res. 2004;47(3):572–83. doi:10.1044/1092-4388(2004/044).
Kendall KA, Leonard RJ, McKenzie S. Airway protection: evaluation with videofluoroscopy. Dysphagia. 2004;19(2):65–70.
Ertekin C, Aydogdu I, Yuceyar N. Piecemeal deglutition and dysphagia limit in normal subjects and in patients with swallowing disorders. J Neurol Neurosurg Psychiatry. 1996;61(5):491–6.
Feinberg MJ, Knebl J, Tully J, Segall L. Aspiration and the elderly. Dysphagia. 1990;5(2):61–71.
Martino R, Foley N, Bhogal S, Diamant N, Speechley M, Teasell R. Dysphagia after stroke: incidence, diagnosis, and pulmonary complications. Stroke. 2005;36(12):2756–63. doi:10.1161/01.STR.0000190056.76543.eb.
Esteves GP, Silva Junior EP, Nunes LG, Greco CS, Melo PL. Configurable portable/ambulatory instrument for the analysis of the coordination between respiration and swallowing. Conf Proc IEEE Eng Med Biol Soc. 2010;2010:90–3. doi:10.1109/iembs.2010.5626157.
Huckabee ML, Butler SG, Barclay M, Jit S. Submental surface electromyographic measurement and pharyngeal pressures during normal and effortful swallowing. Arch Phys Med Rehabil. 2005;86(11):2144–9. doi:10.1016/j.apmr.2005.05.005.
Reyes A, Cruickshank T, Thompson J, Ziman M, Nosaka K. Surface electromyograph activity of submental muscles during swallowing and expiratory muscle training tasks in Huntington’s disease patients. J Electromyogr Kinesiol. 2014;24(1):153–8. doi:10.1016/j.jelekin.2013.09.009.
Kim HR, Lee SA, Kim K, Leigh JH, Han TR, Oh BM. Submental muscle activity is delayed and shortened during swallowing following stroke. PM R. 2015;7(9):938–45. doi:10.1016/j.pmrj.2015.05.018.
Miller AJ. Neurophysiological basis of swallowing. Dysphagia. 1986;1:91–100.
Jean A. Brainstem control of swallowing: localization and organization of the central pattern generator for swallowing. In: Taylor A, editor. Neurophysiology of the jaws and teeth. London: McMillan Press; 1990. pp. 294–321.
Sato K, Umeno H, Chitose S, Nakashima T. Sleep-related deglutition in patients with OSAHS under CPAP therapy. Acta Otolaryngol. 2011;131(2):181–9. doi:10.3109/00016489.2010.520166.
Arici S, Gurgor N, Secil Y, Peker S, Incesu TK, Ozdemirkiran T, Tokucoglu F, Ce P, Celebisoy M, Ertekin C. P10.15 Oropharyngeal swallowing and obstructive sleep apnea syndrome. Clin Neurophysiol. 2011;122(supplement 1):S108. doi:10.1016/S1388-2457(11)60382-9.
Gurgor N, Arici S, Kurt Incesu T, Secil Y, Tokucoglu F, Ertekin C. An electrophysiological study of the sequential water swallowing. J Electromyogr Kinesiol. 2013;23(3):619–26. doi:10.1016/j.jelekin.2012.12.003.
Beckmann Y, Gurgor N, Cakir A, Arici S, Incesu TK, Secil Y, Ertekin C. Electrophysiological evaluation of dysphagia in the mild or moderate patients with multiple sclerosis: a concept of subclinical dysphagia. Dysphagia. 2015;30(3):296–303. doi:10.1007/s00455-015-9598-1.
Aydogdu I, Kiylioglu N, Tarlaci S, Tanriverdi Z, Alpaydin S, Acarer A, Baysal L, Arpaci E, Yuceyar N, Secil Y, Ozdemirkiran T, Ertekin C. Diagnostic value of “dysphagia limit” for neurogenic dysphagia: 17 years of experience in 1278 adults. Clin Neurophysiol. 2014;. doi:10.1016/j.clinph.2014.06.035.
Troche MS, Huebner I, Rosenbek JC, Okun MS, Sapienza CM. Respiratory-swallowing coordination and swallowing safety in patients with Parkinson’s disease. Dysphagia. 2011;26(3):218–24. doi:10.1007/s00455-010-9289-x.
Martin-Harris B. Clinical implications of respiratory-swallowing interactions. Curr Opin Otolaryngol Head Neck Surg. 2008;16(3):194–9. doi:10.1097/MOO.0b013e3282febd4b.
Rugiu MG. Role of videofluoroscopy in evaluation of neurologic dysphagia. Acta Otorhinolaryngol Ital. 2007;27(6):306–16.
Bastian RW. The videoendoscopic swallowing study: an alternative and partner to the videofluoroscopic swallowing study. Dysphagia. 1993;8(4):359–67.
Acknowledgments
This study was supported by Grants from the National Science Council, Taiwan (NSC-101-2314-B-182A-007-MY2) and Chang Gung Memorial Hospital, Taiwan (CMRPG5C0023).
Funding
The study was financially supported by Grants from the National Science Council, Taiwan (NSC-101-2314-B-182A-007-MY2) and Chang Gung Memorial Hospital, Taiwan (CMRPG5C0023).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors have no other funding, financial relationships, or conflicts of interest to disclose.
Rights and permissions
About this article
Cite this article
Wang, CM., Li, HY., Lee, L.A. et al. Non-invasive Assessment of Swallowing and Respiration Coordination for the OSA Patient. Dysphagia 31, 771–780 (2016). https://doi.org/10.1007/s00455-016-9740-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00455-016-9740-8