Abstract
Background
Hepatocellular carcinoma (HCC) is the most common digestive tumor, and we aimed to develop and validate nomogram models, predicting the overall survival (OS) of young and middle-aged male patients with HCC.
Methods
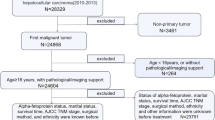
We extracted eligible data from relevant patients between 2000 and 2017 from the Surveillance, Epidemiology, and End Results (SEER) database. In addition, randomly divided all patients into two groups (training and validation = 7:3). The nomogram was established using effective risk factors based on univariate and multivariate analysis. The area under the time-dependent curve, calibration plots, and decision curve analysis (DCA) were used to evaluate the effective performance of the nomogram. The risk stratifications of the nomogram and the AJCC criteria‐based tumor stage were compared.
Results
11 variables were selected by univariate and multivariate analysis to establish the nomogram of HCC. The AUC values of 3, 4, and 5 years of the time–ROC curve are 0.858, 0.862 and 0.859 for the training cohort, and 0.858, 0.877 and 0.869 for the validation cohort, respectively, indicating that the nomogram has a good ability of discrimination. The calibration plots showed favorable consistency between the prediction of the nomogram and actual observations in both the training and validation cohorts. In addition, the decision curve DCA showed that the nomogram was clinically useful and had better discriminative ability to recognize patients at high risk than the AJCC criteria‐based tumor stage.
Conclusion
Prognostic nomogram of young and middle-aged male patients with HCC was developed and validated to help clinicians evaluate the prognosis of patients.






Similar content being viewed by others
Data availability
The data of this study are available in the SEER database (https://seer.cancer.gov/).
Abbreviations
- HCC:
-
Hepatocellular carcinoma
- OS:
-
Overall survival
- TNM:
-
Tumor node metastasis.
- AJCC:
-
American Joint Committee on Cancer
References
Balachandran VP, Gonen M, Smith JJ, DeMatteo RP (2015) Nomograms in oncology: more than meets the eye. Lancet Oncol 16(4):e173–e180
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68(6):394–424
Camp RL, Dolled-Filhart M, Rimm DL (2004) X-tile: a new bio-informatics tool for biomarker assessment and outcome-based cut-point optimization. Clin Cancer Res 10(21):7252–7259
Ha SY, Sohn I, Hwang SH, Yang JW, Park CK (2015) The prognosis of hepatocellular carcinoma after curative hepatectomy in young patients. Oncotarget 6(21):18664–18673
Huang X, Luo Z, Liang W et al (2022) Survival nomogram for young breast cancer patients based on the SEER database and an external validation cohort. Ann Surg Oncol 29(9):5772–5781
Jiang S, Zhao R, Li Y et al (2018) Prognosis and nomogram for predicting postoperative survival of duodenal adenocarcinoma: a retrospective study in China and the SEER database. Sci Rep 8(1):7940
Li C, Chen K, Liu X et al (2020) Analysis of clinicopathological characteristics and prognosis of young patients with hepatocellular carcinoma after hepatectomy. J Clin Transl Hepatol 8(3):285–291
Liao CY, Lee CY, Wei CY et al (2022) Differential prognoses among male and female patients with hepatocellular carcinoma. J Chin Med Assoc 85(5):554–565
Liu K, Huang G, Chang P et al (2020) Construction and validation of a nomogram for predicting cancer-specific survival in hepatocellular carcinoma patients. Sci Rep 10(1):21376
Niederle IM, Wörns MA, Koch S et al (2012) Clinicopathologic features and prognosis of young patients with hepatocellular carcinoma in a large German cohort. J Clin Gastroenterol 46(9):775–778
Pais R, Lebray P, Rousseau G et al (2015) Nonalcoholic fatty liver disease increases the risk of hepatocellular carcinoma in patients with alcohol-associated cirrhosis awaiting liver transplants. Clin Gastroenterol Hepatol 13(5):992–9.e2
Shen J, Li C, Yan L et al (2018) Short- and long-term outcomes between young and older HCC patients exceeding the Milan criteria after hepatectomy. Ann Hepatol 17(1):134–143
Sukocheva OA (2018) Estrogen, estrogen receptors, and hepatocellular carcinoma: are we there yet. World J Gastroenterol 24(1):1–4
Vickers AJ, Elkin EB (2006) Decision curve analysis: a novel method for evaluating prediction models. Med Decis Mak 26(6):565–574
Wan G, Gao F, Chen J et al (2017) Nomogram prediction of individual prognosis of patients with hepatocellular carcinoma. BMC Cancer 17(1):91
Wang C, Wang X, Gong G et al (2012) Increased risk of hepatocellular carcinoma in patients with diabetes mellitus: a systematic review and meta-analysis of cohort studies. Int J Cancer 130(7):1639–1648
Wu J, Zhang H, Li L et al (2020) A nomogram for predicting overall survival in patients with low-grade endometrial stromal sarcoma: A population-based analysis. Cancer Commun (lond) 40(7):301–312
Yan B, Su BB, Bai DS et al (2021) A practical nomogram and risk stratification system predicting the cancer-specific survival for patients with early hepatocellular carcinoma. Cancer Med 10(2):496–506
Yang D, Zhu M, Xiong X et al (2022) Clinical features and prognostic factors in patients with microvascular infiltration of hepatocellular carcinoma: development and validation of a nomogram and risk stratification based on the SEER database. Front Oncol 12:987603
Zhan H, Zhao X, Lu Z, Yao Y, Zhang X (2021) Correlation and survival analysis of distant metastasis site and prognosis in patients with hepatocellular carcinoma. Front Oncol 11:652768
Zou RC, Xiao SF, Shi ZT et al (2019) Identification of metabolism-associated pathways and genes involved in male and female liver cancer patients. J Theor Biol 480:218–228
Zuo Z, Zhang G, Song P et al (2021) Survival nomogram for stage IB non-small-cell lung cancer patients, based on the SEER database and an external validation cohort. Ann Surg Oncol 28(7):3941–3950
Acknowledgements
We appreciate the help from other teammates.
Funding
This work was supported by the National Natural Science Foundation of China (82074425); Key Scientific Research Project of Hunan Provincial (2021SK22006); Natural Foundation of Hunan Provincial (2021JJ30417).
Author information
Authors and Affiliations
Contributions
Study design: XY, RY; data collection: XY; manuscript preparation: XY; data analysis and interpretation: XY, RY, PZ; all authors confirm that they contributed to manuscript reviews, revising it critically for important intellectual content and read and approved the final draft for submission. All authors are also responsible for the manuscript content.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yang, R., Yu, X. & Zeng, P. Construction and validation of a SEER-based prognostic nomogram for young and middle-aged males patients with hepatocellular carcinoma. J Cancer Res Clin Oncol 149, 10099–10108 (2023). https://doi.org/10.1007/s00432-023-04901-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-023-04901-0