Abstract
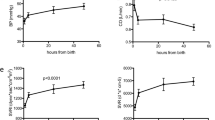
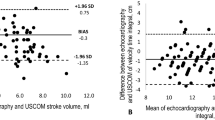
We aimed to establish reference ranges for USCOM parameters in preterm infants, determine factors that affect cardiac output, and evaluate the measurement repeatability. This retro-prospective study was performed at Fondazione IRCCS San Gerardo dei Tintori, Monza, Italy. We included infants below 32 weeks of gestational age (GA) and/or 1500 g of birth weight (BW). We excluded infants with congenital heart diseases or hemodynamic instability. Measurements were performed at 3 ± 1, 7 ± 2, and 14 ± 2 postnatal days. We analyzed 204 measurements from 92 patients (median GA = 30.57 weeks, BW = 1360 g). The mean (SD) cardiac output (CO) was 278 (55) ml/min/kg, cardiac index (CI) was 3.1 (0.5) L/min/m2, and systemic vascular resistance (SVRI) was 1292 (294) d*s*cm−5/m2. CO presented a negative correlation with postmenstrual age (PMA), while SVRI presented a positive correlation with PMA. The repeatability coefficient was 31 ml/kg/min (12%).
Conclusion: This is the first study describing reference values for USCOM parameters in hemodynamically stable preterm infants and factors affecting their variability. Further studies to investigate the usefulness of USCOM for the longitudinal assessment of patients at risk for cardiovascular instability or monitoring the response to therapies are warranted.
What is Known: • The ultrasonic cardiac output monitoring (USCOM) has been widely used on adult and pediatric patients and reference ranges for cardiac output (CO) by USCOM have been established in term infants. | |
What is New: • We established reference values for USCOM parameters in very preterm and very-low-birth-weight infants; the reference ranges for CO by USCOM in the study population were 198-405 ml/kg/min. • CO normalized by body weight presented a significant negative correlation with postmenstrual age (PMA); systemic vascular resistance index presented a significant positive correlation with PMA. |




Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this article. Further enquiries can be directed to the corresponding author.
References
Evans JR, Lou Short B, Van Meurs K, Cheryl Sachs H (2006) Cardiovascular support in preterm infants. Clin Ther 28:1366–1384. https://doi.org/10.1016/j.clinthera.2006.09.006
Koch J, Hensley G, Roy L et al (2006) Prevalence of spontaneous closure of the ductus arteriosus in neonates at a birth weight of 1000 grams or less. Pediatrics 117:1113–1121. https://doi.org/10.1542/peds.2005-1528
Vrancken SL, van Heijst AF, de Boode WP (2018) Neonatal hemodynamics: from developmental physiology to comprehensive monitoring. Front Pediatr 6:1–15. https://doi.org/10.3389/fped.2018.00087
McGovern M, Miletin J (2018) Cardiac output monitoring in preterm infants. Front Pediatr 6:1–10. https://doi.org/10.3389/fped.2018.00084
Groves A, Kuschel CA, Knight DB, Skinner JR (2008) Relationship between blood pressure and blood flow in newborn preterm infants. Arch Dis Child Fetal Neonatal Ed 93:29–33. https://doi.org/10.1136/adc.2006.109520
Kharrat A, Rios DI, Weisz DE et al (2019) The relationship between blood pressure parameters and left ventricular output in neonates. J Perinatol 39:619–625. https://doi.org/10.1038/s41372-019-0337-6
Tibby SM, Hatherill M, Marsh MJ, Murdoch IA (1997) Clinicians’ abilities to estimate cardiac index in ventilated children and infants. Arch Dis Child 77:516–518. https://doi.org/10.1136/adc.77.6.516
Boet A, Jourdain G, Demontoux S (2016) De Luca D (2016) Stroke volume and cardiac output evaluation by electrical cardiometry: accuracy and reference nomograms in hemodynamically stable preterm neonates. J Perinatol 369(36):748–752. https://doi.org/10.1038/jp.2016.65
Fraga MV, Dysart KC, Rintoul N et al (2019) Cardiac Output measurement using the ultrasonic cardiac output monitor: a validation study in newborn infants. Neonatology 116:260–268. https://doi.org/10.1159/000501005
Meyer S, Todd D (2009) Assessment of portable continuous wave Doppler ultrasound (ultrasonic cardiac output monitor) for cardiac output. J Paediatr Child Health 45:464–468. https://doi.org/10.1111/j.1440-1754.2009.01535.x
Cattermole GN, Leung PYM, Ho GYL et al (2017) The normal ranges of cardiovascular parameters measured using the ultrasonic cardiac output monitor. Physiol Rep 5:1–9. https://doi.org/10.14814/phy2.13195
Patel N, Dodsworth M, Mills JF (2011) Cardiac output measurement in newborn infants using the ultrasonic cardiac output monitor: an assessment of agreement with conventional echocardiography, repeatability and new user experience. Arch Dis Child Fetal Neonatal Ed 96. https://doi.org/10.1136/adc.2009.170704
Doni D, Nucera S, Rigotti C et al (2020) Evaluation of hemodynamics in healthy term neonates using ultrasonic cardiac output monitor. Ital J Pediatr 46:1–9. https://doi.org/10.1186/s13052-020-00872-x
He SR, Zhang C, Liu YM et al (2011) Accuracy of the ultrasonic cardiac output monitor in healthy term neonates during postnatal circulatory adaptation. Chin Med J (Engl) 124:2284–2289. https://doi.org/10.3760/cma.j.issn.0366-6999.2011.15.008
Liu YM, Zheng ML, Sun X et al (2022) The clinical value of ultrasonic cardiac output monitor in very-low-birth-weight and extremely-low-birth-weight infants undergoing PDA ligation. Early Hum Dev 165:105522. https://doi.org/10.1016/j.earlhumdev.2021.105522
Quezado ZMN, Natanson C (1992) Systemic hemodynamic abnormalities and vasopressor therapy in sepsis and septic shock. Am J Kidney Dis 20:214–222. https://doi.org/10.1016/S0272-6386(12)80693-7
Du Bois D, Du Bois EF (1916) Clinical calorimetry: tenth paper a formula to estimate the approximate surface area if height and weight be known. Arch Intern Med XVII:863–871. https://doi.org/10.1001/ARCHINTE.1916.00080130010002
Su BH, Watanabe T, Shimizu M, Yanagisawa M (1997) Echocardiographic assessment of patent ductus arteriosus shunt flow pattern in premature infants. Arch Dis Child Fetal Neonatal Ed 77:F36-40. https://doi.org/10.1136/fn.77.1.f36
Cohen J, Cohen P, West SG, Aiken LS (2002) Applied multiple regression/correlation analysis for the behavioral sciences, 3rd edn. Lawrence Erlbaum Associates, New Jersey
Evans N, Kluckow M (1996) Early determinants of right and left ventricular output in ventilated preterm infants. Arch Dis Child 74:88–94. https://doi.org/10.1136/fn.74.2.f88
Koo TK, Li MY (2016) A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med 15:155. https://doi.org/10.1016/J.JCM.2016.02.012
De BW (2020) Advanced hemodynamic monitoring in the neonatal intensive care unit shock hemodynamic monitoring cardiac output. Clin Perinatol 47:423–434. https://doi.org/10.1016/j.clp.2020.05.001
Hudson I, Houston A, Aitchison T et al (1990) Reproducibility of measurements of cardiac output in newborn infants by Doppler ultrasound. Arch Dis Child 65(1 Spec No):15–19. https://doi.org/10.1136/adc.65.1_spec_no.15
Thom O, Taylor DM, Wolfe RE et al (2009) Comparison of a supra-sternal cardiac output monitor (USCOM) with the pulmonary artery catheter. Br J Anaesth 103:800–804. https://doi.org/10.1093/bja/aep296
Knirsch W, Kretschmar O, Tomaske M et al (2008) Cardiac output measurement in children: comparison of the ultrasound cardiac output monitor with thermodilution cardiac output measurement. Intensive Care Med 34:1060–1064. https://doi.org/10.1007/s00134-008-1030-y
Acknowledgements
The authors thank Dr. Giulia Dognini, Dr. Valentina Privitera, Dr. Marianna Zicoia, and Dr. Ester De Luca for their help in data collection.
Author information
Authors and Affiliations
Contributions
DD was the principal investigator, interpreted the data, critically revised the manuscript, and approved the final manuscript as submitted. MF collected the data, drafted the initial manuscript, performed the literature search, and approved the final manuscript as submitted. EZ performed statistical analysis, drafted the figures, reviewed and revised the manuscript, and approved the final manuscript as submitted. AR, CC, and LI contributed to data collection and approved the final manuscript as submitted. VC and MTS contributed to data interpretation, critically revised the manuscript, and approved the final manuscript as submitted. CR contributed to data collection, critically revised the manuscript, and approved the final version as submitted. TF and MLV obtained the resources to conduct the study, contributed to conceiving the study, and approved the final version of the manuscript as submitted.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This study has been conducted in compliance with the principles of the Helsinki Declaration and was approved by the ethical review board of the Fondazione IRCCS San Gerardo dei Tintori, Monza, Italy (protocol nr. 4309/23). The study has been registered, NCT05961657. Informed consent was obtained from the parents/legal guardians of the participants included in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Communicated by Daniele De Luca
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Doni, D., Faraguna, M.C., Zannin, E. et al. Hemodynamic evaluation in preterm infants using ultrasonic cardiac output monitor (USCOM). Eur J Pediatr 183, 2183–2192 (2024). https://doi.org/10.1007/s00431-024-05465-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-024-05465-y