Abstract
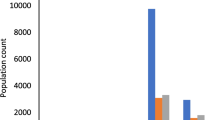
The frequency of vitamin D deficiency in healthy children is relatively high. Moreover, vitamin D supplementation in children is under the requested levels. The aim of this study is to determine the frequency of vitamin D deficiency and the factors that influence vitamin D levels in healthy children. During the study period, 3368 vitamin D levels of healthy children, aged 0–18 years, were evaluated retrospectively. Vitamin D levels were categorized as deficiency (< 12 ng/ml), insufficiency (12–20 ng/ml), and sufficiency (> 20 ng/ml). The prevalence of vitamin D deficiency and insufficiency was found to be 18–24.9% in healthy children, respectively. It was found that the frequency of vitamin D deficiency increased with age. In addition, the most severe and highest risk group for vitamin D deficiency were adolescent girls. Moreover, being in the winter or spring season and living in the north of the 40th parallel are the other risk factors for vitamin D deficiency.
Conclusion: This study showed that vitamin D deficiency still remains a major problem for healthy children and daily supplementation of vitamin D is mandatory. Prophylactic vitamin D supplementation and adequate sunlight exposure should be provided for all children, in particular healthy adolescents. In addition, future studies may focus on screening for vitamin D status in children who did not receive vitamin D supplementation.
What is Known: • Vitamin D is an essential component in bone metabolism. Seasonality, age, sex, dark skin pigmentation, and limited exposure to sunlight are causes of vitamin D deficiency. • The World Health Organization has drawn attention to this increased frequency, recommending lifelong, regular vitamin D prophylaxis. | |
What is New: • The frequency of vitamin D deficiency and insufficiency was found to be 42.9% in healthy children and the frequency significantly increased with age. • There were almost no cases of prophylactic vitamin D usage in adolescent group which are at the highest risk. |


Similar content being viewed by others
Availability of data and material
Data can be provided upon request.
Abbreviations
- 25(OH)D3:
-
25-Hydroxy vitamin D
- AAP:
-
American Academy of Pediatrics
- IU:
-
International unit
- ng/ml:
-
Nanogram/milliliter
- WHO:
-
World Health Organization
References
Misra M, Motil JK, Hoppin AG, Hoppin AG (2022) Vitamin D insufficiency and deficiency in children and adolescents. https://www.uptodate.com/contents/vitamin-d-insufficiency-and-deficiency-in-children-and-adolescents. Accessed 3 January 2023
Pazirandeh S, Burns L, D. Motil JK, Rubinow K (2022) Overview of vitamin D. http://www.uptodate.com.contents.overview-of-vitamin-d. Accessed 8 January 2023
Charoenngam N, Shirvani A, Holick MF (2019) Vitamin D for skeletal and non-skeletal health: what we should know. J Clin Orthop Trauma 10(6):1082–1093. https://doi.org/10.1016/j.jcot.2019.07.004
Carpenter T, Wolfsdorf JI, Hoppin AG (2022) Etiology and treatment of calcipenic rickets in children. https://www.uptodate.com/contents/ etiology-and-treatment-of-calcipenic-rickets-in-children. Accessed 23 January 2023
Kimball SM, Holick MF (2020) Official recommendations for vitamin D through the life stages in developed countries. Eur J Clin Nutr 74(11):1514–1518. https://doi.org/10.1038/s41430-020-00706-3
Ross CA, Taylor LC, Yaktine LA et al (2011) Institute of Medicine, Food and Nutrition Board. Dietary reference intakes for calcium and vitamin D. Washington, DC: National Academy Press,. https://www.ncbi.nlm.nih.gov/NBK56061/?report=reader Accessed 28 January 2023
Kliegman RM, Geme JS (2019) nelson textbook of pediatrics, 21st edition. Part II: growth, development and behavior, pp:26–39. Accessed 29 January 2023
Munns CF, Shaw N, Kiely M et al (2016) Global consensus recommendations on prevention and management of nutritional rickets. J Clin Endocrinol Metab 101(2):394–415. https://doi.org/10.1210/jc.2015-2175
Marino R, Misra M (2019) (2019) Extra-skeletal effects of vitamin D. Nutrients 11(7):1460. https://doi.org/10.3390/nu11071460
Taylor SN (2020) Vitamin D in toddlers, preschool children, and adolescents. Ann Nutr Metab 76(Suppl 2):30–41. https://doi.org/10.1159/000505635
Public Health England, Food Standards Agency. National diet and nutrition survey: results from years 1, 2, 3 and 4 (combined) of the rolling programme (2008/2009–2011/2012). URL: https://www.gov.uk/government/statistics/national-diet-and-nutrition-survey-results-from-years-1-to-4-combined-of-the-rolling-programme-for-2008-and-2009-to-2011-and-2012. Accessed 9 February 2023
Rabenberg M, Scheidt-Nave C, Busch MA et al (2018) Implications of standardization of serum 25-hydroxyvitamin D data for the evaluation of vitamin D status in Germany, including a temporal analysis. BMC Public Health 18(1):845. https://doi.org/10.1186/s12889-018-5769-y
Cairncross CT, Stonehouse W, Conlon CA et al (2017) Predictors of vitamin D status in New Zealand preschool children. Matern Child Nutr.13(3):e12340. https://doi.org/10.1111/mcn.12340
Garg MK, Tandon N, Marwaha RK et al (2014) The relationship between serum 25-hydroxy vitamin D, parathormone and bone mineral density in Indian population. Clin Endocrinol (Oxf) 80(1):41–46. https://doi.org/10.1111/cen.12248
Alpdemir M, Alpdemir MF (2019) Vitamin D deficiency status in Turkey: a meta-analysis. Int J Med Biochem 2(3):118–131. https://doi.org/10.14744/ijmb.2019.04127
Sahin ON, Serdar MS et al (2018) Vitamin D levels and parathyroid hormone variations of children living in a subtropical climate: a data mining study. Ital J Pediatr 44(1):40. https://doi.org/10.1186/s13052-018-0479-8
Guillemant J, Cabrol S, Allemandou A et al (1995) Vitamin D-dependent seasonal variation of PTH in growing male adolescents. Bone 17(6):513–516. https://doi.org/10.1016/8756-3282(95)00401-7
Smotkin-Tangorra M, Purushothaman R, Gupta A et al (2007) Prevalence of vitamin D insufficiency in obese children and adolescents. J Pediatr Endocrinol Metab 20(7):817–823. https://doi.org/10.1515/jpem.2007.20.7.817
Rockell JE, Green TJ, Skeaff CM et al (2005) Season and ethnicity are determinants of serum 25-hydroxyvitamin D concentrations in New Zealand children aged 5–14 y. J Nutr 135(11):2602–2608. https://doi.org/10.1093/jn/135.11.2602
Hill TR, Cotter AA, Mitchell S et al (2008) Vitamin D status and its determinants in adolescents from the Northern Ireland Young Hearts 2000 cohort. Br J Nutr 99(5):1061–1067. https://doi.org/10.1017/S0007114507842826
Varkal MA, Özçetin M, Kılıç A (2021) Frequency of vitamin D deficiency in children: a single-center cross-sectional study in Istanbul. J Contemp Med 11(6), 755–760. https://doi.org/10.16899/jcm984173
D Vitamini Eksikliği Önleme ve Kontrol Programı https://hsgm.saglik.gov.tr/tr/cocukergen-bp-liste/d-vitamini-eksikli%C4%9Fi-%C3%B6nleme-ve-kontrol-program%C4%B1.html. Accessed 7 January 2023
Vitamin D supplementation in infants. https://www.who.int/elena/titles/vitamind_infants/en. Accessed 7 January 2023
Specker BL, Ho ML, Oestreich A et al (1992) Prospective study of vitamin D supplementation and rickets in China. J Pediatr 120(5):733–739. https://doi.org/10.1016/s0022-3476(05)80236-7
Gallo S, Comeau K, Vanstone C et al (2013) Effect of different dosages of oral vitamin D supplementation on vitamin D status in healthy, breastfed infants: a randomized trial. JAMA 309(17):1785–1792. https://doi.org/10.1001/jama.2013.3404
Author information
Authors and Affiliations
Contributions
CK and ADC contributed to the study conception and design. Material preparation, data collection, and analysis were performed by CK. The first draft of the manuscript was written by CK and ADC and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Ankara Pediatrics, Hematology Oncology Education and Research Hospital, Clinical Research Ethics Committee approval was obtained prior the study (Approval No. 2018–109). Due to the retrospective nature of the study, a consent to participate statement was not included. The research was conducted in accordance with the 1964 Helsinki Declaration.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Communicated by Peter de Winter
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Karagol, C., Duyan Camurdan, A. Evaluation of vitamin D levels and affecting factors of vitamin D deficiency in healthy children 0–18 years old. Eur J Pediatr 182, 4123–4131 (2023). https://doi.org/10.1007/s00431-023-05096-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-023-05096-9