Abstract
To compare whether alternate rotation of nasal mask with nasal prongs every 8 h as compared to continuous use of either interface alone decreases the incidence of nasal injury in preterm infants receiving nasal Continuous Positive Airway Pressure (nCPAP). This was an open-label, three-arm, stratified randomized controlled trial where infants < 35 weeks receiving nCPAP were randomized into three groups using two different nasal interfaces (continuous prongs group, continuous mask group, and rotation group). All infants were assessed for nasal injury six hours post-removal of nCPAP using grading suggested by Fischer et al. The nursing care was uniform across all three groups. Intention-to-treat analysis was done. Fifty-seven infants were enrolled, with nineteen in each group. The incidence of nasal injury was 42.1% vs. 47.4% vs. 68.4% in the rotation group, continuous mask, and continuous prongs groups, respectively (P = 0.228). On adjusted analysis (gestational age, birth weight, and duration of nCPAP therapy), the incidence of nasal injury was significantly less in the rotation group as compared to continuous prongs group (Adjusted Odds Ratio [AOR], 95% confidence interval [CI]; 0.10 [0.01–0.69], P = 0.02) and a trend towards lesser nasal injury as compared to continuous mask group (AOR, 95% CI; 0.15 [0.02–1.08], P = 0.06). However, there was no significant difference in incidence of nasal injuries between continuous prongs versus continuous mask group (P = 0.60). The need for surfactant, nCPAP failure rate, duration of nCPAP, and common neonatal co-morbidities were similar across all three groups.
Conclusion: Systematic rotation of nasal mask with nasal prongs significantly reduced nasal injury among preterm infants on nCPAP as compared to continuous use of nasal prongs alone without affecting nCPAP failure rate.
Trial registration: CTRI/2019/01/017320, registered on 31/01/2019.
What is Known: • Use of nasal mask as an interface for nasal Continuous Positive Airway Pressure decreases nasal injury as compared to nasal prongs. | |
What is New: • Rotation of nasal prongs and nasal mask interfaces alternately every 8 h may reduce the nasal injury even further as compared to either interface alone. |
Similar content being viewed by others
Introduction
Nasal continuous positive airway pressure (nCPAP) is the most common form of respiratory support used to manage respiratory distress in preterm infants and is currently the standard of care [1]. However, the nasal interface used to deliver nCPAP causes skin injury [2]. These nasal injuries not only result in pain and discomfort but may also predispose to infection. If severe, it may necessitate change of mode of respiratory support and warrant surgical intervention [3,4,5].
The reported incidence of nasal injuries varies from 20–60% [2, 6,7,8,9], with as high as 90% in some Indian neonatal units [10,11,12,13]. This wide range is primarily due to the varying gestational age of the population studied and the lack of standardised classification system for nasal injuries [14]. Moreover, differences in the various risk factors, including type of nasal interface, quality of nursing care, experience of the neonatal unit, and duration of non-invasive ventilation (NIV), add to this wide variation across various units [15, 16].
Several evidence-based interventions have been shown to decrease nasal injuries, including selection of appropriate size nasal interface, use of nasal barrier dressings and lubricants, and quality improvement initiatives [14, 16,17,18]. The risk of nasal injury is possibly less with nasal masks as compared to short binasal prongs [19,20,21]. However, the quality of evidence is low to very low.
Periodic rotation of nasal prongs with nasal mask has been suggested as one of the potential strategies to reduce nasal injury [14]. This is based on the fact that the continuous pressure produced by the nasal interface over the point of approximation with the skin is believed to be one of the key reasons which compromise skin integrity resulting in nasal injury [5]. The pressure points while using nasal mask for nCPAP delivery are quite different from that of the nasal prong [6]. Hence, rotation of the two nasal interfaces alternately at a fixed time interval may relieve the pressure built-up at any particular point of skin. However, studies evaluating such a strategy are very limited. Newnam et al. demonstrated significantly less nasal injury in preterm infants who received regular rotation of nasal mask and prongs compared to infants who received either of them continuously [22]. However, Bashir et al. failed to replicate similar results [13]. A recent study by Sardar et al. didn’t find any significant difference between the mask and rotation group [23].
Therefore, we wanted to compare the incidence and severity of nasal injury when using two different nasal interfaces (nasal mask and short binasal prongs) in three groups (i.e., continuous prongs group, continuous mask group, and rotation group) among preterm infants (< 35 weeks’ gestation) requiring nCPAP for respiratory distress.
Methods
This study is an open-label, three-arm, stratified randomized controlled trial over 14 months from February 2019 to March 2020 in a level III Neonatal Intensive Care Unit (NICU) in Western India. Inborn infants with gestation < 35 weeks and having respiratory distress requiring nCPAP within 6 h of birth or requiring nCPAP as post-extubation support were eligible for inclusion. Infants with severe perinatal asphyxia (5-min APGAR score of ≤ 3), major congenital anomalies/syndrome, malformations that would prevent delivery of nCPAP, and conditions where nCPAP is contraindicated (poor respiratory efforts, shock) were excluded.
The trial was approved by the Institutional Ethics Committee and registered in the Clinical Trial Registry of India (CTRI/2019/01/017320). The investigator approached the parents or legally authorized representatives of all eligible infants for written informed consent. Infants, who developed respiratory distress in the delivery room itself, were stabilised and transferred to NICU on a T-piece resuscitator.
Randomization procedure
Infants were randomized into three groups (continuous prongs, continuous mask, and rotation group) at the time of starting nCPAP. It was a stratified (< 28, 28 to < 32, and 32 to < 35 weeks), randomized block design with permuted, odd-numbered blocks of randomly varying sizes and a 1:1:1 allocation ratio. Subsequently, a second simple randomization sequence was generated for infants randomized to rotation group to decide the choice of initial interface to be used i.e. nasal mask or nasal prongs. An investigator generated the randomization sequence from a website (www.randomization.com) and was not involved in the recruitment or assessment of subjects. The randomization sequence was concealed using sequentially numbered, opaque, sealed envelopes.
Intervention
Nasal prongs and masks used to deliver nCPAP were of the same make (Drager BabyFlow®). An appropriate size interface was selected as per the manufacturer’s instructions.
Continuous prongs group
Infants randomized to this group received nCPAP via appropriately sized short binasal prongs till they were weaned off from nCPAP.
Continuous mask group
Infants of this group received nCPAP via appropriately sized nasal mask.
Rotation group
Infants in the rotation group were initiated on nCPAP using either short binasal prongs or nasal mask as per the second randomization code and then alternatively switched to the other interface every eight hours till nCPAP was weaned off. Utmost care was taken while changing the nasal interface to minimize the duration of the off-CPAP period.
Blinding
The principal investigator, caregivers, and parents were not blinded due to the nature of the intervention. However, the outcome assessor and the statistician were blinded. Further, every attempt was made to minimize bias by strictly adhering to the study protocol (Supplementary Fig. 1).
Dedicated neonatal ventilators (Drager Babylog® 8000 plus) were used to deliver nCPAP in infants across all three groups. A servo-controlled humidifier (Fisher & Paykel Healthcare, MR850) was used to deliver warm and humidified gases. Skin barrier dressing (DuoDERM®) was also applied over the pressure points in all infants as a standard unit practice.
A uniform protocol for titration, weaning, and removal of nCPAP was followed, which was adapted from the study by Bhatti et al. [24]. Infants were started on nCPAP with the initial settings of Positive End Expiratory Pressure (PEEP) of 5 cm H2O and FiO2 of 25–40%, targeting oxygen saturation (SpO2) between 90–95%. The maximum PEEP used in the trial was 7 cm H2O. CPAP failure was defined as the need for intubation and mechanical ventilation after a trial of maximum pressure of 7 cm H2O and FiO2 > 60%. The criteria used to define CPAP failure was the presence of at least one of the following: (a) worsening respiratory distress on maximum CPAP settings, (b) recurrent apnoeas (⩾3 episodes per hour) (c) SpO2 < 90% and/or PaO2 < 50 mm Hg on FiO2 > 60% d) pH < 7.2 or PaCO2 ⩾55 mm Hg or base excess > -15, (d) and (e) signs of shock [24] (Supplementary Fig. 1).
Weaning was initiated if the infant showed consistent improvement with no respiratory distress and apnoea free, and thereafter the nCPAP was discontinued. Infants remained on room air post CPAP removal with ongoing close monitoring.
A subset of infants was enrolled and randomized post-extubation as per the pre-defined inclusion criteria. The protocol for extubation from mechanical ventilation to nCPAP was adapted from the study by Gupta et al. [25]. All infants post-extubation received nCPAP of 5 cm H2O. The subsequent titration and weaning remained the same.
The unit has been regularly using nCPAP for the last five years, and all the nursing officers are well-trained in administering nCPAP. The nursing care was uniform across all three groups, with hourly recording of vitals, ensuring proper positioning of nasal interface, nasal suctioning as and when required, and ensuring adequate CPAP pressure delivery. The Principal Investigator (PI) re-trained all the nursing officers of the unit to identify nasal injury before the commencement of the study. All infants on nCPAP were regularly assessed for any nasal injury by their respective nursing officers as part of routine care. Any infant developing grade-3 nasal injury was censored from the study from that point onwards, and the treating team decided on further treatment, including the choice of nasal interface.
The surfactant was delivered by INSURE (INtubation-SURfactant-Extubation) technique as per standard unit policy across all three groups. Similarly, the use of caffeine and other practices, including feeding and developmentally supportive care, were similar among all the study infants.
Outcomes
All infants were assessed for nasal injury six hours after the removal of nCPAP. A set of six standardized digital photographs was taken by the PI using a digital camera device (Canon Powershot XS430 IS) for each participant, which was then reviewed by a senior neonatologist at the end of the study in a blinded fashion. The primary outcome was the incidence and severity of nasal injury. The severity of the nasal injury was assessed by a nasal injury grading developed by Fischer et al. (Stage I, II, and III were defined as non-blanching erythema, partial-thickness skin loss [superficial ulcer], and full-thickness skin loss [necrosis], respectively) [9].
The secondary outcomes included the need for surfactant replacement therapy, nCPAP failure rates (as defined earlier), the time to onset of the appearance of any and severe nasal injury, the duration of nCPAP, the incidence of common neonatal co-morbidities [necrotizing enterocolitis (NEC), intraventricular haemorrhage (IVH), periventricular leukomalacia (PVL), bronchopulmonary dysplasia (BPD) and retinopathy of prematurity (ROP)], the duration of NICU stay, and age at discharge or death [26,27,28,29]. All infants were followed till death or discharge, and the relevant data was collected prospectively.
Statistical analysis
Assuming an incidence of nasal injury of 50% among the control group (i.e., either continuous prongs or mask group) with an effect size of 30%, 80% power, and an alpha error of 5%, we needed to enrol 89 infants in each group in a superiority design [10, 11]. However, the study had to be stopped prematurely because of the COVID-19 pandemic, which resulted in diversion of healthcare workers to COVID ICUs and wards. Moreover, there were various other unanticipated logistic issues due to COVID-19-related hospital policy. Therefore, the recruitment of infants was possible only till March 2021, and could enrol only 57 infants till then.
Categorical variables were analysed using the Chi-square test with continuity correction or Fisher’s exact test. Continuous variables were analysed using the ANOVA or Kruskal–Wallis test. Multiple logistic regression analysis was done to adjust for potential confounding variables. The choice of variables to be adjusted for was based on biological plausibility or the significance (P < 0.20) of their association with the outcome of interest in the univariate analysis. Hazard ratio analysis was done using the cox proportional hazard regression model. The multicollinearity between the variables in the regression model was checked using Variance Inflation Factor (VIF), and the goodness-of-fit was checked using Chi-square statistics. An intention-to-treat analysis was done (ITT). All analysis was done using IBM-SPSS v.23. A P < 0.05 was considered significant.
Results
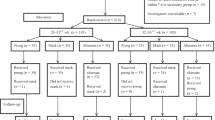
Fifty-seven infants were enrolled in the study, with 19 in each group. Among the rotation group, eight infants received nasal prongs, and 11 received nasal mask as the first nasal interface based on the second randomization sequence. There was no loss to follow-up (Fig. 1).
The mean (SD) gestational age and birth weight of the study population was 31.6 (2.4) weeks and 1534 (508) grams, respectively. Thirty-five (61.4%) infants were between 32+0 to 34+6 weeks of gestation. Twenty-one infants (36.8%) had RDS (Respiratory Distress Syndrome), and three infants received nCPAP therapy as post-extubation support. The median (IQR) age of starting nCPAP was 40 (30, 40) minutes. The birth weight was unequally distributed among the three groups (1419 vs. 1802 vs. 1386 g in the continuous prongs, continuous mask, and rotation group, respectively; P = 0.026). Similarly, small-for-gestational age infants were unequally distributed among the three groups (57.8% vs. 15.8% vs. 31.6% in the continuous prongs, continuous mask, and rotation group, respectively; P = 0.014). The other baseline variables were comparable among the three groups (Table 1).
Overall, 30 (52.6%) infants developed any nasal injury. Among them, 23 (76.7%) had stage-I nasal injury, while 6 (20%) infants developed stage-II injury. Only one infant in the rotation group developed stage-III nasal injury (Table 2). The incidence of nasal injury was 42.1% (8/19) in the rotation group, 68.4% (13/19) in the continuous prongs group, and 47.4% (9/19) in the continuous mask group. On univariate analysis, gestational age (P = 0.001), birth weight (P = 0.001), and the duration of nCPAP (P = 0.010) were identified as potential confounding variables for nasal injury. After adjusting for these confounding factors, the incidence of nasal injury was significantly less in the rotation group as compared to the continuous prongs group (Adjusted Odds Ratio [AOR], 95% confidence interval [CI]; 0.10 [0.01–0.69], P = 0.02) and a trend towards lesser nasal injury as compared to the continuous mask group (AOR, 95% CI; 0.15 [0.02–1.08], P = 0.06). However, there was no significant difference between the continuous prongs vs. continuous mask group (AOR, 95% CI; 1.54 [0.30–7.95], P = 0.60) (Table 3).
The incidence of nCPAP failure rates was comparable among the three groups (P = 0.455). Similarly, the need for surfactant replacement therapy, the duration of nCPAP, the incidence of various co-morbidities (NEC, IVH, PVL, BPD, and ROP), and the duration of NICU stay were also comparable. Eight infants died before discharge from the hospital, with 3 (15.8%), 1 (5.3%), and 4 (21.1%) infants in the continuous prongs, continuous mask, and rotation group, respectively (P = 0.120) (Table 4).
Post-hoc analysis
Time-to-event analysis using hazard ratio did not show any significant difference between the three groups. The adjusted hazard ratio for the incidence of any nasal injury at any point of time comparing continuous prongs versus continuous mask group, continuous prongs versus rotation group, and rotation versus continuous mask group were 0.5 (95% CI; [0.16–1.52], P = 0.22), 0.77 (95% CI; [0.28–2.07], P = 0.6), and 0.65 (95% CI; [0.2–2.02], P = 0.46), respectively (Fig. 2). Similarly, the adjusted hazard ratio for the incidence of highest stage nasal injury at any point of time comparing continuous prongs versus continuous mask group, continuous prongs versus rotation group, and rotation versus continuous mask group were 0.56 (95% CI; [0.19–1.7], P = 0.31), 0.59 (95% CI; [0.2–1.69], P = 0.33), and 0.95 (95% CI; [0.29–3.08], P = 0.94), respectively. Hazard ratios were adjusted for confounding factors of birth weight and duration of CPAP (Supplementary Fig. 2).
Discussion
In this study, we evaluated the effect of timed rotation of the nasal interface as a third arm in addition to continuous use of nasal prongs and mask on the incidence of nasal injury. The incidence of nasal injury was significantly less in the rotation group as compared to continuous prongs group and a similar trend of lesser nasal injury in the rotation group than in the continuous mask group.
The data from adult literature also supports the practice of rotation of nasal interface while giving NIV as it not only decreases nasal injury but also increases the tolerance to interface, thus decreasing the need for intubation [30,31,32,33]. Similar to our findings, Newnam et al. in a three-arm RCT involving 78 very low birth weight infants requiring nCPAP post-extubation, demonstrated that the rotation group had less severe nasal injury than the continuous prongs or mask group (Neonatal Skin Condition Scale scores for excoriation were 1.10, 1.18, and 1.19 respectively, P = 0.007) [22]. However, unlike ours, they rotated interfaces every 4 h instead of 8 h. Less frequent rotation of nasal interface without affecting efficacy seems to be more feasible and acceptable. Moreover, it may be safer by decreasing or altogether preventing the possible de-recruitment of the alveoli which may accompany this procedure.
Our results differed from that of Bashir et al. [13]. Though the maximum CPAP pressures used in this study was similar to ours (7 cm H2O), however, the incidence of nasal injury in the continuous mask group (33.3%) was significantly less as compared to the prongs group (91.6%) and the rotation group (56.9%), P < 0.0001. Interestingly, despite applying skin barrier dressing across all three groups, the incidence of nasal injury was very high (91.6%) in the nasal prongs group. This study differed from ours in the included population (< 30 weeks) and the nature of the two nasal interfaces used. While in our study, the nasal masks and prongs were of similar make and the same company (Draeger Babyflow), Bashir et al. compared Draeger Babyflow nasal mask with Hudson’s short bi-nasal prongs. The former is silicon-based, while the latter contains polypropylene which is comparatively more rigid and less skin-friendly. Newnam et al. compared nasal interfaces of similar make in all the three groups but of a different company (Airlife™) and arrived at the same conclusion as ours thus increasing the generalizability of our results.
Recently, Sardar et al. conducted a three-arm study comparing nasal prongs, nasal mask, and four hourly rotations of both interfaces (Draeger Babyflow) for delivery of non-invasive positive pressure ventilation (NIPPV) among 210 preterm infants. The reported incidence of moderate to severe nasal injury in the mask, prongs and rotation groups were 8.6%, 22.8%, and 11.4%, respectively. Though, the incidence of nasal injury was significantly less in the mask group, however it was not significantly different in the mask versus rotation groups [23]. Interestingly, the incidence of nasal injury was double in the prongs group as compared to rotation group.
The duration of CPAP therapy has been identified as a risk factor for nasal injury [14, 22]. How early a particular type of interface initiates nasal injury and the type of nasal interface associated with earlier onset of the most severe form of nasal injury are also essential questions. In a post-hoc analysis, we noticed that the median time for the onset of nasal injury after initiating nCPAP was 14 h, 15 h, and 59 h in the continuous nasal prongs, mask, and rotation group, respectively. Similarly, the median time taken for the onset of the highest stage nasal injury was 18 h, 22 h, and 72 h in the prongs, mask, and rotation groups, respectively. But, the difference between the three groups was not statistically significant.
The strengths of our study are its robust design with stratified randomization, the inclusion of infants at risk for nasal injury, uniform standardized protocol, comparison of nasal interfaces of similar material and company, a well-defined objective scoring as the outcome, blinded outcome assessment, and complete follow up till discharge. The main limitation of the study is its small sample size due to the premature termination of the trial due to unforeseen reasons. Though it was an open-label trial due to the nature of the intervention, the persons assessing the outcome and analysing the data were blinded to the allocated intervention, thus taking care of ascertainment bias.
This study implies the need for adequately powered trials comparing nasal mask alone with systematic rotation of nasal interfaces with an assessment of both efficacy and safety outcomes. Short of that, clinicians may consider rotation of nasal interfaces as one of the potential strategies to decrease further progression of nasal injury among infants with early skin changes and still requiring nCPAP therapy.
Conclusion
The systematic rotation of short binasal prongs with nasal mask every eight hours in preterm infants < 35 weeks on nCPAP decreases the incidence of nasal injury as compared to continuous use of either interface alone without affecting nCPAP failure rate. However, adequately powered trials are required to confirm these findings.
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- BPD:
-
Broncho Pulmonary Dysplasia
- CTRI:
-
Clinical Trials Registry-India
- IVH:
-
Intra Ventricular Haemorrhage
- INSURE:
-
Intubation-SURfactant-Extubation
- ITT:
-
Intention-to-treat
- FiO2 :
-
Fraction of Inspired Oxygen
- nCPAP:
-
Nasal Continuous Positive Airway Pressure
- NEC:
-
Necrotising enterocolitis
- NICU:
-
Neonatal Intensive Care Unit
- NIPPV:
-
Non-invasive Positive Pressure Ventilation
- NIV:
-
Non-invasive ventilation
- PEEP:
-
Positive End Expiratory Pressure
- PVL:
-
Periventricular Leukomalacia
- ROP:
-
Retinopathy of Prematurity
- VIF:
-
Variance Inflation Factor
References
De Paoli AG, Davis PG, Argus B, Jackson HD (2008) Devices and pressure sources for administration of nasal continuous positive airway pressure (NCPAP) in preterm neonates. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD002977.pub2
Robertson NJ, McCarthy LS, Hamilton PA, Moss AL (1996) Nasal deformities resulting from flow driver continuous positive airway pressure. Arch Dis Child Fetal Neonatal Ed 75:F209–F212. https://doi.org/10.1136/fn.75.3.F209
Carlisle HR, Kamlin COF, Owen LS et al (2010) Oral continuous positive airway pressure (CPAP) following nasal injury in a preterm infant. Arch Dis Child Fetal Neonatal Ed 95:F142–F143. https://doi.org/10.1136/adc.2009.170084
Li Y, Sepulveda A, Buchanan EP (2015) Late presenting nasal deformities after nasal continuous positive airway pressure injury: 33-year experience. J Plast Reconstr Aesthet Surg 68:339–343. https://doi.org/10.1016/j.bjps.2014.10.036
Newnam KM, McGrath JM, Estes T et al (2013) An integrative review of skin breakdown in the preterm infant associated with nasal continuous positive airway pressure. J Obstet Gynecol Neonatal Nurs JOGNN 42:508–516. https://doi.org/10.1111/1552-6909.12233
Yong S-C, Chen S-J, Boo N-Y (2005) Incidence of nasal trauma associated with nasal prong versus nasal mask during continuous positive airway pressure treatment in very low birthweight infants: a randomised control study. Arch Dis Child Fetal Neonatal Ed 90:F480-483. https://doi.org/10.1136/adc.2004.069351
Buettiker V, Hug MI, Baenziger O et al (2004) Advantages and disadvantages of different nasal CPAP systems in newborns. Intensive Care Med 30:926–930. https://doi.org/10.1007/s00134-004-2267-8
Rego MAC, Martinez FE (2002) Comparison of two nasal prongs for application of continuous positive airway pressure in neonates. Pediatr Crit Care Med J Soc Crit Care Med World Fed Pediatr Intensive Crit Care Soc 3:239–243. https://doi.org/10.1097/00130478-200207000-00007
Fischer C, Bertelle V, Hohlfeld J et al (2010) Nasal trauma due to continuous positive airway pressure in neonates. Arch Dis Child Fetal Neonatal Ed 95:F447-451. https://doi.org/10.1136/adc.2009.179416
Goel S, Mondkar J, Panchal H et al (2015) Nasal Mask Versus Nasal Prongs for Delivering Nasal Continuous Positive Airway Pressure in Preterm Infants with Respiratory Distress: A Randomized Controlled Trial. Indian Pediatr 52:1035–1040. https://doi.org/10.1007/s13312-015-0769-9
Chandrasekaran A, Thukral A, Jeeva Sankar M et al (2017) Nasal masks or binasal prongs for delivering continuous positive airway pressure in preterm neonates-a randomised trial. Eur J Pediatr 176:379–386. https://doi.org/10.1007/s00431-017-2851-x
Khan J, Sundaram V, Murki S et al (2017) Nasal injury and comfort with jet versus bubble continuous positive airway pressure delivery systems in preterm infants with respiratory distress. Eur J Pediatr 176:1629–1635. https://doi.org/10.1007/s00431-017-3016-7
Bashir T, Murki S, Kiran S, et al (2019) 'Nasal mask’ in comparison with ‘nasal prongs’ or ‘rotation of nasal mask with nasal prongs’ reduce the incidence of nasal injury in preterm neonates supported on nasal continuous positive airway pressure (nCPAP): A randomized controlled trial. PLoS ONE 14:e0211476. https://doi.org/10.1371/journal.pone.0211476
Imbulana DI, Manley BJ, Dawson JA et al (2018) Nasal injury in preterm infants receiving non-invasive respiratory support: a systematic review. Arch Dis Child Fetal Neonatal Ed 103:F29–F35. https://doi.org/10.1136/archdischild-2017-313418
Ribeiro D de FC, Barros FS, Fernandes BL, et al (2021) Incidence and Severity of Nasal Injuries in Preterm Infants Associated to Non-Invasive Ventilation Using Short Binasal Prong. Glob Pediatr Health 8:2333794X211010459. https://doi.org/10.1177/2333794X211010459
Aly H, Milner JD, Patel K, El-Mohandes AAE (2004) Does the experience with the use of nasal continuous positive airway pressure improve over time in extremely low birth weight infants? Pediatrics 114:697–702. https://doi.org/10.1542/peds.2003-0572-L
Mariam S, Buddhavarapu S (2020) Impact of systematic training and CPAP checklist in the prevention of NCPAP related nasal injuries in neonates-a quality improvement study. Indian J Pediatr 87:256–261
Squires AJ, Hyndman M (2009) Prevention of nasal injuries secondary to NCPAP application in the ELBW infant. Neonatal Netw NN 28:13–27. https://doi.org/10.1891/0730-0832.28.1.13
Jasani B, Ismail A, Rao S, Patole S (2018) Effectiveness and safety of nasal mask versus binasal prongs for providing continuous positive airway pressure in preterm infants-A systematic review and meta-analysis. Pediatr Pulmonol 53:987–992. https://doi.org/10.1002/ppul.24014
King BC, Gandhi BB, Jackson A et al (2019) Mask versus Prongs for Nasal Continuous Positive Airway Pressure in Preterm Infants: A Systematic Review and Meta-Analysis. Neonatology 116:100–114. https://doi.org/10.1159/000496462
Razak A, Patel W (2020) Nasal mask vs binasal prongs for nasal continuous positive airway pressure in preterm infants: A systematic review and meta-analysis. Pediatr Pulmonol 55:2261–2271
Newnam KM, McGrath JM, Salyer J et al (2015) A comparative effectiveness study of continuous positive airway pressure-related skin breakdown when using different nasal interfaces in the extremely low birth weight neonate. Appl Nurs Res ANR 28:36–41. https://doi.org/10.1016/j.apnr.2014.05.005
Sardar S, Pal S, Ghosh M (2022) A Three-Arm Randomized, Controlled Trial of Different Nasal Interfaces on the Safety and Efficacy of Nasal Intermittent Positive-Pressure Ventilation in Preterm Newborns. Indian J Pediatr 1–7
Bhatti A, Khan J, Murki S et al (2015) Nasal Jet-CPAP (variable flow) versus Bubble-CPAP in preterm infants with respiratory distress: an open label, randomized controlled trial. J Perinatol Off J Calif Perinat Assoc 35:935–940. https://doi.org/10.1038/jp.2015.98
Gupta S, Sinha SK, Tin W, Donn SM (2009) A randomized controlled trial of post-extubation bubble continuous positive airway pressure versus Infant Flow Driver continuous positive airway pressure in preterm infants with respiratory distress syndrome. J Pediatr 154:645–650. https://doi.org/10.1016/j.jpeds.2008.12.034
Papile L-A, Burstein J, Burstein R, Koffler H (1978) Incidence and evolution of subependymal and intraventricular hemorrhage: A study of infants with birth weights less than 1,500 gm. J Pediatr 92:529–534. https://doi.org/10.1016/S0022-3476(78)80282-0
Kliegman RM, Walsh MC (1987) Neonatal necrotizing enterocolitis: pathogenesis, classification, and spectrum of illness. Curr Probl Pediatr 17:219–288
Prematurity IC (1960) for the C of R of (2005) The international classification of retinopathy of prematurity revisited. Arch Ophthalmol Chic Ill 123:991–999
Jobe AH, Bancalari E (2001) Bronchopulmonary dysplasia. Am J Respir Crit Care Med 163:1723–1729
Bello G, De Pascale G, Antonelli M (2016) Noninvasive ventilation. Clin Chest Med 37:711–721
Vaschetto R, Turucz E, Dellapiazza F et al (2012) Noninvasive ventilation after early extubation in patients recovering from hypoxemic acute respiratory failure: a single-centre feasibility study. Intensive Care Med 38:1599–1606
Vitaliti G, Vitaliti MC, Finocchiaro MC et al (2017) Randomized comparison of Helmet CPAP versus High-Flow Nasal Cannula Oxygen in Pediatric Respiratory Distress. Respir Care 62:1036–1042. https://doi.org/10.4187/respcare.05384
Raurell-Torredà M, Romero-Collado A, Rodríguez-Palma M et al (2017) Prevention and treatment of skin lesions associated with non-invasive mechanical ventilation. Recommendations of experts. Enferm Intensiva Engl Ed 28:31–41
Author information
Authors and Affiliations
Contributions
Dr. Gaurav Gautam: Designed the study (with NG), recruited participants, compiled the data, and drafted the initial manuscript. Dr. Neeraj Gupta: Conceptualized and planned the study, supervised the recruitment and data collection, analysed and interpreted the data, and did critical revision and finalization of the manuscript. Dr. Rohit Sasidharan: Helped in data collection, helped in the initial analysis, and critically reviewed the manuscript for important intellectual content. Dr. Sivam Thanigainathan: Helped in data analysis and critically reviewed and revised the manuscript for important intellectual content. Dr. Bharti Yadav: Helped in data collection and critically reviewed the manuscript for important intellectual content. Dr. Kuldeep Singh: Supervised recruitment of patients and critically revised the manuscript for important intellectual content. Dr. Arun Singh: Critically revised the manuscript for important intellectual content.
Corresponding author
Ethics declarations
Ethical approval
Approved by Institutional Ethics Board (AIIMS/IEC/2018/1080), dated 19/03/2018.
Consent to participate
Written informed consent taken.
Consent to publish
Written informed consent taken.
Competing interests
None declared.
Additional information
Communicated by Daniele De Luca.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gautam, G., Gupta, N., Sasidharan, R. et al. Systematic rotation versus continuous application of ‘nasal prongs’ or ‘nasal mask’ in preterm infants on nCPAP: a randomized controlled trial. Eur J Pediatr 182, 2645–2654 (2023). https://doi.org/10.1007/s00431-023-04933-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-023-04933-1