Abstract
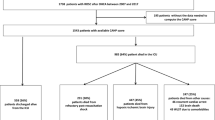
We report on in-hospital cardiac arrest outcomes in the USA. The data were obtained from the National (Nationwide) Inpatient Sample datasets for the years 2000–2017, which includes data from participating hospitals in 47 US states and the District of Columbia. We included pediatric patients (< 18 years of age) with cardiac arrest, and we excluded patients with no cardiopulmonary resuscitation during the hospitalization. Primary outcome of the study was in-hospital mortality after cardiac arrest. A multivariable logistic regression was performed to identify factors associated with survival. A total of 20,654 patients were identified, and 8226 (39.82%) patients survived to discharge. The median length of stay and cost of hospitalization were significantly higher in the survivors vs. non-survivors (LOS 18 days vs. 1 day, and cost $187,434 vs. $45,811, respectively, p < 0.001). In a multivariable model, patients admitted to teaching hospitals, elective admissions, and those admitted on weekdays had higher survival (aOR=1.19, CI: 1.06–1.33; aOR=2.65, CI: 2.37–2.97; and aOR=1.17, CI: 1.07–1.27, respectively). There was no difference in mortality between patients with extracorporeal cardiopulmonary resuscitation (E-CPR) and those with conventional cardiopulmonary resuscitation. E-CPR patients were likely to have congenital heart surgery (51.0% vs. 20.8%).
Conclusion: We highlighted the survival predictors in these events, which can guide future studies aimed at improving outcomes in pediatric cardiac arrest.
What is Known: • In-hospital cardiac arrest occurs in 2–6% of pediatric intensive care admissions. • Cardiac arrests had a significant impact on hospital resources and a significantly high mortality rate. | |
What is New: • Factors associated with higher survival rates in patients with cardiac arrest: admission to teaching hospitals, elective admissions, and week-day admissions. • The use of rescue extracorporeal cardiopulmonary resuscitation in refractory cardiac arrest has increased by threefold over the last two decades. |



Similar content being viewed by others
Data Availability
This is a publicly available data.
Code Availability
N/A
Abbreviations
- IHCA:
-
In-hospital cardiac arrest
- ECPR:
-
Extracorporeal cardiopulmonary resuscitation
- ECMO:
-
Extracorporeal membrane oxygenation
- HCUP:
-
Healthcare Cost and Utilization Project
- ICD-9-CM:
-
International Classification of Diseases, Ninth Revision, Clinical Modification
- ICD-10-CM:
-
International Classification of Diseases, Tenth Revision, Clinical Modification
- CPR:
-
Cardiopulmonary resuscitation
- LOS:
-
Length of hospital stay
- CHD:
-
Congenital heart disease
- IQR:
-
Interquartile range
- ELSO:
-
Extracorporeal Life Support Organization
References
Holmberg MJ, Ross CE, Fitzmaurice GM, Chan PS, Duval-Arnould J, Grossestreuer AV, Yankama T, Donnino MW, Andersen LW, for the American Heart Association’s Get With The Guidelines–Resuscitation Investigators*, Chan P, Grossestreuer AV, Moskowitz A, Edelson D, Ornato J, Berg K, Peberdy MA, Churpek M, Kurz M, Starks MA, Girotra S, Perman S, Goldberger Z, Guerguerian AM, Atkins D, Foglia E, Fink E, Lasa JJ, Roberts J, Bembea M, Gaies M, Kleinman M, Gupta P, Sutton R, Sawyer T (2019) Annual incidence of adult and pediatric in-hospital cardiac arrest in the United States. Circ Cardiovasc Qual Outcomes 12:1–8. https://doi.org/10.1161/CIRCOUTCOMES.119.005580
Berg RA, Nadkarni VM, Clark AE, Moler F, Meert K, Harrison RE, Newth CJ, Sutton RM, Wessel DL, Berger JT, Carcillo J, Dalton H, Heidemann S, Shanley TP, Zuppa AF, Doctor A, Tamburro RF, Jenkins TL, Dean JM, Holubkov R, Pollack MM, Eunice Kennedy Shriver National Institute of Child Health and Human Development Collaborative Pediatric Critical Care Research Network (2016) Incidence and outcomes of cardiopulmonary resuscitation in PICUs. Crit Care Med 44:798–808. https://doi.org/10.1097/CCM.0000000000001484
Holmberg MJ, Wiberg S, Ross CE, Kleinman M, Hoeyer-Nielsen AK, Donnino MW, Andersen LW, For the American Heart Association’s Get With The Guidelines-Resuscitation Investigators (2019) Trends in survival after pediatric in-hospital cardiac arrest in the United States. Circulation 140:1398–1408. https://doi.org/10.1161/CIRCULATIONAHA.119.041667
Girotra S, Spertus JA, Li Y, Berg RA, Nadkarni VM, Chan PS, for the American Heart Association Get With the Guidelines–Resuscitation Investigators (2013) Survival trends in pediatric in-hospital cardiac arrests an analysis from get with the guidelines-resuscitation. Circ Cardiovasc Qual Outcomes 6:42–49. https://doi.org/10.1161/CIRCOUTCOMES.112.967968
Berg RA, Sutton RM, Reeder RW, Berger JT, Newth CJ, Carcillo JA, McQuillen PS, Meert KL, Yates AR, Harrison RE, Moler FW, Pollack MM, Carpenter TC, Wessel DL, Jenkins TL, Notterman DA, Holubkov R, Tamburro RF, Dean JM, Nadkarni VM, Zuppa AF, Graham K, Twelves C, Landis W, DiLiberto MA, Tomanio E, Kwok J, Bell MJ, Abraham A, Sapru A, Alkhouli MF, Heidemann S, Pawluszka A, Hall MW, Steele L, Shanley TP, Weber M, Dalton HJ, Bell AL, Mourani PM, Malone K, Telford R, Coleman W, Peterson A, Thelen J, Doctor A, CPCCRN PICqCPR Investigators (2018) Association between diastolic blood pressure during pediatric in-hospital cardiopulmonary resuscitation and survival. Circulation 137:1784–1795. https://doi.org/10.1161/CIRCULATIONAHA.117.032270
Nadkarni VM, Larkin GL, Peberdy MA, Carey SM, Kaye W, Mancini ME, Nichol G, Lane-Truitt T, Potts J, Ornato JP, Berg RA, National Registry of Cardiopulmonary Resuscitation Investigators (2006) First documented rhythm and clinical outcome from in-hospital cardiac arrest among children and adults. J Am Med Assoc 295:50–57. https://doi.org/10.1001/jama.295.1.50
Agency for Healthcare Research and Quality. Overview of the National (Nationwide) Inpatient Sample (NIS). Available at https://www.hcupus.ahrq.gov/nisoverview.jsp Accessed 23 Sep 2020
Knudson JD, Neish SR, Cabrera AG, Lowry AW, Shamszad P, Morales DL, Graves DE, Williams EA, Rossano JW (2012) Prevalence and outcomes of pediatric in-hospital cardiopulmonary resuscitation in the United States: an analysis of the Kids’ Inpatient Database*. Crit Care Med 40(11):2940–2944. https://doi.org/10.1097/CCM.0b013e31825feb3f
Armstrong RA, Kane C, Oglesby F, Barnard K, Soar J, Thomas M (2019) The incidence of cardiac arrest in the intensive care unit: a systematic review and meta-analysis. J Intensive Care Soc 20:144–154. https://doi.org/10.1177/1751143718774713
Benjamin EJ, Muntner P, Alonso A, Bittencourt MS, Callaway CW, Carson AP, Chamberlain AM, Chang AR, Cheng S, Das SR, Delling FN, Djousse L, Elkind MSV, Ferguson JF, Fornage M, Jordan LC, Khan SS, Kissela BM, Knutson KL, Kwan TW, Lackland DT, Lewis TT, Lichtman JH, Longenecker CT, Loop MS, Lutsey PL, Martin SS, Matsushita K, Moran AE, Mussolino ME, O’Flaherty M, Pandey A, Perak AM, Rosamond WD, Roth GA, Sampson UKA, Satou GM, Schroeder EB, Shah SH, Spartano NL, Stokes A, Tirschwell DL, Tsao CW, Turakhia MP, VanWagner LB, Wilkins JT, Wong SS, Virani SS, On behalf of the American Heart Association Council on Epidemiology and Prevention Statistics Committee and Stroke Statistics Subcommittee (2019) Heart Disease and Stroke Statistics-2019 Update: a report from the American Heart Association. Circulation 139:e56–e528. https://doi.org/10.1161/CIR.0000000000000659
Topjian AA, Raymond TT, Atkins D, Chan M, Duff JP, Joyner BL Jr, Lasa JJ, Lavonas EJ, Levy A, Mahgoub M, Meckler GD, Roberts KE, Sutton RM, Schexnayder SM, Pediatric Basic and Advanced Life Support Collaborators (2020) Part 4: Pediatric Basic and Advanced Life Support: 2020 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 142(16_suppl_2):S469–S523. https://doi.org/10.1161/CIR.0000000000000901
Barbaro RP, Paden ML, Guner YS, Raman L, Ryerson LM, Alexander P, Nasr VG, Bembea MM, Rycus PT, Thiagarajan RR, ELSO member centers (2017) Pediatric Extracorporeal Life Support Organization Registry International Report 2016. ASAIO J 63:456–463. https://doi.org/10.1097/MAT.0000000000000603
Lasa JJ, Rogers RS, Localio R, Shults J, Raymond T, Gaies M, Thiagarajan R, Laussen PC, Kilbaugh T, Berg RA, Nadkarni V, Topjian A (2016) Extracorporeal cardiopulmonary resuscitation (E-CPR) during pediatric in-hospital cardiopulmonary arrest is associated with improved survival to discharge. Circulation 133:165–176. https://doi.org/10.1161/CIRCULATIONAHA.115.016082
Nishisaki A, Pines JM, Lin R, Helfaer MA, Berg RA, Tenhave T, Nadkarni VM (2012) The impact of 24-hr, in-hospital pediatric critical care attending physician presence on process of care and patient outcomes*. Crit Care Med 40(7):2190–2195. https://doi.org/10.1097/CCM.0b013e31824e1cda
Alten JA, Klugman D, Raymond TT, Cooper DS, Donohue JE, Zhang W, Pasquali SK, Gaies MG (2017) Epidemiology and outcomes of cardiac arrest in pediatric cardiac ICUs*. Pediatr Crit Care Med 18:935–943. https://doi.org/10.1097/PCC.0000000000001273
Berg RA, Sutton RM, Holubkov R, Nicholson CE, Dean JM, Harrison R, Heidemann S, Meert K, Newth C, Moler F, Pollack M, Dalton H, Doctor A, Wessel D, Berger J, Shanley T, Carcillo J, Nadkarni VM, Eunice Kennedy Shriver National Institute of Child Health and Human Development Collaborative Pediatric Critical Care Research Network and for the American Heart Association’s Get With the Guidelines-Resuscitation (formerly the National Registry of Cardiopulmonary Resuscitation) Investigators (2013) Ratio of PICU versus ward cardiopulmonary resuscitation events is increasing*. Crit Care Med 41:2292–2297. https://doi.org/10.1097/CCM.0b013e31828cf0c0
Topjian AA, de Caen A, Wainwright MS, Abella BS, Abend NS, Atkins DL, Bembea MM, Fink EL, Guerguerian AM, Haskell SE, Kilgannon JH, Lasa JJ, Hazinski MF (2019) Pediatric post-cardiac arrest care: a scientific statement from the American Heart Association. Circulation 140(6):e194–e233. https://doi.org/10.1161/CIR.0000000000000697
Berens RJ, Cassidy LD, Matchey J, Campbell D, Colpaert KD, Welch T, Lawson M, Peterson C, O’Flynn J, Dearth M, Tieves KS (2011) Probability of survival based on etiology of cardiopulmonary arrest in pediatric patients. Paediatr Anaesth 21:834–840. https://doi.org/10.1111/j.1460-9592.2010.03479.x
Raymond TT, Cunnyngham CB, Thompson MT, Thomas JA, Dalton HJ, Nadkarni VM (2010) Outcomes among neonates, infants, and children after extracorporeal cardiopulmonary resuscitation for refractory inhospital pediatric cardiac arrest: a report from the National Registry of Cardiopulmonary Resuscitation. Pediatr Crit Care Med 11:362–371. https://doi.org/10.1097/PCC.0b013e3181c0141b
Khera R, Tang Y, Girotra S, Nadkarni VM, Link MS, Raymond TT, Guerguerian AM, Berg RA, Chan PS, American Heart Association’s Get With the Guidelines-Resuscitation Investigators (2019) Pulselessness after initiation of cardiopulmonary resuscitation for bradycardia in hospitalized children. Circulation 140(5):370–378. https://doi.org/10.1161/CIRCULATIONAHA.118.039048
Morgan RW, Reeder RW, Meert KL, Telford R, Yates AR, Berger JT, Graham K, Landis WP, Kilbaugh TJ, Newth CJ, Carcillo JA, McQuillen PS, Harrison RE, Moler FW, Pollack MM, Carpenter TC, Notterman D, Holubkov R, Dean JM, Nadkarni VM, Berg RA, Sutton RM, Eunice Kennedy Shriver National Institute of Child Health and Human Development/Collaborative Pediatric Critical Care Research Network (CPCCRN) Pediatric Intensive Care Quality of Cardio-Pulmonary Resuscitation (PICqCPR) Investigators (2020) Survival and hemodynamics during pediatric cardiopulmonary resuscitation for bradycardia and poor perfusion versus pulseless cardiac arrest. Crit Care Med 48(6):881–889. https://doi.org/10.1097/CCM.0000000000004308
Bhanji F, Topjian AA, Nadkarni VM, Praestgaard AH, Hunt EA, Cheng A, Meaney PA, Berg RA, for the American Heart Association’s Get With the Guidelines–Resuscitation Investigators (2017) Survival rates following pediatric in-hospital cardiac arrests during nights and weekends. JAMA Pediatr 171:39–45. https://doi.org/10.1001/jamapediatrics.2016.2535
Peberdy MA, Ornato JP, Larkin GL, Braithwaite RS, Kashner TM, Carey SM, Meaney PA, Cen L, Nadkarni VM, Praestgaard AH, Berg RA, National Registry of Cardiopulmonary Resuscitation Investigators (2008) Survival from in-hospital cardiac arrest during nights and weekends. JAMA 299(7):785–792. https://doi.org/10.1001/jama.299.7.785
Burke CR, Chan T, Brogan TV, McMullan DM (2017) Pediatric extracorporeal cardiopulmonary resuscitation during nights and weekends. Resuscitation 114:47–52. https://doi.org/10.1016/j.resuscitation.2017.03.001
Bembea MM, Ng DK, Rizkalla N, Rycus P, Lasa JJ, Dalton H, Topjian AA, Thiagarajan RR, Nadkarni VM, Hunt EA, American Heart Association’s Get With The Guidelines – Resuscitation Investigators (2019) Outcomes after extracorporeal cardiopulmonary resuscitation of pediatric in-hospital cardiac arrest: a report from the get with the guidelines-resuscitation and the extracorporeal life support organization registries. Crit Care Med 47:e278–e285. https://doi.org/10.1097/CCM.0000000000003622
Ortmann L, Prodhan P, Gossett J, Schexnayder S, Berg R, Nadkarni V, Bhutta A, American Heart Association's Get With the Guidelines–Resuscitation Investigators (2011) Outcomes after in-hospital cardiac arrest in children with cardiac disease: a report from Get With the Guidelines--Resuscitation. Circulation 124(21):2329–2337. https://doi.org/10.1161/CIRCULATIONAHA.110.013466
Author information
Authors and Affiliations
Contributions
Mohammed Hamzah conceptualized and designed the study and drafted the initial manuscript and revised and approved the submitted version. Hasan F. Othman conceptualized and designed the study, drafted the initial manuscript, and revised and approved the submitted version. Mural Al Masri contributed to initial draft and revised and approved the submitted version. Awni al subu contributed to manuscript critical revision and approved the submitted version. Riad Lutfi contributed to manuscript critical revision and approved the submitted version.
Corresponding author
Ethics declarations
Ethics Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Consent to participate
N/A
Consent for publication
N/A
Conflict of Interest
The authors declare no competing interests.
Additional information
Communicated by Piet Leroy
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 16.1 kb )
Rights and permissions
About this article
Cite this article
Hamzah, M., Othman, H.F., Almasri, M. et al. Survival outcomes of in-hospital cardiac arrest in pediatric patients in the USA. Eur J Pediatr 180, 2513–2520 (2021). https://doi.org/10.1007/s00431-021-04082-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-021-04082-3