Abstract
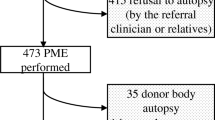
Prevalence of discrepancies between antemortem clinical diagnoses and postmortem autopsy findings is uncertain in pediatric oncology given improving diagnostic capabilities over time. Primary objective was to describe discrepancies between antemortem and postmortem diagnosis of pediatric cancer deaths. Secondary objective was to compare clinical characteristics of deaths with and without major diagnostic discrepancies. This was a retrospective study that included pediatric cancer patients diagnosed and treated in Ontario and who died from 2003 to 2012. Antemortem clinical diagnoses associated with mortality were determined by reviewing the patient’s health records 2 weeks prior to death while the postmortem diagnoses were determined by the autopsy report. Discrepancies among these diagnoses were classified using the Goldman criteria where major discrepancies were directly related to the cause of death in contrast to minor discrepancies. Among the 821 patients who died, 118 (14%) had an autopsy and were included. Of these autopsies, 12 (10%) had a major diagnostic discrepancy between antemortem and postmortem diagnoses. Major discrepancies consisted of opportunistic infections (n = 5), missed cancer diagnosis (n = 3), and organ complications (n = 4). Death in a high acuity setting (12/12, 100% vs. 60/106, 57%; P = 0.003) and treatment-related mortality (12/12, 100% vs. 60/106, 57%; P = 0.003) were significantly associated with major discrepancy. Major diagnostic discrepancy was found in 10% of pediatric oncology autopsies. Missed infections and organ complications were predominant etiologies. Death in a high acuity setting and treatment-related mortality were associated with major diagnostic discrepancies. Autopsies continue to be important for improving diagnostic insight and may improve future clinical care.



Similar content being viewed by others
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- POGO:
-
Pediatric Oncology Group of Ontario
- POGONIS:
-
Pediatric Oncology Group of Ontario Networked Information System
References
Canada PHAo (2017) Cancer in young people in Canada: a report from the enhanced childhood cancer surveillance system. Health Canada
Pritchard-Jones K, Pieters R, Reaman GH et al (2013) Sustaining innovation and improvement in the treatment of childhood cancer: lessons from high-income countries. Lancet Oncol 14(3):e95–e103
SIOPE TESfPO (2015) The SIOPE strategic plan; a European cancer plan for children and adolescents (1st ed.). SIOPE
Koszyca B, Moore L, Toogood I et al (1993) Is postmortem examination useful in pediatric oncology? Pediatr Pathol 13(6):709–715
Kumar P, Taxy J, Angst DB et al (1998) Autopsies in children: are they still useful? Arch Pediatr Adolesc Med 152(6):558–563
Shojania KG, Burton EC, McDonald KM et al (2003) Changes in rates of autopsy-detected diagnostic errors over time: a systematic review. JAMA. 289(21):2849–2856
Nigro JF, Gresik MV, Fernbach DJ (1990) Value of the postmortem examination in a pediatric population with leukemia. J Pediatr 116(3):350–354
Buckner T, Blatt J, Smith SV (2006) The autopsy in pediatrics and pediatric oncology: a single-institution experience. Pediatr Dev Pathol 9(5):374–380
Blanco E, Beyene J, Maloney AM et al (2012) Non-relapse mortality in pediatric acute lymphoblastic leukemia: a systematic review and meta-analysis. Leuk Lymphoma 53(5):878–885
Alexander S, Pole JD, Gibson P et al (2015) Classification of treatment-related mortality in children with cancer: a systematic assessment. Lancet Oncol 16(16):e604–e610
Pole JD, Gibson P, Ethier MC et al (2017) Evaluation of treatment-related mortality among paediatric cancer deaths: a population based analysis. Br J Cancer 116(4):540–545
Battle RM, Pathak D, Humble CG et al (1987) Factors influencing discrepancies between premortem and postmortem diagnoses. JAMA. 258(3):339–344
Pastores SM, Dulu A, Voigt L et al (2007) Premortem clinical diagnoses and postmortem autopsy findings: discrepancies in critically ill cancer patients. Crit Care 11(2):R48
Slavin MA, Heath CH, Thursky KA et al (2008) Antifungal prophylaxis in adult stem cell transplantation and haematological malignancy. Intern Med J 38(6b):468–476
Alexander S, Nieder M, Zerr DM et al (2012) Prevention of bacterial infection in pediatric oncology: what do we know, what can we learn? Pediatr Blood Cancer 59(1):16–20
Science M, Robinson PD, MacDonald T et al (2014) Guideline for primary antifungal prophylaxis for pediatric patients with cancer or hematopoietic stem cell transplant recipients. Pediatr Blood Cancer 61(3):393–400
Stambouly JJ, Kahn E, Boxer RA (1993) Correlation between clinical diagnoses and autopsy findings in critically ill children. Pediatrics. 92(2):248–251
Carlotti AP, Bachette LG, Carmona F et al (2016) Discrepancies between clinical diagnoses and autopsy findings in critically ill children: a prospective study. Am J Clin Pathol 146(6):701–708
Tejerina EE, Padilla R, Abril E et al (2018) Autopsy-detected diagnostic errors over time in the intensive care unit. Hum Pathol 76:85–90
Kelly MS, Spees L, Vinesett R et al (2018) Utility of autopsy among pediatric allogeneic hematopoietic stem cell transplant recipients: one last chance to learn? Biol Blood Marrow Transplant 24(9):1861–1865
Goldstein B, Metlay L, Cox C et al (1996) Association of pre mortem diagnosis and autopsy findings in pediatric intensive care unit versus emergency department versus ward patients. Crit Care Med 24(4):683–686
Funding
This study was funded by an operating grant from the Pediatric Oncology Group of Ontario. LS is the Canada Research Chair in Pediatric Oncology Supportive Care.
Author information
Authors and Affiliations
Contributions
NR and KA collected and analyzed the data and wrote the manuscript. CP, MS, PG, and DJ contributed data. JP critically evaluated the manuscript. SA, UB, and LS analyzed the data. LS wrote the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This study received research ethics board approval from the Hospital for Sick Children Research Ethics Board (#1000041703). Given the retrospective nature of the study, the requirement for informed consent was waived by the SickKids Research Ethics Board.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Code availability
Not applicable.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 21 kb).
Rights and permissions
About this article
Cite this article
Raghuram, N., Alodan, K., Bartels, U. et al. Diagnostic discrepancies between antemortem clinical diagnosis and autopsy findings in pediatric cancer patients. Virchows Arch 478, 1179–1185 (2021). https://doi.org/10.1007/s00428-020-03002-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00428-020-03002-4