Abstract
Introduction
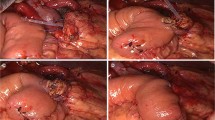
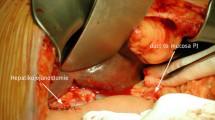
To investigate the application potential of single-layer continuous duct-to-mucosa pancreaticojejunostomy with two figure-of-eight sutures (“1 + 2” PJ) in total laparoscopic pancreaticoduodenectomy (TLPD). Explore the advantages of “1 + 2” PJ over the traditional double-layer interrupted duct-to-mucosa pancreaticojejunostomy (traditional PJ).
Methods
We retrospectively collected the clinical data of 184 patients who were admitted in our department from Oct 2019 to Oct 2022, including 95 cases who underwent TLPD with “1 + 2” PJ and 89 cases who underwent TLPD with traditional PJ. The pre/intra/postoperation data were analyzed and compared.
Results
The “1 + 2” PJ procedures were successfully performed in all the 95 cases. When compared with the traditional PJ group, there were no statistically significant variations between the pre-operative and pathological data. However, the “1 + 2” PJ group had a shorter operation time (235 (210, 300) minutes vs. 310 (270, 360) minutes in the traditional PJ group, P < 0.001), shorter pancreaticojejunostomy time (15 (10, 20) minutes vs. 50 (45, 55) minutes in the traditional PJ group, P < 0.001), lower pancreatic fistula (both grade B/C) rate (4.21% vs. 12.34% in the traditional group, P = 0.044), and abdominal infection rate (2.11% vs. 8.99% in the traditional group, P = 0.044), as well as reduced hospital stay (11 (9, 15) days vs. 13 (11, 15) days in the traditional PJ group, P = 0.013). In the “1 + 2” PJ group, the median diameter of the pancreatic duct was 3 (3, 4) mm; 82 cases (86.31%) had a normal pancreatic texture, while nine (9.47%) cases had a hard texture, and seven (7.37%) cases had a soft texture; the median intraoperative blood loss was 200 (100, 400) mL and 19 cases (20.00%) needed intraoperative transfusion; eight cases (8.4%) developed postoperative complications, including four cases (4.2%) of pancreatic fistula (including both grade B/C), one case (1.1%) of bile leakage, three cases (3.2%) of delayed gastric emptying, three cases (3.2%) of postoperative hemorrhage, two cases (2.1%) of abdominal infection, and one case (1.1%) of reoperation; the median hospital stay was 13 (8, 17) days; 25 cases were pathologically classified as pancreatic cancer, 35 cases as bile duct cancer, 23 cases as duodenal cancer, and 12 cases as ampullary cancer.
Conclusion
Single-layer continuous duct-to-mucosa pancreaticojejunostomy with two figure-of-eight sutures is a feasible and safe procedure that can be applied in TLPD.


Similar content being viewed by others
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Wang M, Li D, Chen R et al (2021) Laparoscopic versus open pancreatoduodenectomy for pancreatic or periampullary tumours: a multicentre, open-label, randomised controlled trial. Lancet Gastroenterol Hepatol 6(6):438–447
Palanivelu C, Senthilnathan P, Sabnis SC et al (2017) Randomized clinical trial of laparoscopic versus open pancreatoduodenectomy for periampullary tumours. Br J Surg 104(11):1443–1450
Jin J, Xiong G, Li J et al (2021) Predictive factors of postoperative pancreatic fistula after laparoscopic pancreatoduodenectomy. Ann Transl Med 9(1):41
Kawaida H, Kono H, Hosomura N et al (2019) Surgical techniques and postoperative management to prevent postoperative pancreatic fistula after pancreatic surgery. World J Gastroenterol 25(28):3722–3737
Hong SS, Chong JU, Hwang HK, Lee WJ, Kang CM (2021) Laparoscopic pancreaticoduodenectomy reduces incidence of clinically relevant postoperative pancreatic fistula in soft pancreas with a smaller than 2 mm pancreatic duct. Surg Endosc 35(12):7094–7103
Gai YW, Wang HT, Tan XD (2022) Pancreaticojejunostomy conducive to biological healing in minimally invasive pancreaticoduodenectomy. J Gastrointest Surg 26(9):1967–1981
Qin R, Kendrick ML, Wolfgang CL et al (2020) International expert consensus on laparoscopic pancreaticoduodenectomy. Hepatobiliary Surg Nutr 9(4):464–483
Liu J, Xing Z, Duan J et al (2018) Application of double-stitch pancreaticojejunostomy in laparoscopic pancreaticoduodenectomy. Chin J Gen Sur 33(03):257–258
Zhang J, Li D, Liu J et al (2019) Clinical application of parachute-like-suture double-pouch pancreaticojejunostomy in laparoscopic pancreaticoduodenectomy. Chin J Hepatobiliary Surg 25(6):431–434. https://doi.org/10.3760/cma.j.issn.1007-8118.2019.06.008
Li Q, Wu Z, Zhang J et al (2022) The use of the single purse-string parachute suturing technique for pancreaticojejunostomy in laparscopic pancreaticoduodenectomy. Chin J Hepatobiliary Surg 28(4):254–258. https://doi.org/10.3760/cma.j.cn113884-20211116-00367
Zhang J, Li Q, Feng F (2018) Clinical application of the modified double-pouch pancreaticojejunostomy in laparoscopic pancreaticoduodenectomy. Chin J Hepatobiliary Surg 24(8):562–564. https://doi.org/10.3760/cma.j.issn.1007-8118.2018.08.016
Chen S, Zhao W, Zhou Z et al (2020) Application of pancreaticojejunostomy with pancreatic duct binding external drainage in laparoscopic pancreatoduodenectomy. Chin J Surg 58(07):516–519. https://doi.org/10.3760/cma.j.cn112139-20191230-00644
Zhang S, Zhou X, Feng F et al (2022) Progress analysis of pancreatic jejunal anastomosis in laparoscopic pancreaticoduodenectomy techniques. Chin J Hepatobiliary Surg 28(6):454–455. https://doi.org/10.3760/cma.j.cn113884-20211210-00408
Schuh F, Mihaljevic AL, Probst P et al (2023) A simple classification of pancreatic duct size and texture predicts postoperative pancreatic fistula: a classification of the International Study Group of Pancreatic Surgery. Ann Surg 277(3):e597–e608
Bassi C, Marchegiani G, Dervenis C et al (2017) The 2016 update of the International Study Group (ISGPS) definition and grading of postoperative pancreatic fistula: 11 years after. Surgery 161(3):584–591
Wente MN, Veit JA, Bassi C et al (2007) Postpancreatectomy hemorrhage (PPH): an International Study Group of Pancreatic Surgery (ISGPS) definition. Surgery 142(1):20–25
Wente MN, Bassi C, Dervenis C et al (2007) Delayed gastric emptying (DGE) after pancreatic surgery: a suggested definition by the International Study Group of Pancreatic Surgery (ISGPS). Surgery 142(5):761–768
Clavien PA, Barkun J, de Oliveira ML et al (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250(2):187–196
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213
de Rooij T, Lu MZ, Steen MW et al (2016) Minimally invasive versus open pancreatoduodenectomy: systematic review and meta-analysis of comparative cohort and registry studies. Ann Surg 264(2):257–267
van Hilst J, de Rooij T, Bosscha K et al (2019) Laparoscopic versus open pancreatoduodenectomy for pancreatic or periampullary tumours (LEOPARD-2): a multicentre, patient-blinded, randomised controlled phase 2/3 trial. Lancet Gastroenterol Hepatol 4(3):199–207
Vladimirov M, Bausch D, Stein HJ, Keck T, Wellner U (2022) Hybrid laparoscopic versus open pancreatoduodenectomy. A meta-analysis World J Surg 46(4):901–915
Liu CZ, Zhu JK, Xu Q, Liu FY, Wang YD, Zhu M (2018) Application of pancreaticojejunostomy with one-layer suture in pancreaticoduodenectomy: a retrospective cohort study. Int J Surg 56:68–72
Li Y, Zhang L, Zeng Z et al (2015) Application value of end-to-side closed in situ pancreaticojejunostomy in pancreaticoduodenectomy. Chin J Dig Surg 14(11):925–929. https://doi.org/10.3760/cma.j.issn.1673-9752.2015.11.009
Zhang L, Li Z, Wu X, Li Y, Zeng Z (2015) Sealing pancreaticojejunostomy in combination with duct parenchyma to mucosa seromuscular one-layer anastomosis: a novel technique to prevent pancreatic fistula after pancreaticoduodenectomy. J Am Coll Surg 220(5):e71–e77
Zeng ZL, Sun Y, Xue D, Liu PL, Chen WM, Zhang L (2020) Effect of six-stitch pancreaticojejunostomy on pancreatic fistula: a propensity score-matched comparative cohort study. Hepatobiliary Pancreat Dis Int 19(3):277–283
Liu Q, Zhao Z, Gao Y et al (2020) Novel single-layer continuous suture of pancreaticojejunostomy for robotic pancreaticoduodenectomy. J Hepatobiliary Pancreat Sci 27(2):56–63
Li B, Xu C, Qiu ZQ et al (2018) An end-to-side suspender pancreaticojejunostomy: a new invagination pancreaticojejunostomy. Hepatobiliary Pancreat Dis Int 17(2):163–168
Fu Y, Wang S, Meng L et al (2022) Application of Hong’s single-stitch duct to mucosa pancreaticoenterostomy in laparoscopic pancreaticoduodenectomy. Chin J Pancreatol 22(3):191–195. https://doi.org/10.3760/cma.j.cn115667-20211021-00193
Hong DF, Liu YH, Zhang YH et al (2017) The role of Hong’s single-stitch duct to mucosa pancreaticojejunostomy in laparoscopic pancreaticoduodenectomy. Zhonghua Wai Ke Za Zhi 55(2):136–140
Hong D, Cheng J, Wu W, Liu X, Zheng X (2021) How to perform total laparoscopic duodenum-preserving pancreatic head resection safely and efficiently with innovative techniques. Ann Surg Oncol 28(6):3209–3216
Ma D, Du G, Yang J et al (2021) Clinical application of a modified double purse-string continuous suture technique for pancreaticojejunostomy: reliable for laparoscopic surgery and small size main pancreatic duct. Biomed Res Int 2021:6676999
Lu Y, Ruan Y, Wang L et al (2020) Application of double-purse-string bridge suture in laparoscopic pancreaticoduodenectomy. Chin J Gen Surg 35(07):563–564. https://doi.org/10.3760/cma.j.cn113855-20191009-00588
Du Y, Wang J, Li Y et al (2019) Clinical application of a modified pancreatojejunostomy technique for laparoscopic pancreaticoduodenectomy. HPB (Oxford) 21(10):1336–1343
Zhou Y, Yang J, Wei L et al (2021) A novel anastomosis technique facilitates pancreaticojejunostomy in total laparoscopic pancreaticoduodenectomy (with video). Langenbecks Arch Surg 406(8):2891–2897
Cai Y, Luo H, Li Y, Gao P, Peng B (2019) A novel technique of pancreaticojejunostomy for laparoscopic pancreaticoduodenectomy. Surg Endosc 33(5):1572–1577
Fujii T, Sugimoto H, Yamada S et al (2014) Modified Blumgart anastomosis for pancreaticojejunostomy: technical improvement in matched historical control study. J Gastrointest Surg 18(6):1108–1115
Geng C, Li J, Nie X et al (2020) Observation study of the healing types of pancreticojejunostomy anastomotic stoma. Chin J Surg 58(03):235–237. https://doi.org/10.3760/cma.j.issn.0529-5815.2020.03.013
Acknowledgements
The manuscript has been approved by the Institutional Ethics Committee(s) of the Second Hospital of Hebei Medical University.
Funding
No competing financial interests exist. This work was supported by the Nature Science Foundation of Hebei Province of China under Grant No. H2022206284.
Author information
Authors and Affiliations
Contributions
DRL, CXD, WHZ, SYL, HTL, and WWB did the clinical work, collected, and analyzed the preclinical and clinical data. WBW and LDR wrote the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This study was performed in accordance with the relevant guidelines and regulations and was approved by the Research Ethics Committee of the Second Hospital of Hebei Medical University (No. 2019-R209). Written informed consent was obtained from all the study subjects.
Consent to publish
The written consent to publish the images and clinical details of the participants in this study was obtained from study participants. Proof of consent to publish from study participants can be requested at any time.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, D., Du, C., Zhao, W. et al. Application of single-layer continuous duct-to-mucosa pancreaticojejunostomy with two figure-of-eight sutures in total laparoscopic pancreaticoduodenectomy. Langenbecks Arch Surg 408, 434 (2023). https://doi.org/10.1007/s00423-023-03155-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00423-023-03155-1