Abstract
Background
Cosmesis is an essential aspect of laparoscopic surgery. Various methods of skin closure techniques have been described. We conducted a study to evaluate the cosmesis and patient satisfaction with the scars three months after laparoscopic surgery using transcutaneous suture (TS) vs. adhesive strips (AS) and subcuticular suturing (SS).
Methods
A randomized, controlled, prospective study was conducted at AIIMS, Bhubaneswar. The included patients were randomly assigned among the three arms. The time for skin closure was measured. Wounds were assessed till discharge, at 14 days, one month, and three months. Cosmesis was measured by the Hollander Wound evaluation scale (HWES) for each incision separately, and patient satisfaction by a 10-
point Visual analog scale (VAS).
Results
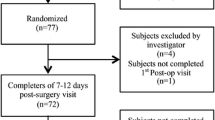
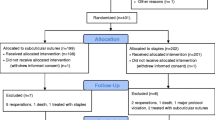
One hundred six patients were assessed for eligibility, and 90 patients were randomized. Three-month follow-up data was obtained from 83 patients (92.22%). Baseline characteristics were similar among the groups. Cosmetic outcome was assessed in 312 incisions across 83 patients, and 206 (66.03%) incisions had an HWE Score of 0, but there was no significant difference (p = 0.86). Patient satisfaction was highest in the TS group (TS = 1.29, SS = 1.79, AS = 2.04, p = 0.03). Time for skin closure was the least in the AS arm (41.4 secs, p = 0.00). Skin dehiscence was significantly more in the AS arm. Four (4.44%) patients had port site infections.
Conclusion
This study demonstrates that skin closure by transcutaneous, subcuticular, or adhesive strip methods had comparable cosmetic outcomes at three months. However, the transcutaneous closure method showed better patient satisfaction and minimal post-operative complications.

Similar content being viewed by others
Data Availability
Raw data supporting the findings of this study are available from the corresponding author, upon reasonable request.
References
Rodeheaver GT, Spengler MD, Edlich RF (1987) Performance of new wound closure tapes. J Emerg Med 5(6):451–462
Zempsky WT, Parrotti D, Grem C, Nichols J (2004) Randomized controlled comparison of cosmetic outcomes of simple facial lacerations closed with Steri Strip™ Skin Closures or Dermabond™ tissue adhesive. Pediatr Emerg Care 20(8):519–524
Romero P, Frongia G, Wingerter S, Holland-Cunz S (2011) Prospective, randomized, controlled trial comparing a tissue adhesive (Dermabond™) with adhesive strips (Steri-Strips™) for the closure of laparoscopic trocar wounds in children. Eur J Pediatr Surg 21(3):159–162
Rosen DMB, Carlton MA (1997) Skin closure at laparoscopy. J Am Assoc Gynecol Laparosc 4(3):347–351
Buchweitz O, Frye C, Moeller CP, Nugent W, Krueger E, Nugent A et al (2016) Cosmetic outcome of skin adhesives versus transcutaneous sutures in laparoscopic port-site wounds: a prospective randomized controlled trial. Surg Endosc 30(6):2326–2331
Quinn J, Wells G, Sutcliffe T (1998) Tissue adhesive versus suture wound repair at 1 year : randomized clinical trial correlating early, 3-month, and 1-year cosmetic outcome. Ann Emerg Med 32(2):645–9
Nguyen TA, Feldstein SI, Shumaker PR, Krakowski AC (2015) A review of scar assessment scales. Semin Cutan Med Surg 34(1):28–36
Hollander JE, Singer AJ, Valentine S, Henry MC (1995) Wound registry: development and validation. Ann Emerg Med 25(5):675–684
Kanegaye JT, Vance CW, Chan L, Schonfeld N (1997) Comparison of skin stapling devices and standard sutures for pediatric scalp lacerations: a randomized study of cost and time benefits. J Pediatr 130(5):808–813
Matin SF (2003) Prospective randomized trial of skin adhesive versus sutures for closure of 217 laparoscopic port-site incisions. J Am Coll Surg 196(6):845–853
Lazar HL, McCann J, Fitzgerald CA, Thompson J, Bao Y, Cabral HJ (2008) Novel adhesive skin closures improve wound healing following saphenous vein harvesting. J Card Surg 23(2):152–155
Buchweitz O, Wülfing P, Kiesel L (2005) A prospective randomized trial of closing laparoscopic trocar wounds by transcutaneous versus subcuticular suture or adhesive papertape. Surg Endosc Other Interv Tech 19(1):148–151
Sajid MS, Siddiqui MR, Khan MA, Baig MK (2009) Meta-analysis of skin adhesives versus sutures in closure of laparoscopic port-site wounds. Surg Endosc 23(6):1191–1197
Huda F, Gajula B, Singh S, Kumar S, Lokavarapu MJ, Sowmya D (2021) Staples versus sutures for skin closure in standard four port laparoscopic cholecystectomy: A prospective cohort study. Cureus 13(3):e13725. https://doi.org/10.7759/cureus.13725
Ranaboldo CJ, Rowe-Jones DC (1992) Closure of Iaparotomy wounds: skin staples versus sutures. Br J Surg 79(11):1172–1173
Martin JG, Hollenbeck ST, Janas G, Makar RA, Pabon-Ramos WM, Suhocki PV et al (2017) Randomized controlled trial of octyl cyanoacrylate skin adhesive versus subcuticular suture for skin closure after implantable venous port placement. J Vasc Interv Radiol [Internet] 28(1):111–6. https://doi.org/10.1016/j.jvir.2016.08.009
Richard M, Seligman SJ (2012) The effect of various wound closure methods. Infection 11203:6–7
Dowson CC, Gilliam AD, Speake WJ, Lobo DN, Beckingham IJ (2006) A prospective, randomized controlled trial comparing n-butyl cyanoacrylate tissue adhesive (liquiband) with sutures for skin closure after laparoscopic general surgical procedures. Surg Laparosc Endosc Percutaneous Tech 16(3):146–150
Guyuron B, Vaughan C (1996) Comparison of polydioxanone and polyglactin 910 in intradermal repair. Plast Reconstr Surg 98(5):817–820
Sheth R, Kamat A, Doshi A, Lodaya B (2012) Cosmetic dermatologic surgery in ethnic skin. In: dermatologic surgery, Nouri K (Ed.), pp 293–298. https://doi.org/10.1002/9781118412633.ch37
Acknowledgements
We are in humble debt to the patients who had participated in this study and for their faith in us.
We would like to give special thanks to Dr. Manash Ranjan Sahoo, Head of the Department, for providing us with ample opportunity and scope to conduct the study with full fervour and ensure that the protocols were being adhered to. Without Sir's guidance and encouragement, it would have been impossible to conduct and complete the study.
Our sincere gratitude to all the faculties Dr. Shantanu K. Sahu, Dr. Mithilesh K. Sinha, Dr. Bikram Rout and Dr. Monika Gureh, who have helped us collect the data and also for their guidance and support.
A special word of thanks goes to Dr. Ankit Sahoo, Dr. Siddhant Sarthak, Dr. Mahesh Sethi, Dr. Harshavardhan H.P., Dr. Vikram VS, Dr. Chiranjeevi H, Dr. Swastik S. Mishra, Dr. Pranav Joshi, Dr. Madhuri KV, Dr. Sanhita Panigrahi, Dr. Ankit Shetter, Dr. Preeti K. Gond and Dr. Umesha R, Dr. Bhargavi, Dr. Pravanjan, Dr. Ankit Rana, Dr. Sai Krishna, Dr. ShriGanesh and Dr. Medhavi, who have supported us in data collection and follow-up. This study would not have been possible without the support of the anaesthesiology team and the nursing staff in the elective OT complex. We would like to thank all the nursing staff in the OPD, OT and Ward for being supportive in the process.
Author information
Authors and Affiliations
Contributions
Dr. Pradeep, Dr. Kallol, and Dr. Prakash conceptualised the study, did review of the literature, and prepared the study protocol. All the authors followed all the patients. Dr. Pradeep and Dr. Kallol did the data collection. Dr. Pradeep, Dr. Kallol, and Dr. Prakash prepared the draft manuscript and analysed the data. The final manuscript was prepared after review by all the co-authors.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Disclosures
Dr. Pradeep Kumar Singh, Dr. Kallol Kumar Das Poddar, Dr. Prakash Kumar Sasmal, Dr. Pankaj Kumar, Dr. S. Manwar Ali and Dr. Tushar Subhadarshan Mishra have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Singh, P.K., Das Poddar, K.K., Sasmal, P.K. et al. Comparison of laparoscopic port site skin closure techniques (CLOSA): transcutaneous suturing versus subcuticular sutures versus adhesive strips: a prospective single-blinded randomized control trial. Langenbecks Arch Surg 408, 228 (2023). https://doi.org/10.1007/s00423-023-02950-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00423-023-02950-0