Abstract
Background
Clinically relevant postoperative pancreatic fistula (CR-POPF) is a common complication after pancreaticoduodenectomy (PD). However, whether irrigation-suction (IS) decreases the incidence and severity of CR-POPF has not yet been well elucidated.
Methods
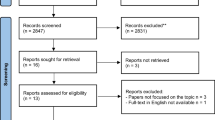
One hundred and twenty patients with planned PD were enrolled in the study at a high-volume pancreatic center in China from August 2018 to January 2020. A randomized controlled trial (RCT) was conducted to evaluate whether irrigation-suction (IS) decreases the incidence and severity of CR-POPF and other postoperative complications after PD. The primary endpoint was the incidence of CR-POPF, and the secondary endpoints were other postoperative complications.
Results
Sixty patients were assigned to the control group and 60 patients to the IS group. The IS group had a comparable POPF rate (15.0% vs. 18.3%, p = 0.806) but a lower incidence of intra-abdominal infection (8.3% vs. 25.0%, p = 0.033) than the control group. The incidences of other postoperative complications were comparable in the two groups. The subgroup analysis for patients with intermediate/high risks for POPF also showed an equivalent POPF rate (17.0% vs. 20.4%, p = 0.800) and a significantly decreased incidence of intra-abdominal infection (8.5% vs. 27.8%, p = 0.020) in the IS group than that in the control group. The logistic regression models indicated that POPF was an independent risk factor for intra-abdominal infection (OR 0.049, 95% CI 0.013-0.182, p = 0.000).
Conclusions
Irrigation-suction near pancreaticojejunostomy does not reduce the incidence or severity of postoperative pancreatic fistula but decreases the incidence of intra-abdominal infection after pancreaticoduodenectomy.


Similar content being viewed by others
References
Simon R (2021) Complications after pancreaticoduodenectomy. Surg Clin North Am 101(5):865–874. https://doi.org/10.1016/j.suc.2021.06.011
Ellis RJ, Brock Hewitt D, Liu JB, Cohen ME, Merkow RP, Bentrem DJ, Bilimoria KY, Yang AD (2019) Preoperative risk evaluation for pancreatic fistula after pancreaticoduodenectomy. J Surg Oncol 119(8):1128–1134. https://doi.org/10.1002/jso.25464
Andrianello S, Marchegiani G, Malleo G, Masini G, Balduzzi A, Paiella S, Esposito A, Landoni L, Casetti L, Tuveri M, Salvia R, Bassi C (2020) Pancreaticojejunostomy with externalized stent vs pancreaticogastrostomy with externalized stent for patients with high-risk pancreatic anastomosis: a single-center, phase 3, randomized clinical trial. JAMA Surg 155(4):313–321. https://doi.org/10.1001/jamasurg.2019.6035
Smits FJ, van Santvoort HC, Besselink MG, Batenburg MCT, Slooff RAE, Boerma D, Busch OR, Coene P, van Dam RM, van Dijk DPJ, van Eijck CHJ, Festen S, van der Harst E, de Hingh I, de Jong KP, Tol J, Borel Rinkes IHM, Molenaar IQ, Dutch Pancreatic Cancer G (2017) Management of severe pancreatic fistula after pancreatoduodenectomy. JAMA Surg 152(6):540–548. https://doi.org/10.1001/jamasurg.2016.5708
Luu AM, Krasemann L, Fahlbusch T, Belyaev O, Janot-Matuschek M, Uhl W, Braumann C (2020) Facing the surgeon’s nightmare: incidence and management of postoperative pancreatic fistulas grade C after pancreaticoduodenectomy based on the updated definition of the International Study Group of Pancreatic Surgery (ISGPS). J Hepatobiliary Pancreat Sci 27(4):171–181. https://doi.org/10.1002/jhbp.713
Keck T, Wellner UF, Bahra M, Klein F, Sick O, Niedergethmann M, Wilhelm TJ, Farkas SA, Borner T, Bruns C, Kleespies A, Kleeff J, Mihaljevic AL, Uhl W, Chromik A, Fendrich V, Heeger K, Padberg W, Hecker A et al (2016) Pancreatogastrostomy versus pancreatojejunostomy for RECOnstruction After PANCreatoduodenectomy (RECOPANC, DRKS 00000767): perioperative and long-term results of a multicenter randomized controlled trial. Ann Surg 263(3):440–449. https://doi.org/10.1097/SLA.0000000000001240
Sunagawa M, Yokoyama Y, Yamaguchi J, Ebata T, Sugawara G, Igami T, Mizuno T, Nagino M (2019) Is constant negative pressure for external drainage of the main pancreatic duct useful in preventing pancreatic fistula following pancreatoduodenectomy? Pancreatology 19(4):602–607. https://doi.org/10.1016/j.pan.2019.04.002
Dong Z, Xu J, Wang Z, Petrov MS (2016) Stents for the prevention of pancreatic fistula following pancreaticoduodenectomy. Cochrane Database Syst Rev 2016(5):CD008914. https://doi.org/10.1002/14651858.CD008914.pub3
Tarvainen T, Siren J, Kokkola A, Sallinen V (2020) Effect of hydrocortisone vs pasireotide on pancreatic surgery complications in patients with high risk of pancreatic fistula: a randomized clinical trial. JAMA Surg 155(4):291–298. https://doi.org/10.1001/jamasurg.2019.6019
Cao Z, Qiu J, Guo J, Xiong G, Jiang K, Zheng S, Kuang T, Wang Y, Zhang T, Sun B, Qin R, Chen R, Miao Y, Lou W, Zhao Y (2021) A randomised, multicentre trial of somatostatin to prevent clinically relevant postoperative pancreatic fistula in intermediate-risk patients after pancreaticoduodenectomy. J Gastroenterol 56(10):938–948. https://doi.org/10.1007/s00535-021-01818-8
Brubaker LS, Casciani F, Fisher WE, Wood AL, Cagigas MN, Trudeau MT, Parikh VJ, Baugh KA, Asbun HJ, Ball CG, Behrman SW, Berger AC, Bloomston MP, Callery MP, Christein JD, Fernandez-Del Castillo C, Dillhoff ME, Dixon E, House MG, Hughes SJ, Kent TS, Kunstman JW, Wolfgang CL, Zureikat AH, Vollmer CM, Jr., Van Buren G, 2nd (2021) A risk-adjusted analysis of drain use in pancreaticoduodenectomy: some is good, but more may not be better. Surgery 171(4):1058-1066https://doi.org/10.1016/j.surg.2021.07.026
Linnemann RJA, Patijn GA, van Rijssen LB, Besselink MG, Mungroop TH, de Hingh IH, Kazemier G, Festen S, de Jong KP, van Eijck CHJ, Scheepers JJG, van der Kolk M, Dulk MD, Bosscha K, Busch OR, Boerma D, van der Harst E, Nieuwenhuijs VB, Dutch Pancreatic Cancer G (2019) The role of abdominal drainage in pancreatic resection - a multicenter validation study for early drain removal. Pancreatology 19(6):888–896. https://doi.org/10.1016/j.pan.2019.07.041
Maehira H, Iida H, Mori H, Yasukawa D, Maekawa T, Muramoto K, Takebayashi K, Kaida S, Miyake T, Tani M (2021) Superior perianastomotic fluid collection in the early postoperative period affects pseudoaneurysm occurrence after pancreaticoduodenectomy. Langenbecks Arch Surg 406(5):1461–1468. https://doi.org/10.1007/s00423-020-02072-x
Adamenko O, Ferrari C, Porreca A, Seewald S, Groth S, Gutzwiller J-P, Kulaksiz H, Schmidt J (2022) Perianastomotic irrigation with passive drainage dramatically decreases POPF rate after high-risk pancreaticoduodenectomy. Annals of Surgery Open 3(2):e154. https://doi.org/10.1097/as9.0000000000000154
Cecka F, Jon B, Skalicky P, Cermakova E, Neoral C, Lovecek M (2018) Results of a randomized controlled trial comparing closed-suction drains versus passive gravity drains after pancreatic resection. Surgery 164(5):1057–1063. https://doi.org/10.1016/j.surg.2018.05.030
Marchegiani G, Perri G, Pulvirenti A, Sereni E, Azzini AM, Malleo G, Salvia R, Bassi C (2018) Non-inferiority of open passive drains compared with closed suction drains in pancreatic surgery outcomes: a prospective observational study. Surgery 164(3):443–449. https://doi.org/10.1016/j.surg.2018.04.025
Kone LB, Maker VK, Banulescu M, Maker AV (2020) Should drains suck? A propensity score analysis of closed-suction versus closed-gravity drainage after pancreatectomy. J Gastrointest Surg 25(5):1224–1232. https://doi.org/10.1007/s11605-020-04613-7
Tol JA, Gouma DJ, Bassi C, Dervenis C, Montorsi M, Adham M, Andren-Sandberg A, Asbun HJ, Bockhorn M, Buchler MW, Conlon KC, Fernandez-Cruz L, Fingerhut A, Friess H, Hartwig W, Izbicki JR, Lillemoe KD, Milicevic MN, Neoptolemos JP et al (2014) Definition of a standard lymphadenectomy in surgery for pancreatic ductal adenocarcinoma: a consensus statement by the International Study Group on Pancreatic Surgery (ISGPS). Surgery 156(3):591–600. https://doi.org/10.1016/j.surg.2014.06.016
Yamashita K, Sasaki T, Itoh R, Kato D, Hatano N, Soejima T, Ishii K, Takenawa T, Hiromatsu K, Yamashita Y (2015) Pancreatic fistulae secondary to trypsinogen activation by Pseudomonas aeruginosa infection after pancreatoduodenectomy. J Hepatobiliary Pancreat Sci 22(6):454–462. https://doi.org/10.1002/jhbp.223
Bassi C, Marchegiani G, Dervenis C, Sarr M, Abu Hilal M, Adham M, Allen P, Andersson R, Asbun HJ, Besselink MG, Conlon K, Del Chiaro M, Falconi M, Fernandez-Cruz L, Fernandez-Del Castillo C, Fingerhut A, Friess H, Gouma DJ, Hackert T et al (2017) The 2016 update of the International Study Group (ISGPS) definition and grading of postoperative pancreatic fistula: 11 Years After. Surgery 161(3):584–591. https://doi.org/10.1016/j.surg.2016.11.014
Wente MN, Bassi C, Dervenis C, Fingerhut A, Gouma DJ, Izbicki JR, Neoptolemos JP, Padbury RT, Sarr MG, Traverso LW, Yeo CJ, Buchler MW (2007) Delayed gastric emptying (DGE) after pancreatic surgery: a suggested definition by the International Study Group of Pancreatic Surgery (ISGPS). Surgery 142(5):761–768. https://doi.org/10.1016/j.surg.2007.05.005
Besselink MG, van Rijssen LB, Bassi C, Dervenis C, Montorsi M, Adham M, Asbun HJ, Bockhorn M, Strobel O, Buchler MW, Busch OR, Charnley RM, Conlon KC, Fernandez-Cruz L, Fingerhut A, Friess H, Izbicki JR, Lillemoe KD, Neoptolemos JP et al (2017) Definition and classification of chyle leak after pancreatic operation: a consensus statement by the International Study Group on Pancreatic Surgery. Surgery 161(2):365–372. https://doi.org/10.1016/j.surg.2016.06.058
Wente MN, Veit JA, Bassi C, Dervenis C, Fingerhut A, Gouma DJ, Izbicki JR, Neoptolemos JP, Padbury RT, Sarr MG, Yeo CJ, Buchler MW (2007) Postpancreatectomy hemorrhage (PPH): an International Study Group of Pancreatic Surgery (ISGPS) definition. Surgery 142(1):20–25. https://doi.org/10.1016/j.surg.2007.02.001
Shubert CR, Wagie AE, Farnell MB, Nagorney DM, Que FG, Reid Lombardo KM, Truty MJ, Smoot RL, Kendrick ML (2015) Clinical risk score to predict pancreatic fistula after pancreatoduodenectomy: independent external validation for open and laparoscopic approaches. J Am Coll Surg 221(3):689–698. https://doi.org/10.1016/j.jamcollsurg.2015.05.011
Bertens KA, Crown A, Clanton J, Alemi F, Alseidi AA, Biehl T, Helton WS, Rocha FG (2017) What is a better predictor of clinically relevant postoperative pancreatic fistula (CR-POPF) following pancreaticoduodenectomy (PD): postoperative day one drain amylase (POD1DA) or the fistula risk score (FRS)? HPB (Oxford) 19(1):75–81. https://doi.org/10.1016/j.hpb.2016.10.001
McMillan MT, Soi S, Asbun HJ, Ball CG, Bassi C, Beane JD, Behrman SW, Berger AC, Bloomston M, Callery MP, Christein JD, Dixon E, Drebin JA, Castillo CF, Fisher WE, Fong ZV, House MG, Hughes SJ, Kent TS et al (2016) Risk-adjusted outcomes of clinically relevant pancreatic fistula following pancreatoduodenectomy: a model for performance evaluation. Ann Surg 264(2):344–352. https://doi.org/10.1097/SLA.0000000000001537
Horiuchi A, Watanabe Y, Sato K, Yoshida M, Yamamoto Y, Sugishita H, Kameoka K, Kawachi K (2010) Continuous irrigation with gabexate mesilate around pancreaticojejunostomy after pancreaticoduodenectomy. Hepatogastroenterology 57(102-103):1291–1294
Van Buren G, Bloomston M, Hughes SJ, Winter J, Behrman SW, Zyromski NJ, Vollmer C, Velanovich V, Riall T, Muscarella P, Trevino J, Nakeeb A, Schmidt CM, Behrns K, Ellison EC, Barakat O, Perry KA, Drebin J, House M et al (2014) A randomized prospective multicenter trial of pancreaticoduodenectomy with and without routine intraperitoneal drainage. Ann Surg 259(4):605–612. https://doi.org/10.1097/SLA.0000000000000460
Jiang H, Liu N, Zhang M, Lu L, Dou R, Qu L (2016) A randomized trial on the efficacy of prophylactic active drainage in prevention of complications after pancreaticoduodenectomy. Scand J Surg 105(4):215–222. https://doi.org/10.1177/1457496916665543
Maatman TK, Weber DJ, Timsina LR, Qureshi B, Ceppa EP, Nakeeb A, Schmidt CM, Zyromski NJ, Koniaris LG, House MG (2019) Antibiotic irrigation during pancreatoduodenectomy to prevent infection and pancreatic fistula: a randomized controlled clinical trial. Surgery 166(4):469–475. https://doi.org/10.1016/j.surg.2019.05.053
Ludolph I, Fried FW, Kneppe K, Arkudas A, Schmitz M, Horch RE (2018) Negative pressure wound treatment with computer-controlled irrigation/instillation decreases bacterial load in contaminated wounds and facilitates wound closure. Int Wound J 15(6):978–984. https://doi.org/10.1111/iwj.12958
Eisenberg JD, Rosato EL, Lavu H, Yeo CJ, Winter JM (2015) Delayed gastric emptying after pancreaticoduodenectomy: an analysis of risk factors and cost. J Gastrointest Surg 19(9):1572–1580. https://doi.org/10.1007/s11605-015-2865-5
Yamashita K, Kato D, Sasaki T, Shiwaku H, Ishii F, Naito S, Yamashita Y, Hasegawa S (2018) Contaminated drainage fluid and pancreatic fistula after pancreatoduodenectomy: a retrospective study. Int J Surg 52:314–319. https://doi.org/10.1016/j.ijsu.2018.02.057
Hata T, Mizuma M, Motoi F, Nakagawa K, Masuda K, Ishida M, Morikawa T, Hayashi H, Kamei T, Naitoh T, Unno M (2020) Early postoperative drainage fluid culture positivity from contaminated bile juice is predictive of pancreatic fistula after pancreaticoduodenectomy. Surg Today 50(3):248–257. https://doi.org/10.1007/s00595-019-01885-8
Demir E, Abdelhai K, Demir IE, Jager C, Scheufele F, Schorn S, Rothe K, Friess H, Ceyhan GO (2020) Association of bacteria in pancreatic fistula fluid with complications after pancreatic surgery. BJS Open 4(3):432–437. https://doi.org/10.1002/bjs5.50272
McMillan MT, Fisher WE, Van Buren G, McEIhany A, Bloomston M, Hughes SJ, Winter J, Behrman SW, Zyromski NJ, Velanovich V, Brown K, Morgan KA, Vollmer C (2015) The value of drains as a fistula mitigation strategy for pancreatoduodenectomy: something for everyone? Results of a randomized prospective multi-institutional study. J Gastrointest Surg 19(1):21–30. https://doi.org/10.1007/s11605-014-2640-z
McMillan MT, Malleo G, Bassi C, Butturini G, Salvia R, Roses RE, Lee MK, Fraker DL, Drebin JA, Vollmer CM Jr (2015) Drain management after pancreatoduodenectomy: reappraisal of a prospective randomized trial using risk stratification. J Am Coll Surg 221(4):798–809. https://doi.org/10.1016/j.jamcollsurg.2015.07.005
McMillan MT, Malleo G, Bassi C, Allegrini V, Casetti L, Drebin JA, Esposito A, Landoni L, Lee MK, Pulvirenti A, Roses RE, Salvia R, Vollmer CM Jr (2017) Multicenter, prospective trial of selective drain management for pancreatoduodenectomy using risk stratification. Ann Surg 265(6):1209–1218. https://doi.org/10.1097/SLA.0000000000001832
Dai M, Liu Q, Xing C, Tian X, Cao F, Tang W, Lv S, Ma Y, Zhang D, Kleeff J, Yang Y, Liu R, He Q, Li F, Li G, Guo J, Liao Q, Zhao Y (2021) Early drain removal is safe in patients with low or intermediate risk of pancreatic fistula after pancreaticoduodenectomy: a multicenter, randomized controlled trial. Ann Surg 275(2):e307–e314. https://doi.org/10.1097/SLA.0000000000004992
Nakano H, Asakura T, Sakurai J, Koizumi S, Asano T, Watanabe T, Otsubo T (2008) Prophylactic irrigation around a pancreaticojejunostomy for the treatment of a pancreatic fistula after a pancreaticoduodenectomy in patients with a risky pancreatic remnant. Hepatogastroenterology 55(82-83):717–721
Barie PS (2002) Are we draining the life from our patients? Surg Infect (Larchmt) 3(3):159–160. https://doi.org/10.1089/109629602761624162
Funding
The study was supported by Medical Minimally Invasive Center Program of Fujian Province, China (no. 2017-171) and Key Clinical Specialty Discipline Construction Program of Fujian Province, China (no. 2012-649).
Author information
Authors and Affiliations
Contributions
(I) Conception and design: Ronggui Lin and Heguang Huang; (II) acquisition of data: Yuanyuan Yang, Congfei Wang, and Haizong Fang; (III) data analysis and interpretation: Xianchao Lin, Fengchun Lu, and Yanchang Chen; (IV) manuscript writing: Yuhuang Liu and Ronggui Lin; (V) final approval of manuscript: all authors.
Corresponding author
Ethics declarations
Ethical approval
This study was approved by the Ethical Committee of Fujian Medical University Union Hospital (2018YF014-02).
Human and animal rights
This article does not contain any studies with animals performed by any of the authors.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lin, R., Liu, Y., Lin, X. et al. A randomized controlled trial evaluating effects of prophylactic irrigation-suction near pancreaticojejunostomy on postoperative pancreatic fistula after pancreaticoduodenectomy. Langenbecks Arch Surg 408, 137 (2023). https://doi.org/10.1007/s00423-023-02873-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00423-023-02873-w