Abstract
Purpose
Two non-inferiority randomised control trials have questioned the utility of laparoscopic surgery for rectal cancer by failing to prove that pathological markers of high-quality surgery are equivalent to those achieved by open technique. We present short- and long-term post-operative outcomes from the largest single surgeon series of consecutive patients undergoing laparoscopic TME for rectal cancer. We describe the standardised laparoscopic technique developed by the principal surgeon, and the short-term outcomes from three surgeons who were trained in and subsequently adopted the same approach.
Methods
Prospectively acquired data from consecutive patients undergoing surgery for rectal cancer by the principal surgeon at the minimally invasive colorectal unit in Portsmouth between 2006 and 2014 were analysed along with data acquired between 2010 and 2017 from surgeons at three further international centres. Endpoints were overall and disease-free survival at 5 years, and early post-operative clinical and pathological outcomes.
Results
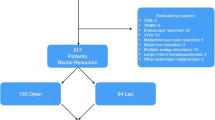
Two hundred sixty-three consecutive patients underwent laparoscopic TME surgery by the principal surgeon. At 5 years, overall survival was 82.9% (Dukes’ A = 94.4%; B = 81.6%; C = 73.7%); disease-free survival was 84.0% (Dukes’ A = 93.3%; B = 86.8%; C = 72.6%). Post-operative length of stay, lymph node harvest, mean operating time, rate of conversion, major morbidity and 30-day mortality were not significantly different between the principal surgeon and those he had trained when subsequently in independent practices.
Conclusion
Laparoscopic TME produces excellent long-term survival outcomes for patients with rectal cancer. A standardised approach has the potential to improve outcomes by setting benchmarks for surgical quality, and providing a step-by-step method for surgical training.


Similar content being viewed by others
References
MacFarlane JK, Ryall RD, Heald RJ (1993) Mesorectal excision for rectal cancer. Lancet 341(8843):457–460
Heald RJ (1988) The “Holy Plane” of rectal surgery. J R Soc Med 81(9):503–508
Heald RJ, Ryall RD (1986) Recurrence and survival after total mesorectal excision for rectal cancer. Lancet 1(8496):1479–1482
Vennix S, Pelzers L, Bouvy N, Beets GL, Pierie JP, Wiggers T et al (2014) Laparoscopic versus open total mesorectal excision for rectal cancer. Cochrane Database Syst Rev 4:CD005200
Green BL, Marshall HC, Collinson F, Quirke P, Guillou P, Jayne DG, Brown JM (2013) Long-term follow-up of the Medical Research Council CLASICC trial of conventional versus laparoscopically assisted resection in colorectal cancer. Br J Surg 100(1):75–82
Bonjer HJ, Deijen CL, Haglind E, Group CIS (2015) A randomized trial of laparoscopic versus open surgery for rectal Cancer. N Engl J Med 373(2):194
Nussbaum DP, Speicher PJ, Ganapathi AM, Englum BR, Keenan JE, Mantyh CR et al (2015) Laparoscopic versus open low anterior resection for rectal cancer: results from the national cancer data base. J Gastrointest Surg 19(1):124–131 discussion 31–2
Draeger T, Volkel V, Gerken M, Klinkhammer-Schalke M, Furst A (2018) Long-term oncologic outcomes after laparoscopic versus open rectal cancer resection: a high-quality population-based analysis in a Southern German district. Surg Endosc 32(10):4096–4104
Jeong SY, Park JW, Nam BH, Kim S, Kang SB, Lim SB, Choi HS, Kim DW, Chang HJ, Kim DY, Jung KH, Kim TY, Kang GH, Chie EK, Kim SY, Sohn DK, Kim DH, Kim JS, Lee HS, Kim JH, Oh JH (2014) Open versus laparoscopic surgery for mid-rectal or low-rectal cancer after neoadjuvant chemoradiotherapy (COREAN trial): survival outcomes of an open-label, non-inferiority, randomised controlled trial. Lancet Oncol 15(7):767–774
Fleshman J, Branda M, Sargent DJ, Boller AM, George V, Abbas M, Peters WR Jr, Maun D, Chang G, Herline A, Fichera A, Mutch M, Wexner S, Whiteford M, Marks J, Birnbaum E, Margolin D, Larson D, Marcello P, Posner M, Read T, Monson J, Wren SM, Pisters PWT, Nelson H (2015) Effect of laparoscopic-assisted resection vs open resection of stage II or III rectal cancer on pathologic outcomes: the ACOSOG Z6051 randomized clinical trial. JAMA 314(13):1346–1355
Stevenson AR, Solomon MJ, Lumley JW, Hewett P, Clouston AD, Gebski VJ, Davies L, Wilson K, Hague W, Simes J, ALaCaRT Investigators (2015) Effect of laparoscopic-assisted resection vs open resection on pathological outcomes in rectal cancer: the ALaCaRT randomized clinical trial. JAMA 314(13):1356–1363
Abbas SK, Yelika SB, You K, Mathai J, Essani R, Krivokapic Z et al (2017) Rectal cancer should not be resected laparoscopically: the rationale and the data. Tech Coloproctol 21(3):237–240
Martinez-Perez A, Carra MC, Brunetti F, de’Angelis N (2017) Pathologic outcomes of laparoscopic vs open mesorectal excision for rectal cancer: a systematic review and meta-analysis. JAMA Surg 152(4):e165665
Spinelli A, D'Hoore A, Panis Y, Bemelman WA, Jayne DG, Furst A (2017) Critical appraisal of two randomized clinical trials on pathologic outcomes laparoscopic vs. open resection for rectal cancer. Coloproctology 39(4):277
Quirke P, Durdey P, Dixon MF, Williams NS (1986) Local recurrence of rectal adenocarcinoma due to inadequate surgical resection. Histopathological study of lateral tumour spread and surgical excision. Lancet 2(8514):996–999
Nagtegaal ID, Quirke P (2008) What is the role for the circumferential margin in the modern treatment of rectal cancer? J Clin Oncol 26(2):303–312
Xiong B, Ma L, Huang W, Zhao Q, Cheng Y, Liu J (2015) Robotic versus laparoscopic total mesorectal excision for rectal cancer: a meta-analysis of eight studies. J Gastrointest Surg 19(3):516–526
Penna M, Hompes R, Arnold S, Wynn G, Austin R, Warusavitarne J, Moran B, Hanna GB, Mortensen NJ, Tekkis PP, TaTME Registry Collaborative (2017) Transanal total mesorectal excision: international registry results of the first 720 cases. Ann Surg 266(1):111–117
Guillou PJ, Quirke P, Thorpe H, Walker J, Jayne DG, Smith AM et al (2005) Short-term endpoints of conventional versus laparoscopic-assisted surgery in patients with colorectal cancer (MRC CLASICC trial): multicentre, randomised controlled trial. Lancet 365(9472):1718–1726
Rickles AS, Dietz DW, Chang GJ, Wexner SD, Berho ME, Remzi FH, Greene FL, Fleshman JW, Abbas MA, Peters W, Noyes K, Monson JR, Fleming FJ, Consortium for Optimizing the Treatment of Rectal Cancer (OSTRiCh) (2015) High rate of positive circumferential resection margins following rectal cancer surgery: a call to action. Ann Surg 262(6):891–898
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, de Santibañes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250(2):187–196
Kehlet H (1997) Multimodal approach to control postoperative pathophysiology and rehabilitation. Br J Anaesth 78(5):606–617
Hemandas A, Flashman KG, Farrow J, O'Leary DP, Parvaiz A (2011) Modular training in laparoscopic colorectal surgery maximizes training opportunities without clinical compromise. World J Surg 35(2):409–414
van der Pas MH, Haglind E, Cuesta MA, Furst A, Lacy AM, Hop WC et al (2013) Laparoscopic versus open surgery for rectal cancer (COLOR II): short-term outcomes of a randomised, phase 3 trial. Lancet Oncol 14(3):210–218
Jayne DG, Thorpe HC, Copeland J, Quirke P, Brown JM, Guillou PJ (2010) Five-year follow-up of the Medical Research Council CLASICC trial of laparoscopically assisted versus open surgery for colorectal cancer. Br J Surg 97(11):1638–1645
Galandiuk S (2015) Standardization or centralization: can one have one without the other? Circumferential resection margins and rectal Cancer. Ann Surg 262(6):899–900
Miskovic D, Foster J, Agha A, Delaney CP, Francis N, Hasegawa H, Karachun A, Kim SH, Law WL, Marks J, Morino M, Panis Y, Uriburu JCP, Wexner SD, Parvaiz A (2015) Standardization of laparoscopic total mesorectal excision for rectal cancer: a structured international expert consensus. Ann Surg 261(4):716–722
Mack LA, Temple WJ (2005) Education is the key to quality of surgery for rectal cancer. Eur J Surg Oncol 31(6):636–644
Cheung HY, Ng KH, Leung AL, Chung CC, Yau KK, Li MK (2011) Laparoscopic sphincter-preserving total mesorectal excision: 10-year report. Color Dis 13(6):627–631
Staudacher C, Di Palo S, Tamburini A, Vignali A, Orsenigo E (2007) Total mesorectal excision (TME) with laparoscopic approach: 226 consecutive cases. Surg Oncol 16(Suppl 1):S113–S116
Sartori CA, Dal Pozzo A, Franzato B, Balduino M, Sartori A, Baiocchi GL (2011) Laparoscopic total mesorectal excision for rectal cancer: experience of a single center with a series of 174 patients. Surg Endosc 25(2):508–514
Author information
Authors and Affiliations
Contributions
Acquisition of data by Marc Bullock, Anil Hemandas, Tahseen Qureshi, Nuno Figueiredo and Amjad Parvaiz; analysis and interpretation of data was done by Marc Bullock, Irfan Ul Islam Nasir, Anil Hemandas, Tahseen Qureshi, Nuno Figueiredo and Amjad Parvaiz; drafting of manuscript was done by Marc Bullock, Irfan Ul Islam Nasir, Anil Hemandas, Tahseen Qureshi, Nuno Figueiredo, Richard Heald and Amjad Parvaiz; critical revision of manuscript was done by Marc Bullock, Irfan Ul Islam Nasir, Richard Heald and Amjad Parvaiz.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bullock, M., Nasir, I.U.I., Hemandas, A. et al. Standardised approach to laparoscopic total mesorectal excision for rectal cancer: a prospective multi-centre analysis. Langenbecks Arch Surg 404, 547–555 (2019). https://doi.org/10.1007/s00423-019-01806-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-019-01806-w