Abstract
Purpose
The present study compared the prognostic value of the lymph node ratio (LNR) and the 6th and the 7th TNM edition as three different lymph node classifications for rectal cancer patients.
Methods
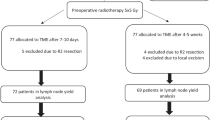
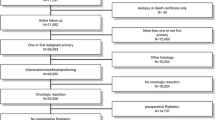
A total of 630 patients who underwent total mesorectal excision for primary rectal cancer between October 2001 and December 2007 were included. Prognostic factors of overall survival were analyzed using Cox proportional hazards models.
Results
The median follow-up was 36.1 months and the 5-year overall survival rate was 70.3 ± 4.7%. The median number of lymph nodes was 15.0 (12.0–19.0). All three lymph node evaluations correlated with survival (p < 0.0001). The assessment of nodal status in the 7th TNM edition enabled further prognostic stratification. The prognostic value of the three classifications were independent of neoadjuvant therapy and lymph node count. On multivariate analyses, the N2 stage of the 6th TNM edition (Hazard ratio 2.08; 95% confidence interval 1.21–3.58) and the N2b stage of the 7th TNM edition (2.18; 1.17–4.07) correlated with poor survival. A LNR of 0.42–0.69 was also associated with unfavorable prognosis (2.97; 1.46–6.03), as was an LNR > 0.69 (2.51; 1.04–6.05). The LNR did not provide prognostic information in addition to the N stage of the TNM classifications.
Conclusions
The evaluated lymph node classifications were of comparable prognostic utility in patients with rectal cancer. The LNR did not provide prognostic information in addition to the N stage of the TNM classifications.

Similar content being viewed by others
References
Phillips RK, Hittinger R, Blesovsky L, Fry JS, Fielding LP (1984) Local recurrence following 'curative' surgery for large bowel cancer: II. The rectum and rectosigmoid. Br J Surg 71(1):17–20
Quirke P, Durdey P, Dixon MF, Williams NS (1986) Local recurrence of rectal adenocarcinoma due to inadequate surgical resection. Histopathological study of lateral tumour spread and surgical excision. Lancet 2(8514):996–999
Heald RJ, Ryall RD (1986) Recurrence and survival after total mesorectal excision for rectal cancer. Lancet 1(8496):1479–1482
Martling A, Holm T, Johansson H, Rutqvist LE, Cedermark B (2001) The Stockholm II trial on preoperative radiotherapy in rectal carcinoma: long-term follow-up of a population-based study. Cancer 92(4):896–902
Rahbari NN, Ulrich AB, Bruckner T, Munter M, Nickles A, Contin P, Loffler T, Reissfelder C, Koch M, Buchler MW, Weitz J (2011) Surgery for locally recurrent rectal cancer in the era of total mesorectal excision: is there still a chance for cure? Ann Surg 253(3):522–533. https://doi.org/10.1097/SLA.0b013e3182096d4f
Rahbari NN, Aigner M, Thorlund K, Mollberg N, Motschall E, Jensen K, Diener MK, Buchler MW, Koch M, Weitz J (2010) Meta-analysis shows that detection of circulating tumor cells indicates poor prognosis in patients with colorectal cancer. Gastroenterology
Weitz J, Koch M, Debus J, Hohler T, Galle PR, Buchler MW (2005) Colorectal cancer. Lancet 365(9454):153–165
Freedman LS, Macaskill P, Smith AN (1984) Multivariate analysis of prognostic factors for operable rectal cancer. Lancet 2(8405):733–736
Park JK, Kim YW, Hur H, Kim NK, Min BS, Sohn SK, Choi YD, Kim YT, Ahn JB, Roh JK, Keum KC, Seong JS (2009) Prognostic factors affecting oncologic outcomes in patients with locally recurrent rectal cancer: impact of patterns of pelvic recurrence on curative resection. Langenbecks ArchSurg 394(1):71–77
Staib L, Link KH, Blatz A, Beger HG (2002) Surgery of colorectal cancer: surgical morbidity and five- and ten-year results in 2400 patients—monoinstitutional experience. World J Surg 26(1):59–66
Sobin LH, Wittekind C (2002) UICC: TNM classification of malignant tumours, vol 6th. Wiley, London
Sobin LH, Gospodarowicz MK, Wittekind C (2009) UICC: TNM classification of malignant tumours, vol 7th. Wiley, New York
Berger AC, Sigurdson ER, LeVoyer T, Hanlon A, Mayer RJ, Macdonald JS, Catalano PJ, Haller DG (2005) Colon cancer survival is associated with decreasing ratio of metastatic to examined lymph nodes. J Clin Oncol 23(34):8706–8712
De Ridder M, Vinh-Hung V, Van NY, Hoorens A, Sermeus A, Storme G (2006) Prognostic value of the lymph node ratio in node positive colon cancer. Gut 55(11):1681
Rosenberg R, Friederichs J, Schuster T, Gertler R, Maak M, Becker K, Grebner A, Ulm K, Hofler H, Nekarda H, Siewert JR (2008) Prognosis of patients with colorectal cancer is associated with lymph node ratio: a single-center analysis of 3,026 patients over a 25-year time period. Ann Surg 248(6):968–978
Peschaud F, Benoist S, Julie C, Beauchet A, Penna C, Rougier P, Nordlinger B (2008) The ratio of metastatic to examined lymph nodes is a powerful independent prognostic factor in rectal cancer. Ann Surg 248(6):1067–1073
Holm T, Ljung A, Haggmark T, Jurell G, Lagergren J (2007) Extended abdominoperineal resection with gluteus maximus flap reconstruction of the pelvic floor for rectal cancer. Br J Surg 94(2):232–238
Rosenberg R, Engel J, Bruns C, Heitland W, Hermes N, Jauch KW, Kopp R, Putterich E, Ruppert R, Schuster T, Friess H, Holzel D (2010) The prognostic value of lymph node ratio in a population-based collective of colorectal cancer patients. Ann Surg 251(6):1070–1078
O'Connell JB, Maggard MA, Ko CY (2004) Colon cancer survival rates with the new American Joint Committee on Cancer sixth edition staging. J Natl Cancer Inst 96(19):1420–1425
Van Cutsem E, Oliveira J (2009) Primary colon cancer: ESMO clinical recommendations for diagnosis, adjuvant treatment and follow-up. AnnOncol 20 Suppl 4:49–50
Schmiegel W, Reinacher-Schick A, Arnold D, Graeven U, Heinemann V, Porschen R, Riemann J, Rodel C, Sauer R, Wieser M, Schmitt W, Schmoll HJ, Seufferlein T, Kopp I, Pox C (2008) Update S3-guideline “colorectal cancer” 2008. Z Gastroenterol 46(8):799–840
Merkel S, Mansmann U, Papadopoulos T, Wittekind C, Hohenberger W, Hermanek P (2001) The prognostic inhomogeneity of colorectal carcinomas stage III: a proposal for subdivision of stage III. Cancer 92(11):2754–2759
Greene FL, Stewart AK, Norton HJ (2002) A new TNM staging strategy for node-positive (stage III) colon cancer: an analysis of 50,042 patients. Ann Surg 236(4):416–421
Greene FL, Stewart AK, Norton HJ (2004) New tumor-node-metastasis staging strategy for node-positive (stage III) rectal cancer: an analysis. J Clin Oncol 22(10):1778–1784
Nelson H, Petrelli N, Carlin A, Couture J, Fleshman J, Guillem J, Miedema B, Ota D, Sargent D (2001) Guidelines 2000 for colon and rectal cancer surgery. J Natl Cancer Inst 93(8):583–596
Chang GJ, Rodriguez-Bigas MA, Skibber JM, Moyer VA (2007) Lymph node evaluation and survival after curative resection of colon cancer: systematic review. J Natl Cancer Inst 99(6):433–441
Hashiguchi Y, Hase K, Ueno H, Mochizuki H, Kajiwara Y, Ichikura T, Yamamoto J (2010) Prognostic significance of the number of lymph nodes examined in colon cancer surgery: clinical application beyond simple measurement. Ann Surg 251(5):872–881
Tepper JE, O'Connell MJ, Niedzwiecki D, Hollis D, Compton C, Benson AB III, Cummings B, Gunderson L, Macdonald JS, Mayer RJ (2001) Impact of number of nodes retrieved on outcome in patients with rectal cancer. J Clin Oncol 19(1):157–163
Kim YW, Kim NK, Min BS, Lee KY, Sohn SK, Cho CH (2009) The influence of the number of retrieved lymph nodes on staging and survival in patients with stage II and III rectal cancer undergoing tumor-specific mesorectal excision. Ann Surg 249(6):965–972
Abdel-Misih SR, Wei L, Benson AB 3rd, Cohen S, Lai L, Skibber J, Wilkinson N, Weiser M, Schrag D, Bekaii-Saab T (2016) Neoadjuvant therapy for rectal cancer affects lymph node yield and status without clear implications on outcome: the case for eliminating a metric and using preoperative staging to guide therapy. J Natl Compr Cancer Netw: JNCCN 14(12):1528–1534
Moug SJ, Saldanha JD, McGregor JR, Balsitis M, Diament RH (2009) Positive lymph node retrieval ratio optimises patient staging in colorectal cancer. Br J Cancer 100(10):1530–1533
Dekker JW, Peeters KC, Putter H, Vahrmeijer AL, van de Velde CJ (2010) Metastatic lymph node ratio in stage III rectal cancer; prognostic significance in addition to the 7th edition of the TNM classification. Eur J Surg Oncol
Thorn CC, Woodcock NP, Scott N, Verbeke C, Scott SB, Ambrose NS (2004) What factors affect lymph node yield in surgery for rectal cancer? Color Dis 6(5):356–361
Mekenkamp LJ, van Krieken JH, Marijnen CA, van de Velde CJ, Nagtegaal ID (2009) Lymph node retrieval in rectal cancer is dependent on many factors—the role of the tumor, the patient, the surgeon, the radiotherapist, and the pathologist. Am J Surg Pathol 33(10):1547–1553
Morcos B, Baker B, Al MM, Haddad H, Hashem S (2010) Lymph node yield in rectal cancer surgery: effect of preoperative chemoradiotherapy. Eur J Surg Oncol 36(4):345–349
Ha YH, Jeong SY, Lim SB, Choi HS, Hong YS, Chang HJ, Kim DY, Jung KH, Park JG (2010) Influence of preoperative chemoradiotherapy on the number of lymph nodes retrieved in rectal cancer. Ann Surg 252(2):336–340
Marijnen CA, Nagtegaal ID, Klein KE, Hermans J, van de Velde CJ, Leer JW, van Krieken JH (2001) No downstaging after short-term preoperative radiotherapy in rectal cancer patients. J Clin Oncol 19(7):1976–1984
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All procedures were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Fritzmann, J., Contin, P., Reissfelder, C. et al. Comparison of three classifications for lymph node evaluation in patients undergoing total mesorectal excision for rectal cancer. Langenbecks Arch Surg 403, 451–462 (2018). https://doi.org/10.1007/s00423-018-1662-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-018-1662-5