Abstract
Purpose
To contrast older and younger adults’ prefrontal cortex (PFC) neural activity (through changes in oxygenated hemoglobin) during single and dual tasks, and to compare decrements in task performance.
Methods
Changes in oxygenated hemoglobin of dorsolateral PFC were monitored using functional near-infrared spectroscopy during single tasks of spelling backwards (cognitive task) and 30 m preferred paced walk; and a dual task combining both. Gait velocity was measured by a pressure sensitive mat.
Results
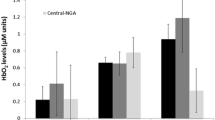
Twenty sex-matched younger (27.6 ± 3.5 years) and 17 older adults (71.2 ± 4.9 years) were recruited. The left PFC oxygenated hemoglobin decreased from start (1st quintile) to the end (5th quintile) of the walking task in younger adults ( – 0.03 ± 0.03 to – 0.72 ± 0.20 µM; p < .05) unlike the non-significant change in older adults (0.03 ± 0.06 to – 0.41 ± 0.32 µM, p > .05). Overall, oxygenation increased bilaterally during dual versus single walk task in older adults (Left PFC: 0.22 ± 0.16 vs. – 0.23 ± 0.21 µM, respectively; Right PFC: 0.17 ± 0.18 vs. – 0.33 ± 0.22 µM, respectively), but only in right PFC in younger adults ( – 0.02 ± 0.15 vs. – 0.47 ± 0.13 µM). Older adults exhibited lower velocity during the dual task compared to younger adults (1.03 ± 0.16 vs. 1.20 ± 0.17 m/s, respectively). Older age was associated with dual task cost on velocity during walking after adjusting for confounding variables.
Conclusions
Age-related cognitive decline in older adults may increase neural activity for cognitive tasks and diminish walking automaticity that may lead to decrements during dual tasking; the greater PFC increases in the oxygenated hemoglobin and lower velocity may be due to increased cognitive load and limited attentional resources.



Similar content being viewed by others
Availability of data and material
The datasets of the current study are available from the corresponding author on reasonable request.
Code availability
Not applicable.
Abbreviations
- ∆O2Hb:
-
Changes in oxygenated hemoglobin
- BMI:
-
Body mass index
- fNIRS:
-
Functional near-infrared spectroscopy
- PFC:
-
Prefrontal cortex
- PPW:
-
Preferred paced walk
- Q1:
-
First quintile
- Q5:
-
Fifth quintile
- SB:
-
Spelling backwards
References
Al-Yahya E, Dawes H, Smith L, Dennis A, Howells K, Cockburn J (2011) Cognitive motor interference while walking: a systematic review and meta-analysis. Neurosci Biobehav Rev 35:715–728. https://doi.org/10.1016/j.neubiorev.2010.08.008
Artinis medical systems (2000) The theory of Near Infrared Spectroscopy. Artinis Medical Systems | fNIRS and NIRS devices. Available at: https://www.artinis.com/theory-of-nirs [Accessed June 7, 2021]
Ayaz H (2010) Functional near infrared spectroscopy based brain computer interface
Berger L, Bernard-Demanze L (2011) Age-related effects of a memorizing spatial task in the adults and elderly postural control. Gait Posture 33:300–302. https://doi.org/10.1016/j.gaitpost.2010.10.082
Beurskens R, Helmich I, Rein R, Bock O (2014) Age-related changes in prefrontal activity during walking in dual-task situations: a fNIRS study. Int J Psychophysiol 92:122–128. https://doi.org/10.1016/j.ijpsycho.2014.03.005
Bonetti LV, Hassan SA, Kasawara KT, Reid WD (2019) The effect of mental tracking task on spatiotemporal gait parameters in healthy younger and middle- and older aged participants during dual tasking. Exp Brain Res 237:3123–3132. https://doi.org/10.1007/s00221-019-05659-z
Bu Z, Huang A, Xue M, Li Q, Bai Y, Xu G (2021) Cognitive frailty as a predictor of adverse outcomes among older adults: A systematic review and meta-analysis. Brain and Behavior 11:e01926. https://doi.org/10.1002/brb3.1926
Cabeza R, Nyberg L (2000) Imaging cognition II: An empirical review of 275 PET and fMRI studies. J Cogn Neurosci 12:1–47
Cabeza R, Anderson ND, Locantore JK, McIntosh AR (2002) Aging gracefully: compensatory brain activity in high-performing older adults. Neuroimage 17:1394–1402. https://doi.org/10.1006/nimg.2002.1280
Cabeza R, Albert M, Belleville S, Craik FIM, Duarte A, Grady CL et al (2018) Maintenance, reserve and compensation: the cognitive neuroscience of healthy ageing. Nat Rev Neurosci 19:701–710. https://doi.org/10.1038/s41583-018-0068-2
Chen M, Pillemer S, England S, Izzetoglu M, Mahoney JR, Holtzer R (2017) Neural correlates of obstacle negotiation in older adults: An fNIRS study. Gait Posture 58:130–135. https://doi.org/10.1016/j.gaitpost.2017.07.043
Clark DJ (2015) Automaticity of walking: functional significance, mechanisms, measurement and rehabilitation strategies. Front Hum Neurosci. https://doi.org/10.3389/fnhum.2015.00246
Corp DT, Youssef GJ, Clark RA, Gomes-Osman J, Yücel MA, Oldham SJ et al (2018) Reduced motor cortex inhibition and a ‘cognitive-first’ prioritisation strategy for older adults during dual-tasking. Exp Gerontol 113:95–105. https://doi.org/10.1016/j.exger.2018.09.018
Dale W, Kotwal AA, Shega JW, Schumm LP, Kern DW, Pinto J et al (2018) Cognitive function and its risk factors among older US adults living at home. Alzheimer Dis Assoc Disord 32:207–213. https://doi.org/10.1097/WAD.0000000000000241
Deyo RA, Cherkin DC, Ciol MA (1992) Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol 45:613–619
Fraser SA, Dupuy O, Pouliot P, Lesage F, Bherer L (2016) Comparable cerebral oxygenation patterns in younger and older adults during dual-task walking with increasing load. Front Aging Neurosci. https://doi.org/10.3389/fnagi.2016.00240
Friden T, Zätterström R, Lindstrand A, Moritz U (1989) A stabilometric technique for evaluation of lower limb instabilities. Am J Sports Med 17:118–122. https://doi.org/10.1177/036354658901700120
Guimaraes RM, Isaacs B (1980) Characteristics of the gait in old people who fall. Int Rehabil Med 2:177–180. https://doi.org/10.3109/09638288009163984
Harada T, Miyai I, Suzuki M, Kubota K (2009) Gait capacity affects cortical activation patterns related to speed control in the elderly. Exp Brain Res 193:445–454. https://doi.org/10.1007/s00221-008-1643-y
Hawkins KA, Fox EJ, Daly JJ, Rose DK, Christou EA, McGuirk TE et al (2018) Prefrontal over-activation during walking in people with mobility deficits: Interpretation and functional implications. Hum Mov Sci 59:46–55. https://doi.org/10.1016/j.humov.2018.03.010
Herman T, Mirelman A, Giladi N, Schweiger A, Hausdorff JM (2010) Executive control deficits as a prodrome to falls in healthy older adults: a prospective study linking thinking, walking, and falling. J Gerontol A Biol Sci Med Sci 65:1086–1092. https://doi.org/10.1093/gerona/glq077
Hermand E, Compagnat M, Dupuy O, Salle J-Y, Daviet J-C, Perrochon A (2020) Functional status is associated with prefrontal cortex activation in gait in subacute stroke patients: a functional near-infrared spectroscopy study. Front Neurol 11:1298. https://doi.org/10.3389/fneur.2020.559227
Hollman JH, Childs KB, McNeil ML, Mueller AC, Quilter CM, Youdas JW (2010) Number of strides required for reliable measurements of pace, rhythm and variability parameters of gait during normal and dual task walking in older individuals. Gait Posture 32:23–28. https://doi.org/10.1016/j.gaitpost.2010.02.017
Holtzer R, Mahoney JR, Izzetoglu M, Izzetoglu K, Onaral B, Verghese J (2011) fNIRS study of walking and walking while talking in young and old individuals. J Gerontol A Biol Sci Med Sci 66:879–887. https://doi.org/10.1093/gerona/glr068
Holtzer R, Epstein N, Mahoney JR, Izzetoglu M, Blumen HM (2014) Neuroimaging of mobility in aging: a targeted review. J Gerontol Series A 69:1375–1388. https://doi.org/10.1093/gerona/glu052
Holtzer R, Mahoney JR, Izzetoglu M, Wang C, England S, Verghese J (2015) Online fronto-cortical control of simple and attention-demanding locomotion in humans. Neuroimage 112:152–159. https://doi.org/10.1016/j.neuroimage.2015.03.002
Li Z, Moore AB, Tyner C, Hu X (2009) Asymmetric Connectivity Reduction and its Relationship to “HAROLD” in Aging Brain. Brain Res 1295:149–158. https://doi.org/10.1016/j.brainres.2009.08.004
Li KZH, Bherer L, Mirelman A, Maidan I, Hausdorff JM (2018) Cognitive involvement in balance, gait and dual-tasking in aging: a focused review from a neuroscience of aging perspective. Front Neurol 9:913. https://doi.org/10.3389/fneur.2018.00913
Lindenberger U, Marsiske M, Baltes PB (2000) Memorizing while walking: increase in dual-task costs from young adulthood to old age. Psychol Aging 15:417–436
MacDonald AW, Cohen JD, Stenger VA, Carter CS (2000) Dissociating the role of the dorsolateral prefrontal and anterior cingulate cortex in cognitive control. Science 288:1835–1838
Maidan I, Nieuwhof F, Bernad-Elazari H, Reelick MF, Bloem BR, Giladi N et al (2016) The role of the frontal lobe in complex walking among patients with Parkinson’s disease and healthy older adults: an fNIRS study. Neurorehabil Neural Repair 30:963–971. https://doi.org/10.1177/1545968316650426
Manor B, Zhou J, Jor’dan A, Zhang J, Fang J, Pascual-Leone A (2016) Reduction of dual-task costs by noninvasive modulation of prefrontal activity in healthy elders. J Cognit Neurosci 28:275–281. https://doi.org/10.1162/jocn_a_00897
McKendrick R, Mehta R, Ayaz H, Scheldrup M, Parasuraman R (2017) Prefrontal hemodynamics of physical activity and environmental complexity during cognitive work. Hum Factors 59:147–162. https://doi.org/10.1177/0018720816675053
Mirelman A, Maidan I, Bernad-Elazari H, Shustack S, Giladi N, Hausdorff JM (2017) Effects of aging on prefrontal brain activation during challenging walking conditions. Brain Cogn 115:41–46. https://doi.org/10.1016/j.bandc.2017.04.002
Nasreddine ZS, Phillips NA, Bédirian V, Charbonneau S, Whitehead V, Collin I et al (2005) The montreal cognitive assessment, MoCA: a brief screening tool for mild cognitive impairment. J Am Geriatr Soc 53:695–699. https://doi.org/10.1111/j.1532-5415.2005.53221.x
Nóbrega-Sousa P, Gobbi LTB, Orcioli-Silva D, da Conceição NR, Beretta VS, Vitório R (2020) Prefrontal cortex activity during walking: effects of aging and associations with gait and executive function. Neurorehabil Neural Repair 34:915–924. https://doi.org/10.1177/1545968320953824
Papegaaij S, Hortobágyi T, Godde B, Kaan WA, Erhard P, Voelcker-Rehage C (2017) Neural correlates of motor-cognitive dual-tasking in young and old adults. PLoS ONE 12:e0189025. https://doi.org/10.1371/journal.pone.0189025
Pashler H, Johnston JC (1998) “Attentional limitations in dual-task performance,” in Attention (Hove, England: Psychology Press/Erlbaum (UK) Taylor & Francis), 155–189
Patel P, Lamar M, Bhatt T (2014) Effect of type of cognitive task and walking speed on cognitive-motor interference during dual-task walking. Neuroscience 260:140–148. https://doi.org/10.1016/j.neuroscience.2013.12.016
Pelicioni PHS, Tijsma M, Lord SR, Menant J (2019) Prefrontal cortical activation measured by fNIRS during walking: effects of age, disease and secondary task. PeerJ 7:e6833. https://doi.org/10.7717/peerj.6833
Petrides M (1995) Functional organization of the human frontal cortex for mnemonic processing. Evidence from neuroimaging studies. Ann N Y Acad Sci 769:85–96
Piper SK, Krueger A, Koch SP, Mehnert J, Habermehl C, Steinbrink J et al (2014) A wearable multi-channel fNIRS system for brain imaging in freely moving subjects. Neuroimage. https://doi.org/10.1016/j.neuroimage.2013.06.062
Pochon JB, Levy R, Poline JB, Crozier S, Lehéricy S, Pillon B et al (2001) The role of dorsolateral prefrontal cortex in the preparation of forthcoming actions: an fMRI study. Cereb Cortex 11:260–266
Ross D, Wagshul ME, Izzetoglu M, Holtzer R (2021) Prefrontal cortex activation during dual-task walking in older adults is moderated by thickness of several cortical regions. GeroScience 43:1959–1974. https://doi.org/10.1007/s11357-021-00379-1
Salzman T, Tobón Vallejo D, Polskaia N, Michaud L, St-Amant G, Lajoie Y et al (2021) Hemodynamic and behavioral changes in older adults during cognitively demanding dual tasks. Brain Behavior 11:e02021. https://doi.org/10.1002/brb3.2021
Silsupadol P, Lugade V, Shumway-Cook A, van Donkelaar P, Chou L-S, Mayr U et al (2009) Training-related changes in dual-task walking performance of elderly persons with balance impairment: a double-blind, randomized controlled trial. Gait Posture 29:634–639. https://doi.org/10.1016/j.gaitpost.2009.01.006
Smith E, Cusack T, Blake C (2016) The effect of a dual task on gait speed in community dwelling older adults: A systematic review and meta-analysis. Gait Posture 44:250–258. https://doi.org/10.1016/j.gaitpost.2015.12.017
St-Amant G, Rahman T, Polskaia N, Fraser S, Lajoie Y (2020) Unveilling the cerebral and sensory contributions to automatic postural control during dual-task standing. Hum Mov Sci 70:102587. https://doi.org/10.1016/j.humov.2020.102587
Stuart S, Belluscio V, Quinn JF, Mancini M (2019) Pre-frontal cortical activity during walking and turning is reliable and differentiates across young, older adults and people with Parkinson’s disease. Front Neurol 10:536. https://doi.org/10.3389/fneur.2019.00536
Techayusukcharoen R, Iida S, Aoki C (2019) Observing brain function via functional near-infrared spectroscopy during cognitive program training (dual task) in young people. J Phys Ther Sci 31:550–555. https://doi.org/10.1589/jpts.31.550
Thompson WR, Gordon NF, Pescatello Li, S. (eds) (2010) American College of Sports Medicine. ACSM’s guidelines for exercise testing and prescription, 8th edn. Lippincott Williams & Wilkins/Wolter Kluwer, Philadelphia
Tombu M, Jolicoeur P (2003) A central capacity sharing model of dual-task performance. J Exp Psychol Hum Percept Perform 29:3–18. https://doi.org/10.1037//0096-1523.29.1.3
Vandenbossche J, Deroost N, Soetens E, Coomans D, Spildooren J, Vercruysse S et al (2013) Freezing of gait in Parkinson’s disease: disturbances in automaticity and control. Front Hum Neurosci 6:356. https://doi.org/10.3389/fnhum.2012.00356
Wechsler D (1997) WAIS-III: Administration and scoring manual: Wechsler adult intelligence scale--third edition. 3rd edition. Psychological Corporation
WHO (2020) Obesity and overweight. Available at: https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight [Accessed March 1, 2021]
Yogev-Seligmann G, Hausdorff JM, Giladi N (2012) Do we always prioritize balance when walking? Towards an integrated model of task prioritization. Mov Disord 27:765–770. https://doi.org/10.1002/mds.24963
Acknowledgements
The authors would like to acknowledge Dr. Masatoshi Hanada for his assistance with data collection and Dr. Hasan Ayaz for his technical support with fNIRS data.
Funding
This work was funded by the Research and Innovation Ontario, Grant number 501683, Canada Foundation for Innovation, Grant number 501682, Ontario Respiratory Care Society, Grant number 503659, the Department of Physical Therapy 208294 and Rehabilitation Sciences Institute 100771 at the University of Toronto. The sponsors had no role in the design and conduct of the study; in the collection, analysis, and interpretation of data; in the preparation of the manuscript; or in the review or approval of the manuscript.
Author information
Authors and Affiliations
Contributions
Conceptualization: WDR and LVB; methodology: WDR, LVB and DR; software, SAH; validation: all authors; formal analysis: SAH. WDR, DR; investigation: SAH, LVB and KTK; resources: WDR; data curation: SAH, KTK and WDR; writing—original draft preparation: SAH; writing—review and editing: all authors; visualization: SAH and WDR; supervision: WDR; project administration: all authors; funding acquisition: WDR. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Ethics approval
The study protocol was approved by the Research Ethics Board of University of Toronto (protocol ID: 33,466).
Consent to participate
All participants provided written informed consent before participation.
Consent for publication
All participants consented to having their data published and/or used in presentations.
Additional information
Communicated by Lori Ann Vallis.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hassan, S.A., Bonetti, L.V., Kasawara, K.T. et al. Decreased automaticity contributes to dual task decrements in older compared to younger adults. Eur J Appl Physiol 122, 965–974 (2022). https://doi.org/10.1007/s00421-022-04891-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-022-04891-w