Abstract
Purpose
Orthostatic hypotension, leading to cerebral hypoperfusion, can result in postural instability and falls in older adults. We determined the efficacy of a novel, intermittent pneumatic compression system, applying pressure around the lower legs, as a countermeasure against orthostatic stress in older adults.
Methods
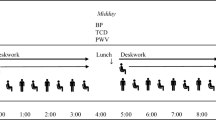
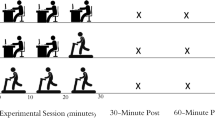
Data were collected from 13 adults (4 male) over 65 years of age. Non-invasive ultrasound measured middle cerebral artery blood velocity (MCAv) and finger photoplethysmography measured mean arterial blood pressure (MAP). Intermittent lower leg compression was applied in a peristaltic manner in the local diastolic phase of each cardiac cycle to optimize venous return during 1-min of seated rest and during a sit-to-stand transition to 1-min of quiet standing with compression initiated 15 s before transition.
Results
During seated rest, compression resulted in a 4.5 ± 6.5 mmHg increase in MAP, and 2.3 ± 2.1 cm/s increase in MCAv (p < 0.05). MAP and MCAv increased during the 15 s of applied compression before the posture transition (2.3 ± 7.2 mmHg and 2.1 ± 4.0 cm/s, respectively, p < 0.05) with main effects for both variables confirming continued benefit during the transition and quiet stand periods.
Conclusions
Application of carefully timed, intermittent compression to the lower legs of older adults increased MAP and MCAv during seated rest and maintained an elevated MAP and MCAv during a transition to standing posture. Future research could assess the benefits of this technology for persons at risk for orthostatic hypotension on standing and while walking in an effort to reduce injurious, unexplained falls in older adults.

Similar content being viewed by others
Abbreviations
- CO2 :
-
Carbon dioxide
- CVRi:
-
Cerebrovascular resistance index
- ECG:
-
Electrocardiogram
- HR:
-
Heart rate
- HHb:
-
Deoxygenated hemoglobin concentration
- MAP:
-
Mean arterial pressure
- MCAv:
-
Middle cerebral artery blood velocity
- O2Hb:
-
Oxygenated hemoglobin concentration
- PETCO2 :
-
Partial pressure of end tidal carbon dioxide
- \(\dot{Q}\) :
-
Cardiac output
- SD:
-
Standard deviation
- SFA:
-
Superficial femoral artery
- SV:
-
Stroke volume
- TCD:
-
Transcranial Doppler
- tHb:
-
Total hemoglobin concentration
- TSI:
-
Tissue saturation index
References
Aaslid R, Lindegaard KF, Sorteberg W, Nornes H (1989) Cerebral autoregulation dynamics in humans. Stroke 20(1):45–52. https://doi.org/10.1161/01.STR.20.1.45
Bates D, Mächler M, Bolker B, Walker S (2015) Fitting linear mixed-effects models using lme4. J Stat Softw 67(1):1–48. https://doi.org/10.18637/jss.v067.i01
Bhangu J, Hall P, Devaney N, Bennett K, Carroll L, Kenny RA, McMahon CG (2019) The prevalence of unexplained falls and syncope in older adults presenting to an Irish urban emergency department. Eur J Emerg Med 26(2):100–104. https://doi.org/10.1097/MEJ.0000000000000548
Bickel A, Shturman A, Grevtzev I, Roguin N, Eitan A (2011) The physiological impact of intermittent sequential pneumatic compression (ISPC) leg sleeves on cardiac activity. Am J Surg 202(1):16–22. https://doi.org/10.1016/j.amjsurg.2010.04.020
Brignole M, Moya A, De Lange FJ, Deharo JC, Elliott PM, Fanciulli A, Fedorowski A, Furlan R, Kenny RA, Martín A, Probst V, Reed MJ, Rice CP, Sutton R, Ungar A, Van Dijk JG (2018) 2018 ESC Guidelines for the diagnosis and management of syncope. Eur Heart J 39(21):1883–1948. https://doi.org/10.1093/eurheartj/ehy037
Bronzwaer ASGT, Verbree J, Stok WJ, Daemen MJAP, van Buchem MA, van Osch MJP, van Lieshout JJ (2017) Aging modifies the effect of cardiac output on middle cerebral artery blood flow velocity. Physiol Rep 5(17):1–10. https://doi.org/10.14814/phy2.13361
Collaboration from accreditation Canada/the Canadian institute for health information/the Canadian patient safety institute (2014) Preventing falls: from evidence to improvement in Canadianhealth care. https://www.patientsafetyinstitute.ca/en/toolsResources/pages/preventing-falls---from-evidence-to-improvement.aspx
Coverdale NS, Gati JS, Opalevych O, Perrotta A, Shoemaker JK (2014) Cerebral blood flow velocity underestimates cerebral blood flow during modest hypercapnia and hypocapnia. J Appl Physiol 117(10):1090–1096. https://doi.org/10.1152/japplphysiol.00285.2014
Delis KT, Knaggs AL (2005) Duration and amplitude decay of acute arterial leg inflow enhancement with intermittent pneumatic leg compression: an insight into the implicated physiologic mechanisms. J Vasc Surg 42(4):717–725. https://doi.org/10.1016/j.jvs.2005.06.004
Delis KT, Azizi ZA, Stevens RJG, Wolfe JHN, Nicolaides AN (2000) Optimum intermittent pneumatic compression stimulus for lower-limb venous emptying. Eur J Vasc Endovasc Surg 19(3):261–269. https://doi.org/10.1053/ejvs.1999.1047
Dixit NK, Vazquez LD, Cross NJ, Kuhl EA, Serber ER, Kovacs A, Dede DE, Conti JB, Sears SF (2010) Cardiac resynchronization therapy: a pilot study examining cognitive change in patients before and after treatment. Clin Cardiol 33(2):84–88. https://doi.org/10.1002/clc.20710
Fanelli G, Zasa M, Baciarello M, Mazzani R, Di Cianni S, Rossi M, Casati A (2008) Systemic hemodynamic effects of sequential pneumatic compression of the lower limbs: a prospective study in healthy volunteers. J Clin Anesth 20(5):338–342. https://doi.org/10.1016/j.jclinane.2008.02.005
Finucane C, O’Connell MDL, Fan CW, Savva GM, Soraghan CJ, Nolan H, Cronin H, Kenny RA (2014) Age-related normative changes in phasic orthostatic blood pressure in a large population study: findings from the Irish longitudinal study on ageing (TILDA). Circulation 130(20):1780–1789. https://doi.org/10.1161/CIRCULATIONAHA.114.009831
Finucane C, O’Connell MDL, Donoghue O, Richardson K, Savva GM, Kenny RA (2017) Impaired orthostatic blood pressure recovery is associated with unexplained and injurious falls. J Am Geriatr Soc 65(3):474–482. https://doi.org/10.1111/jgs.14563
Florence CS, Bergen G, Atherly A, Burns E, Stevens J, Drake C (2018) Medical costs of fatal and nonfatal falls in older adults. J Am Geriatr Soc 66(4):693–698. https://doi.org/10.1111/jgs.15304
Freeman R, Wieling W, Axelrod FB, Benditt DG, Benarroch E, Biaggioni I, Cheshire WP, Chelimsky T, Cortelli P, Gibbons CH, Goldstein DS, Hainsworth R, Hilz MJ, Jacob G, Kaufmann H, Jordan J, Lipsitz LA, Levine BD, Low PA et al (2011) Consensus statement on the definition of orthostatic hypotension, neurally mediated syncope and the postural tachycardia syndrome. Clin Auton Res 21(2):69–72. https://doi.org/10.1007/s10286-011-0119-5
Gibbons TD, Zuj KA, Prince CN, Kingston DC, Peterson SD, Hughson RL (2019) Haemodynamic and cerebrovascular effects of intermittent lower-leg compression as countermeasure to orthostatic stress. Exp Physiol 104(12):1790–1800. https://doi.org/10.1113/EP088077
Heyer EJ, Mergeche JL, Connolly ES (2014) Middle cerebral artery pulsatility index and cognitive improvement after carotid endarterectomy for symptomatic stenosis: clinical article. J Neurosurg 120(1):126–131. https://doi.org/10.3171/2013.8.JNS13931
Juraschek SP, Daya N, Appel LJ, Miller ER, Windham BG, Pompeii L, Griswold ME, Kucharska-Newton A, Selvin E (2017) Orthostatic hypotension in middle-age and risk of falls. Am J Hypertens 30(2):188–195. https://doi.org/10.1093/ajh/hpw108
Kakkos SK, Griffin M, Geroulakos G, Nicolaides AN (2005) The efficacy of a new portable sequential compression device (SCD express) in preventing venous stasis. J Vasc Surg 42(2):296–303. https://doi.org/10.1016/j.jvs.2005.03.031
Kurukahvecioglu O, Sare M, Karamercan A, Gunaydin B, Anadol Z, Tezel E (2008) Intermittent pneumatic sequential compression of the lower extremities restores the cerebral oxygen saturation during laparoscopic cholecystectomy. Surg Endosc Other Interv Tech 22(4):907–911. https://doi.org/10.1007/s00464-007-9505-4
Kwak HJ, Lee D, Lee YW, Yu GY, Shinn HK, Kim JY (2011) The intermittent sequential compression device on the lower extremities attenuates the decrease in regional cerebral oxygen saturation during sitting position under sevoflurane anesthesia. J Neurosurg Anesthesiol 23(1):1–5. https://doi.org/10.1097/ANA.0b013e3181e97a5e
Labropoulos N, Watson WC, Mansour MA, Kang SS, Littooy FN, Baker WH (1998) Acute effects of intermittent pneumatic compression on popliteal artery blood flow. Arch Surg 133(10):1072–1075. https://doi.org/10.1001/archsurg.133.10.1072
Lenth RV (2016) Least-squares means: the R package lsmeans. J Stat Softw 69(1):1–33. https://doi.org/10.18637/jss.v069.i01
Malone MD, Cisek PL, Comerota AJ, Holland B, Eid IG, Comerota AJ (1999) High-pressure, rapid-inflation pneumatic compression improves venous hemodynamics in healthy volunteers and patients who are post-thrombotic. J Vasc Surg 29(4):593–599. https://doi.org/10.1016/S0741-5214(99)70303-4
McNicholas T, Tobin K, Carey D, O’Callaghan S, Kenny RA (2018) Is baseline orthostatic hypotension associated with a decline in global cognitive performance at 4‐year follow‐up? Data from TILDA (The Irish Longitudinal Study on Ageing). J Am Heart Assoc. https://doi.org/10.1161/jaha.118.008976
Meng L, Hou W, Chui J, Han R, Gelb AW (2015) Cardiac output and cerebral blood flow. Anesthesiology 123(5):1198–1208. https://doi.org/10.1097/aln.0000000000000872
Ogoh S (2017) Relationship between cognitive function and regulation of cerebral blood flow. J Physiol Sci 67(3):345–351. https://doi.org/10.1007/s12576-017-0525-0
Ogoh S, Brothers M, Barnes Q, Eubank WL, Hawkins MN, Purkayastha S, O-Yurvati A, Raven PB (2005) The effect of changes in cardiac output on middle cerebral artery mean blood velocity at rest and during exercise. J Physiol 569(2):697–704. https://doi.org/10.1113/jphysiol.2005.095836
Ogoh S, Brothers RM, Eubank WL, Raven PB (2008) Autonomic neural control of the cerebral vasculature: acute hypotension. Stroke 39(7):1979–1987. https://doi.org/10.1161/STROKEAHA.107.510008
Quinn C, Deegan B, Cooke J, Carew S, Hannigan A, Dunne C, Lyons D (2015) Therapeutic use of compression stockings for orthostatic hypotension: an assessment of patient and physician perspectives and practices. Age Ageing 44(2):339–342. https://doi.org/10.1093/ageing/afu162
Roman DD, Kubo SH, Ormaza S, Francis GS, Bank AJ, Shumway SJ (1997) Memory improvement following cardiac transplantation. J Clin Exp Neuropsychol 19(5):692–697. https://doi.org/10.1080/01688639708403754
Romero-Ortuno R, Cogan L, Foran T, Kenny RA, Fan CW (2011) Continuous noninvasive orthostatic blood pressure measurements and their relationship with orthostatic intolerance, falls, and frailty in older people. J Am Geriatr Soc 59(4):655–665. https://doi.org/10.1111/j.1532-5415.2011.03352.x
Shaw BH, Loughin TM, Robinovitch SN, Claydon VE (2015) Cardiovascular responses to orthostasis and their association with falls in older adults. BMC Geriatr 15(1):1–8. https://doi.org/10.1186/s12877-015-0168-z
Smeenk HE, Koster MJ, Faaij RA, de Geer DB, Hamaker ME (2014) Compression therapy in patients with orthostatic hypotension: a systematic review. Neth J Med 72(2):80–85. https://doi.org/10.1007/s00134-003-2075-6
Sorond FA, Khavari R, Serrador JM, Lipsitz LA (2005) Regional cerebral autoregulation during orthostatic stress: age-related differences. J Gerontol Ser A Biol Sci Med Sci 60(11):1484–1487. https://doi.org/10.1093/gerona/60.11.1484
Tochikubo O, Ri S, Kura N (2006) Effects of pulse-synchronized massage with air cuffs on peripheral blood flow and autonomic nervous system. Circ J 70(9):1159–1163. https://doi.org/10.1253/circj.70.1159
Verbree J, Bronzwaer ASGT, Ghariq E, Versluis MJ, Daemen MJAP, Van Buchem MA, Dahan A, Van Lieshout JJ, Van Osch MJP (2014) Assessment of middle cerebral artery diameter during hypocapnia and hypercapnia in humans using ultra-high-field MRI. J Appl Physiol 117(10):1084–1089. https://doi.org/10.1152/japplphysiol.00651.2014
Wieling W, Krediet CTP, Van Dijk N, Linzer M, Tschakovsky ME (2007) Initial orthostatic hypotension: review of a forgotten condition. Clin Sci 112(3–4):157–165. https://doi.org/10.1042/CS20060091
Wolters FJ, Zonneveld HI, Hofman A, Van Der Lugt A, Koudstaal PJ, Vernooij MW, Ikram MA (2017) Cerebral perfusion and the risk of dementia: a population-based study. Circulation 136(8):719–728. https://doi.org/10.1161/CIRCULATIONAHA.117.027448
Zuj KA, Prince CN, Hughson RL, Peterson SD (2018) Enhanced muscle blood flow with intermittent pneumatic compression of the lower leg during plantar flexion exercise and recovery. J Appl Physiol 124(2):302–311. https://doi.org/10.1152/japplphysiol.00784.2017
Zuj KA, Prince CN, Hughson RL, Peterson SD (2019) Superficial femoral artery blood flow with intermittent pneumatic compression of the lower leg applied during walking exercise and recovery. J Appl Physiol 127(2):559–567. https://doi.org/10.1152/japplphysiol.00656.2018
Funding
This work was supported by a Spark 2018 grant from the Centre for Aging and Brain Health Innovation (Baycrest) [to J.D.M.]; Natural Sciences and Engineering Research Council of Canada operating grant [#RGPIN-6473 to R.L.H.]; Natural Sciences and Engineering Research Council of Canada Collaborative Research Development Grant [#CRD-493144-2015 to S.D.P]; and additional grant support from Lockheed Martin Corporation. R.L.H. is Schlegel Research Chair in Vascular Aging and Brain Health.
Author information
Authors and Affiliations
Contributions
The study was conceived and designed by KAZ, ETH, JDM, SDP and RLH, data were collected by KAZ and ETH, analysis was by KAZ, ETH, all authors contributed to the draft manuscript and final version.
Corresponding author
Ethics declarations
Conflict of interest
S.D.P. and R.L.H. are named inventors on U.S. Patent application number 15/564,054 titled “System and method for synchronizing external compression of a limb for increased blood flow”. The patent is owned by Pression LLC, a company aiming to commercialize compression technology. S.D.P. owns a 15% stake in Pression LLC.
Additional information
Communicated by Ellen Adele Dawson.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zuj, K.A., Hedge, E.T., Milligan, J.D. et al. Intermittent compression of the calf muscle as a countermeasure to protect blood pressure and brain blood flow in upright posture in older adults. Eur J Appl Physiol 121, 839–848 (2021). https://doi.org/10.1007/s00421-020-04547-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-020-04547-7