Abstract
Purpose
Dementia is common among patients with primary open angle glaucoma (POAG) and neovascular age-related macular degeneration (nAMD). This study compares visit frequency, diagnostic test utilization, and treatment patterns for POAG and nAMD among persons with vs. without dementia.
Methods
Optum’s de-identified Clinformatics® Data Mart Database (January 1, 2000-June 30, 2022) was used for this study. Two cohorts were created from newly diagnosed POAG or nAMD patients. Within each cohort, an exposure cohort was created of newly diagnosed dementia patients. The primary outcome was the number of visits to an eye care provider. Secondary analyses for the POAG cohort assessed the number of visual field tests, optical coherence tomography (OCT), and glaucoma medication prescription coverage. The secondary analysis for the nAMD cohort included the number of injections performed. Poisson regression was used to determine the relative rates of outcomes.
Results
POAG patients with dementia had reduced rates of eye care visits (RR 0.76, 95% CI: 0.75–0.77), lower rates of testing utilization for visual fields (RR 0.66, 95% CI: 0.63–0.68) and OCT (RR 0.67, 95% CI: 0.64–0.69), and a lower rate of glaucoma prescription medication coverage (RR 0.83, 95% CI: 0.83–0.83). nAMD patients with dementia had reduced rates of eye care visits (RR 0.74, 95% CI: 0.70–0.79) and received fewer intravitreal injections (RR 0.64, 95% CI: 0.58–0.69) than those without dementia.
Conclusions
POAG and nAMD patients with dementia obtained less eye care and less monitoring and treatment of their disease. These findings suggest that this population may be vulnerable to gaps in ophthalmic care.
Key messages
What is known
● Older adults with dementia are less likely to see an ophthalmologist or receive cataract surgery, but treatment disparities have not been examined in the context of other eye diseases.
What is new
● Patients with primary open-angle glaucoma who have dementia are less likely to be seen by an ophthalmologist, have a visual field test or OCT, or have an active prescription for an intraocular pressure-lowering eyedrop than those without dementia.
● Neovascular age-related macular degeneration patients with dementia are also less likely to see an ophthalmologist or receive intravitreal injections than those without dementia.
● Persons living with dementia may be vulnerable to gaps in ophthalmic care.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
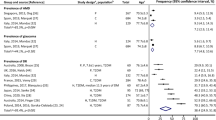
Approximately 7 million people currently live with dementia in the U.S [1]. , and because age is the primary risk factor for dementia, this number is expected to increase dramatically in the coming decades as the older adult population grows in size [2]. Age is also a risk factor for many common eye diseases: by age 80, one out of every 20 individuals has glaucoma, late-stage age-related macular degeneration (AMD), or both [3, 4]. As a result, dementia is a common comorbidity among older adults with macular degeneration and glaucoma.
Visual impairment is a known risk factor for cognitive decline and neuropsychiatric symptoms of dementia [5,6,7], so close monitoring and treatment of ophthalmic disease may have a role in improving functional outcomes and quality of life in these patients in addition to preserving vision. However, there are multiple challenges associated with treating eye disease in older adults with dementia. Patients require frequent visits with an ophthalmologist, especially when receiving intravitreal therapies for AMD, which may strain the limits of caregiver availability. Once patients transition to living in a nursing home, they are even less likely to continue receiving specialty care [8]. Neuropsychiatric symptoms of dementia such as agitation may make intraocular pressure-lowering eyedrops for glaucoma challenging to administer, and in the case of in-office or surgical procedures like intravitreal injections, certain treatments may not be possible if patients are unable to lie still. Even when treatments are possible, ophthalmologists may perceive that patients with functional impairment and reduced life expectancy are unlikely to benefit from them.
Several recent studies have found that persons living with dementia are less likely to see an ophthalmologist or receive cataract surgery compared to those without dementia [9,10,11]. However, these differences have not been examined in the context of other age-related eye diseases such as glaucoma or AMD, for which delays in diagnosis and treatment are associated with adverse visual outcomes [12]. In this study, we used administrative claims data to compare visit frequency, diagnostic test utilization, and treatment patterns for glaucoma and neovascular AMD among persons with vs. without dementia.
Methods
Database
Optum’s de-identified Clinformatics® Data Mart Database was used to abstract data for this study. The database contains all outpatient medical claims (office visits, procedures, and medications given) as well as demographic data and some laboratory values for all patients enrolled in commercial and Medicare Advantage insurance plans. The subset of data available for this study included all patients in the database from January 1, 2000, to June 30, 2022. Due to the de-identified nature of the data, The University of Pennsylvania’s Institutional Review Board deemed this study exempt from review.
Cohorts
All newly diagnosed patients with primary open angle glaucoma (POAG) or neovascular age-related macular degeneration (nAMD) were included in the study creating two cohorts, one for each disease state. (Please see Supplemental Table 1 for the full list of ICD-9/ICD-10 and CPT codes used during this study.) Patients in the POAG cohort were excluded for having a diagnosis of a non-POAG form of glaucoma at any time in the plan. Patients were excluded from the nAMD cohort having any other disease that could be treated with a vascular endothelial growth factor (VEGF)-directed agent. Within each of the two cohorts, an exposure cohort was created of patients who were concurrently diagnosed with dementia. The index date was considered the earliest date of dementia diagnosis. Additional exclusion occurred for any patient who had less than 1 year of time in the insurance plan before and after the index date. To better assess the impact the diagnosis of dementia had on the care of these patients, all patients who were diagnosed with dementia prior to the cohort disease state (POAG, nAMD) were also excluded.
Disease-specific controls were identified from each cohort and matched up to 3:1 with dementia cases based on age, race, sex, and insurance plan start and stop date (± 4 months). After matching occurred, controls were assigned the index date of their dementia-exposed match. All exclusion and inclusion criteria were then applied to the controls the same as the exposed cohort. A secondary analysis was also performed that defined dementia either by ICD code or a prescription of a memory-enhancing medication. Of note, while diagnosis codes have good positive predictive value (up to 70%) for identifying people living with dementia [13], the timing of diagnosis is much less reliable. Specifically, because of its insidious onset and known delays in diagnosis [14], the months or years prior to the first appearance of a diagnosis code are likely also characterized by the presence of dementia. For this reason, we chose to compare POAG and nAMD patients with dementia to those without dementia rather than examining healthcare utilization before vs. after dementia diagnosis.
Outcomes
The primary outcome for both cohorts was the number of visits to an eye care provider in the year following the index date. Secondary analyses for the POAG cohort also included the number of visual field tests performed, OCT’s obtained, and the number of days of glaucoma prescription coverage over the year following the index date. The secondary analysis for the nAMD cohort included the number of injections performed over the following year.
Statistical analysis and covariates
Poisson regression was used to determine the relative rates of outcomes as outlined above. Inverse probability treatment weighting (IPTW) was used to better balance baseline covariates between the dementia patients and matched controls. Covariates assessed included in the multivariable model included age, gender, race, history of diabetes mellitus, hypertension, hypercholesterolemia, kidney disease, stroke, ischemic heart disease, congestive heart failure, previous myocardial infarction, arrhythmia, peripheral artery disease, smoking, education level, household income, and geographic location. Missing values for demographic variables were categorized as “unknown”. To help adjust for the severity of glaucoma, any previous glaucoma surgeries were assessed as were the number of glaucoma medication classes used in the year prior to the index date. All statistical analyses were performed using SAS version 9.4 (SAS Institute Inc., Cary, NC) software. All tests were considered statistically significant at P values of 0.05 (two-tailed).
Results
We included 45,470 individuals with POAG (13,182 with dementia; 32,288 without) and 2,840 with nAMD (932 with dementia; 1908 without). Those included and excluded are summarized in Fig. 1, and demographic characteristics and comorbidities of the POAG and nAMD cohorts before and after inverse probability weighting are presented in Tables 1 and 2. Cases (dementia) and controls (no dementia) were generally well matched with excellent balance (standardized mean difference < 0.1) in both the POAG and nAMD cohorts after IPTW (Tables 1 and 2).
The number of eye care visits and associated diagnostic tests and procedures in the first year after the index date for POAG and nAMD are presented in Table 3. POAG patients with dementia averaged 1.48 (SD ± 1.86) eye care visits in the first year after diagnosis compared with 2.15 (SD ± 2.15) in POAG patients without dementia. The average number of HVF (0.31 vs. 0.53), OCTs (0.23 vs. 0.39) and average days of prescription coverage (59.94 vs. 84.54) were also lower in POAG patients with dementia compared to those without. In IPTW Poisson regression models, POAG patients with dementia had a reduced rate of eye care visits (RR 0.76, 95% CI: 0.75–0.77, p < 0.0001) compared to those without dementia. The disparity between dementia and control patients was more pronounced for the rate of visual fields (RR 0.66, 95% CI: 0.62–0.68, p < 0.0001) and OCT (RR 0.67, 95% CI: 0.64–0.69, p < 0.0001) testing utilization. POAG patients with dementia had a lower rate of prescription coverage for intraocular pressure-lowering medications than controls (RR 0.83, 95% CI: 0.83–0.83, p < 0.0001).
nAMD patients with dementia were also seen less often by eye care providers (1.33 vs. 2.07 visits, RR 0.74, 95% CI: 0.70–0.79, p < 0.0001) and received fewer intravitreal anti-VEGF injections (0.64 vs. 1.19 injections; RR 0.64, 95% CI: 0.58–0.69, p < 0.0001) than nAMD patients without dementia. Similar findings were observed in our secondary analysis in which dementia cases were identified using a combination of diagnosis codes and dementia-related prescriptions (Supplemental Table 2).
Discussion
In this study of over 45,000 older adults in the U.S., we examined healthcare utilization patterns for POAG and nAMD among persons newly diagnosed with dementia. We found that compared to those without dementia, POAG and nAMD patients with dementia obtained less eye care and received less monitoring and treatment of their disease. The rate of reduction in care was fairly consistent across both disease cohorts, with patients having dementia averaging about 75% of the number of visits for non-dementia patients. In-office testing and treatment were also similarly reduced across both diseases, with dementia patients receiving about two thirds of the testing and injections that patients without dementia received. Prescription drug coverage, while reduced, was not as impacted, with dementia patients receiving only 17% less coverage. This may be due to the ease of obtaining prescription medications without the requirement of an office visit. It is possible that reduced POAG medication use in patients with dementia was due to an increase in the use of selective laser trabeculoplasty (SLT) or argon laser trabeculoplasty (ALT), but this is unlikely because these procedures would not impact the need for disease monitoring within the first year of diagnosis and treatment, and we adjusted our analyses for baseline glaucoma surgical history. While our study is not determinative of a causal relationship between dementia and reduced treatment rate, these findings suggest that persons living with dementia may be vulnerable to gaps in ophthalmic care.
Our results are consistent with previous studies showing that persons living with dementia are less likely to be seen by an ophthalmologist or receive cataract surgery [9,10,11]. Disparities in anti-VEGF treatment for AMD have been observed on the basis of race [15], but to our knowledge, the effect of dementia on healthcare utilization for nAMD has not previously been examined. This growing body of literature indicates that persons living with dementia are vulnerable to gaps in ophthalmic care. While our study was not equipped to identify the specific reasons why patients with dementia were less likely to be seen by an ophthalmologist, potential reasons include difficulty making, remembering, and arranging transportation to appointments, especially if caregiver support is limited. Hospitalizations and other comorbidities may also limit the continuity of outpatient ophthalmic care. Visual impairment is an important determinant of quality of life and is associated with progression and neuropsychiatric complications of dementia [5,6,7], so it is possible that promoting eye care utilization in this population may improve functional outcomes. However, while there is preliminary evidence that regular eye care encounters and cataract surgery are associated with a lower incidence of dementia and functional decline [16, 17], the effects of eye care utilization on outcomes among those already living with dementia have not been examined.
Of note, not all underutilization of ophthalmic care is necessarily avoidable or harmful. We found that POAG patients with dementia were 34% less likely to have a visual field test than those without dementia, but because of the cognitive demands associated with maintaining fixation and responding quickly and accurately, visual field tests may not be possible or produce reliable results in persons living with dementia [18]. If cognitive concerns were the primary reason that visual field tests were underutilized, we would have expected greater utilization of OCT, which is more rapid and relies less heavily on prolonged fixation and patient participation. However, interpreting retinal nerve fiber layer and ganglion cell layer thinning in the setting of comorbid glaucoma and dementia is challenging, as these changes are known to occur in neurodegenerative diseases such as Alzheimer’s disease independent of glaucoma [19, 20]. Most patients with POAG are asymptomatic in their early stages, and treatment is aimed at reducing the progression of visual field constriction over years or decades. For people with limited life expectancy due to advanced dementia, these treatments may not yield meaningful benefits if death is expected to occur before clinically significant visual impairment due to untreated glaucoma develops. However, such decisions would require a highly personalized assessment of life expectancy and glaucoma progression, and the clinical and health-economic implications of the de-escalation of ophthalmic care at the end of life have not been examined. In the case of nAMD, anti-VEGF injections have the potential to result in more immediate improvements in visual acuity, but these benefits must be weighed against the tradeoffs in quality of life associated with frequent ophthalmology visits and injection-related discomfort and logistical barriers such as ability to consent and availability of legal guardianship.
The results of this study must be considered within the limitations of its design. Due to the deidentified nature of administrative claims data, we lacked information about ocular disease severity such as visual acuity and OCT results, which are important determinants of visit frequency and treatment. The identification of ophthalmic diagnoses and healthcare utilization within administrative claims data is contingent upon insurance billing and reimbursement, so if patients paid for visits, procedures, or medications out of pocket, these would theoretically not be captured. However, this is very unlikely because the outcomes we examined are covered by insurance, and therefore unlikely for patients to ignore their insurance benefit to pay more out of pocket for these services. Another limitation is the reliance on ICD codes to identify dementia, as dementia is frequently underdiagnosed in clinical practice [21]. To counter this, we tested a more expansive definition of dementia, which did not alter the results of the study. Moreover, if the control population contained persons living with dementia who were misclassified as controls, we would expect this to bias results toward the null, suggesting that our results are an underestimate of the impact of dementia on eye care utilization for these disease states. Older adults in this dataset have private health insurance or are primarily covered through Medicare Advantage plans, and while we would expect similar findings in the Medicare fee-for-service (FFS) population, this is difficult to confirm due to known demographic and socioeconomic differences between FFS and Medicare Advantage enrollees. Finally, type 1 error is always a possibility, especially in the context of multiple hypothesis testing.
We found that being diagnosed with dementia leads to lower utilization of eye care in the year following diagnosis. Although the rate of eye care visits was lower, the largest disparities in care were related to the ancillary testing utilization and treatment. Future studies should examine whether eye care underutilization is associated with worse visual, cognitive, and functional outcomes in people living with dementia. If this is the case, then efforts to promote access to eye care may have a positive public health impact in this population.
References
(2021) 2021 Alzheimer’s disease facts and figures. Alzheimers Dement J Alzheimers Assoc 17:327–406. https://doi.org/10.1002/alz.12328
Dorsey ER, George BP, Leff B, Willis AW (2013) The coming crisis: obtaining care for the growing burden of neurodegenerative conditions. Neurology 80:1989–1996. https://doi.org/10.1212/WNL.0b013e318293e2ce
Rein DB, Wittenborn JS, Burke-Conte Z et al (2022) Prevalence of age-related Macular Degeneration in the US in 2019. JAMA Ophthalmol 140:1202–1208. https://doi.org/10.1001/jamaophthalmol.2022.4401
Gupta P, Zhao D, Guallar E et al (2016) Prevalence of Glaucoma in the United States: the 2005–2008 National Health and Nutrition Examination Survey. Invest Ophthalmol Vis Sci 57:2905–2913. https://doi.org/10.1167/iovs.15-18469
Frank CR, Xiang X, Stagg BC, Ehrlich JR (2019) Longitudinal associations of Self-reported vision impairment with symptoms of anxiety and Depression among older adults in the United States. JAMA Ophthalmol 137:793–800. https://doi.org/10.1001/jamaophthalmol.2019.1085
Chen SP, Azad AD, Pershing S (2021) Bidirectional Association between Visual Impairment and Dementia among older adults in the United States over Time. Ophthalmology 128:1276–1283. https://doi.org/10.1016/j.ophtha.2021.02.021
Hamedani AG, Thibault DP, Shea JA, Willis AW (2020) Self-reported vision and hallucinations in older adults: results from two longitudinal US health surveys. Age Ageing 49:843–849. https://doi.org/10.1093/ageing/afaa043
Ulyte A, Mehrotra A, Huskamp HA et al (2022) Specialty care after transition to long-term care in nursing home. J Am Geriatr Soc. https://doi.org/10.1111/jgs.18129
Pershing S, Henderson VW, Bundorf MK et al (2019) Differences in cataract surgery Rates based on Dementia Status. J Alzheimers Dis JAD 69:423–432. https://doi.org/10.3233/JAD-181292
Pershing S, Goldstein MK, Henderson VW et al (2020) Receipt of Eye Care Services among Medicare Beneficiaries with and without dementia. Ophthalmology 127:1000–1011. https://doi.org/10.1016/j.ophtha.2020.02.022
Stagg BC, Ehrlich JR, Choi H, Levine DA (2018) Association of Cognitive Impairment and Dementia with receipt of cataract surgery among Community-Dwelling Medicare beneficiaries. JAMA Ophthalmol. https://doi.org/10.1001/jamaophthalmol.2018.5138
Ramakrishnan MS, Yu Y, VanderBeek BL (2020) Association of Visit Adherence and visual acuity in patients with Neovascular Age-Related Macular Degeneration: secondary analysis of the comparison of age-related Macular Degeneration Treatment Trial. JAMA Ophthalmol 138:237–242. https://doi.org/10.1001/jamaophthalmol.2019.4577
McCarthy EP, Chang C-H, Tilton N et al (2022) Validation of Claims algorithms to identify Alzheimer’s Disease and related dementias. J Gerontol Biol Sci Med Sci 77:1261–1271. https://doi.org/10.1093/gerona/glab373
Bradford A, Kunik ME, Schulz P et al (2009) Missed and delayed diagnosis of dementia in primary care: prevalence and contributing factors. Alzheimer Dis Assoc Disord 23:306–314. https://doi.org/10.1097/WAD.0b013e3181a6bebc
Mahr MA, Hodge DO, Erie JC (2018) Racial differences in Age-Related Macular Degeneration and Associated Anti-vascular endothelial growth factor Intravitreal injections among Medicare Beneficiaries. Ophthalmol Retina 2:1188–1195. https://doi.org/10.1016/j.oret.2018.05.005
Lee CS, Gibbons LE, Lee AY et al (2022) Association between cataract extraction and development of Dementia. JAMA Intern Med 182:134–141. https://doi.org/10.1001/jamainternmed.2021.6990
Sloan FA, Picone G, Brown DS, Lee PP (2005) Longitudinal analysis of the relationship between regular eye examinations and changes in visual and functional status. J Am Geriatr Soc 53:1867–1874. https://doi.org/10.1111/j.1532-5415.2005.53560.x
Raman P, Khy Ching Y, Sivagurunathan PD et al (2019) The Association between Visual Field Reliability Indices and cognitive impairment in Glaucoma patients. J Glaucoma 28:685–690. https://doi.org/10.1097/IJG.0000000000001269
Thomson KL, Yeo JM, Waddell B et al (2015) A systematic review and meta-analysis of retinal nerve fiber layer change in dementia, using optical coherence tomography. Alzheimers Dement Amst Neth 1:136–143. https://doi.org/10.1016/j.dadm.2015.03.001
Cheung CY, Mok V, Foster PJ et al (2021) Retinal imaging in Alzheimer’s disease. J Neurol Neurosurg Psychiatry 92:983–994. https://doi.org/10.1136/jnnp-2020-325347
McGrath R, Robinson-Lane SG, Klawitter L et al (2022) Undiagnosed dementia is Associated with poor physical function in older adults. J Alzheimers Dis JAD 89:473–482. https://doi.org/10.3233/JAD-220257
Funding
This work was supported by the National Eye Institute (grant number K23 EY033438-02 to AGH) and the University of Pennsylvania Core Grant for Vision Research (2P30EYEY001583). The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH. Additional funding was provided by the Metzger Family, Research to Prevent Blindness and the Paul and Evanina Mackall Foundation. Funding from each of the above sources was received in the form of block research grants. None of the funding organizations had any role in the design or conduction of the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the University of Pennsylvania Institutional Review Board and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Brian VanderBeek had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hamedani, A.G., Chang, A.Y., Chen, Y. et al. Disparities in glaucoma and macular degeneration healthcare utilization among persons living with dementia in the United States. Graefes Arch Clin Exp Ophthalmol (2024). https://doi.org/10.1007/s00417-024-06573-z
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00417-024-06573-z