Abstract
Purpose
To compare central corneal thickness (CCT) measured with optical coherence tomography (OCT) using an automatic algorithm (A-OCT) vs. manual measurements (M-OCT) with respect to the gold standard ultrasound pachymetry (USP).
Methods
CCT measurements were performed on both eyes of 28 healthy subjects at four times of the day. A-OCT used an automatic software analysis of the corneal image, M-OCT was performed by two operators by setting a digital calliper on the corneal borders, and USP was performed after corneal anesthesia. Measurements were compared using a three-way repeated measures ANOVA. Bland–Altman plots were used to evaluate the agreement between OCT measurements and USP.
Results
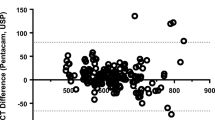
Both A-OCT and M-OCT significantly underestimated the USP measures, with the mean difference, i.e., the systematic error, being larger for A-OCT (− 19.0 µm) than for M-OCT (− 6.5 µm). Good reproducibility between the two operators was observed. Bland–Altman plots showed that both OCT methods suffered from proportional errors, which were not affected by time and eye.
Conclusions
Measuring CCT with OCT yielded lower values than USP. Therefore, clinicians should be aware that corneal thickness values may be influenced by the measurement method and that the various devices should not be used interchangeably in following up a given patient. Intriguingly, M-OCT had less systematic error than A-OCT, an important outcome that clinicians should consider when deciding to use an OCT device.



Similar content being viewed by others
References
Cui J, Zhang X, Hu Q, Zhou WY, Yang F (2016) Evaluation of corneal thickness and volume parameters of subclinical keratoconus using a Pentacam Scheimflug System. Curr Eye Res 41:923–926. https://doi.org/10.3109/02713683.2015.1082188
Shousha MA, Perez VL, Wang J, Ide T, Jiao S, Chen Q, Chang V, Buchser N, Dubovy SR, Feuer W, Yoo SH (2010) Use of ultra-high-resolution optical coherence tomography to detect in vivo characteristics of Descemet’s Membrane in Fuchs’ Dystrophy. Ophthalmology 117:1220–1227. https://doi.org/10.1016/j.ophtha.2009.10.027
Hillenaar T, Van Cleynenbreugel H, Verjans GM, Wubbels RJ, Remeijer L (2012) Monitoring the inflammatory process in herpetic stromal keratitis: the role of in vivo confocal microscopy. Ophthalmology 19:1102–1110. https://doi.org/10.1016/j.ophtha.2011.12.002
Brandt JD, Beiser JA, Kass MA, Gordon MO (2020) Ocular Hypertension Treatment Study (OHTS) Group. Central Corneal Thickness in the Ocular Hypertension Treatment Study (OHTS). Ophthalmology 127:S72–S81. https://doi.org/10.1016/j.ophtha.2020.01.028
Miglior S, Albe E, Guareschi M, Mandelli G, Gomarasca S, Orzalesi N (2004) Intraobserver and interobserver reproducibility in the evaluation of ultrasonic pachymetry measurements of central corneal thickness. Br J Ophthalmol 88:174–177. https://doi.org/10.1136/bjo.2003.023416
Sadoughi MM, Einollahi B, Einollahi N, Rezaei J, Roshandel D, Feizi S (2015) Measurement of central corneal thickness using ultrasound pachymetry and Orbscan II in normal eyes. J Ophthalmic Vis Res 10(1):4–9. https://doi.org/10.4103/2008-322X.156084
Sanchis-Gimeno JA, Palanca-Sanfrancisco JM, García-Lázaro S, Madrid-Costa D, Cerviño A (2013) The effect of anesthetic eye drop instillation on the distribution of corneal thickness. Cornea 32:e102–e105. https://doi.org/10.1097/ICO.0b013e318275e7a6
Li EY, Mohamed S, Leung CK, Rao SK, Cheng AC, Cheung CY, Lam DS (2007) Agreement among 3 methods to measure corneal thickness: ultrasound pachymetry, Orbscan II, and Visante anterior segment optical coherence tomography. Ophthalmology 114:1842–1847. https://doi.org/10.1016/j.ophtha.2007.02.017
Bechmann M, Thiel M, Naubauer A, Ullrich S, Ludwig K, Kenyon KR, Ulbig MW (2001) Central corneal thickness measurement with a retinal optical coherence tomography device versus standard Ultrasound Pachymetry. Cornea 20:50–54. https://doi.org/10.1097/00003226-200101000-00010
Wells M, Wu N, Kokkinakis J, Sutton G (2013) Correlation of central corneal thickness measurements using Topcon TRK-1P, Zeiss Visnte AS-OCT and DGH Pachmate 55 handheld ultrasonic pachymeter. Clin Exp Optom 96:385–387. https://doi.org/10.1111/cxo.12013
Scotto R, Bagnis A, Papadia M, Cutolo CA, Risso D, Traverso CE (2017) Comparison of central corneal thickness measurements using ultrasonic pachymetry, anterior segment OCT and noncontact specular microscopy. J Glaucoma 26:860–865. https://doi.org/10.1097/IJG.0000000000000745
Khaja W, Grover S, Kelmenson A, Ferguson LR, Sambhav K, Chalam KV (2015) Comparison of central corneal thickness: ultrasound pachymetry versus slit-lamp coherence tomography, specular microscopy, and Orbscan. Clin Ophthalmol 9:1065–1070. https://doi.org/10.2147/OPTH.S81376
Artuç T, Batur M (2023) Comparison of central corneal thickness in corneal edema by ultrasound pachymetry, specular microscopy, and anterior segment optical coherence tomography. Saudi J Ophthalmol 9(37):1–5. https://doi.org/10.4103/sjopt.sjopt_63_20
Ayala M, Strandas R (2015) Accuracy of optical coherence tomography (OCT) in pachymetry for glaucoma patients. BMC Ophthalmol 15:124. https://doi.org/10.1186/s12886-015-0116-x
Yoshizo K (1973) Diurnal variation in corneal thickness. Exp Eye Res 15:1–9. https://doi.org/10.1016/0014-4835(73)90183-8
Shah S, Spedding C, Bhojwani R, Kwartz J, Henson D, McLeod D (2000) Assessment of the diurnal variation in central corneal thickness and intraocular pressure for patients with suspected glaucoma. Ophthalmology 107:1191–1193. https://doi.org/10.1016/s0161-6420(00)00090-7
Fogagnolo P, Rossetti L, Mazzolani F, Orzalesi N (2006) Circardian variations in central corneal thickness and intraocular pressure in patients with glaucoma. Br J Ophthalmol 90:24–28. https://doi.org/10.1136/bjo.2005.079285
Du Toit R, Vega JA, Fonn D, Simpson T (2003) Diurnal variation of corneal sensitivity and thickness. Cornea 22:205–209. https://doi.org/10.1097/00003226-200304000-00004
Hamilton KE, Pye DC, Aggarwala S, Evian S, Khosla J, Perera R (2007) Diurnal variation of central corneal thickness and Goldmann applanation tonometry estimates of intraocular pressure. J Glaucoma 16:29–35. https://doi.org/10.1097/IJG.0b013e31802b350f
Read SA, Collins MJ (2009) Diurnal variation of corneal shape and thickness. Optom Vis Sci 86:170–180. https://doi.org/10.1097/OPX.0b013e3181981b7e
Feng Y, Varikooty J, Simpson T (2001) Diurnal variation of corneal and corneal epithelial thickness measured using optical coherence tomography. Cornea 20:408–483. https://doi.org/10.1097/00003226-200107000-00008
Bruttini C, Verticchio Vercellin A, Klersy C, De Silvestri A, Tinelli C, Riva I, Oddone F, Katsanos A, Quaranta L (2020) The Mont Blanc Study: the effect of altitude on intra ocular pressure and central corneal thickness. PLoS ONE 15:e0237343. https://doi.org/10.1371/journal.pone.0237343
Perez-Bermejo M, Cervino A, Calvo-Maroto AM, Moscardo M, Murillo-Llorente M, Sanchis-Gimeno JA (2018) Corneal thickness response after anesthetic eye drops: our own results and meta-analysis. Biomed Res Int 5(2018):4743721. https://doi.org/10.1155/2018/4743721
Ogbuehi KC, Chijuka JC, Osuagwu UL (2012) Changes in central corneal thickness values after instillation of oxybuprocaine hydrochloride 0.4%. Cont Lens Anterior Eye 35:199–202. https://doi.org/10.1016/j.clae.2012.05.004
Fernandez-Garcia P, Cerviño A, Quiles-Guiñau L, Albarran-Diego C, Garcia-Lazaro S, Sanchis-Gimeno JA (2015) Corneal thickness differences between sexes after oxybuprocaine eye drops. Optom Vis Sci 92:89–94. https://doi.org/10.1097/OPX.0000000000000449
Belovay GW, Goldberg I (2018) The thick and thin of the central corneal thickness in glaucoma. Eye (Lond) 32(5):915–923. https://doi.org/10.1038/s41433-018-0033-3
Bograd A, Himmel I, Pfister IB, Seiler TG, Frueh BE, Tappeiner C (2023) Comparison of corneal measurements in keratoconus eyes with two swept-source-optical coherence tomography devices and a Scheimpflug device. Graefes Arch Clin Exp Ophthalmol. Epub ahead of print. https://doi.org/10.1007/s00417-023-06219-6
Doğan M, Ertan E (2019) Comparison of central corneal thickness measurements with standard ultrasonic pachymetry and optical devices. Clin Exp Optom 102:126–130. https://doi.org/10.1111/cxo.12865
Mansoori T, Balakrishna N (2018) Repeatability and agreement of central corneal thickness measurement with non-contact methods: a comparative study. Int Ophthalmol 38:959–966. https://doi.org/10.1007/s10792-017-0543-1
Gokcinar NB, Yumusak E, Ornek N, Yorubulut S, Onaran Z (2019) Agreement and repeatability of central corneal thickness measurements by four different optical devices and an ultrasound pachymeter. Int Ophthalmol 39:1589–1598. https://doi.org/10.1007/s10792-018-0983-2
Chao-Wen L, Tsing-Hong W, Yu-Hsuan H, Jehn-Yu H (2013) Agreement and repeatability of central corneal thickness measurements made by ultrasound pachymetry and anterior segment optical coherence tomography. Taiwan J Ophthalmol 3:98–102. https://doi.org/10.1016/j.tjo.2013.04.007
Kim Y, Joung JY, Ryu SJ, Lim HW (2018) Analysis of which device is reliable for measuring central corneal thickness in novice examiner. Invest Ophthalmol Vis Sci 59:5733
Acknowledgements
The authors would like to thank Dr. Martina Venturi for her support in collecting data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the Fondazione IRCCS Policlinico San Matteo, Pavia, Italy, and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study was approved by The Ethics Committee of the Fondazione IRCCS Policlinico San Matteo, Pavia, Italy (ID # n.20170001732).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bruttini, C., Esposti, R., Pece, A. et al. Comparison of central corneal thickness measured by automatic and manual analysis of optical coherence tomography. Graefes Arch Clin Exp Ophthalmol (2024). https://doi.org/10.1007/s00417-023-06354-0
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00417-023-06354-0