Abstract
Objective
To compare the demographic and clinical phenotypes of thyroid-associated ophthalmopathy (TAO) with euthyroidism (Eu-TAO), hyperthyroidism (Hr-TAO), and hypothyroidism (Ho-TAO).
Methods
We enrolled 2158 TAO patients in this retrospective study and assessed their demographics, clinical manifestations, activity, and severity.
Results
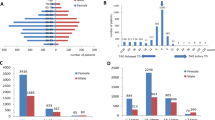
Among the enrolled patients, 526 (24.37%) had Eu-TAO, 1544 (71.55%) had Hr-TAO, and 88 (4.08%) had Ho-TAO. Compared to Hr-TAO (2.02) and Ho-TAO (2.52) patients, Eu-TAO (1.57) patients had the lowest female-to-male ratio (p = 0.026). The mean ages of Eu-TAO, Hr-TAO, and Ho-TAO patients were 43.11 ± 12.05, 42.23 ± 13.63, and 47.39 ± 13.28 years, respectively (p = 0.001). Patients with Eu-TAO had more unilateral involvement (50% vs. 14.38% vs. 21.59%, p < 0.001) than Hr-TAO or Ho-TAO patients. Clinically active TAO patients presented 8.56% in euthyroid vs. 13.86% in hyperthyroid vs. 11.36% in hypothyroid (p = 0.006). Regarding the severity of the European Group on Graves’ Orbitopathy (EUGOGO) classification among euthyroid, hyperthyroid, and hypothyroid patients, mild TAO was present in 67.68, 54.27, and 72.72% of participants, moderate-to-severe TAO in 31.18, 42.49, and 26.14%, and sight-threatening TAO in 1.14, 3.24, and 1.14%, respectively. Eu-TAO was positively correlated with unilateral involvement (OR = 5.671, p < 0.001) and age (OR = 1.013, p = 0.003) and negatively correlated with the female-to-male ratio (OR = 0.656, p < 0.001) and TAO severity (OR = 0.742, p < 0.01).
Conclusions
Eu-TAO patients are older and less likely to be female, and show more unilateral and milder clinical phenotypes than hyper/hypothyroid TAO patients.



Similar content being viewed by others
References
Hiromatsu Y, Eguchi H, Tani J, Kasaoka M, Teshima Y (2014) Graves’ ophthalmopathy: epidemiology and natural history. Int Med (Tokyo, Japan) 53:353–360. https://doi.org/10.2169/internalmedicine.53.1518
Bartalena L, Baldeschi L, Boboridis K, Eckstein A, Kahaly GJ, Marcocci C, Perros P, Salvi M, Wiersinga WM (2016) The 2016 European Thyroid Association/European Group on Graves’ Orbitopathy guidelines for the management of Graves’ orbitopathy. Eur Thyroid J 5:9–26. https://doi.org/10.1159/000443828
Bahn RS (2010) Graves’ ophthalmopathy. N Engl J Med 362:726–738. https://doi.org/10.1056/NEJMra0905750
Li Q, Ye H, Ding Y, Chen G, Liu Z, Xu J, Chen R, Yang H (2017) Clinical characteristics of moderate-to-severe thyroid associated ophthalmopathy in 354 Chinese cases. PLoS One 12:e0176064. https://doi.org/10.1371/journal.pone.0176064
Chin YH, Ng CH, Lee MH, Koh JWH, Kiew J, Yang SP, Sundar G, Khoo CM (2020) Prevalence of thyroid eye disease in Graves’ disease: a meta-analysis and systematic review. Clin Endocrinol. https://doi.org/10.1111/cen.14296
Ben Simon GJ, Katz G, Zloto O, Leiba H, Hadas B, Huna-Baron R (2015) Age differences in clinical manifestation and prognosis of thyroid eye disease. Graefe’s Arch Clin Exp Ophthalmol = Albrecht von Graefes Archiv fur klinische und experimentelle Ophthalmologie 253: 2301–2308. https://doi.org/10.1007/s00417-015-3156-2
Bartalena L, Piantanida E, Gallo D, Lai A, Tanda ML (2020) Epidemiology, natural history, risk factors, and prevention of Graves’ orbitopathy. Front Endocrinol 11:615993. https://doi.org/10.3389/fendo.2020.615993
Eckstein AK, Losch C, Glowacka D, Schott M, Mann K, Esser J, Morgenthaler NG (2009) Euthyroid and primarily hypothyroid patients develop milder and significantly more asymmetrical Graves ophthalmopathy. Br J Ophthalmol 93:1052–1056. https://doi.org/10.1136/bjo.2007.137265
Kashkouli MB, Pakdel F, Kiavash V, Heidari I, Heirati A, Jam S (2011) Hyperthyroid vs hypothyroid eye disease: the same severity and activity. Eye (Lond) 25:1442–1446. https://doi.org/10.1038/eye.2011.186
Suzuki N, Noh JY, Kameda T, Yoshihara A, Ohye H, Suzuki M, Matsumoto M, Kunii Y, Iwaku K, Watanabe N, Mukasa K, Kozaki A, Inoue T, Sugino K, Ito K (2018) Clinical course of thyroid function and thyroid associated-ophthalmopathy in patients with euthyroid Graves’ disease. Clin Ophthalmol (Auckland, NZ) 12:739–746. https://doi.org/10.2147/opth.S158967
Ponto KA, Binder H, Diana T, Matheis N, Otto AF, Pitz S, Pfeiffer N, Kahaly GJ (2015) Prevalence, phenotype, and psychosocial well-being in euthyroid/hypothyroid thyroid-associated orbitopathy. Thyroid 25:942–948. https://doi.org/10.1089/thy.2015.0031
Leo M, Menconi F, Rocchi R, Latrofa F, Sisti E, Profilo MA, Mazzi B, Albano E, Nardi M, Vitti P, Marcocci C, Marino M (2015) Role of the underlying thyroid disease on the phenotype of Graves’ orbitopathy in a tertiary referral center. Thyroid 25:347–351. https://doi.org/10.1089/thy.2014.0475
Bartley GB, Gorman CA (1995) Diagnostic criteria for Graves’ ophthalmopathy. Am J Ophthalmol 119:792–795. https://doi.org/10.1016/s0002-9394(14)72787-4
Mourits MP, Koornneef L, Wiersinga WM, Prummel MF, Berghout A, van der Gaag R (1989) Clinical criteria for the assessment of disease activity in Graves’ ophthalmopathy: a novel approach. Br J Ophthalmol 73:639–644. https://doi.org/10.1136/bjo.73.8.639
Bartalena L, Kahaly GJ, Baldeschi L, Dayan CM, Eckstein A, Marcocci C, Marinò M, Vaidya B, Wiersinga WM (2021) The 2021 European Group on Graves’ Orbitopathy (EUGOGO) clinical practice guidelines for the medical management of Graves’ orbitopathy. Eur J Endocrinol 185:G43-g67. https://doi.org/10.1530/eje-21-0479
Muñoz-Ortiz J, Sierra-Cote MC, Zapata-Bravo E, Valenzuela-Vallejo L, Marin-Noriega MA, Uribe-Reina P, Terreros-Dorado JP, Gómez-Suarez M, Arteaga-Rivera K, de-la-Torre A (2020) Prevalence of hyperthyroidism, hypothyroidism, and euthyroidism in thyroid eye disease: a systematic review of the literature. Syst Rev 9:201. https://doi.org/10.1186/s13643-020-01459-7
Muralidhar A, Das S, Tiple S (2020) Clinical profile of thyroid eye disease and factors predictive of disease severity. Indian J Ophthalmol 68:1629–1634. https://doi.org/10.4103/ijo.IJO_104_20
Termote K, Decallonne B, Mombaerts I (2014) The influence of prior hyperthyroidism on euthyroid Graves’ ophthalmopathy. J Ophthalmol 2014:426898. https://doi.org/10.1155/2014/426898
Kim JM, LaBree L, Levin L, Feldon SE (2004) The relation of Graves’ ophthalmopathy to circulating thyroid hormone status. Br J Ophthalmol 88:72–74. https://doi.org/10.1136/bjo.88.1.72
Taylor PN, Albrecht D, Scholz A, Gutierrez-Buey G, Lazarus JH, Dayan CM, Okosieme OE (2018) Global epidemiology of hyperthyroidism and hypothyroidism. Nat Rev Endocrinol 14:301–316. https://doi.org/10.1038/nrendo.2018.18
Li HX, Xiang N, Hu WK, Jiao XL (2016) Relation between therapy options for Graves’ disease and the course of Graves’ ophthalmopathy: a systematic review and meta-analysis. J Endocrinol Invest 39:1225–1233. https://doi.org/10.1007/s40618-016-0484-y
Panagiotou G, Perros P (2020) Asymmetric Graves’ orbitopathy. Front Endocrinol 11:611845. https://doi.org/10.3389/fendo.2020.611845
Bartley GB (1994) The epidemiologic characteristics and clinical course of ophthalmopathy associated with autoimmune thyroid disease in Olmsted County, Minnesota. Trans Am Ophthalmol Soc 92:477–588
Kozaki A, Inoue R, Komoto N, Maeda T, Inoue Y, Inoue T, Ayaki M (2010) Proptosis in dysthyroid ophthalmopathy: a case series of 10,931 Japanese cases. Optom Vis Sci 87:200–204. https://doi.org/10.1097/OPX.0b013e3181ce5702
Murchison AP, Sires BA, Jian-Amadi A (2009) Margin reflex distance in different ethnic groups. Arch Facial Plast Surg 11:303–305. https://doi.org/10.1001/archfacial.2009.9
Marinò M, Ionni I, Lanzolla G, Sframeli A, Latrofa F, Rocchi R, Marcocci C (2020) Orbital diseases mimicking Graves’ orbitopathy: a long-standing challenge in differential diagnosis. J Endocrinol Invest 43:401–411. https://doi.org/10.1007/s40618-019-01141-3
Siakallis LC, Uddin JM, Miszkiel KA (2018) Imaging investigation of thyroid eye disease. Ophthalmic Plast Reconstr Surg 34:S41-s51. https://doi.org/10.1097/iop.0000000000001139
Jang SY, Lee SY, Lee EJ, Yoon JS (2012) Clinical features of thyroid-associated ophthalmopathy in clinically euthyroid Korean patients. Eye (Lond) 26:1263–1269. https://doi.org/10.1038/eye.2012.132
Funding
This work was supported by West China Hospital, Sichuan University (grant number 2018HXFH024); and Sichuan Provincial Science and Technology Program (grant number 18ZDYF1977).
Author information
Authors and Affiliations
Contributions
Mei Yang: conception, design, data collection, literature search, and preparation and editing of the manuscript. Baixue Du: collection and interpretation of data. Yujiao Wang and Weimin He: critically revising the manuscript for important intellectual content. All authors reviewed and approved the manuscript.
Corresponding author
Ethics declarations
Ethical approval and consent to participate
All procedures performed in this study involving human participants were in accordance with and approved by the review board of West China Hospital of Sichuan University and conformed to the Declaration of Helsinki.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yang, M., Wang, Y., Du, B. et al. Clinical phenotypes of euthyroid, hyperthyroid, and hypothyroid thyroid-associated ophthalmopathy. Graefes Arch Clin Exp Ophthalmol 261, 1995–2002 (2023). https://doi.org/10.1007/s00417-023-05998-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-023-05998-2