Abstract
Aims
The present study investigated the difference in choriocapillaris (CC) perfusion between different AL/K ratio groups with similar spherical equivalent refraction (SER) and analyzed factors affecting CC perfusion.
Methods
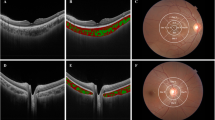
This cross-sectional study included 129 children with low-to-moderate myopia. Axial length (AL), average K-reading (Ave-K), and SER were measured. Choroidal vascularity, including the total choroidal area (TA), choroidal luminal area (LA), stromal area (SA), choroidal vascularity index (CVI), CC flow voids (FVs), and FVs%, was obtained using optical coherence tomography angiography.
Results
Participants with similar SER were divided into two groups (high AL/K ratio, n = 57; low AL/K ratio, n = 72). The high AL/K group had lower LA, TA, and CVI (P < 0.01) and lower FVs (inner ring and fovea, P < 0.05) and FVs% (outer ring, inner ring, and fovea, P < 0.05). The AL/K ratio and FVs% were negatively correlated in the outer ring (r = − 0.174, P < 0.05) and inner ring (r = − 0.174, P < 0.05). The Ave-K and inner FVs (r = 0.178, P < 0.05), outer FVs% (r = 0.175, P < 0.05), and inner FVs% (r = 0.196, P < 0.05) were positively correlated. In stepwise multiple regression for the outer ring, the horizontal CVI was related to FVs (β = 0.175, P < 0.05), and the vertical CVI was related to FVs% (β = 0.232, P < 0.01). Independent risk factors associated with inner FVs area were vertical CVI (β = 0.329; P < 0.001) and SER (β = − 0.196, P < 0.05); FVs% was also associated with vertical CVI (β = 0.360, P < 0.01) and SER (β = − 0.196, P < 0.05).
Conclusion
With a similar SER, myopic eyes with a higher AL/K ratio maintained more CC perfusion and lower CVI, which may indicate rapid myopic progression. Low K-reading eyes had more CC perfusion and less CVI, which may explain the relatively poor myopia control efficacy in the clinic.


Similar content being viewed by others
Abbreviations
- AL:
-
Axial length
- CCT:
-
Central corneal thickness
- ACD:
-
Anterior chamber depth
- LT:
-
Lens thickness
- VCD:
-
Vitreous chamber depth
- Ave-K:
-
Average cornea K-reading
- SER:
-
Spherical equivalent refraction
- ChBF:
-
Choroidal blood flow
- FVs:
-
Blood flow voids
- FVs%:
-
Percentage of blood flow voids
- CVI:
-
Choroidal vascular index
- H-CVI-3 mm:
-
CVI in horizontal scan within 3 mm
- H-CVI-6 mm:
-
CVI in horizontal scan within 6 mm
- V-CVI-3 mm:
-
CVI in vertical scan within 3 mm
- V-CVI-6 mm:
-
CVI in vertical scan within 6 mm
- SFChT:
-
Subfoveal choroidal thickness
- SA:
-
Stromal area
- LA:
-
Luminal area
- TA:
-
Total choroidal area
- NO:
-
Nasal region of the outer ring in ETDRS
- TO:
-
Temporal region of the outer ring in ETDRS
- IO:
-
Inferior region of the outer ring in ETDRS
- SO :
-
Superior region of the outer ring in ETDRS
- NI:
-
Nasal region of the inner ring in ETDRS
- TI:
-
Temporal region of the inner ring in ETDRS
- II:
-
Inferior region of the inner ring in ETDRS
- SI:
-
Superior region of the inner ring in ETDRS
References
Morgan IG, Ohno-Matsui K, Saw SM (2012) Myopia Lancet 379:1739–1748. https://doi.org/10.1016/S0140-6736(12)60272-4
Morgan IG, French AN, Ashby RS, Guo X, Ding X, He M, Rose KA (2018) The epidemics of myopia: aetiology and prevention. Prog Retin Eye Res 62:134–149. https://doi.org/10.1016/j.preteyeres.2017.09.004
Leo SW, Scientific Bureau of World Society of Paediatric O, Strabismus (2017) Current approaches to myopia control. Curr Opin Ophthalmol 28:267–275. https://doi.org/10.1097/ICU.0000000000000367
Vincent SJ, Collins MJ, Read SA, Carney LG (2013) Retinal and choroidal thickness in myopic anisometropia. Invest Ophthalmol Vis Sci 54:2445–2456. https://doi.org/10.1167/iovs.12-11434
Wu H, Zhang G, Shen M, Xu R, Wang P, Guan Z, Xie Z, Jin Z, Chen S, Mao X, Qu J, Zhou X (2021) Assessment of choroidal vascularity and choriocapillaris blood perfusion in anisomyopic adults by SS-OCT/OCTA. Invest Ophthalmol Vis Sci 62:8. https://doi.org/10.1167/iovs.62.1.8
Wu Q, Chen Q, Lin B, Huang S, Wang Y, Zhang L, Lin H, Wang J, Lu F, Shen M (2020) Relationships among retinal/choroidal thickness, retinal microvascular network and visual field in high myopia. Acta Ophthalmol 98:e709–e714. https://doi.org/10.1111/aos.14372
Liu Y, Wang L, Xu Y, Pang Z, Mu G (2021) The influence of the choroid on the onset and development of myopia: from perspectives of choroidal thickness and blood flow. Acta Ophthalmol. https://doi.org/10.1111/aos.14773
Zhang S, Zhang G, Zhou X, Xu R, Wang S, Guan Z, Lu J, Srinivasalu N, Shen M, Jin Z, Qu J, Zhou X (2019) Changes in choroidal thickness and choroidal blood perfusion in guinea pig myopia. Invest Ophthalmol Vis Sci 60:3074–3083. https://doi.org/10.1167/iovs.18-26397
Wakabayashi T, Ikuno Y (2010) Choroidal filling delay in choroidal neovascularisation due to pathological myopia. Br J Ophthalmol 94:611–615. https://doi.org/10.1136/bjo.2009.163535
Wu H, Chen W, Zhao F, Zhou Q, Reinach PS, Deng L, Ma L, Luo S, Srinivasalu N, Pan M, Hu Y, Pei X, Sun J, Ren R, Xiong Y, Zhou Z, Zhang S, Tian G, Fang J, Zhang L, Lang J, Wu D, Zeng C, Qu J, Zhou X (2018) Scleral hypoxia is a target for myopia control. Proc Natl Acad Sci USA 115:E7091–E7100. https://doi.org/10.1073/pnas.1721443115
Swarbrick HA, Alharbi A, Watt K, Lum E, Kang P (2015) Myopia control during orthokeratology lens wear in children using a novel study design. Ophthalmology 122:620–630. https://doi.org/10.1016/j.ophtha.2014.09.028
Zhao W, Li Z, Hu Y, Jiang J, Long W, Cui D, Chen W, Yang X (2021) Short-term effects of atropine combined with orthokeratology (ACO) on choroidal thickness. Cont Lens Anterior Eye 44:101348. https://doi.org/10.1016/j.clae.2020.06.006
Zhou X, Zhang S, Zhang G, Chen Y, Lei Y, Xiang J, Xu R, Qu J, Zhou X (2020) Increased choroidal blood perfusion can inhibit form deprivation myopia in guinea pigs. Invest Ophthalmol Vis Sci 61:25. https://doi.org/10.1167/iovs.61.13.25
Agrawal R, Gupta P, Tan KA, Cheung CM, Wong TY, Cheng CY (2016) Choroidal vascularity index as a measure of vascular status of the choroid: measurements in healthy eyes from a population-based study. Sci Rep 6:21090. https://doi.org/10.1038/srep21090
Chou PI, Lu DW, Chen JT (2002) Effect of sympathetic denervation on rabbit choroidal blood flow. Ophthalmologica 216:60–64. https://doi.org/10.1159/000048299
Li Z, Long W, Hu Y, Zhao W, Zhang W, Yang X (2020) Features of the choroidal structures in myopic children based on image binarization of optical coherence tomography. Invest Ophthalmol Vis Sci 61:18. https://doi.org/10.1167/iovs.61.4.18
Mehta N, Braun PX, Gendelman I, Alibhai AY, Arya M, Duker JS, Waheed NK (2020) Repeatability of binarization thresholding methods for optical coherence tomography angiography image quantification. Sci Rep 10:15368. https://doi.org/10.1038/s41598-020-72358-z
Karakucuk Y, Beyoglu A, Comez A (2020) Quantitative assessment of the effect of fasting on macular microcirculation: an optical coherence tomography angiography study. Br J Ophthalmol 104:1098–1102. https://doi.org/10.1136/bjophthalmol-2019-314962
Riva CE, Titze P, Hero M, Movaffaghy A, Petrig BL (1997) Choroidal blood flow during isometric exercises. Invest Ophthalmol Vis Sci 38:2338–2343
Spaide RF (2016) Choriocapillaris flow features follow a power law distribution: implications for characterization and mechanisms of disease progression. Am J Ophthalmol 170:58–67. https://doi.org/10.1016/j.ajo.2016.07.023
Tan CS, Lim LW, Chow VS, Chay IW, Tan S, Cheong KX, Tan GT, Sadda SR (2016) Optical coherence tomography angiography evaluation of the parafoveal vasculature and its relationship with ocular factors. Invest Ophthalmol Vis Sci 57: OCT224–234 DOI https://doi.org/10.1167/iovs.15-18869
Su L, Ji YS, Tong N, Sarraf D, He X, Sun X, Xu X, Sadda SR (2020) Quantitative assessment of the retinal microvasculature and choriocapillaris in myopic patients using swept-source optical coherence tomography angiography. Graefes Arch Clin Exp Ophthalmol 258:1173–1180. https://doi.org/10.1007/s00417-020-04639-2
Lin T, Yang Y, Lin J, Zhang J, Wen Q, He X, Chen G (2021) A comparative study of macular and choroidal thickness and blood-flow parameters in patients with intermediate and simple juvenile moderate myopia. Int J Gen Med 14:1343–1348. https://doi.org/10.2147/IJGM.S301702
Jonas JB, Nangia V, Sinha A, Gupta R (2011) Corneal refractive power and its associations with ocular and general parameters: the Central India Eye and Medical Study. Ophthalmology 118:1805–1811. https://doi.org/10.1016/j.ophtha.2011.02.001
AlMahmoud T, Priest D, Munger R, Jackson WB (2011) Correlation between refractive error, corneal power, and thickness in a large population with a wide range of ametropia. Invest Ophthalmol Vis Sci 52:1235–1242. https://doi.org/10.1167/iovs.10-5449
Milani P, Montesano G, Rossetti L, Bergamini F, Pece A (2018) Vessel density, retinal thickness, and choriocapillaris vascular flow in myopic eyes on OCT angiography. Graefes Arch Clin Exp Ophthalmol 256:1419–1427. https://doi.org/10.1007/s00417-018-4012-y
Al-Sheikh M, Phasukkijwatana N, Dolz-Marco R, Rahimi M, Iafe NA, Freund KB, Sadda SR, Sarraf D (2017) Quantitative OCT angiography of the retinal microvasculature and the choriocapillaris in myopic eyes. Invest Ophthalmol Vis Sci 58:2063–2069. https://doi.org/10.1167/iovs.16-21289
Scherm P, Pettenkofer M, Maier M, Lohmann CP, Feucht N (2019) Choriocapillary blood flow in myopic subjects measured with OCT angiography. Ophthalmic Surg Lasers Imaging Retina 50:E133–E139. https://doi.org/10.3928/23258160-20190503-13
Patil P, Karthikeyan A (2020) A survey on K-means clustering for analyzing variation in data. Springer Singapore, Singapore, pp. 317–323.
Iovino C, Chhablani J, Rasheed MA, Tatti F, Bernabei F, Pellegrini M, Giannaccare G, Peiretti E (2021) Effects of different mydriatics on the choroidal vascularity in healthy subjects. Eye (Lond) 35:913–918. https://doi.org/10.1038/s41433-020-0995-9
Arej N, Azar G, Salviat F, Alonso AS, Zuber K, Metten MA, Salomon L, Vasseur V, Mauget-Faysse M (2021) Study of choroidal thickness variations after ingestion of a taurine and caffeine-containing energy drink. Clin Nutr ESPEN 43:245–249. https://doi.org/10.1016/j.clnesp.2021.04.007
Tan CS, Ouyang Y, Ruiz H, Sadda SR (2012) Diurnal variation of choroidal thickness in normal, healthy subjects measured by spectral domain optical coherence tomography. Invest Ophthalmol Vis Sci 53:261–266. https://doi.org/10.1167/iovs.11-8782
Llanas S, Linderman RE, Chen FK, Carroll J (2020) Assessing the use of incorrectly scaled optical coherence tomography angiography images in peer-reviewed studies: a systematic review. JAMA Ophthalmol 138:86–94. https://doi.org/10.1001/jamaophthalmol.2019.4821
Sampson DM, Gong P, An D, Menghini M, Hansen A, Mackey DA, Sampson DD, Chen FK (2017) Axial length variation impacts on superficial retinal vessel density and foveal avascular zone area measurements using optical coherence tomography angiography. Invest Ophthalmol Vis Sci 58:3065–3072. https://doi.org/10.1167/iovs.17-21551
Bennett AG, Rudnicka AR, Edgar DF (1994) Improvements on Littmann’s method of determining the size of retinal features by fundus photography. Graefes Arch Clin Exp Ophthalmol 232:361–367. https://doi.org/10.1007/BF00175988
Chu Z, Cheng Y, Zhang Q, Zhou H, Dai Y, Shi Y, Gregori G, Rosenfeld PJ, Wang RK (2020) Quantification of choriocapillaris with Phansalkar local thresholding: pitfalls to avoid. Am J Ophthalmol 213:161–176. https://doi.org/10.1016/j.ajo.2020.02.003
Reiner A, Fitzgerald MEC, Del Mar N, Li C (2018) Neural control of choroidal blood flow. Prog Retin Eye Res 64:96–130. https://doi.org/10.1016/j.preteyeres.2017.12.001
Flower RW, Fryczkowski AW, McLeod DS (1995) Variability in choriocapillaris blood flow distribution. Invest Ophthalmol Vis Sci 36:1247–1258
Li C, Fitzgerald MEC, Del Mar N, Haughey C, Reiner A (2018) Defective choroidal blood flow baroregulation and retinal dysfunction and pathology following sympathetic denervation of choroid. Invest Ophthalmol Vis Sci 59:5032–5044. https://doi.org/10.1167/iovs.18-24954
Sun G, Chen C, Jiang J, Yi Z, Wang X, Miao Q, Xu A, He L (2021) New insights into the association between choroidal vessels and choriocapillaris in normal eyes. Retina. https://doi.org/10.1097/IAE.0000000000003238
Li SM, Ren MY, Gan J, Zhang SG, Kang MT, Li H, Atchison DA, Rozema J, Grzybowski A, Wang N, Anyang Childhood Eye Study G (2022) Machine learning to determine risk factors for myopia progression in primary school children: the Anyang Childhood Eye Study. Ophthalmol Ther. https://doi.org/10.1007/s40123-021-00450-2
Lam CS, Edwards M, Millodot M, Goh WS (1999) A 2-year longitudinal study of myopia progression and optical component changes among Hong Kong schoolchildren. Optom Vis Sci 76:370–380. https://doi.org/10.1097/00006324-199906000-00016
Kong Q, Guo J, Zhou J, Zhang Y, Dou X (2017) Factors determining effective orthokeratology treatment for controlling juvenile myopia progression. Iran J Public Health 46:1217–1222
Wan K, Cheung SW, Wolffsohn JS, Orr JB, Cho P (2018) Role of corneal biomechanical properties in predicting of speed of myopic progression in children wearing orthokeratology lenses or single-vision spectacles. BMJ Open Ophthalmol 3:e000204. https://doi.org/10.1136/bmjophth-2018-000204
Flitcroft DI (2012) The complex interactions of retinal, optical and environmental factors in myopia aetiology. Prog Retin Eye Res 31:622–660. https://doi.org/10.1016/j.preteyeres.2012.06.004
Hughes RP, Vincent SJ, Read SA, Collins MJ (2020) Higher order aberrations, refractive error development and myopia control: a review. Clin Exp Optom 103:68–85. https://doi.org/10.1111/cxo.12960
Zhang X, Ma JH, Xi X, Guan L (2020) Characteristics of corneal high-order aberrations in adolescents with mild to moderate myopia. BMC Ophthalmol 20:465. https://doi.org/10.1186/s12886-020-01727-z
Hiraoka T, Kotsuka J, Kakita T, Okamoto F, Oshika T (2017) Relationship between higher-order wavefront aberrations and natural progression of myopia in schoolchildren. Sci Rep 7:7876. https://doi.org/10.1038/s41598-017-08177-6
Chen X, Sankaridurg P, Donovan L, Lin Z, Li L, Martinez A, Holden B, Ge J (2010) Characteristics of peripheral refractive errors of myopic and non-myopic Chinese eyes. Vision Res 50:31–35. https://doi.org/10.1016/j.visres.2009.10.004
Mutti DO, Sholtz RI, Friedman NE, Zadnik K (2000) Peripheral refraction and ocular shape in children. Invest Ophthalmol Vis Sci 41:1022–1030
Ouyang Y, Heussen FM, Mokwa N, Walsh AC, Durbin MK, Keane PA, Sanchez PJ, Ruiz-Garcia H, Sadda SR (2011) Spatial distribution of posterior pole choroidal thickness by spectral domain optical coherence tomography. Invest Ophthalmol Vis Sci 52:7019–7026. https://doi.org/10.1167/iovs.11-8046
Ikuno Y, Kawaguchi K, Nouchi T, Yasuno Y (2010) Choroidal thickness in healthy Japanese subjects. Invest Ophthalmol Vis Sci 51:2173–2176. https://doi.org/10.1167/iovs.09-4383
Funding
This work was supported by the National Natural Science Foundation of China (Grant No. 82171092, 81870684) and the National Key R&D Program of China (Grant No.2020YFC2008200).
Author information
Authors and Affiliations
Contributions
X. Li participated in conception and design of this work, data acquisition and analysis, and in literature search and manuscript writing. M. Lu and J. Hu contributed to data collection and the acquisition of fundus photograph and picture processing of the datasets. Q. Xu contributed to data collection and data analysis. Y. Li, J. Qu, and M. Zhao contributed to the interpretation of data, and revision of the manuscript for this study. K. Wang contributed to design of the work, interpretation of data, and revision of the manuscript for this study. All authors read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study design adhered to the principles of the Helsinki Declaration and was approved by the Ethics Committee of Peking University People’s Hospital. Study approval number is 2020PHB276.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Li, X., Ma, L., Hu, J. et al. Corneal morphology correlates with choriocapillaris perfusion in myopic children. Graefes Arch Clin Exp Ophthalmol 260, 3375–3385 (2022). https://doi.org/10.1007/s00417-022-05675-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-022-05675-w