Abstract
Purpose
To investigate microvascular abnormalities in diabetic patients without conventional clinical signs of diabetic retinopathy (DR).
Methods
In this cross-sectional observational cohort study, the study group included randomly chosen participants of a community-based cohort with diabetes type 2 without DR, and the control group consisted of non-diabetic individuals from a population-based study. All participants underwent optical coherence tomographic angiography (OCTA).
Results
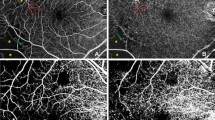
Upon OCTA, 118 (40.4%) eyes of the study group (n = 292 eyes) showed microvascular abnormalities including foveal avascular zone erosion (95 (32.5%) eyes), non-perfusion areas in the superficial and deep retinal layers (39 (13.4%) eyes and 19 (6.5%) eyes, respectively), and microaneurysms in the superficial and deep retinal layers (22 (7.5%) eyes and 31 (10.6%) eyes, resp.). None of these abnormalities was detected in the control group (n = 80). The study group showed a lower vessel density in the superficial retinal vascular layer in all regions except for the foveal region (P < 0.001), and higher vessel density in the parafoveal region in the deep retinal vascular layer (P = 0.01). Higher diabetes prevalence was associated with lower superficial retinal vascular density (P = 0.005) in multivariable analysis. A lower radial peripapillary capillary flow density was correlated (regression coefficient r, 0.62) with higher fasting blood concentration of glucose (P < 0.001) in multivariable analysis.
Conclusions
OCTA revealed microvascular abnormalities in 40% of eyes of diabetic patients without ophthalmoscopically detectable diabetic fundus changes in a community-based population. The early stage of DR may be re-defined upon OCTA.


Similar content being viewed by others
References
Danaei G, Finucane MM, Lu Y, Singh GM, Cowan MJ, Paciorek CJ, Lin JK, Farzadfar F, Khang YH, Stevens GA, Rao M, Ali MK, Riley LM, Robinson CA, Ezzati M, Global Burden of Metabolic Risk Factors of Chronic Diseases Collaborating Group (Blood Glucose) (2011) National, regional, and global trends in fasting plasma glucose and diabetes prevalence since 1980: systematic analysis of health examination surveys and epidemiological studies with 370 country-years and 2•7 million participants. Lancet 378:31–40
NCD Risk Factor Collaboration (2016) Worldwide trends in diabetes since 1980: pooled analysis of 751 population-based measurement studies with over 4.4 million participants. Lancet 387:1513–1530
Yau JWY, Rogers SL, Kawasaki R, Lamoureux EL, Kowalski JW, Bek T, Chen SJ, Dekker JM, Fletcher A, Grauslund J, Haffner S, Hamman RF, Ikram MK, Kayama T, Klein BE, Klein R, Krishnaiah S, Mayurasakorn K, O'Hare JP, Orchard TJ, Porta M, Rema M, Roy MS, Sharma T, Shaw J, Taylor H, Tielsch JM, Varma R, Wang JJ, Wang N, West S, Xu L, Yasuda M, Zhang X, Mitchell P, Wong TY, Meta-Analysis for Eye Disease (META-EYE) Study Group (2012) The global prevalence and major risk factors of diabetic retinopathy and vision-threatening retinopathy in persons with diabetes. Diabetes Care 35:556–564
Leasher JL, Bourne RR, Flaxman SR, Jonas JB, Keeffe J, Naidoo K, Pesudovs K, Price H, White RA, Wong TY, Resnikoff S, Taylor HR, Vision Loss Expert Group of the Global Burden of Disease Study (2016) Global estimates on the number of people blind or visually impaired by diabetic retinopathy: a meta-analysis from 1990 to 2010. Diabetes Care 39:1643–1649
Sabanayagam C, Banu R, Chee ML, Lee R, Wang YX, Tan G, Jonas JB, Lamoureux EL, Cheng CY, Klein BEK, Mitchell P, Klein R, Cheung CMG, Wong TY (2019) Incidence and progression of diabetic retinopathy: a systematic review. Lancet Diabetes Endocrinol 7:140–149
Kim AY, Chu Z, Shahidzadeh A, Wang RK, Puliafito CA, Kashani AH (2016) Quantifying microvascular density and morphology in diabetic retinopathy using spectral-domain optical coherence tomography angiography. Invest Ophthalmol Vis Sci 57:362–370
Salz DA, de Carlo TE, Adhi M, Moult E, Choi W, Baumal CR, Witkin AJ, Duker JS, Fujimoto JG, Waheed NK (2016) Select features of diabetic retinopathy on swept-source optical coherence tomographic angiography compared with fluorescein angiography and normal eyes. JAMA Ophthalmol 134:644–650
Bandello F, Corbelli E, Carnevali A, Pierro L, Querques G (2016) Optical coherence tomography angiography of diabetic retinopathy. Dev Ophthalmol 56:107–112
Simonett JM, Scarinci F, Picconi F, Giorno P, De Geronimo D, Di Renzo A, Varano M, Frontoni S, Parravano M (2017) Early microvascular retinal changes in optical coherence tomography angiography in patients with type 1 diabetes mellitus. Acta Ophthalmol 95:e751–e755
Dimitrova G, Chihara E, Takahashi H, Amano H, Okazaki K (2017) Quantitative retinal optical coherence tomography angiography in patients with diabetes without diabetic retinopathy. Invest Ophthalmol Vis Sci 58:190–196
Soares M, Neves C, Marques IP, Pires I, Schwartz C, Costa MÂ, Santos T, Durbin M, Cunha-Vaz J (2017) Comparison of diabetic retinopathy classification using fluorescein angiography and optical coherence tomography angiography. Br J Ophthalmol 101:62–68
Tang FY, Ng DS, Lam A, Luk F, Wong R, Chan C, Mohamed S, Fong A, Lok J, Tso T, Lai F, Brelen M, Wong TY, Tham CC, Cheung CY (2017) Determinants of quantitative optical coherence tomography angiography metrics in patients with diabetes. Sci Rep 7:2575
Chen Q, Ma Q, Wu C, Tan F, Chen F, Wu Q, Zhou R, Zhuang X, Lu F, Qu J, Shen M (2017) Macular vascular fractal dimension in the deep capillary layer as an early indicator of microvascular loss for retinopathy in type 2 diabetic patients. Invest Ophthalmol Vis Sci 58:3785–3794
Scarinci F, Picconi F, Giorno P, Boccassini B, De Geronimo D, Varano M, Frontoni S, Parravano M (2018) Deep capillary plexus impairment in patients with type 1 diabetes mellitus with no signs of diabetic retinopathy revealed using optical coherence tomography angiography. Acta Ophthalmol 96:e264–e265
Safi H, Safi S, Hafezi-Moghadam A, Ahmadieh H (2018) Early detection of diabetic retinopathy. Surv Ophthalmol 63:601–608
Rosen RB, Andrade Romo JS, Krawitz BD, Mo S, Fawzi AA, Linderman RE, Carroll J, Pinhas A, Chui TYP (2019) Earliest evidence of preclinical diabetic retinopathy revealed using OCT angiography (OCTA) perfused capillary density. Am J Ophthalmol 203:103–115
Li Z, Wen X, Zeng P, Liao Y, Fan S, Zhang Y, Li Y, Xiao J, Lan Y (2019) Do microvascular changes occur preceding neural impairment in early-stage diabetic retinopathy? Evidence based on the optic nerve head using optical coherence tomography angiography. Acta Diabetol 56:531–539
Zeng Y, Cao D, Yu H, Yang D, Zhuang X, Hu Y, Li J, Yang J, Wu Q, Liu B, Zhang L (2019, 2019) Early retinal neurovascular impairment in patients with diabetes without clinically detectable retinopathy. Br J Ophthalmol. https://doi.org/10.1136/bjophthalmol-2018-313582
Miwa Y, Murakami T, Suzuma K, Uji A, Yoshitake S, Fujimoto M, Yoshitake T, Tamura Y, Yoshimura N (2016) Relationship between functional and structural changes in diabetic vessels in optical coherence tomography angiography. Sci Rep 6:29064
Bhanushali D, Anegondi N, Gadde SG, Srinivasan P, Chidambara L, Yadav NK, Sinha Roy A (2016) Linking retinal microvasculature features with severity of diabetic retinopathy using optical coherence tomography angiography. Invest Ophthalmol Vis Sci 57:OCT519–OCT525
Balaratnasingam C, Inoue M, Ahn S, McCann J, Dhrami-Gavazi E, Yannuzzi LA, Freund KB (2016) Visual acuity is correlated with the area of the foveal avascular zone in diabetic retinopathy and retinal vein occlusion. Ophthalmology 123:2352–2367
Lee J, Moon BG, Cho AR, Yoon YH (2016) Optical coherence tomography angiography of DME and its association with anti-VEGF treatment response. Ophthalmology 123:2368–2375
Samara WA, Shahlaee A, Adam MK, Khan MA, Chiang A, Maguire JI, Hsu J, Ho AC (2017) Quantification of diabetic macular ischemia using optical coherence tomography angiography and its relationship with visual acuity. Ophthalmology 124:235–244
Durbin MK, An L, Shemonski ND, Soares M, Santos T, Lopes M, Neves C, Cunha-Vaz J (2017) Quantification of retinal microvascular density in optical coherence tomographic angiography images in diabetic retinopathy. JAMA Ophthalmol 135:370–376
Kashani AH, Chen CL, Gahm JK, Zheng F, Richter GM, Rosenfeld PJ, Shi Y, Wang RK (2017) Optical coherence tomography angiography: a comprehensive review of current methods and clinical applications. Prog Retin Eye Res 60:66–100
Hirano T, Kitahara J, Toriyama Y, Kasamatsu H, Murata T, Sadda S (2019) Quantifying vascular density and morphology using different swept-source optical coherence tomography angiographic scan patterns in diabetic retinopathy. Br J Ophthalmol 103:216–221
Parravano M, De Geronimo D, Scarinci F, Virgili G, Querques L, Varano M, Bandello F, Querques G (2019) Progression of diabetic microaneurysms according to the internal reflectivity on structural optical coherence tomography and visibility on optical coherence tomography angiography. Am J Ophthalmol 198:8–16
Xu J, Wei WB, Yuan MX, Yuan SY, Wan G, Zheng YY, Li YB, Wang S, Xu L, Fu HJ, Zhu LX, Pu XL, Zhang JD, Du XP, Li YL, Ji Y, Gu XN, Li Y, Pan SF, Cui XL, Bai W, Chen YJ, Wang ZM, Zhu QS, Gao Y, Liu DY, Ji YT, Yang Z, Jonas JB (2012) Prevalence and risk factors for diabetic retinopathy: the Beijing Communities Diabetes Study 6. Retina (Philadelphia, Pa) 32:322–329
Han QL, Wu SL, Liu XX, An SS, Wu YT, Gao JS, Chen SH, Liu XK, Zhang Q, Mao RY, Shang XM, Jonas JB (2016) Ideal cardiovascular health score and incident end-stage renal disease in a community-based longitudinal cohort study: the Kailuan Study. BMJ Open 6:e012486
Spaide RF (2016) Retinal vascular cystoid macular edema: review and new theory. Retina (Philadelphia, Pa) 36:1823–1842
Hirano T, Kakihara S, Toriyama Y, Nittala MG, Murata T, Sadda S (2018) Wide-field en face swept-source optical coherence tomography angiography using extended field imaging in diabetic retinopathy. Br J Ophthalmol 102:1199–1203
Sawada O, Ichiyama Y, Obata S, Ito Y, Kakinoki M, Sawada T, Saishin Y, Ohji M (2018) Comparison between wide-angle OCT angiography and ultra-wide field fluorescein angiography for detecting non-perfusion areas and retinal neovascularization in eyes with diabetic retinopathy. Graefes Arch Clin Exp Ophthalmol 256:1275–1280
Acknowledgements
The authors would like to thank the support from the Xinjiekou and Jinsong Community Health Service Centers for their assistance of recruiting diabetes participants and the Beijing Communities Diabetes Study for contributing systemic parameters.
Funding
This study was financially supported by the Beijing Municipal Administration of Hospitals Clinical Medicine Development of Special Funding Support (code: ZYLX201307), National Natural Science Foundation of China (Nr. 81272981), Beijing Natural Science Foundation (Nr. 7151003), Advanced Health Care Professionals Development Project of Beijing Municipal Health Bureau (No. 2014-2-003), The priming scientific research foundation for the junior research in Beijing Tongren Hospital Capital Medical University (2017-YJJ-ZZL-009 and NO. 2018-YJJ-ZZL-046), and Beijing Municipal Administration of Hospitals Incubating Program (Code: PX2019008).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no competing interests.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study was approved by the Medical Ethics Committee of the Beijing Tongren Hospital, and written informed consent was obtained from all study participants, and all methods were performed in accordance with the relevant guidelines and regulations.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yang, J.Y., Wang, Q., Yan, Y.N. et al. Microvascular retinal changes in pre-clinical diabetic retinopathy as detected by optical coherence tomographic angiography. Graefes Arch Clin Exp Ophthalmol 258, 513–520 (2020). https://doi.org/10.1007/s00417-019-04590-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-019-04590-x