Abstract
Purpose
To compare and evaluate the agreement between the measurements obtained with a swept-source optical coherence tomography (OCT)-based biometer, the IOLMaster® 700 (IOLM), and those obtained by an optical biometer based on optical low-coherence interferometry (OLCI), the Aladdin (ALD); To evaluate the ability to perform biometric measurements in those eyes with transparency alterations.
Methods
Fifty-five eyes of 55 subjects were included in this study. Axial length (AL), corneal power (K, in diopters) and its astigmatism, anterior chamber depth (ACD), central corneal thickness (CCT), and lens thickness (LT) measures were obtained within both biometers, Zeiss IOLMaster 700 and Topcon Aladdin. Results were analyzed and compared using the Student’s paired samples t-test, Bland–Altman analysis and intraclass correlation coefficient (ICC).
Results
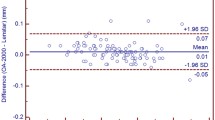
Mean age was 73.12 ± 2.63 (62–89 years). The IOLM mean AL, K, and LT values did not show a statistically significant difference from ALD values and showed excellent agreement and correlation (ICC = 1.000, 0.970, 0.952). IOLM measured a lower mean ACD (−0.036 mm) and higher CCT measurements (9.296 μm). Those results were statistically different (p < 0.001 in both cases) but showed an excellent correlation coefficients (ICC = 0.994, 0.938). IOLM was able to obtain measures from all the eyes examined, while ALD did not measure in two cases with dense nuclear cataract. ALD showed spherical K measures in 7.27% of cases.
Conclusion
Overall a quite good agreement between IOLM and ALD was found. ALD showed spherical keratometry measures in 7.27% of cases. IOLMaster 700 was more effective in obtaining AL measurements in eyes with dense cataracts.







Similar content being viewed by others
References
Rabsilber TM, Jepsen C, Auffarth GU et al (2010) Intraocular lens power calculation: clinical comparison of 2 optical biometry devices. J Cataract Refract Surg 36(2):230–234
Kaswin G, Rousseau A, Mgarrech M, Barreau E, Labetoulle M (2014) Biometry and intraocular lens power calculation results with a new optical biometry device: comparison with the gold standard. J Cataract Refract Surg 40(4):593–600
Mandal P, Berrow EJ, Naroo SA, Wolffsohn JS, Uthoff D, Holland D et al (2014) Validity and repeatability of the Aladdin ocular biometer. Br J Ophthalmol 98(2):256–258
Akman A, Asena L, Gungor SG (2015) Evaluation and comparison of the new swept source OCT-based IOLMaster 700 with the IOLMaster 500. Br J Ophthalmol. Published Online First: 16 December 2015. https://doi.org/10.1136/bjophthalmol-2015-307779
Huang J, Savini G, Wu F, Yu X, Yang J, Yu A et al (2015) Repeatability and reproducibility of ocular biometry using a new noncontact optical low-coherence interferometer. J Cataract Refract Surg 41(10):2233–2241
Srivannaboon S, Chirapapaisan C, Chonpimai P, Loket S (2015) Clinical comparison of a new swept-source optical coherence tomography-based optical biometer and a time-domain optical coherence tomography-based optical biometer. J Cataract Refract Surg 41(10):2224–2232
Hoffer KJ, Shammas HJ, Savini G, Huang J (2016) Multicenter study of optical low-coherence interferometry and partial-coherence interferometry optical biometers with patients from the United States and China. J Cataract Refract Surg 42(1):62–67
Kurian M, Negalur N, Das S, Puttaiah NK, Haria D, J TS et al (2016) Biometry with a new swept-source optical coherence tomography biometer: repeatability and agreement with an optical low-coherence reflectometry device. J Cataract Refract Surg 42(4):577–581
Li J, Chen H, Savini G, Lu W, Yu X, Bao F et al (2016) Measurement agreement between a new biometer based on partial coherence interferometry and a validated biometer based on optical low-coherence reflectometry. J Cataract Refract Surg 42(1):68–75
Sabatino F, Findl O, Maurino V (2016) Comparative analysis of optical biometers. J Cataract Refract Surg 42(5):685–693
Findl O (2005) Biometry and intraocular lens power calculation. Curr Opin Ophthalmol 16(1):61–64
Haigis W, Lege B, Miller N, Schneider B (2000) Comparison of immersion ultrasound biometry and partial coherence interferometry for intraocular lens calculation according to Haigis. Graefes Arch Clin Exp Ophthalmol 238(9):765–773
Chylack LT Jr, Wolfe JK, Singer DM, Leske MC, Bullimore MA, Bailey IL et al (1993) The lens opacities classification system III. The Longitudinal Study of Cataract Study Group. Arch Ophthalmol 111(6):831–836
McAlinden C, Khadka J, Pesudovs K (2011) Statistical methods for conducting agreement (comparison of clinical tests) and precision (repeatability or reproducibility) studies in optometry and ophthalmology. Ophthalmic Physiol Opt 31(4):330–338
Olsen T (1992) Sources of error in intraocular lens power calculation. J Cataract Refract Surg 18(2):125–129
Sanders DR, Retzlaff JA, Kraff MC, Gimbel HV, Raanan MG (1990) Comparison of the SRK/T formula and other theoretical and regression formulas. J Cataract Refract Surg 16(3):341–346
Aristodemou P, Knox Cartwright NE, Sparrow JM, Johnston RL (2011) Formula choice: Hoffer Q, Holladay 1, or SRK/T and refractive outcomes in 8108 eyes after cataract surgery with biometry by partial coherence interferometry. J Cataract Refract Surg 37(1):63–71
Eom Y, Kang SY, Song JS, Kim YY, Kim HM (2014) Comparison of Hoffer Q and Haigis formulae for intraocular lens power calculation according to the anterior chamber depth in short eyes. Am J Ophthalmol 157(4):818.e2–824.e2
Funding
No funding was received for this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge, or beliefs) in the subject matter or materials discussed in this manuscript.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee (INCIVI – Madrid Spain) and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Calvo-Sanz, J.A., Portero-Benito, A. & Arias-Puente, A. Efficiency and measurements agreement between swept-source OCT and low-coherence interferometry biometry systems. Graefes Arch Clin Exp Ophthalmol 256, 559–566 (2018). https://doi.org/10.1007/s00417-018-3909-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-018-3909-9