Abstract
Purpose
The purpose of this study was to investigate the long-term outcome of high hypermetropic refractive errors in childhood.
Methods
We retrospectively reviewed data from the clinical records of 164 children with spherical equivalent (SE) hypermetropic refractive errors in three medical centers collected over 29 years. Refractive errors between +1.00 and +3.00 diopter (D) on initial examination were classified as mild hypermetropia and those +5.00D or greater were classified as high hypermetropia. The four variables studied were, age, refractive error, strabismus, and gender. The rate of reduction in hypermetropic refractive error was calculated over time in years. We identified subgroups according to age, gender, and initial refractive error.
Results
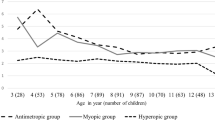
Seventy-eight children with high hypermetropia and 86 children with mild hypermetropia were studied. High hypermetropia was detected at a mean age of 3.3 years, while mild hypermetropia was detected at a mean 4 years of age. The mean follow-up was 6.6 years for high hypermetropia and 6.4 years for mild hypermetropia. Over the follow-up period, children in all subgroups tended to reduce their refractive errors. The reduction in refraction power was small for both mild and high hypermetropic refractive errors. Amblyopia in the high hypermetropia group was more common and more refractory to treatment.
Conclusions
Most children with hypermetropia of less than +3.00D experience a reduction in hyperopic refractive error over time and will outgrow any need for corrective lenses. Children with hyperopia greater than +5.00D will not experience a significant reduction in the power of the refractive error.
Similar content being viewed by others
References
Cook RC, Glasscock RE (1951) Refractive and ocular findings in the newborn. Am J Ophthalmol 34(10):1407–1413
Atkinson J, Braddick O, Nardini M, Anker S (2007) Infant hyperopia: detection, distribution, changes and correlates-outcomes from the Cambridge infant screening programs. Optom Vis Sci 84(2):84–96
Robaei D, Rose K, Ojaimi E et al (2005) Visual acuity and the causes of visual loss in a population-based sample of 6-year-old Australian children. Ophthalmology 112(7):1275–1282
Ip JM, Huynh SC, Robaei D et al (2008) Ethnic differences in refraction and ocular biometry in a population-based sample of 11–15-year-old Australian children. Eye (London) 22(5):649–656
Ojaimi E, Rose KA, Morgan IG et al (2005) Distribution of ocular biometric parameters and refraction in a population-based study of Australian children. Invest Ophthalmol Vis Sci 46(8):2748–2754
Hirsch M, Weymouth F (1991) Prevalence of refractive anomalies. In: Grovenor T, Flom M (eds) Refractive abnormalities research and clinical applications. Butterworth-Heinemann, Boston
Colburn JD, Morrison DG, Estes RL et al (2010) Longitudinal follow-up of hypermetropic children identified during preschool vision screening. J AAPOS 14(3):211–215
Ingram RM, Gill LE, Lambert TW (2008) Effect of spectacles on changes of spherical hypermetropia in infants who did, and did not, have strabismus. Br J Ophthalmol 84(3):324–326
Blouza JA, Loukil I, Mhenni A et al (2007) Management of hyperopia in children. J Fr Ophtalmol 30(3):255–259
Li CH, Chen PL, Chen JT, Fu JJ (2009) Different corrections of hypermetropic errors in the successful treatment of hypermetropic amblyopia in children 3 to 7 years of age. Am J Ophthalmol 147(2):357–363
Walline JJ, Sinnott L, Johnson ED et al (2008) What do kids think about kids in eyeglasses? Ophthalmic Physiol Opt 28(3):218–224
Edwards M (1991) The refractive status of Hong Kong Chinese infants. Ophthalmic Physiol Opt 11(4):297–303
Saunders KJ, Woodhouse JM, Westall CA (1995) Emmetropisation in human infancy: rate of change is related to initial refractive error. Vis Res 35(9):1325–1328
Breslin KM, O’Donoghue L, Saunders KJ (2013) A prospective study of spherical refractive error and ocular components among Northern Irish schoolchildren (the NICER study). Invest Ophthalmol Vis Sci 54(7):4843–4850
Littell R, Milliken G, Stroup W et al (2006) SAS for mixed models, 2nd edn. SAS Institute, Inc., Cary
Mayer DL, Hansen RM, Moore BD et al (2001) Cycloplegic refractions in healthy children aged 1 through 48 months. Arch Ophthalmol 119(11):1625–1628
Mutti DO, Mitchell GL, Jones LA et al (2005) Axial growth and changes in lenticular and corneal power during emmetropization in infants. Invest Ophthalmol Vis Sci 46(9):3074–3080
Mutti DO, Mitchell GL, Jones LA et al (2009) Accommodation, acuity, and their relationship to emmetropization in infants. Optom Vis Sci 86(6):666–676
Kuo A, Sinatra RB, Donahue SP (2003) Distribution of refractive error in healthy infants. J AAPOS 7(3):174–177
French AN, Morgan IG, Mitchell P, Rose KA (2013) Risk factors for incident myopia in Australian schoolchildren: the Sydney adolescent vascular and eye study. Ophthalmology 120(10):2100–2108
Saunders KJ (1995) Early refractive development in humans. Surv Ophthalmol 40(3):207–216
Tarczy-Hornoch K (2007) The epidemiology of early childhood hyperopia. Optom Vis Sci 84(2):115–123
Gwiazda J, Thorn F, Bauer J, Held R (1993) Myopic children show insufficient accommodative response to blur. Invest Ophthalmol Vis Sci 34(3):690–694
Ohlsson J, Baumann M, Sjostrand J (2004) Longterm refractive and visual outcomes in subjects with high hyperopia. Acta Ophthalmol Scand 82(4):486–487
Kulp MT, Foster NC, Holmes JM et al (2012) Effect of ocular alignment on emmetropization in children <10 years with amblyopia. Am J Ophthalmol 154(2):297–302, e1
Bankes JL (1983) Do unnecessary spectacles make the eyes worse. Arch Dis Child 58(10):766
Teikari J, Koskenvuo M, Kaprio J, O’Donnell J (1990) Study of gene-environment effects on development of hyperopia: a study of 191 adult twin pairs from the Finnish Twin cohort study. Acta Genet Med Gemellol (Roma) 39(1):133–136
Medina A (1987) A model for emmetropization: predicting the progression of ametropia. Ophthalmologica 194(2–3):133–139
Atkinson J, Braddick O, Robier B et al (1996) Two infant vision screening programmes: prediction and prevention of strabismus and amblyopia from photo- and videorefractive screening. Eye (London) 10(Pt 2):189–198
Simons K (2005) Amblyopia characterization, treatment, and prophylaxis. Surv Ophthalmol 50(2):123–166
Edelman PM, Borchert MS (1997) Visual outcome in high hypermetropia. J AAPOS 1(3):147–150
Fern KD (1989) Visual acuity outcome in isometropic hyperopia. Optom Vis Sci 66(10):649–658
Schoenleber DB, Crouch ER Jr (1987) Bilateral hypermetropic amblyopia. J Pediatr Ophthalmol Strabismus 24(2):75–77
Chen W, Chen J, Zhang F et al (2013) Visual outcome in isoametropic amblyopic children with high hyperopia and the effect of therapy on retinal thickness. Am J Ophthalmol 155(3):536–543, e1
Acknowledgments
We would like to thank Prof. Ayala Cohen and Dr. Tatiana Umansky, Statistics Laboratory, Faculty of Industrial Engineering and Management, Technion – Israel Institute of Technology, Haifa, Israel, and Boris Futerman, MSc, Clinical Epidemiology Unit, Rambam Healthcare Campus, Haifa, Israel, for performing the statistical modeling and calculations.
Financial interest (all authors)
None
Conflict of interest
All authors certify that they have no affiliation with and no involvement in any organization or entity with any financial interest (such as honoraria; educational grants, participation in speakers, bureaus, membership, employment, consultancies, stock or ownership, or other equity interest; and expert testimony or patent-licensing arrangements) or non-financial interest (such as personal or professional relationships, affiliations, knowledge or benefits) in the subject matter or material discussed in this manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
Institutions at which the study was conducted include the Department of Ophthalmology, Rambam Health Care Campus, Haifa, Israel; Hamburg University, Hamburg, Germany; and the University of Pittsburgh School of Medicine, Pittsburgh, PA, USA.
Rights and permissions
About this article
Cite this article
Mezer, E., Meyer, E., Wygnansi-Jaffe, T. et al. The long-term outcome of the refractive error in children with hypermetropia . Graefes Arch Clin Exp Ophthalmol 253, 1013–1019 (2015). https://doi.org/10.1007/s00417-015-3033-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-015-3033-z