Abstract
Background
With the development of noninvasive brain stimulation (NIBS) techniques, many researchers have turned their attention to NIBS as a promising treatment for cerebellar ataxia. Therefore, we conducted a systematic review and meta-analysis to investigate the efficacy and safety of NIBS in treating patients with cerebellar ataxia.
Methods
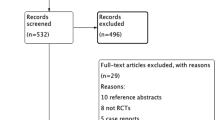
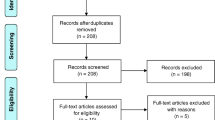
Databases, including PubMed, Embase, Web of Science, Medline, and Cochrane Library, were retrieved for relevant randomized controlled trials (RCTs). Two researchers conducted literature screening, data extraction, literature quality assessment, and heterogeneity analysis between RCTs. According to the magnitude of heterogeneity I2, an appropriate data analysis model was selected for meta-analysis.
Results
A total of 14 RCTs including 406 patients with cerebellar ataxia met the inclusion criteria. The included RCTs had an overall low-risk bias and an intermediate level of evidence recommendation for key outcome indicators, such as the scale for the assessment and rating of ataxia (SARA) and international cooperative ataxia rating scale (ICARS). The results of meta-analysis showed that cerebellar NIBS, including transcranial direct current stimulation (tDCS) and repetitive transcranial magnetic stimulation (rTMS), was effective in reducing the SARA scores (MD = − 3.45, 95%CI = [− 4.85, − 2.50], P < 0.05) and ICARS scores (MD = − 10.87, 95%CI = [− 14.46, − 7.28], P < 0.05) in patients with cerebellar ataxia compared to controls. Subgroup analysis showed that the efficacy of tDCS and rTMS was statistically different in patients with cerebellar ataxia as assessed by the SARA scores, but not by the ICARS scores. There was statistically significant difference in the efficacy of NIBS for the treatment of cerebellar ataxia caused by different etiologies. As for safety, 8 of 14 included studies documented the adverse effects of NIBS, and only two studies reported the mild adverse events of NIBS.
Conclusions
Cerebellar NIBS was safe and effective in improving the motor coordination of patients with cerebellar ataxia, and tDCS was better than rTMS in the treatment of cerebellar ataxia. In addition, the efficacy of NIBS was different in the treatment of different types of cerebellar ataxia.


















Similar content being viewed by others
Data availability
Published data used for the systematic review and meta-analysis are available from the authors.
References
Brusse E, Maat-Kievit JA, van Swieten JC (2007) Diagnosis and management of early- and late-onset cerebellar ataxia. Clin Genet 71(1):12–24
Manto MU (2005) The wide spectrum of spinocerebellar ataxias (SCAs). Cerebellum 4(1):2–6
Pandolfo M (2009) Friedreich ataxia: the clinical picture. J Neurol 256(Suppl 1):3–8
Evidente VG et al (2000) Hereditary ataxias. Mayo Clin Proc 75(5):475–490
Manto M, Marmolino D (2009) Cerebellar ataxias. Curr Opin Neurol 22(4):419–429
Zesiewicz TA et al (2018) Comprehensive systematic review summary: treatment of cerebellar motor dysfunction and ataxia: Report of the Guideline Development, Dissemination, and Implementation Subcommittee of the American Academy of Neurology. Neurology 90(10):464–471
Liberati A et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med 6(7):e1000100
Higgins JP et al (2011) The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343:d5928
Higgins JP et al (2003) Measuring inconsistency in meta-analyses. BMJ 327(7414):557–560
Goldet G, Howick J (2013) Understanding GRADE: an introduction. J Evid Based Med 6(1):50–54
Guyatt G et al (2011) GRADE guidelines: 1. Introduction-GRADE evidence profiles and summary of findings tables. J Clin Epidemiol 64(4):383–394
Egger M et al (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315(7109):629–634
Cha HG (2017) The effect of low-frequency (1 Hz) rTMS on the cerebellar cortex in patients with ataxia after a posterior circulation stroke: randomized control trial. J Magn 22(4):625–629
Kim WS et al (2014) Effect of repetitive transcranial magnetic stimulation over the cerebellum on patients with ataxia after posterior circulation stroke: a pilot study. J Rehabil Med 46(5):418–423
França C et al (2020) Effects of cerebellar transcranial magnetic stimulation on ataxias: a randomized trial. Parkinsonism Relat Disord 80:1–6
Chen TX et al (2021) The efficacy and safety of transcranial direct current stimulation for cerebellar ataxia: a systematic review and meta-analysis. Cerebellum 20(1):124–133
Song P et al (2020) Repetitive transcranial magnetic stimulation of the cerebellum improves ataxia and cerebello-fronto plasticity in multiple system atrophy: a randomized, double-blind, sham-controlled and TMS-EEG study. Aging (Albany NY) 12(20):20611–20622
Manor B et al (2019) Repetitive transcranial magnetic stimulation in spinocerebellar ataxia: a pilot randomized controlled trial. Front Neurol 10:73 (electronic resource)
Shiga Y et al (2002) Transcranial magnetic stimulation alleviates truncal ataxia in spinocerebellar degeneration. J Neurol Neurosurg Psychiatry 72(1):124–126
Benussi A et al (2015) Cerebellar transcranial direct current stimulation in patients with ataxia: a double-blind, randomized, sham-controlled study. Mov Disord 30(12):1701–1705
Maas R et al (2022) Cerebellar transcranial direct current stimulation in spinocerebellar ataxia type 3: a randomized, double-blind, sham-controlled trial. Neurotherapeutics 02:02
Benussi A et al (2018) Cerebello-spinal tDCS in ataxia: a randomized, double-blind, sham-controlled, crossover trial. Neurology 91(12):e1090–e1101
Benussi A et al (2017) Long term clinical and neurophysiological effects of cerebellar transcranial direct current stimulation in patients with neurodegenerative ataxia. Brain Stimul 10(2):242–250
Ahn JH et al (2022) M1 and cerebellar tDCS for MSA-C: a double-blind, randomized, sham-controlled, crossover study. Cerebellum. https://doi.org/10.1007/s12311-022-01416-1
Benussi A et al (2021) Motor and cognitive outcomes of cerebello-spinal stimulation in neurodegenerative ataxia. Brain 144(8):2310–2321
Barretto TL et al (2019) Transcranial direct current stimulation in the treatment of cerebellar ataxia: a two-phase, double-blind, auto-matched, pilot study. Clin Neurol Neurosurg 182:123–129
Joo BE, Lee CN, Park KW (2012) Prevalence rate and functional status of cerebellar ataxia in Korea. Cerebellum 11(3):733–738
Marchina S et al (2021) Transcranial direct current stimulation for post-stroke dysphagia: a systematic review and meta-analysis of randomized controlled trials. J Neurol 268(1):293–304
Elsner B, Kugler J, Mehrholz J (2020) Transcranial direct current stimulation (tDCS) for improving aphasia after stroke: a systematic review with network meta-analysis of randomized controlled trials. J Neuroeng Rehabil 17(1):88
Yao L et al (2020) Low-frequency repetitive transcranial magnetic stimulation in patients with poststroke aphasia: systematic review and meta-analysis of its effect upon communication. J Speech Lang Hear Res 63(11):3801–3815
De Risio L et al (2020) Recovering from depression with repetitive transcranial magnetic stimulation (rTMS): a systematic review and meta-analysis of preclinical studies. Transl Psychiatry 10(1):393
Lefaucheur JP et al (2017) Evidence-based guidelines on the therapeutic use of transcranial direct current stimulation (tDCS). Clin Neurophysiol 128(1):56–92
Choi JH et al (2022) Placebo response in degenerative cerebellar ataxias: a descriptive review of randomized, placebo-controlled trials. J Neurol 269(1):62–71
Funding
This work was supported by the Key Research and Development Project of Jiangxi Province (20203BBGL73127) to Mao-Yuan Wang.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflicts of interest
None.
Ethical approval
This article is a meta-analysis of randomized controlled trials and does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
In this article, no patient care was involved.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gong, C., Long, Y., Peng, XM. et al. Efficacy and safety of noninvasive brain stimulation for patients with cerebellar ataxia: a systematic review and meta-analysis of randomized controlled trials. J Neurol 270, 4782–4799 (2023). https://doi.org/10.1007/s00415-023-11799-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-023-11799-8