Abstract
Background
The best treatment for acute ischemic stroke (AIS) due to isolated cervical internal carotid artery occlusion (CICAO) (i.e., without associated occlusion of the circle of Willis) is still unknown. In this study, we aimed to describe EVT safety and clinical outcome in patients with CICAO.
Methods
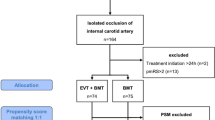
We analyzed data of all consecutive patients, included in the Endovascular Treatment in Ischemic Stroke (ETIS) Registry between 2013 and 2020, who presented AIS and proven CICAO on angiogram and underwent EVT. We assessed carotid recanalization, procedural complications, National Institutes of Health Stroke Scale (NIHSS) at 24 h post-EVT, and 3-month favorable outcome (modified Rankin Scale, mRS ≤ 2 or equal to the pre-stroke value).
Results
Forty-five patients were included (median age: 70 years; range: 62–82 years). The median NIHSS before EVT was 14 (9–21). Carotid stenting was performed in 23 (51%) patients. Carotid recanalization at procedure end and on control imaging was observed in 37 (82%) and 29 (70%) patients, respectively. At day 1 post-EVT, the NIHSS remained stable or decreased in 25 (60%) patients; 12 (29%) patients had early neurologic deterioration (NIHSS ≥ 4 points). The rate of procedural complications was 36%, including stent thrombosis (n = 7), intracranial embolism (n = 7), and symptomatic intracranial hemorrhage (n = 1). At 3 months, 18 (40%) patients had a favorable outcome, and 10 (22%) were dead.
Conclusion
Our study suggests that EVT in AIS patients with moderate/severe initial deficit due to CICAO led to high rate of recanalization at day 1, and a 40% rate of favorable outcome at 3 months. There was a high rate of procedural complication which is of concern. Randomized controlled trials assessing the superiority of EVT in patients with CICAO and severe deficits are needed.




Similar content being viewed by others
Data availability statement
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Abbreviations
- ASPECTS:
-
Alberta stroke program early CT score
- CICAO:
-
Cervical isolated internal carotid artery occlusion
- CT:
-
Computed tomography
- DSA:
-
Digital subtraction angiography
- END:
-
Early neurological deterioration
- ETIS:
-
Endovascular treatment in ischemic stroke
- EVT:
-
Endovascular treatment
- ICA:
-
Internal carotid artery
- IVT:
-
Intravenous thrombolysis
- LVO:
-
Large vessel occlusion
- MRI:
-
Magnetic resonance imaging
- mRS:
-
Modified rankin scale
- NIHSS:
-
National institutes of health stroke scale
References:
Paciaroni M, Caso V, Venti M et al (2005) Outcome in patients with stroke associated with internal carotid artery occlusion. Cerebrovasc Dis 20:108–113. https://doi.org/10.1159/000086800
Damania D, Kung NT-M, Jain M et al (2016) Factors associated with recurrent stroke and recanalization in patients presenting with isolated symptomatic carotid occlusion. Eur J Neurol 23:127–132. https://doi.org/10.1111/ene.12819
Ter Schiphorst A, Gaillard N, Dargazanli C, Mourand I, Corti L, Charif M, Ayrignac X, Lippi A, Bouly S, Thibault L et al (2021) Symptomatic isolated internal carotid artery occlusion with initial medical management: a monocentric cohort. J Neurol 268:346–355
Mazya MV, Cooray C, Lees KR et al (2018) Minor stroke due to large artery occlusion. When is intravenous thrombolysis not enough? Results from the SITS International Stroke Thrombolysis Register. Eur Stroke J 3:29–38. https://doi.org/10.1177/2396987317746003
Boulenoir N, Turc G, Henon H, Laksiri N, Mounier-Véhier F, Buttaz IG, Duong D-L, Papassin J, Yger M, Triquenot A et al (2021) Early neurological deterioration following thrombolysis for minor stroke with isolated internal carotid artery occlusion. Eur J Neurol 28:479–490
Gliem M, Lee J-I, Barckhan A et al (2017) Outcome and treatment effects in stroke associated with acute cervical ICA occlusion. PLoS ONE 12:e0170247. https://doi.org/10.1371/journal.pone.0170247
Yeo LLL, Kong WY, Paliwal P et al (2016) Intravenous thrombolysis for acute ischemic stroke due to cervical internal carotid artery occlusion. J Stroke Cerebrovasc Dis 25:2423–2429. https://doi.org/10.1016/j.jstrokecerebrovasdis.2016.06.014
Pechlaner R, Knoflach M, Matosevic B et al (2013) Recanalization of extracranial internal carotid artery occlusion after i.v. thrombolysis for acute ischemic stroke. PLoS ONE 8:e55318. https://doi.org/10.1371/journal.pone.0055318
EC/IC Bypass Study Group (1985) Failure of extracranial-intracranial arterial bypass to reduce the risk of ischemic stroke. N Engl J Med 313:1191–1200. https://doi.org/10.1056/NEJM198511073131904
Powers WJ, Clarke WR, Grubb RL et al (2011) Extracranial-intracranial bypass surgery for stroke prevention in hemodynamic cerebral ischemia: the carotid occlusion surgery study randomized trial. JAMA 306:1983–1992. https://doi.org/10.1001/jama.2011.1610
Powers WJ, Rabinstein AA, Ackerson T et al (2019) Guidelines for the early management of patients with acute ischemic stroke: 2019 update to the 2018 guidelines for the early management of acute ischemic stroke: a guideline for Healthcare Professionals From the American Heart Association/American Stroke Association. Stroke. https://doi.org/10.1161/STR.0000000000000211
Goyal M, Menon BK, van Zwam WH et al (2016) Endovascular thrombectomy after large-vessel ischaemic stroke: a meta-analysis of individual patient data from five randomised trials. Lancet 387:1723–1731. https://doi.org/10.1016/S0140-6736(16)00163-X
Bracard S, Ducrocq X, Mas JL et al (2016) Mechanical thrombectomy after intravenous alteplase versus alteplase alone after stroke (THRACE): a randomised controlled trial. Lancet Neurol 15:1138–1147. https://doi.org/10.1016/S1474-4422(16)30177-6
Nogueira RG, Jadhav AP, Haussen DC et al (2018) Thrombectomy 6 to 24 hours after stroke with a mismatch between deficit and infarct. N Engl J Med 378:11–21. https://doi.org/10.1056/NEJMoa1706442
Albers GW, Marks MP, Kemp S et al (2018) Thrombectomy for stroke at 6 to 16 hours with selection by perfusion imaging. N Engl J Med 378:708–718. https://doi.org/10.1056/NEJMoa1713973
Mesnil D, de Rochemont R, Sitzer M, Neumann-Haefelin T et al (2004) Endovascular recanalization of acute atherothrombotic carotid artery occlusion holds up progressive stroke. Neuroradiology 46:583–586. https://doi.org/10.1007/s00234-004-1214-2
Jovin TG, Gupta R, Uchino K et al (2005) Emergent stenting of extracranial internal carotid artery occlusion in acute stroke has a high revascularization rate. Stroke 36:2426–2430. https://doi.org/10.1161/01.STR.0000185924.22918.51
Dabitz R, Triebe S, Leppmeier U et al (2007) Percutaneous recanalization of acute internal carotid artery occlusions in patients with severe stroke. Cardiovasc Intervent Radiol 30:34–41. https://doi.org/10.1007/s00270-005-0286-7
Bae G-Y, Hong J-H, Sohn S-I, et al (2008) Emergent carotid stenting in acute stroke patients with steno-occlusion of proximal internal carotid artery
Baik SK, Jeon U, Choo KS et al (2011) What is the real risk of dislodging thrombi during endovascular revascularization of a proximal internal carotid artery occlusion? Neurosurgery 68:1084–1091. https://doi.org/10.1227/NEU.0b013e31820a19fc
Kono K, Tanaka Y, Yoshimura R et al (2011) Emergent carotid artery stenting using a flow reversal system for acute atherosclerotic occlusion of the internal carotid artery. Acta Neurochir 153:2175–2180. https://doi.org/10.1007/s00701-011-1142-y
Matsubara N, Miyachi S, Tsukamoto N et al (2013) Endovascular intervention for acute cervical carotid artery occlusion. Acta Neurochir 155:1115–1123. https://doi.org/10.1007/s00701-013-1697-x
Dalyai RT, Chalouhi N, Singhal S et al (2013) Stent-assisted endovascular recanalization of extracranial internal carotid artery occlusion in acute ischemic stroke. World Neurosurg 79:143–148. https://doi.org/10.1016/j.wneu.2012.08.017
Choi JY, Lee JI, Lee TH et al (2014) Emergent recanalization with stenting for acute stroke due to athero-thrombotic occlusion of the cervical internal carotid artery: a single center experience. J Kor Neurosurg Soc 55:313. https://doi.org/10.3340/jkns.2014.55.6.313
Kwak JH, Zhao L, Kim JK et al (2014) The outcome and efficacy of recanalization in patients with acute internal carotid artery occlusion. Am J Neuroradiol 35:747–753. https://doi.org/10.3174/ajnr.A3747
Son S, Choi DS, Oh MK et al (2015) Emergency carotid artery stenting in patients with acute ischemic stroke due to occlusion or stenosis of the proximal internal carotid artery: a single-center experience. J NeuroIntervent Surg 7:238–244. https://doi.org/10.1136/neurintsurg-2014-011141
Cohen JE, Gomori JM, Leker RR et al (2016) Emergency revascularization of acute internal carotid artery occlusion: follow the spike, it guides you. J Clin Neurosci 29:95–99. https://doi.org/10.1016/j.jocn.2015.12.013
Jadhav A, Panczykowski D, Jumaa M et al (2018) Angioplasty and stenting for symptomatic extracranial non-tandem internal carotid artery occlusion. J NeuroIntervent Surg 10:1155–1160. https://doi.org/10.1136/neurintsurg-2018-013810
Nakagawa N, Fukawa N, Tsuji K et al (2018) Urgent carotid artery stenting for carotid-related stroke-in-evolution. Oper Neurosurg 14:9–15. https://doi.org/10.1093/ons/opx073
de Castro-Afonso LH, Nakiri GS, Moretti Monsignore L et al (2019) Endovascular reperfusion for acute isolated cervical carotid occlusions: the concept of “hemodynamic thrombectomy.” Intervent Neurol. https://doi.org/10.1159/000493021
Mizowaki T, Fujita A, Inoue S et al (2020) Outcome and effect of endovascular treatment in stroke associated with acute extracranial internal carotid artery occlusion: single-center experience in Japan. J Stroke Cerebrovasc Dis 29:104824. https://doi.org/10.1016/j.jstrokecerebrovasdis.2020.104824
Desilles J-P, Consoli A, Redjem H et al (2017) Successful reperfusion with mechanical thrombectomy is associated with reduced disability and mortality in patients with pretreatment diffusion-weighted imaging-alberta stroke program early computed tomography score ≤6. Stroke 48:963–969. https://doi.org/10.1161/STROKEAHA.116.015202
Kernan WN, Ovbiagele B, Black HR et al (2014) Guidelines for the prevention of stroke in patients with stroke and transient ischemic attack: a guideline for healthcare professionals From the American Heart Association/American Stroke Association. Stroke 45:2160–2236. https://doi.org/10.1161/STR.0000000000000024
Legrand L, Tisserand M, Turc G et al (2015) Do FLAIR vascular hyperintensities beyond the DWI lesion represent the ischemic penumbra? Am J Neuroradiol 36:269–274. https://doi.org/10.3174/ajnr.A4088
ter Schiphorst A, Charron S, Hassen WB, et al (2020) Tissue no-reflow despite full recanalization following thrombectomy for anterior circulation stroke with proximal occlusion: a clinical study. J Cereb Blood Flow Metab. https://doi.org/10.1177/0271678X20954929
Prosser J, Butcher K, Allport L et al (2005) Clinical-diffusion mismatch predicts the putative penumbra with high specificity. Stroke 36:1700–1704. https://doi.org/10.1161/01.STR.0000173407.40773.17
Jovin TG, Chamorro A, Cobo E et al (2015) Thrombectomy within 8 hours after symptom onset in ischemic stroke. N Engl J Med 372:2296–2306. https://doi.org/10.1056/NEJMoa1503780
Seners P, Turc G, Tisserand M et al (2014) Unexplained early neurological deterioration after intravenous thrombolysis: incidence, predictors, and associated factors. Stroke 45:2004–2009. https://doi.org/10.1161/STROKEAHA.114.005426
Hacke W, Kaste M, Fieschi C et al (1998) Randomised double-blind placebo-controlled trial of thrombolytic therapy with intravenous alteplase in acute ischaemic stroke (ECASS II). The Lancet 352:1245–1251. https://doi.org/10.1016/S0140-6736(98)08020-9
Weimar C, Goertler M, Harms L et al (2006) Distribution and outcome of symptomatic stenoses and occlusions in patients with acute cerebral ischemia. Arch Neurol 63:1287. https://doi.org/10.1001/archneur.63.9.1287
Yilmaz U, Körner H, Mühl-Benninghaus R et al (2017) Acute occlusions of dual-layer carotid stents after endovascular emergency treatment of tandem lesions. Stroke 48:2171–2175. https://doi.org/10.1161/STROKEAHA.116.015965
Eker OF, Bühlmann M, Dargazanli C et al (2018) Endovascular treatment of atherosclerotic tandem occlusions in anterior circulation stroke: technical aspects and complications compared to isolated intracranial occlusions. Front Neurol. https://doi.org/10.3389/fneur.2018.01046
Pop R, Zinchenko I, Quenardelle V et al (2019) Predictors and clinical impact of delayed stent thrombosis after thrombectomy for acute stroke with tandem lesions. Am J Neuroradiol 40:533–539. https://doi.org/10.3174/ajnr.A5976
Pfaff JAR, Maurer C, Broussalis E et al (2020) Acute thromboses and occlusions of dual layer carotid stents in endovascular treatment of tandem occlusions. J NeuroIntervent Surg 12:33–37. https://doi.org/10.1136/neurintsurg-2019-015032
Mokin M, Kass-Hout T, Kass-Hout O et al (2012) Intravenous thrombolysis and endovascular therapy for acute ischemic stroke with internal carotid artery occlusion: a systematic review of clinical outcomes. Stroke 43:2362–2368. https://doi.org/10.1161/STROKEAHA.112.655621
Acknowledgements
We would like to thank Jessica Hattinguais and Amel Benali for their help in data collection. On behalf of the ETIS-Research Investigators: CHRU Montpellier: Cyril Dargazanli, Caroline Arquizan, Vincent Costalat, Grégory Gascou, Pierre-Henri Lefèvre, Imad Derraz, Carlos Riquelme, Nicolas Gaillard, Isabelle Mourand, Lucas Corti, Federico Cagnazzo, Adrien ter Schiphorst; Hôpital Foch: Adrien Wang, Serge Evrard, Maya.Tchikviladze, Nadia Ajili, Bertrand Lapergue, David Weisenburger-Lile, Lucas Gorza, Géraldine Buard, Oguzhan Coskun, Arturo Consoli, Federico Di Maria, Georges Rodesh, Sergio Zimatore, Morgan Leguen, Julie Gratieux, Fernando Pico, Haja Rakotoharinandrasana, Philippe Tassan, Roxanna Poll, Sylvie Marinier; CHRU-Nancy: Benjamin Gory, Serge Bracard, René Anxionnat, Marc Braun, Anne-Laure Derelle, Romain Tonnelet, Liang Liao, François Zhu, Emmanuelle Schmitt, Sophie Planel, Sébastien Richard, Lisa Humbertjean, Gioia Mione, Jean-Christophe Lacour, Nolwenn Riou-Comte, Gérard Audibert, Marcela Voicu, Lionel Alb, Marie Reitter, Madalina Brezeanu, Agnès Masson, Adriana Tabarna, Iona Podar; CHRU Bordeaux: Gaultier Marnat, Florent Gariel, Xavier Barreau, Jérôme Berge, Louis Veunac, Patrice Menegon, Igor Sibon, Ludovic Lucas, Stéphane Olindo, Pauline Renou, Sharmila Sagnier, Mathilde Poli, Sabrina Debruxelles, François Rouanet, Thomas Tourdias, Jean-Sebastien Liegey, Pierre Briau, Nicolas Pangon; CHRU Nantes: Romain Bourcier, Lili Detraz, Benjamin Daumas-Duport, Pierre-Louis Alexandre, Monica Roy, Cédric Lenoble, Hubert Desal, Benoît Guillon, Solène de Gaalon, Cécile Preterre; Fondation Rothschild: Michel Piotin, Raphaël Blanc, Hocine Redjem, Simon Escalard, Jean-Philippe Desilles, François Delvoye, Stanislas Smajda, Benjamin Maier, Solène Hebert, Mikaël Mazighi, Mikael Obadia, Candice Sabben, Pierre Seners, Igor Raynouard, Ovide Corabianu, Thomas de Broucker, Eric Manchon, Guillaume Taylor, Malek Ben Maacha, Thion Laurie-Anne, Lecler Augustin, Savatovsjy Julien; Hôpital Kremlin-Bicêtre: Laurent Spelle, Christian Denier, Olivier Chassin, Vanessa Chalumeau, Jildaz Caroff, Olivier Chassin, Laura Venditti
Funding
This research received no specific Grant from any funding agency in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Consortia
Contributions
CA, AtS, RP, BL, MO, and CD: carried out the study design, planned the study data collection, participated to the interpretation of data, drafted and critically revised the manuscript, and approved the final version to be published. JL made the data analysis and interpretation, critically revised the manuscript, and approved the final version to be published. BR, GB, RS, MG, SI, GB, BR, DC, SL, CA, and CV: made substantial contributions to the acquisition of the data, critically revised the manuscript, and approved the final version to be published. All authors agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflicts of interest
None declared.
Additional information
The ETIS Registry Investigators member names are listed in Acknowledgement section.
Rights and permissions
About this article
Cite this article
ter Schiphorst, A., Peres, R., Dargazanli, C. et al. Endovascular treatment of ischemic stroke due to isolated internal carotid artery occlusion: ETIS registry data analysis. J Neurol 269, 4383–4395 (2022). https://doi.org/10.1007/s00415-022-11078-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-022-11078-y