Abstract
Background and purpose
This study aimed to evaluate the efficacy of intra-arterial thrombectomy (IAT) and prognosis for acute ischaemic stroke patients with active cancer.
Methods
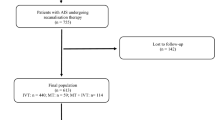
We retrospectively reviewed 253 patients who underwent IAT within 24 h after stroke onset between January 2012 and August 2017. We classified the patients into active cancer (n = 26) and control groups (n = 227) and compared clinical data. Primary outcome was a modified Rankin scale score at 3 months with ordinal logistic regression (shift analysis).
Results
Initial National Institutes of Health Stroke Scale (NIHSS) and rate of successful recanalisation did not differ between groups, but the active cancer group showed poor outcomes at 3 months on shift analysis (P = 0.001). The independent predictors of poor prognosis were age [adjusted common odds ratio (aOR) 1.03, 95% confidence interval (CI) 1.01–1.05], baseline NIHSS (aOR 1.14, 95% CI 1.09–1.19), baseline C-reactive protein level (aOR 1.14, 95% CI 1.03–1.25), any cerebral haemorrhage (aOR 1.92, 95% CI 1.21–3.06), and active cancer (aOR 2.35, 95% CI 1.05–5.25). Mortality at 90 days was 30.8% in the cancer group and 8.8% in the control group (P = 0.003).
Conclusions
Although baseline characteristics and recanalisation rate after IAT up to 24 h after stroke onset were similar between acute ischaemic stroke patients with active cancer and without any cancer, stroke-related death and short-term outcome were significantly poorer in patients with active cancer than the controls. Post-procedural haemorrhage and active cancer itself were independent predictors of a decrease in functional independence at 3 months.


Similar content being viewed by others
References
Grisold W, Oberndorfer S, Struhal W (2009) Stroke and cancer: a review. Acta Neurol Scand 119(1):1–16. https://doi.org/10.1111/j.1600-0404.2008.01059.x
Cronin KA, Lake AJ, Scott S, Sherman RL, Noone AM, Howlader N, Henley SJ, Anderson RN, Firth AU, Ma J, Kohler BA, Jemal A (2018) Annual Report to the Nation on the Status of Cancer, part I: National cancer statistics. Cancer 124(13):2785–2800. https://doi.org/10.1002/cncr.31551
Cappellari M, Carletti M, Micheletti N, Tomelleri G, Ajena D, Moretto G, Bovi P (2013) Intravenous alteplase for acute ischemic stroke in patients with current malignant neoplasm. J Neurol Sci 325(1–2):100–102. https://doi.org/10.1016/j.jns.2012.12.008
Masrur S, Abdullah AR, Smith EE, Hidalgo R, El-Ghandour A, Rordorf G, Schwamm LH (2011) Risk of thrombolytic therapy for acute ischemic stroke in patients with current malignancy. J Stroke Cerebrovasc Dis 20(2):124–130. https://doi.org/10.1016/j.jstrokecerebrovasdis.2009.10.010
Casado-Naranjo I, Calle ML, Falcon A, Serrano A, Portilla JC, Ramirez-Moreno JM (2011) Intravenous thrombolysis for acute stroke in patients with cancer. J Neurol Neurosurg Psychiatry 82(12):1404–1405. https://doi.org/10.1136/jnnp.2010.207472
Graber JJ, Nayak L, Deangelis LM (2012) Use of recombinant tissue plasminogen activator in cancer patients with acute stroke. J Neurooncol 107(3):571–573. https://doi.org/10.1007/s11060-011-0780-5
Powers WJ, Rabinstein AA, Ackerson T, Adeoye OM, Bambakidis NC, Becker K, Biller J, Brown M, Demaerschalk BM, Hoh B, Jauch EC, Kidwell CS, Leslie-Mazwi TM, Ovbiagele B, Scott PA, Sheth KN, Southerland AM, Summers DV, Tirschwell DL (2018) 2018 guidelines for the early management of patients with acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 49(3):e46–e110. https://doi.org/10.1161/str.0000000000000158
Matsumoto N, Fukuda H, Handa A, Kawasaki T, Kurosaki Y, Chin M, Yamagata S (2016) Histological examination of trousseau syndrome-related thrombus retrieved through acute endovascular thrombectomy: report of 2 cases. J Stroke Cerebrovasc Dis 25(12):e227–e230. https://doi.org/10.1016/j.jstrokecerebrovasdis.2016.08.041
Merkler AE, Marcus JR, Gupta A, Kishore SA, Leifer D, Patsalides A, DeAngelis LM, Navi BB (2014) Endovascular therapy for acute stroke in patients with cancer. Neurohospitalist 4(3):133–135. https://doi.org/10.1177/1941874413520509
Saver JL, Goyal M, Bonafe A, Diener HC, Levy EI, Pereira VM, Albers GW, Cognard C, Cohen DJ, Hacke W, Jansen O, Jovin TG, Mattle HP, Nogueira RG, Siddiqui AH, Yavagal DR, Baxter BW, Devlin TG, Lopes DK, Reddy VK, du Mesnil de Rochemont R, Singer OC, Jahan R, Investigators SP, (2015) Stent-retriever thrombectomy after intravenous t-PA vs. t-PA alone in stroke. N Engl J Med 372(24):2285–2295. https://doi.org/10.1056/NEJMoa1415061
Jovin TG, Chamorro A, Cobo E, de Miquel MA, Molina CA, Rovira A, San Roman L, Serena J, Abilleira S, Ribo M, Millan M, Urra X, Cardona P, Lopez-Cancio E, Tomasello A, Castano C, Blasco J, Aja L, Dorado L, Quesada H, Rubiera M, Hernandez-Perez M, Goyal M, Demchuk AM, von Kummer R, Gallofre M, Davalos A, Investigators RT (2015) Thrombectomy within 8 hours after symptom onset in ischemic stroke. N Engl J Med 372(24):2296–2306. https://doi.org/10.1056/NEJMoa1503780
Goyal M, Demchuk AM, Menon BK, Eesa M, Rempel JL, Thornton J, Roy D, Jovin TG, Willinsky RA, Sapkota BL, Dowlatshahi D, Frei DF, Kamal NR, Montanera WJ, Poppe AY, Ryckborst KJ, Silver FL, Shuaib A, Tampieri D, Williams D, Bang OY, Baxter BW, Burns PA, Choe H, Heo JH, Holmstedt CA, Jankowitz B, Kelly M, Linares G, Mandzia JL, Shankar J, Sohn SI, Swartz RH, Barber PA, Coutts SB, Smith EE, Morrish WF, Weill A, Subramaniam S, Mitha AP, Wong JH, Lowerison MW, Sajobi TT, Hill MD, Investigators ET (2015) Randomized assessment of rapid endovascular treatment of ischemic stroke. N Engl J Med 372(11):1019–1030. https://doi.org/10.1056/NEJMoa1414905
Campbell BC, Mitchell PJ, Kleinig TJ, Dewey HM, Churilov L, Yassi N, Yan B, Dowling RJ, Parsons MW, Oxley TJ, Wu TY, Brooks M, Simpson MA, Miteff F, Levi CR, Krause M, Harrington TJ, Faulder KC, Steinfort BS, Priglinger M, Ang T, Scroop R, Barber PA, McGuinness B, Wijeratne T, Phan TG, Chong W, Chandra RV, Bladin CF, Badve M, Rice H, de Villiers L, Ma H, Desmond PM, Donnan GA, Davis SM, Investigators E-I (2015) Endovascular therapy for ischemic stroke with perfusion-imaging selection. N Engl J Med 372(11):1009–1018. https://doi.org/10.1056/NEJMoa1414792
Berkhemer OA, Fransen PS, Beumer D, van den Berg LA, Lingsma HF, Yoo AJ, Schonewille WJ, Vos JA, Nederkoorn PJ, Wermer MJ, van Walderveen MA, Staals J, Hofmeijer J, van Oostayen JA, Lycklama a Nijeholt GJ, Boiten J, Brouwer PA, Emmer BJ, de Bruijn SF, van Dijk LC, Kappelle LJ, Lo RH, van Dijk EJ, de Vries J, de Kort PL, van Rooij WJ, van den Berg JS, van Hasselt BA, Aerden LA, Dallinga RJ, Visser MC, Bot JC, Vroomen PC, Eshghi O, Schreuder TH, Heijboer RJ, Keizer K, Tielbeek AV, den Hertog HM, Gerrits DG, van den Berg-Vos RM, Karas GB, Steyerberg EW, Flach HZ, Marquering HA, Sprengers ME, Jenniskens SF, Beenen LF, van den Berg R, Koudstaal PJ, van Zwam WH, Roos YB, van der Lugt A, van Oostenbrugge RJ, Majoie CB, Dippel DW, Investigators MC. A randomized trial of intraarterial treatment for acute ischemic stroke. N Engl J Med. 2015;372(1):11–20. https://doi.org/10.1056/NEJMoa1411587.
Cho KH, Kim JS, Kwon SU, Cho AH, Kang DW (2005) Significance of susceptibility vessel sign on T2*-weighted gradient echo imaging for identification of stroke subtypes. Stroke 36(11):2379–2383. https://doi.org/10.1161/01.STR.0000185932.73486.7a
Adams HP Jr, Bendixen BH, Kappelle LJ, Biller J, Love BB, Gordon DL, Marsh EE 3rd (1993) Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke 24(1):35–41
Saver JL, Gornbein J (2009) Treatment effects for which shift or binary analyses are advantageous in acute stroke trials. Neurology 72(15):1310–1315. https://doi.org/10.1212/01.wnl.0000341308.73506.b7
Zaidat OO, Yoo AJ, Khatri P, Tomsick TA, von Kummer R, Saver JL, Marks MP, Prabhakaran S, Kallmes DF, Fitzsimmons BF, Mocco J, Wardlaw JM, Barnwell SL, Jovin TG, Linfante I, Siddiqui AH, Alexander MJ, Hirsch JA, Wintermark M, Albers G, Woo HH, Heck DV, Lev M, Aviv R, Hacke W, Warach S, Broderick J, Derdeyn CP, Furlan A, Nogueira RG, Yavagal DR, Goyal M, Demchuk AM, Bendszus M, Liebeskind DS (2013) Recommendations on angiographic revascularization grading standards for acute ischemic stroke: a consensus statement. Stroke 44(9):2650–2663. https://doi.org/10.1161/strokeaha.113.001972
Fiorelli M, Bastianello S, von Kummer R, del Zoppo GJ, Larrue V, Lesaffre E, Ringleb AP, Lorenzano S, Manelfe C, Bozzao L (1999) Hemorrhagic transformation within 36 hours of a cerebral infarct: relationships with early clinical deterioration and 3-month outcome in the European Cooperative Acute Stroke Study I (ECASS I) cohort. Stroke 30(11):2280–2284
Zhang YY, Chan DK, Cordato D, Shen Q, Sheng AZ (2006) Stroke risk factor, pattern and outcome in patients with cancer. Acta Neurol Scand 114(6):378–383. https://doi.org/10.1111/j.1600-0404.2006.00709.x
Cutting S, Wettengel M, Conners JJ, Ouyang B, Busl K (2017) Three-month outcomes are poor in stroke patients with cancer despite acute stroke treatment. J Stroke Cerebrovasc Dis 26(4):809–815. https://doi.org/10.1016/j.jstrokecerebrovasdis.2016.10.021
Navi BB, Reiner AS, Kamel H, Iadecola C, Okin PM, Elkind MSV, Panageas KS, DeAngelis LM (2017) Risk of arterial thromboembolism in patients with cancer. J Am Coll Cardiol 70(8):926–938. https://doi.org/10.1016/j.jacc.2017.06.047
Murthy SB, Karanth S, Shah S, Shastri A, Rao CP, Bershad EM, Suarez JI (2013) Thrombolysis for acute ischemic stroke in patients with cancer: a population study. Stroke 44(12):3573–3576. https://doi.org/10.1161/STROKEAHA.113.003058
Sobolewski P, Brola W, Szczuchniak W, Fudala M, Sobota A (2015) Safety of intravenous thrombolysis for acute ischaemic stroke including concomitant neoplastic disease sufferers—experience from Poland. Int J Clin Pract 69(6):666–673. https://doi.org/10.1111/ijcp.12586
Desilles JP, Rouchaud A, Labreuche J, Meseguer E, Laissy JP, Serfaty JM, Lapergue B, Klein IF, Guidoux C, Cabrejo L, Sirimarco G, Lavallee PC, Schouman-Claeys E, Amarenco P, Mazighi M (2013) Blood-brain barrier disruption is associated with increased mortality after endovascular therapy. Neurology 80(9):844–851. https://doi.org/10.1212/WNL.0b013e31828406de
Lei C, Wu B, Liu M, Chen Y (2014) Asymptomatic hemorrhagic transformation after acute ischemic stroke: is it clinically innocuous? J Stroke Cerebrovasc Dis 23(10):2767–2772. https://doi.org/10.1016/j.jstrokecerebrovasdis.2014.06.024
Ghabaee M, Zandieh A, Mohebbi S, Fakhri M, Sadeghian H, Divani F, Amirifard H, Mousavi-Mirkala M, Ghaffarpour M (2014) Predictive ability of C-reactive protein for early mortality after ischemic stroke: comparison with NIHSS score. Acta Neurol Belg 114(1):41–45. https://doi.org/10.1007/s13760-013-0238-y
Pandey A, Shrivastava AK, Saxena K (2014) Neuron specific enolase and c-reactive protein levels in stroke and its subtypes: correlation with degree of disability. Neurochem Res 39(8):1426–1432. https://doi.org/10.1007/s11064-014-1328-9
VanGilder RL, Davidov DM, Stinehart KR, Huber JD, Turner RC, Wilson KS, Haney E, Davis SM, Chantler PD, Theeke L, Rosen CL, Crocco TJ, Gutmann L, Barr TL (2014) C-reactive protein and long-term ischemic stroke prognosis. J Clin Neurosci 21(4):547–553. https://doi.org/10.1016/j.jocn.2013.06.015
Nam KW, Kim CK, Kim TJ, An SJ, Oh K, Mo H, Kang MK, Han MK, Demchuk AM, Ko SB, Yoon BW (2017) Predictors of 30-day mortality and the risk of recurrent systemic thromboembolism in cancer patients suffering acute ischemic stroke. PLoS ONE 12(3):e0172793. https://doi.org/10.1371/journal.pone.0172793
Lee MJ, Chung JW, Ahn MJ, Kim S, Seok JM, Jang HM, Kim GM, Chung CS, Lee KH, Bang OY (2017) Hypercoagulability and mortality of patients with stroke and active cancer: the OASIS-CANCER study. J Stroke 19(1):77–87. https://doi.org/10.5853/jos.2016.00570
Jung S, Jung C, Hyoung Kim J, Se Choi B, Jung Bae Y, Sunwoo L, Geol Woo H, Young Chang J, Joon Kim B, Han MK, Bae HJ (2018) Procedural and clinical outcomes of endovascular recanalization therapy in patients with cancer-related stroke. Interv Neuroradiol 24(5):520–528. https://doi.org/10.1177/1591019918776207
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no conflicts of interest to report.
Ethical standards
This study was approved by Asan Medical Center institutional review board.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lee, D., Lee, D.H., Suh, D.C. et al. Intra-arterial thrombectomy for acute ischaemic stroke patients with active cancer. J Neurol 266, 2286–2293 (2019). https://doi.org/10.1007/s00415-019-09416-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-019-09416-8