Abstract
Introduction
Aspirin-exacerbated respiratory disease (AERD) refers to the combination of asthma rhinosinusitis and poliposis; ingestion of aspirin or other non-steroid anti-inflammatory drugs exacerbate asthma-like symptoms. The pathogenesis of AERD is unknown, and genetic and environmental factors contribute to the disease. Our objective is identifying polymorphisms associated with susceptibility in a Mexican mestizo population.
Methods
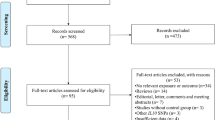
Primarily we performed custom Illumina goldengate array-based genotyping of 1512 SNPs, carefully selected from a variety of acute/chronic inflammatory lung conditions previously reported. Four SNPs in TRPM3 gene showed the lowest p-values (rs10780946, rs7025694, rs1889915, and rs7047645). We further selected rs10780946 and rs7025694 for validation using Taqman genotyping (n = 743; 288 AERD, 272 ATA, and 183 HC).
Results
rs10780946 showed association when compared between AERD and ATA groups under co-dominant (p = 0.006), dominant (p = 0.002), overdominant (p = 0.01), and log-additive (p = 0.03) genetic models. AERD showed increased heterozygous TC (rs10780946–rs7025694) haplotype compared to ATA and HC (p < 0.05). We could not confirm any association between rs7025694 and AERD.
Conclusion
rs10780946 TRPM3 polymorphism is associated with AERD susceptibility.




Similar content being viewed by others
References
Szczeklik A, Nizankowska E (2000) Clinical features and diagnosis of aspirin induced asthma. Thorax 55:S42–S44
Berges-Gimeno MP, Simon RA, Stevenson DD (2002) The natural history and clinical characteristics of aspirin-exacerbated respiratory disease. Ann Allergy Asthma Immunol 89:474–478
Jenkins C, Costello J, Hodge L (2004) Systematic review of prevalence of aspirin induced asthma and its implications for clinical practice. BMJ 328:434
Choi JH, Kim MA, Park HS (2014) An update on the pathogenesis of the upper airways in aspirin-exacerbated respiratory disease. Curr Opin Allergy Clin Immunol 14:1–6
Szczeklik A, Stevenson DD (2003) Aspirin-induced asthma: advances in pathogenesis, diagnosis, and management. J Allergy Clin Immunol 111:913–921
Narayanankutty A, Reséndiz-Hernández JM, Falfán-Valencia R et al (2013) Biochemical pathogenesis of aspirin exacerbated respiratory disease (AERD). Clin Biochem 46:566–578
Farooque SP, Lee TH (2009) Aspirin-sensitive respiratory disease. Annu Rev Physiol 71:465–487
Laidlaw TM, Cutler AJ, Kidder MS et al (2014) Prostaglandin E2 resistance in granulocytes from patients with aspirin-exacerbated respiratory disease. J Allergy Clin Immunol 133:1692–1701
Mastalerz L, Sanak M, Gawlewicz-Mroczka A et al (2008) Prostaglandin E2 systemic production in patients with asthma with and without aspirin hypersensitivity. Thorax 63:27–34
Laidlaw TM, Kidder MS, Bhattacharyya N et al (2012) Cysteinyl leukotriene overproduction in aspirin-exacerbated respiratory disease is driven by platelet-adherent leukocytes. Blood 119:3790–3798
Sestini P, Armetti L, Gambaro G et al (1996) Inhaled PGE2 prevents aspirin-induced bronchoconstriction and urinary LTE4 excretion in aspirin-sensitive asthma. Am J Respir Crit Care Med 153:572–575
Stevenson DD, Szczeklik A (2006) Clinical and pathologic perspectives on aspirin sensitivity and asthma. J Allergy Clin Immunol 118:773–786
Steinke JW, Liu L, Huyett P et al (2013) Prominent role of IFN-γ in patients with aspirin-exacerbated respiratory disease. J Allergy Clin Immunol 132:856–865
Park HS (1995) Early and late onset asthmatic responses following lysine-aspirin inhalation in aspirin-sensitive asthmatic patients. Clin Exp Allergy 25:38–40
Crapo RO, Casaburi R, Coates AL et al (2000) Guidelines for methacholine and exercise challenge testing-1999. This official statement of the American Thoracic Society was adopted by the ATS Board of Directors, July 1999. Am J Respir Crit Care Med 161:309–329
Adler AJ, Wiley GB, Gaffney PM (2013) Infinium assay for large-scale SNP genotyping applications. J Vis Exp 81:e50683
Purcell S, Neale B, Todd-Brown K et al (2007) PLINK: a tool set for whole-genome association and population-based linkage analyses. Am J Hum Genet 81:559–575
Solé X, Guinó E, Valls J et al (2006) SNPStats: a web tool for the analysis of association studies. Bioinformatics 22:1928–1929
Laidlaw TM, Boyce JA (2015) Platelets in patients with aspirin-exacerbated respiratory disease. J Allergy Clin Immunol 135:1407–1414
Cowburn AS, Sladek K, Soja J, Adamek L et al (1998) Overexpression of leukotriene C4 synthase in bronchial biopsies from patients with aspirin-intolerant asthma. J Clin Invest 101:834–846
Kamil A, Ghaffar O, Lavigne F et al (1998) Comparison of inflammatory cell profile and Th2 cytokine expression in the ethmoid sinuses, maxillary sinuses, and turbinates of atopic subjects with chronic sinusitis. Otolaryngol Head Neck Surg 118:804–809
Payne SC, Early SB, Huyett P et al (2011) Evidence for distinct histologic profile of nasal polyps with and without eosinophilia. Laryngoscope 121:2262–2267
Fischer AR, Rosenberg MA, Lilly CM et al (1994) Direct evidence for a role of the mast cell in the nasal response to aspirin in aspirin-sensitive asthma. J Allergy Clin Immunol 94:1046–1056
Sladek K, Szczeklik A (1993) Cysteinyl leukotrienes overproduction and mast cell activation in aspirin-provoked bronchospasm in asthma. Eur Respir J 6:391–399
Grimm C, Kraft R, Sauerbruch S et al (2003) Molecular and functional characterization of the melastatin-related cation channel TRPM3. J Biol Chem 278:21493–21501
Grimm C, Kraft R, Schultz G et al (2005) Activation of the melastatin-related cation channel TRPM3 by D-erythro-sphingosine. Mol Pharmacol 67:798–805
Freichel M, Almering J, Tsvilovskyy V (2012) The Role of TRP Proteins in Mast Cells. Front Immunol 3:150
Humphray SJ, Oliver K, Hunt AR et al (2004) DNA sequence and analysis of human chromosome 9. Nature 429:369–374
Steinke JW, Negri J, Liu L et al (2014) Aspirin activation of eosinophils and mast cells: implications in the pathogenesis of aspirin-exacerbated respiratory disease. J Immunol 193:41–47
Telleria JJ, Blanco-Quiros A, Varillas D et al (2008) ALOX5 promoter genotype and response to montelukast in moderate persistent asthma. Respir Med 102:857–861
Acknowledgments
This paper constitutes a partial fulfillment of the Graduate Program in Doctorado en Investigación en Medicina of the Instituto Politécnico Nacional (IPN) for AN. A Narayanankutty acknowledges the scholarship and financial support provided by the National Council of Science and Technology (CONACyT) # 265560.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
None.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Narayanankutty, A., Palma-Lara, I., Pavón-Romero, G. et al. Association of TRPM3 Polymorphism (rs10780946) and Aspirin-Exacerbated Respiratory Disease (AERD). Lung 194, 273–279 (2016). https://doi.org/10.1007/s00408-016-9852-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-016-9852-9