Abstract
Objective
Data are sparse regarding the prevalence of pulmonary hypertension (PH) in obstructive sleep apnoea (OSA) patients without COPD and clinically manifest cardiac diseases and the role of continuous positive airway pressure (CPAP) and Uvulopalatopharyngoplasty (UPPP) in normalizing this parameter.
Patients/Methods
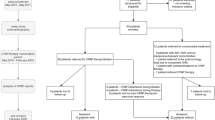
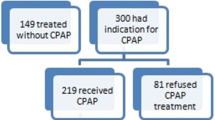
We studied 75 consecutive OSA patients, 55 of them men, using transthoracic echocardiography. A mild PH [pulmonary artery pressure (PAPs) 38.2 ± 6.8] was found in 25 subjects (prevalence 33 %). These patients were divided into two groups: group 1A (n = 17), those treated with CPAP, and group 1B (n = 8), those who have the indication for a UPPP. We scheduled a follow-up at 3, 6 and 9 months. During follow-up, we performed echocardiography, measurement of anthropometric parameters (BMI, neck and waist–hip circumference), and of biochemical parameters (uric acid, fasting glucose, cholesterol, triglycerides) and blood pressure.
Results
Patients with PH had a higher BMI: 32 ± 6 versus 29 ± 4 (p < 0.001) and NC: 39.8 ± 4.76 versus 37.14 ± 3.49 (p = 0.003), were predominantly men (72 %) and older: 64 ± 20 versus 55 ± 16 (p = 0.025) and had a significantly higher value of uric acid: 7.91 ± 2.35 versus 6.56 ± 1.31 (p = 0.003). We found a positive correlation between PH and BMI (r = 0.456; p < 0.001) and between uric acidic and PH (r = 0.636; p < 0.001). PAPs significantly changed, from 39.8 ± 4.1 to 27.1 ± 4, to 25.2 ± 3.1 and to 22.2 ± 3 mmHg (CI 95 %; 15.09–20.11; p < 0.001) in group 1A and from 39.5 ± 5.1 to 23.4 ± 3.2, to 23.0 ± 3.1 and to 21.9 ± 2.9 mmHg (CI 95 %; 13.15–22.05; p < 0.001) in group 1B (difference between the groups p = 0.12).
Conclusions
PH was frequent in OSA patients and normalized after 6 months with both CPAP and UPPP. A similar trend was noted in diastolic blood pressure.



Similar content being viewed by others
References
Atwood CW, Mc Crory D, Garcia JGN et al (2004) Pulmonary artery hypertension and sleep disordered breathing. ACCP evidence based clinical practice guidelines. Chest 126:72S–77S
Minai OA, Ricaurte B, Kaw R et al (2009) Frequency and impact of pulmonary hypertension in patients with obstructive sleep apnea syndrome. Am J Cardiol 104:1300–1306
Naeije R, Torbicki A (1995) More on the non invasive diagnosis of pulmonary hypertension: Doppler echocardiography revisited. Eur Respir J 8:1445–1449
Sajkov D, Wang T, Saunders NA et al (2002) Continuous positive airway pressure treatment improves pulmonary hemodynamics in patients with obstructive sleep apnea. Am J Respir Crit Care Med 165:152–158
Gordon P, Sanders MH (2005) Positive airway pressure therapy for obstructive sleep apnoea/hypopnoea syndrome. Thorax 60:68–75
Sun X, Luo J, Xiao J (2014) Continuous positive airway pressure is associated with a decrease in pulmonary artery hypertension in patients with OSA: a meta-analysis. Respirology 19:670–674
Braga A, Grechi TH, Eckeli A et al (2013) Predictors of UPPP success in the treatment of obstructive sleep apnoea syndrome. Sleep Med 14:1266–1271
Coccagna G, Pollini A, Provini F (2006) Cardiovascular disorders and obstructive sleep apnoea. Clin Exp Hypertens 28:217–224
Bady E, Achkar A, Pascal S et al (2000) Pulmonary arterial hypertension in patients with sleep apnoea syndrome. Thorax 55:934–939
Alchanatis M, Tourkohoriti G, Kakouros S et al (2001) Daytime pulmonary hypertension in patients with obstructive sleep apnea. The effect of continuous positive airway pressure on pulmonary hemodynamics. Respiration 68:566–572
Arias MA, Garcia Rio F, Alfonso Fernandez A et al (2006) Pulmonary hypertension in obstructive sleep apnoea: effects of continuous positive airway pressure. A randomized control cross-over study. Eur Heart J 27:1106–1113
Minic M, Granton JT, Ryan CM (2014) Sleep disordered breathing in group 1 pulmonary arterial hypertension. J Clin Sleep Med 10:277–283
Bhattacharyya N (2014) Revisits and readmissions following ambulatory uvulopalatopharyngoplasty. Laryngoscope. doi:10.1002/lary.24706
Varendh M, Berg S, Andersson M (2012) Long term follow-up of patients operated with UPPP from 1985 to 1991. Respir Med 106:1788–1793
Prudon B, Roddy E, Stradling JR et al (2013) Serum urate levels are unchanged with CPAP therapy for OSA: a randomized controlled trial. Sleep Med 14:1419–1421
Kanbay A, Inou H, Solak Y et al (2014) Uric acid as a potential mediator of cardiovascular morbidity in obstructive sleep apnea syndrome. Eur J Intern Med 25:471–476
Conflict of interest
We have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Marvisi, M., Vento, M.G., Balzarini, L. et al. Continuous Positive Airways Pressure and Uvulopalatopharyngoplasty Improves Pulmonary Hypertension in Patients with Obstructive Sleep Apnoea. Lung 193, 269–274 (2015). https://doi.org/10.1007/s00408-015-9694-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-015-9694-x