Abstract
Purpose
Voice abuse is known to be a common risk factor of voice disorders and prolonged; high-intensity phonation has been shown to damage the vocal fold epithelium. We aim to evaluate the effects of phonation on the integrity and barrier function of vocal fold epithelium using a porcine laryngeal model.
Methods
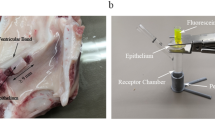
Ex vivo porcine larynges were phonated at low intensity or high intensity for 15, 30, or 60 min within 4 h after harvest. Vocal fold epithelium was visualized using transmission electron microscopy (TEM). The barrier function of vocal fold epithelium was evaluated by measuring the permeability to model molecules, fluorescein (376 Da), and fluorescein isothiocyanate (FITC)–dextrans of 4000 and 10,000 Da (FD4, FD10), in a Franz diffusing cell.
Results
Cell death and dilated intercellular space after phonation were observed using TEM. Thickness of vocal fold epithelium was significantly reduced after low-intensity phonation for 30 and 60 min and high-intensity phonation for 15, 30, and 60 min. Epithelial permeability to fluorescein was significantly increased after low-intensity phonation for 30 and 60 min, and high-intensity phonation. Permeability to FD4 was significantly increased after high-intensity phonation for 30 and 60 min. Phonation did not alter the permeability to FD10 significantly.
Conclusion
Long-duration phonation destroys the integrity and barrier function of vocal fold epithelium. These effects likely make vocal folds more vulnerable to other environmental irritants, such as tobacco smoke, reflux components, allergens, and inhaled pollutants. Destroyed barrier function may be an important factor in the pathogenesis of voice lesions related to voice abuse.





Similar content being viewed by others
References
Nerurkar NK, Kapre GM, Kothari NN (2016) Correlation between personality type and vocal pathology: a nonrandomized case control study. Laryngoscope 126(9):2063–2066. https://doi.org/10.1002/lary.25810
Altman KW (2007) Vocal fold masses. Otolaryng Clin N Am 40(5):1091–1108. https://doi.org/10.1016/j.otc.2007.05.011
Jiang JJ, Shah AG, Hess MM, Verdolini K, Banzali FM Jr, Hanson DG (2001) Vocal fold impact stress analysis. J Voice 15(1):4–14. https://doi.org/10.1016/S0892-1997(01)00002-9
Gray S, Titze I (1988) Histologic investigation of hyperphonated canine vocal cords. Ann Otol Rhinol Laryngol 97(4 Pt 1):381–388. https://doi.org/10.1177/000348948809700410
Kojima T, Valenzuela CV, Novaleski CK, Van Deusen M, Mitchell JR, Garrett CG, Sivasankar MP, Rousseau B (2014) Effects of phonation time and magnitude dose on vocal fold epithelial genes, barrier integrity, and function. Laryngoscope 124(12):2770–2778. https://doi.org/10.1002/lary.24827
Kojima T, Van Deusen M, Jerome WG, Garrett CG, Sivasankar MP, Novaleski CK, Rousseau B (2014) Quantification of acute vocal fold epithelial surface damage with increasing time and magnitude doses of vibration exposure. Plos One 9(3):e91615. https://doi.org/10.1371/journal.pone.0091615
Novaleski CK, Kimball EE, Mizuta M, Rousseau B (2016) Acute exposure to vibration is an apoptosis-inducing stimulus in the vocal fold epithelium. Tissue Cell 48(5):407–416. https://doi.org/10.1016/j.tice.2016.08.007
Cipriani NA, Martin DE, Corey JP, Portugal L, Caballero N, Lester R, Anthony B, Taxy JB (2011) The clinicopathologic spectrum of benign mass lesions of the vocal fold due to vocal abuse. Int J Surg Pathol 19(5):583–587. https://doi.org/10.1177/1066896911411480
Wallis L, Jackson-Menaldi C, Holland W, Giraldo A (2004) Vocal fold nodule vs. vocal fold polyp: answer from surgical pathologist and voice pathologist point of view. J Voice 18(1):125–129. https://doi.org/10.1016/j.jvoice.2003.07.003
Van Stan JH, Mehta DD, Zeitels SM, Burns JA, Barbu AM, Hillman RE (2015) Average ambulatory measures of sound pressure level, fundamental frequency, and vocal dose do not differ between adult females with phonotraumatic lesions and matched control subjects. Ann Otol Rhinol Laryngol 124(11):864–874. https://doi.org/10.1177/0003489415589363
Martins RH, do Amaral HA, Tavares EL, Martins MG, Goncalves TM, Dias NH (2016) Voice disorders: etiology and diagnosis. J Voice 30(6):761 e1–761 e9. https://doi.org/10.1016/j.jvoice.2015.09.017
Garcia Alvarez CD, Campos Banales ME, Lopez Campos D, Rivero J, Perez Pinero B, Lopez Aguado D (1999) Polyps, nodules, and Reinke edema. An epidemiological and histopathological study. Acta Otorrinolaringol Esp 50(6):443–447
Levendoski EE, Leydon C, Thibeault SL (2014) Vocal fold epithelial barrier in health and injury: a research review. J Speech Lang Hear Res 57(5):1679–1691. https://doi.org/10.1044/2014_JSLHR-S-13-0283
Martins RH, Defaveri J, Custodio Domingues MA, de Albuquerque ESR, Fabro A (2010) Vocal fold nodules: morphological and immunohistochemical investigations. J Voice 24(5):531–539. https://doi.org/10.1016/j.jvoice.2009.01.002
Dikkers FG, Hulstaert CE, Oosterbaan JA, Cervera-Paz FJ (1993) Ultrastructural changes of the basement membrane zone in benign lesions of the vocal folds. Acta Otolaryngol 113(1):98–101
Rousseau B, Suehiro A, Echemendia N, Sivasankar M (2011) Raised intensity phonation compromises vocal fold epithelial barrier integrity. Laryngoscope 121(2):346–351. https://doi.org/10.1002/lary.21364
Jiang JJ, Raviv JR, Hanson DG (2001) Comparison of the phonation-related structures among pig, dog, white-tailed deer, and human larynges. Ann Otol Rhinol Laryngol 110(12):1120–1125. doi:https://doi.org/10.1177/000348940111001207
Sivasankar M, Erickson E, Rosenblatt M, Branski RC (2010) Hypertonic challenge to porcine vocal folds: effects on epithelial barrier function. Otolaryngol Head Neck Surg 142(1):79–84. https://doi.org/10.1016/j.otohns.2009.09.011
Erickson-Levendoski E, Sivasankar MP (2012) Role for ion transport in porcine vocal fold epithelial defense to acid challenge. Otolaryngol Head Neck Surg 146(2):272–278. https://doi.org/10.1177/0194599811428273
Jiang JJ, Titze IR (1993) A methodological study of hemilaryngeal phonation. Laryngoscope 103(8):872–882. https://doi.org/10.1288/00005537-199308000-00008
Zhang Y, Reynders WJ, Jiang JJ, Tateya I (2007) Determination of phonation instability pressure and phonation pressure range in excised larynges. J Speech Lang Hear Res 50(3):611–620. https://doi.org/10.1044/1092-4388(2007/043)
Li L, Zhang Y, Calawerts W, Jiang JJ (2016) Vibratory dynamics of four types of excised larynx phonations. J Voice 30(6):649–655. https://doi.org/10.1016/j.jvoice.2015.08.012
Zhang Y, Krausert CR, Kelly MP, Jiang JJ (2009) Typing vocal fold vibratory patterns in excised larynx experiments via digital kymography. Ann Otol Rhinol Laryngol 118(8):598–605
Farre R, van Malenstein H, De Vos R, Geboes K, Depoortere I, Vanden Berghe P, Fornari F, Blondeau K, Mertens V, Tack J, Sifrim D (2008) Short exposure of oesophageal mucosa to bile acids, both in acidic and weakly acidic conditions, can impair mucosal integrity and provoke dilated intercellular spaces. Gut 57(10):1366–1374. https://doi.org/10.1136/gut.2007.141804
Vidyasagar S, MacGregor G (2016) Ussing chamber technique to measure intestinal epithelial permeability. Methods Mol Biol 1422:49–61. https://doi.org/10.1007/978-1-4939-3603-8_6
Rubio L, Alonso C, Lopez O, Rodriguez G, Coderch L, Notario J, de la Maza A, Parra JL (2011) Barrier function of intact and impaired skin: percutaneous penetration of caffeine and salicylic acid. Int J Dermatol 50(7):881–889. https://doi.org/10.1111/j.1365-4632.2010.04819.x
Chen X, Oshima T, Tomita T, Fukui H, Watari J, Matsumoto T, Miwa H (2011) Acidic bile salts modulate the squamous epithelial barrier function by modulating tight junction proteins. Am J Physiol Gastrointest Liver Physiol 301(2):G203-209. https://doi.org/10.1152/ajpgi.00096.2011
Caon T, Simoes CM (2011) Effect of freezing and type of mucosa on ex vivo drug permeability parameters. AAPS PharmSciTech 12(2):587–592. https://doi.org/10.1208/s12249-011-9621-2
Gill GA, Buda A, Moorghen M, Dettmar PW, Pignatelli M (2005) Characterisation of adherens and tight junctional molecules in normal animal larynx; determining a suitable model for studying molecular abnormalities in human laryngopharyngeal reflux. J Clin Pathol 58(12):1265–1270. https://doi.org/10.1136/jcp.2004.016972
Hahn MS, Kobler JB, Starcher BC, Zeitels SM, Langer R (2006) Quantitative and comparative studies of the vocal fold extracellular matrix. I: Elastic fibers and hyaluronic acid. Ann Otol Rhinol Laryngol 115(2):156–164. https://doi.org/10.1177/000348940611500213
Levendoski EE, Sivasankar MP (2014) Vocal fold ion transport and mucin expression following acrolein exposure. J Membr Biol 247(5):441–450. https://doi.org/10.1007/s00232-014-9651-2
Bulmer DM, Ali MS, Brownlee IA, Dettmar PW, Pearson JP (2010) Laryngeal mucosa: its susceptibility to damage by acid and pepsin. Laryngoscope 120(4):777–782. https://doi.org/10.1002/lary.20665
Jiang JJ, Titze IR (1994) Measurement of vocal fold intraglottal pressure and impact stress. J Voice 8(2):132–144
Ozawa M, Iwadate K, Matsumoto S, Asakura K, Ochiai E, Maebashi K (2013) The effect of temperature on the mechanical aspects of rigor mortis in a liquid paraffin model. Leg Med 15(6):293–297. https://doi.org/10.1016/j.legalmed.2013.08.001
Oshizaka T, Todo H, Sugibayashi K (2012) Effect of direction (epidermis-to-dermis and dermis-to-epidermis) on the permeation of several chemical compounds through full-thickness skin and stripped skin. Pharm Res 29(9):2477–2488. https://doi.org/10.1007/s11095-012-0777-6
Gao XC, Qi HP, Bai JH, Huang L, Cui H (2014) Effects of oleic acid on the corneal permeability of compounds and evaluation of its ocular irritation of rabbit eyes. Curr Eye Res 39(12):1161–1168. https://doi.org/10.3109/02713683.2014.904361
Tobey NA, Hosseini SS, Argote CM, Dobrucali AM, Awayda MS, Orlando RC (2004) Dilated intercellular spaces and shunt permeability in nonerosive acid-damaged esophageal epithelium. Am J Gastroenterol 99(1):13–22. https://doi.org/10.1046/j.1572-0241.2003.04018.x
Kuhn J, Toohill RJ, Ulualp SO, Kulpa J, Hofmann C, Arndorfer R, Shaker R (1998) Pharyngeal acid reflux events in patients with vocal cord nodules. Laryngoscope 108(8):1146–1149. doi:https://doi.org/10.1097/00005537-199808000-00008
Chung JH, Tae K, Lee YS, Jeong JH, Cho SH, Kim KR, Park CW, Han DS (2009) The significance of laryngopharyngeal reflux in benign vocal mucosal lesions. Otolaryngol Head Neck 141(3):369–373. https://doi.org/10.1016/j.otohns.2009.05.033
Marcotullio D, Magliulo G, Pezone T (2002) Reinke’s edema and risk factors: clinical and histopathologic aspects. Am J Otolaryngol 23(2):81–84. https://doi.org/10.1053/ajot.2002.30961
Roth D, Ferguson BJ (2010) Vocal allergy: recent advances in understanding the role of allergy in dysphonia. Curr Opin Otolaryngol Head Neck Surg 18(3):176–181. https://doi.org/10.1097/MOO.0b013e32833952af
Park B, Choi HG (2016) Association between asthma and dysphonia: a population-based study. J Asthma 53(7):679–683. https://doi.org/10.3109/02770903.2016.1140181
Lauriello M, Angelone AM, Businco LD, Passali D, Bellussi LM, Passali FM (2011) Correlation between female sex and allergy was significant in patients presenting with dysphonia. Acta Otorhinolaryngol Ital 31(3):161–166
Karkos PD, McCormick M (2009) The etiology of vocal fold nodules in adults. Curr Opin Otolaryngol Head Neck Surg 17(6):420–423. https://doi.org/10.1097/MOO.0b013e328331a7f8
Pralong JA, Cartier A, Vandenplas O, Labrecque M (2012) Occupational asthma: new low-molecular-weight causal agents, 2000–2010. J Allergy. https://doi.org/10.1155/2012/597306
Acknowledgements
This work was supported by the grant from the National Natural Science Foundation of China, Project 81329001.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interests to disclose.
Ethical approval
This article does not contain any studies with live animals or human participants performed by any of the authors. Tissue was procured from animal cadavers and sacrificed for reasons unrelated to this research.
Rights and permissions
About this article
Cite this article
Zhang, C., Paddock, K., Chou, A. et al. Prolonged phonation impairs the integrity and barrier function of porcine vocal fold epithelium: a preliminary study. Eur Arch Otorhinolaryngol 275, 1547–1556 (2018). https://doi.org/10.1007/s00405-018-4973-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-018-4973-9