Abstract
Objectives
To evaluate the international literature for studies reporting outcomes for obstructive sleep apnea (OSA) in children undergoing isolated tongue surgeries.
Methods
Two authors searched from inception through November 14, 2016 in four databases including PubMed/MEDLINE.
Results
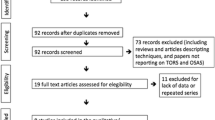
351 studies were screened. Eleven studies (116 children) met criteria. Most children were syndromic and had craniofacial disorders, co-morbidities, or other serious medical issues. Surgeries included base-of-tongue (BOT) reduction (n = 114), tongue suspension (n = 1), and hypoglossal nerve stimulation (n = 1). The pre- and post-BOT reduction surgeries decreased apnea–hypopnea index (AHI) from a mean (M) and standard deviation (SD) of 16.9 ± 12.2/h to 8.7 ± 10.6/h (48.5% reduction) in 114 patients. Random effects modeling (109 patients) demonstrated a standardized mean difference for AHI of −0.78 (large magnitude of effect) [95% CI −1.06, −0.51], p value <0.00001. For BOT surgery in 53 non-syndromic children, the AHI decreased 59.2% from 14.0 ± 11.4 to 5.7 ± 6.7/h, while in 55 syndromic children, the AHI decreased 40.0% from 20.5 ± 19.1 to 12.3 ± 18.2/h. BOT reduction improved lowest oxygen saturation from M ± SD of 84.7 ± 7.4–87.9 ± 6.5% in 113 patients. Hypoglossal nerve stimulation and tongue-base suspension are limited to case reports.
Conclusions
Most children undergoing tongue surgeries in the literature were syndromic and had craniofacial disorders, co-morbidities, or other serious medical issues. Children with a body mass index <25 kg/m2 and non-syndromic children have had the most improvement in AHI. The specific type of surgery must be tailored to the patient. Patients with co-morbidities should undergo treatment in centers that are equipped to provide appropriate perioperative care.



Similar content being viewed by others
References
Brietzke SE, Gallagher D (2006) The effectiveness of tonsillectomy and adenoidectomy in the treatment of pediatric obstructive sleep apnea/hypopnea syndrome: a meta-analysis. Otolaryngol Head Neck Surg 134:979–984
Guilleminault C, Li K, Quo S, Inouye RN (2004) A prospective study on the surgical outcomes of children with sleep-disordered breathing. Sleep 27:95–100
Villa MP, Malagola C, Pagani J et al (2007) Rapid maxillary expansion in children with obstructive sleep apnea syndrome: 12-month follow-up. Sleep Med 8:128–134
Chan DK, Jan TA, Koltai PJ (2012) Effect of obesity and medical comorbidities on outcomes after adjunct surgery for obstructive sleep apnea in cases of adenotonsillectomy failure. Arch Otolaryngol Head Neck Surg 138:891–896
Camacho M, Dunn B, Torre C et al (2016) Supraglottoplasty for laryngomalacia with obstructive sleep apnea: a systematic review and meta-analysis. Laryngoscope 126:1246–1255
Camacho M, Certal V, Abdullatif J et al (2015) Myofunctional therapy to treat obstructive sleep apnea: a systematic review and meta-analysis. Sleep 38:669–675
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6:e1000097
Camacho M, Noller MW, Zaghi S et al (2017) Tongue-lip adhesion and tongue repositioning for obstructive sleep apnoea in Pierre Robin sequence: a systematic review and meta-analysis. J Laryngol Otol 1–6. doi:10.1017/S0022215117000056
Methods for development of NICE public health guidance (2009) National Institute for Health and Clinical Excellence, London
Cohen J (1988) Statistical power analysis for the behavioral sciences. Erlbaum, Hillsdale
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ (Clinical research ed) 327:557–560
Lau J, Ioannidis JP, Schmid CH (1997) Quantitative synthesis in systematic reviews. Ann Intern Med 127:820–826
Abdel-Aziz M, Ibrahim N, Ahmed A, El-Hamamsy M, Abdel-Khalik MI, El-Hoshy H (2011) Lingual tonsils hypertrophy; a cause of obstructive sleep apnea in children after adenotonsillectomy: operative problems and management. Int J Pediatr Otorhinolaryngol 75:1127–1131
Acar GO, Cansz H, Duman C, Oz B, Cigerciogullar E (2011) Excessive reactive lymphoid hyperplasia in a child with persistent obstructive sleep apnea despite previous tonsillectomy and adenoidectomy. J Craniofac Surg 22:1413–1415
Babademez MA, Yorubulut M, Yurekli MF et al (2011) Comparison of minimally invasive techniques in tongue base surgery in patients with obstructive sleep apnea. Otolaryngol Head Neck Surg 145:858–864
Barakate M, Havas T (2008) Lingual tonsillectomy: a review of 5 years experience and evolution of surgical technique. Otolaryngol Head Neck Surg 139:222–227
Breugem CC, Olesen PR, Fitzpatrick DG, Courtemanche DJ (2008) Subperiosteal release of the floor of the mouth in airway management in Pierre Robin sequence. J Craniofac Surg 19:609–615
Burstein FD, Cohen SR, Scott PH, Teague GR, Montgomery GL, Kattos AV (1995) Surgical therapy for severe refractory sleep apnea in infants and children: application of the airway zone concept. Plast Reconstr Surg 96:34–41
Caouette-Laberge L, Borsuk DE, Bortoluzzi PA (2012) Subperiosteal release of the floor of the mouth to correct airway obstruction in pierre robin sequence: review of 31 cases. Cleft Palate-Craniofac J 49:14–20
Caouette-Laberge L, Plamondon C, Larocque Y (1996) Subperiosteal release of the floor of the mouth in Pierre Robin sequence: experience with 12 cases. Cleft Palate-Craniofac J 33:468–472
Cheng AT, Corke M, Loughran-Fowlds A, Birman C, Hayward P, Waters KA (2011) Distraction osteogenesis and glossopexy for Robin sequence with airway obstruction. ANZ J Surg 81:320–325
Conache ID, Meikle D, O’Brien C (2002) Tracheostomy, lingular tonsillectomy and sleep-related breathing disorders. Br J Anaesth 88:724–726
Delorme RP, Larocque Y, Caouette-Laberge L (1989) Innovative surgical approach for the Pierre Robin anomalad: subperiosteal release of the floor of the mouth musculature. Plast Reconstr Surg 83:960–964 (discussion 965–966)
Diercks GR, Keamy D, Kinane TB et al (2016) Hypoglossal nerve stimulator implantation in an adolescent with down syndrome and sleep apnea. Pediatrics 137(5):pii: e20153663. doi:10.1542/peds.2015-3663
Dudkiewicz Z, Sekula E, Nielepiec-Jalosinska A (2000) Gastroesophageal reflux in Pierre Robin sequence—early surgical treatment. Cleft Palate-Craniofac J 37:205–208
Eskiizmir G (2010) Lingual tonsillectomy for the management of persistent obstructive sleep apnea after adenotonsillectomy in children. Otolaryngol Head Neck Surg 142:301
Faye-Lund H, Djupesland G, Lyberg T (1992) Glossopexia—evaluation of a new surgical method for treating obstructive sleep apnea syndrome. Acta Oto-laryngologica Supplementum 492:46–49
Flores RL, Tholpady SS, Sati S et al (2014) The surgical correction of Pierre Robin sequence: mandibular distraction osteogenesis versus tongue-lip adhesion. Plast Reconstr Surg 133:1433–1439
Freed G, Pearlman MA, Brown AS, Barot LR (1988) Polysomnographic indications for surgical intervention in Pierre Robin sequence: acute airway management and follow-up studies after repair and take-down of tongue-lip adhesion. Cleft Palate J 25:151–155.
Genta PR, Eckert DJ, Gregorio MG et al (2011) Critical closing pressure during midazolam-induced sleep. J Appl Physiol (1985) 111:1315–1322
Greathouse ST, Costa M, Ferrera A et al (2016) The surgical treatment of robin sequence. Ann Plast Surg 77(4):416–419. doi:10.1097/SAP.0000000000000630
Guimaraes CV, Kalra M, Donnelly LF et al (2008) The frequency of lingual tonsil enlargement in obese children. AJR 190:973–975
Hartzell LD, Guillory RM, Munson PD, Dunham AK, Bower CM, Richter GT (2013) Tongue base suspension in children with cerebral palsy and obstructive sleep apnea. Int J Pediatr Otorhinolaryngol 77:534–537
Hwang MS, Salapatas AM, Yalamanchali S, Joseph NJ, Friedman M (2015) Factors associated with hypertrophy of the lingual tonsils. Otolaryngol Head Neck Surg 152:851–855
Ingram DG, Ruiz A, Friedman NR (2015) Friedman tongue position: age distribution and relationship to sleep-disordered breathing. Int J Pediatr Otorhinolaryngol 79:666–670
Kezirian EJ, Powell NB, Riley RW, Hester JE (2005) Incidence of complications in radiofrequency treatment of the upper airway. Laryngoscope 115:1298–1304
Kluszynski BA, Matt BH (2006) Lingual tonsillectomy in a child with obstructive sleep apnea: a novel technique. Laryngoscope 116:668–669
Krespi YP, Har-El G, Levine TM, Ossoff RH, Wurster CF, Paulsen JW (1989) Laser lingual tonsillectomy. Laryngoscope 99:131–135
Leonardis RL, Duvvuri U, Mehta D (2013) Transoral robotic-assisted lingual tonsillectomy in the pediatric population. JAMA Otolaryngol Head Neck Surg 139:1032–1036
Lin AC, Koltai PJ (2009) Persistent pediatric obstructive sleep apnea and lingual tonsillectomy. Otolaryngol Head Neck Surg 141:81–85
Linz A, Bacher M, Kagan KO, Buchenau W, Arand J, Poets CF (2011) [Pierre Robin Sequence: interdisciplinary treatment after prenatal diagnosis]. Z Geburtshilfe Neonatol 215:105–108
Manickam PV, Shott SR, Boss EF et al (2016) Systematic review of site of obstruction identification and non-CPAP treatment options for children with persistent pediatric obstructive sleep apnea. Laryngoscope 126:491–500
Maturo SC, Hartnick CJ (2012) Pediatric lingual tonsillectomy. Adv Otorhinolaryngol 73:109–111
Maturo SC, Mair EA (2006) Submucosal minimally invasive lingual excision: an effective, novel surgery for pediatric tongue base reduction. Ann Otol Rhinol Laryngol 115:624–630
Mixter RC, Ewanowski SJ, Carson LV (1993) Central tongue reduction for macroglossia. Plast Reconstr Surg 91:1159–1162
Nakazawa K, Ikeda D, Ishikawa S, Makita K (2003) A case of difficult airway due to lingual tonsillar hypertrophy in a patient with Down’s syndrome. Anesth Analg 97:704–705
Nishimura T, Morishima N, Hasegawa S, Shibata N, Iwanaga K, Yagisawa M (1996) Effect of surgery on obstructive sleep apnea. Acta Otolaryngol Suppl 523:231–233
Oomen KPQ, Modi VK (2014) Epiglottopexy with and without lingual tonsillectomy. Laryngoscope 124:1019–1022
Paludetti G, Zampino G, Della Marca G, Di Girolamo S, Scarano E, Rigante M (2003) The tongue-base suspension using Repose™ bone screw system in a child with Simpson–Golabi–Behmel syndrome. Case report. Int J Pediatr Otorhinolaryngol 67:1143–1147
Pavelec V, Hamans E, Stuck BA (2011) A study of the new generation of the advance system tongue implants: three- and six-month effects of tongue to mandible tethering for obstructive sleep apnea. Laryngoscope 121:2487–2493
Phillips DE, Rogers JH (1988) Down’s syndrome with lingual tonsil hypertrophy producing sleep apnoea. J Laryngol Otol 102:1054–1055
Propst EJ, Amin R, Talwar N et al (2017) Midline posterior glossectomy and lingual tonsillectomy in obese and nonobese children with down syndrome: Biomarkers for success. Laryngoscope 127(3):757–763. doi:10.1002/lary.26104
Prosser JD, Shott SR, Rodriguez O, Simakajornboon N, Meinzen-Derr J, Ishman SL (2017) Polysomnographic outcomes following lingual tonsillectomy for persistent obstructive sleep apnea in down syndrome. Laryngoscope 127(2):520–524. doi:10.1002/lary.26202
Resnick CM, Dentino K, Katz E, Mulliken JB, Padwa BL (2016) Effectiveness of tongue-lip adhesion for obstructive sleep apnea in infants with robin sequence measured by polysomnography. Cleft Palate Craniofac J 53(5):584–588. doi:10.1597/15-058
Robinson S, Ettema SL, Brusky L, Woodson BT (2006) Lingual tonsillectomy using bipolar radiofrequency plasma excision. Otolaryngol Head Neck Surg 134:328–330
Rombaux P, Hamoir M, Bertrand B, Aubert G, Liistro G, Rodenstein D (2003) Postoperative pain and side effects after uvulopalatopharyngoplasty, laser-assisted uvulopalatoplasty, and radiofrequency tissue volume reduction in primary snoring. Laryngoscope 113:2169–2173
Sedaghat AR, Anderson IC, McGinley BM, Rossberg MI, Redett RJ, Ishman SL (2012) Characterization of obstructive sleep apnea before and after tongue-lip adhesion in children with micrognathia. Cleft Palate-Craniofac J 49:21–26
Sedaghat AR, Flax-Goldenberg RB, Gayler BW, Capone GT, Ishman SL (2012) A case-control comparison of lingual tonsillar size in children with and without Down syndrome. Laryngoscope 122:1165–1169
Sher AE, Flexon PB, Hillman D et al (2001) Temperature-controlled radiofrequency tissue volume reduction in the human soft palate. Otolaryngol Head Neck Surg 125:312–318
Siddique S, Haupert M, Rozelle A (2000) Subperiosteal release of the floor of the mouth musculature in two cases of Pierre Robin sequence. Ear Nose Throat J 79:816–819
Stricker PA, Rizzi MD, Schwartz AJ (2010) Lingual tonsil. Anesthesiology 112:746
Tan HL, Kheirandish-Gozal L, Abel F, Gozal D (2016) Craniofacial syndromes and sleep-related breathing disorders. Sleep Med Rev 27:74–88
Thottam PJ, Govil N, Duvvuri U, Mehta D (2015) Transoral robotic surgery for sleep apnea in children: Is it effective? Int J Pediatr Otorhinolaryngol 79:2234–2237
Wootten CT, Chinnadurai S, Goudy SL (2014) Beyond adenotonsillectomy: outcomes of sleep endoscopy-directed treatments in pediatric obstructive sleep apnea. Int J Pediatr Otorhinolaryngol 78:1158–1162
Wootten CT, Shott SR (2010) Evolving therapies to treat retroglossal and base-of-tongue obstruction in pediatric obstructive sleep apnea. Arch Otolaryngol Head Neck Surg 136:983–987
Wouters B, van Overbeek JJ, Buiter CT, Hoeksema PE (1989) Laser surgery in lingual tonsil hyperplasia. Clin Otolaryngol Allied Sci 14:291–296
Yoskovitch A, Samaha M, Sweet R (2000) Suction cautery use in lingual tonsillectomy. J Otolaryngol 29:117–118
Montevecchi F, Bellini C, Meccariello G et al (2017) Transoral robotic-assisted tongue base resection in pediatric obstructive sleep apnea syndrome: case presentation, clinical and technical consideration. Eur Arch Oto-rhino-laryngol 274(2):1161–1166. doi:10.1007/s00405-016-4269-x
Camacho M, Capasso R, Schendel S (2014) Airway changes in obstructive sleep apnoea patients associated with a supine versus an upright position examined using cone beam computed tomography. J Laryngol Otol 128:824–830
Friedman NR, Prager JD, Ruiz AG, Kezirian EJ (2016) A pediatric grading scale for lingual tonsil hypertrophy. Otolaryngol Head Neck Surg 154:171–174
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no competing interest.
Funding
There was no funding for this review.
Ethical approval
The Tripler Army Medical Center Investigational Review Board provided approval for this meta-analysis.
Human rights
This article does not contain any studies with human participants performed by any of the authors.
Additional information
The views expressed in this manuscript are those of the authors and do not reflect the official policy or position of the Department of the Army, Department of Defense, or the US Government.
Rights and permissions
About this article
Cite this article
Camacho, M., Noller, M.W., Zaghi, S. et al. Tongue surgeries for pediatric obstructive sleep apnea: a systematic review and meta-analysis. Eur Arch Otorhinolaryngol 274, 2981–2990 (2017). https://doi.org/10.1007/s00405-017-4545-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-017-4545-4