Abstract
Purpose
We aim to compare the perinatal outcomes of two consecutive management strategies for fetal growth restriction (FGR), with or without the inclusion of additional Doppler parameters.
Methods
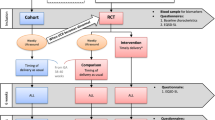
A quasi-experimental before/after study was conducted in which we compared a composite perinatal outcome, prematurity rate, and neonatal complications between two management strategies in small fetuses. In the strategy 1 (S1), the management was based on fetal biometry and umbilical artery Doppler. The second strategy (S2) added the assessment of uterine and middle cerebral artery Doppler. We also compared outcomes between strategies according to early (≤ 32 weeks) and late (> 32 weeks) diagnosis subgroups.
Results
We included 396 patients, 163 in S1 and 233 in S2. There were no significant differences in the perinatal composite outcome (p 0.98), prematurity (p 0.19), or in the subgroup analysis. We found a significant reduction in respiratory distress syndrome (RDS) rate with S2 both globally (OR 0.50, p 0.02), and in the early diagnosis subgroup (OR 0.45, p 0.01). In addition, we observed a significant reduction in the incidence of sepsis with S2 both globally (OR 0.30, p 0.04) and in the early diagnosis subgroup (OR 0.25, p 0.02). We did not observe significant differences in necrotizing enterocolitis (p 0.41) and intraventricular hemorrhage (p 1.00).
Conclusion
The expanded strategy for the management of FGR did not show significant differences in the primary composite outcome or prematurity. However, it was associated with a lower incidence of RDS and neonatal sepsis.



Similar content being viewed by others
References
American college of obstetricians and gynecologists (2013) Practice bulletin No. 134: fetal growth restriction. Obstet Gynecol 1122–1133. https://doi.org/10.1097/01.aog.0000429658.85846.f9
McCowan LM, Figueras F, Anderson NH (2018) Evidence-based national guidelines for the management of suspected fetal growth restriction: comparison, consensus, and controversy. Am J Obstet Gynecol. https://doi.org/10.1016/j.ajog.2017.12.004
Gordijn SJ, Beune IM, Thilaganathan B, Papageorghiou A, Baschat AA, Baker PN et al (2016) Consensus definition of fetal growth restriction: a Delphi procedure. Ultrasound Obstet Gynecol 48:333–339. https://doi.org/10.1002/uog.15884
Lees CC, Stampalija T, Baschat A, da Silva CF, Ferrazzi E, Figueras F et al (2020) ISUOG practice guidelines: diagnosis and management of small-for-gestational-age fetus and fetal growth restriction. Ultrasound Obstet Gynecol 56:298–312. https://doi.org/10.1002/uog.22134
Salam RA, Das JK, Bhutta ZA (2014) Impact of intrauterine growth restriction on long-term health. Curr Opin Clin Nutr Metab Care 17:249–254. https://doi.org/10.1097/MCO.0000000000000051
Kopec G, Shekhawat PS, Mhanna MJ (2017) Prevalence of diabetes and obesity in association with prematurity and growth restriction. Diabetes Metab Syndr Obes 10:285–295. https://doi.org/10.2147/DMSO.S115890
Ross MG, Beall MH (2008) Adult Sequelae of Intrauterine Growth Restriction. Semin Perinatol. https://doi.org/10.1053/j.semperi.2007.11.005
Hawkes N (2018) Trial of Viagra for fetal growth restriction is halted after baby deaths. BMJ. https://doi.org/10.1136/bmj.k3247
Villanueva-García D, Mota-Rojas D, Hernández-González R, Sánchez-Aparicio P, Alonso-Spilsbury M, Trujillo-Ortega ME et al (2007) A systematic review of experimental and clinical studies of sildenafil citrate for intrauterine growth restriction and pre-term labour. J Obstet Gynaecol. https://doi.org/10.1080/01443610701194978
Sharp A, Cornforth C, Jackson R, Harrold J, Turner MA, Kenny LC et al (2018) Maternal sildenafil for severe fetal growth restriction (STRIDER): a multicentre, randomised, placebo-controlled, double-blind trial. Lancet Child Adolesc Health 2:93–102. https://doi.org/10.1016/S2352-4642(17)30173-6
Spencer R, Ambler G, Brodszki J, Diemert A, Figueras F, EVERREST Consortium et al (2017) EVERREST prospective study: a 6-year prospective study to define the clinical and biological characteristics of pregnancies affected by severe early onset fetal growth restriction. BMC Pregnancy Childbirth. https://doi.org/10.1186/s12884-017-1226-7
Say L, Metin Gülmezoglu A, Justus HG (2003) Maternal oxygen administration for suspected impaired fetal growth. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.cd000137
Laurin J, Persson P-H (1987) The effect of bedrest in hospital on fetal outcome in pregnancies complicated by intrauterine growth retardation. Acta Obstet Gynecol Scand. https://doi.org/10.3109/00016348709022043
Say L, Metin Gülmezoglu A, Justus HG (2003) Maternal nutrient supplementation for suspected impaired fetal growth. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.cd000148
Say L, Metin Gülmezoglu A, Justus HG (2001) Betamimetics for suspected impaired fetal growth. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.cd000036
Kingdom JCP, Burrell SJ, Kaufmann P (1997) Pathology and clinical implications of abnormal umbilical artery Doppler waveforms. Ultrasound Obstet Gynecol. https://doi.org/10.1046/j.1469-0705.1997.09040271.x
Karsdorp VHM, van Vugt JMG, van Geijn HP, Kostense PJ, Arduim D, Montenegro N et al (1994) Clinical significance of absent or reversed end diastolic velocity waveforms in umbilical artery. Lancet. https://doi.org/10.1016/s0140-6736(94)90457-x
Society for Maternal-Fetal Medicine Publications Committee, Berkley E, Chauhan SP, Abuhamad A (2012) Doppler assessment of the fetus with intrauterine growth restriction. Am J Obstet Gynecol 206:300–308. https://doi.org/10.1016/j.ajog.2012.01.022
Ott WJ (2000) Intrauterine growth restriction and Doppler ultrasonography. J Ultrasound Med 19(10):661–665. https://doi.org/10.7863/jum.2000.19.10.661
Bamfo JE, Odibo AO (2011) Diagnosis and management of fetal growth restriction. J pregnancy. https://doi.org/10.1155/2011/640715
Figueras F, Gardosi J (2011) Intrauterine growth restriction: new concepts in antenatal surveillance, diagnosis, and management. Am J Obstet Gynecol 204(4):288–300. https://doi.org/10.1016/j.ajog.2010.08.055
Salomon LJ, Alfirevic Z, Da Silva CF, Deter RL, Figueras F, Ghi T et al (2019) ISUOG practice guidelines: ultrasound assessment of fetal biometry and growth. Ultrasound Obstet Gynecol 53:715–723. https://doi.org/10.1002/uog.20272
Melamed N, Baschat A, Yinon Y, Athanasiadis A, Mecacci F, Figueras F et al (2021) FIGO (international Federation of Gynecology and obstetrics) initiative on fetal growth: best practice advice for screening, diagnosis, and management of fetal growth restriction. Int J Gynaecol Obstet 152(Suppl 1):3–57. https://doi.org/10.1002/ijgo.13522
Figueras F, Gratacos E (2014) Stage-based approach to the management of fetal growth restriction. Prenat Diagn 34:655–659. https://doi.org/10.1002/pd.4412
Gómez O, Figueras F, Fernández S, Bennasar M, Martínez JM, Puerto B, Gratacós E (2008) Reference ranges for uterine artery mean pulsatility index at 11–41 weeks of gestation. Ultrasound Obstet Gynecol: Off J Int Soc Ultrasound Obstet Gynecol 32(2):128–132. https://doi.org/10.1002/uog.5315
Ciobanu A, Wright A, Syngelaki A, Wright D, Akolekar R, Nicolaides KH (2019) Fetal Medicine Foundation reference ranges for umbilical artery and middle cerebral artery pulsatility index and cerebroplacental ratio. Ultrasound Obstet Gynecol 53(4):465–472. https://doi.org/10.1002/uog.20157
Savchev S, Figueras F, Sanz-Cortes M, Cruz-Lemini M, Triunfo S, Botet F et al (2014) Evaluation of an optimal gestational age cut-off for the definition of early- and late-onset fetal growth restriction. Fetal Diagn Ther 36:99–105. https://doi.org/10.1159/000355525
Unterscheider J, Daly S, Geary MP, Kennelly MM, McAuliffe FM, O’Donoghue K et al (2013) Optimizing the definition of intrauterine growth restriction: the multicenter prospective PORTO Study. Am J Obstet Gynecol 208(290):e1-6. https://doi.org/10.1016/j.ajog.2013.02.007
Meler E, Mazarico E, Eixarch E, Gonzalez A, Peguero A, Martinez J et al (2020) A 10-year experience of protocol-based management of fetal growth restriction: perinatal outcomes in late pregnancy cases diagnosed after 32 weeks. Ultrasound Obstet Gynecol. https://doi.org/10.1002/uog.23537
Acknowledgements
The authors would like to thank Diego Hernan Giunta, Cristina Maria Elizondo, Lucas Otaño, Pablo Hernan Brener, Mariana Leda Bucich, and Maria Lourdes Posadas-Martinez for their valuable contribution to this study.
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
Conceptualization: SPD, AE, and CHM; methodology: SPD and AE; acquisition of data: SPD, GD, and MCB. Formal analysis and investigation: SPD, AE, and CHM; writing—original draft preparation: SPD; writing—review and editing: AE and CM.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethics approval
The study protocol was approved by our institutional review board.
Consent for publication
All authors agree on the final manuscript and the order of authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Demirdjian, S.P., Meller, C.H., Berruet, M.C. et al. Perinatal outcomes of two consecutive strategies for the management of fetal growth restriction: a before–after study. Arch Gynecol Obstet 307, 319–326 (2023). https://doi.org/10.1007/s00404-022-06641-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-022-06641-x