Abstract
Purpose
To study the prediction of gestational diabetes mellitus (GDM) in high-risk pregnant women by testing fasting blood glucose, 1-h(1hPG) and 2-h plasma glucose (2hPG) after an oral glucose tolerance test, and glycated hemoglobin (HbA1c) in early pregnancy (6–14 weeks).
Methods
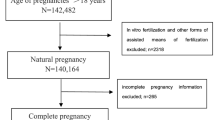
We recruited 1311 pregnant women at high risk for diabetes from the Obstetrics Clinic of Daxing District People’s Hospital between June 2017 and December 2019. The tests performed during the first trimester included fasting blood glucose (FPG), HbA1c, and 75-g oral glucose tolerance test (OGTT) with 1hPG and 2hPG. Seventy-three pregnant women diagnosed with pregestational diabetes mellitus (PGDM) early in pregnancy and 36 who were missed in the second trimester were excluded. A total of 1202 women were followed up until 24–28 weeks for GDM. The receiver operating characteristic (ROC) and area under the ROC curve (AUC) were calculated to determine the predictive values of FPG, 1hPG, 2hPG, and HbA1c for GDM in early pregnancy in high-risk pregnant women.
Results
The AUC for 1hPG for the prediction of GDM in high-risk pregnant women was greater than those for FPG, 2hPG, and HbA1c. All differences were significant.
The AUCs for the predictive values of FPG, 1hPG, 2hPG, and HbA1c in high-risk pregnant women were 0.63, 0.76, 0.71, and 0.67, respectively. The prevalence of PGDM among pregnant women at high risk of diabetes was 5.6%.
Conclusion
First-trimester levels of FPG, 1hPG, 2hPG, and HbA1c in high-risk women are significant predictors of GDM, with 1hPG having the most significant predictive value.


Similar content being viewed by others
References
HAPO Study Cooperative Research Group, Geometer BE, Lowe LP et al (2008) Hyperbole academia and adverse pregnancy outcomes. N Encl J Med 358(19):1991–2002. https://doi.org/10.1056/NEJMoa0707943
Waters TP, Dyer AR, Schoolmates DM et al (2016) Maternal and neonatal morbidity for women who would be added to the diagnosis of GDM using IADPSG criteria: a secondary analysis of the hyperglycemia and adverse pregnancy outcome study. Diabetes Care 39(12):2204–2210. https://doi.org/10.2337/dc16-1194
Brown FM, Gigantism E, James-Todd T (2019) Much to HAPO FUS about: increasing maternal hypoglycemia in pregnancy is associated with worsening childhood glucose metabolism. Diabetes Care 42(3):393–395. https://doi.org/10.2337/dci18-0064
Lowe WL Jr, Lowe LP, Huang A et al (2019) Maternal glucose levels during pregnancy and childhood adipose in the hyperglycemia and adverse pregnancy outcome follow-up study. Dialectology 62(4):598–610. https://doi.org/10.1007/s00125-018-4809-6
Kim SY, England JL, Dharma JA, Orogeny T (2011) Gestational diabetes mellifluous and risk of childhood overweight and obesity in offspring: a systematic review. Exp Diabetes Res 2011:541308. https://doi.org/10.1155/2011/541308
International Association of Diabetes and Pregnancy Study Groups Consensus Panel, Geometer BE, Abbe G et al (2010) International association of diabetes and pregnancy study groups recommendations on the diagnosis and classification of hyperglycemia in pregnancy. Diabetes Care 33(3):676–682. https://doi.org/10.2337/dc09-1848
Wei Y, Yang H et al (2017) Characteristics of pre-gestational diabetes mellitus diagnosed during pregnancy and the effects on pregnancy outcomes. Chinese J of Obstet Gynecol 52(4):227–232. https://doi.org/10.3760/CAM.j.ISS.0529-567x.2017.04.003
Peng X, Wu K et al (2019) Blood glucose screening and its influencing factors in first trimester of pregnant women at high risk of diabetes mellitus. Chinese Gen Pract 22(29):3609–3613. https://doi.org/10.12114/j.ISS.1007-9572.2019.00.230
Coma V, Nonmember J, Aground L, Boule P, Arena E, Brunet C, Mares P, Dinero M, Bani S, Demarcate C, Guided AM (2021) A prospective cohort study of postpartum glucose metabolic disorders in early versus standard diagnosed gestational diabetes mellifluous. Sci Rep 11(1):10430. https://doi.org/10.1038/s41598-021-89679-2
Resurgent ML, van So est EEL, et al (2019) High maternal early-pregnancy blood glucose levels are associated with altered fetal growth and increased risk of adverse birth outcomes. Dialectology 62(10):1880–1890. https://doi.org/10.1007/s00125-019-4957-3
Propranolol C, Tangjitgamol S (2008) Use of oral glucose tolerance test in early pregnancy to predict late-onset gestational diabetes mellifluous in high-risk women. J Obstet Gynaecol Res 34(3):331–336. https://doi.org/10.1111/j.1447-0756.2007.00693
Bitó T, Földesi I et al (2005) Prediction of gestational diabetes mellitus in a high-risk group by insulin measurement in early pregnancy. Diabet Med 22(10):1434–1439. https://doi.org/10.1111/j.1464-5491.2005.01634.x
Amylidi S, Mosimann B et al (2016) First-trimester glycosylated hemoglobin in women at high risk for gestational diabetes. Acta Obstet Gynecol Scand 95(1):93–97. https://doi.org/10.1111/aogs.12784
Yoles I, Sheiner E, Wainstock T (2021) First pregnancy risk factors and future gestational diabetes mellitus. Arch Gynecol Obstet 304:929–934. https://doi.org/10.1007/s00404-021-06024-8
Lin TC, Mu CF et al (2015) Risk factors for gestational diabetes mellitus: ethnic disparities. Aust J Rural Health 23(3):176–180. https://doi.org/10.1111/ajr.12151
Chen P, Wang S, Ji J et al (2015) Risk factors and management of gestational diabetes. Cell Biochem Biophys 71(2):689–694. https://doi.org/10.1007/s12013-014-0248-2
Lee KW, Ching SM, Ramachandran V et al (2018) Prevalence and risk factors of gestational diabetes mellitus in Asia: a systematic review and meta-analysis. BMC Pregnancy Childbirth 18(1):494. https://doi.org/10.1186/s12884-018-2131-4
Durnwald C (2015) Gestational diabetes: Linking epidemiology, excessive gestational weight gain, adverse pregnancy outcomes, and future metabolic syndrome. Semin Perinatol 39:254–258. https://doi.org/10.1053/j.semperi.2015.05.002
Levy A, Wiznitzer A, Holcberg G, Mazor M, Sheiner E (2010) Family history of diabetes mellitus as an independent risk factor for macrosomia and cesarean delivery. J Matern Fetal Neonatal Med 23:148–152. https://doi.org/10.3109/14767050903156650
Agha-Jaffar R, Oliver NS, Kostoula M, Godsland IF, Yu C, Terry J, Johnston D, Gable D, Robinson S (2019) Hyperglycemia recognised in early pregnancy is phenotypically type 2 diabetes mellitus not gestational diabetes mellitus: a case control study. J Matern Fetal Neonatal Med 26:1–7. https://doi.org/10.1080/14767058.2019.1593959
Chaves C, Cunha FM, Martinho M et al (2022) First trimester fasting glucose and glycated haemoglobin cut-offs associated with abnormal glucose homeostasis in the post-partum reclassification in women with hyperglycaemia in pregnancy. Arch Gynecol Obstet 305:475–482. https://doi.org/10.1007/s00404-021-06107-6
Shepherd E, Gomersall JC, Tieu J, Han S, Crowther CA, Middleton P (2017) Combined diet and exercise interventions for preventing gestational diabetes mellitus. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD010443.pub3
Wang S, Ma JM et al (2015) Lifestyle intervention for gestational diabetes mellitus prevention: a cluster⁃randomized controlled study[J]. Chronic Dis Transl Med 1(3):169–174. https://doi.org/10.1016/j.cdtm.2015.09.001
Ming WK, Ding W, Zhang CJP et al (2018) The effect of exercise during pregnancy on gestational diabetes mellitus in normal-weight women: a systematic review and meta-analysis. BMC Pregnancy Childbirth 18(1):440. https://doi.org/10.1186/s12884-018-2068-7
Zhong C, Li X, Chen R et al (2017) Greater early and mid⁃pregnancy gestational weight gain are associated with increased risk of gestational diabetes mellitus: a prospective cohort study[J]. Clin Nutr ESPEN. https://doi.org/10.1016/j.clnesp.2017.08.013
Abdul-Ghani MA, Williams K, DeFronzo RA, Stern M (2007) What is the best predictor of future type 2 diabetes? Diabetes Care 30(6):1544–1548. https://doi.org/10.2337/dc06-1331
Kansu-Celik H, Ozgu-Erdinc AS, Kisa B, Findik RB, Yilmaz C, Tasci Y (2019) Prediction of gestational diabetes mellitus in the first trimester comparison of maternal fetuin-A, N terminal proatrial natriuretic peptide high sensitivity C-reactive protein and fasting glucose levels. Arch Endocrinol Metab 63(2):121–127. https://doi.org/10.20945/2359-3997000000126
Ozgu-Erdinc AS, Yilmaz S, Yeral MI, Seckin KD, Erkaya S, Danisman AN (2015) Prediction of gestational diabetes mellitus in the first trimester: comparison of C-reactive protein, fasting plasma glucose, insulin and insulin sensitivity indices. J Matern Fetal Neonatal Med 28(16):1957–1962. https://doi.org/10.3109/14767058.2014.973397
Hao M, Lin L (2017) Fasting plasma glucose and body mass index during the first trimester of pregnancy as predictors of gestational diabetes mellitus in a Chinese population. Endocr J 64(5):561–569. https://doi.org/10.1507/endocrj.EJ16-0359
Riskin-Mashiah S, Damti A et al (2010) First trimester fasting hyperglycemia as a predictor for the development of gestational diabetes mellitus. Eur J Obstet Gynecol Reprod Biol 152(2):163–167. https://doi.org/10.1016/j.ejogrb.2010.05.036
Agarwal MM, Dhatt GS (2007) Fasting plasma glucose as a screening test for gestational diabetes mellitus. Arch Gynecol Obstet 275(2):81–87. https://doi.org/10.1007/s00404-006-0245-9
Li M, Lan J-R, Liang J-L, Xiong X-L (2020) Diagnostic accuracy of fasting plasma glucose as a screening test for gestational diabetes mellitus a systematic review and meta analysis. Eur Rev Med Pharmacol Sci Actions 24(21):11172–11186. https://doi.org/10.26355/eurrev_202011_23605
Li P, Lin S et al (2019) First-trimester fasting plasma glucose as a predictor of gestational diabetes mellitus and the association with adverse pregnancy outcomes. Pak J Med Sci 35(1):95–100. https://doi.org/10.12669/pjms.35.1.216
Khalafallah A, Phuah E, Al-Barazan AM et al (2016) Glycosylated haemoglobin for screening and diagnosis of gestational diabetes mellitus. BMJ Open 6(4):e011059. https://doi.org/10.1136/bmjopen-2016-011059
Fei X, Zhu Y et al (2018) The clinical significance of fasting plasma glucose body mass index glycosylated hemoglobin and blood fat of early pregnancy (8–14 Weeks) in predicting gestational diabetes mellitus. Chinese J Labor Diagn 22(11):1931–1934. https://doi.org/10.3969/j.issn.1007-4287.2018.11.019
Jiang H, Hu Z et al (2020) The clinical effects of glycated hemoglobin fasting blood glucose and serum C peptide combined screening for gestational diabetes screening and its clinical significance. Chinese J Postgraduates Med 43(4):375–378. https://doi.org/10.3760/cma.j.cn115455-20191108-00897
Funding
This work was funded by The Capital Health Development Scientific Research Project (Grant no. 2018-3-7121); Promotion and application of early diabetes screening in high-risk pregnant women suitable for primary hospitals (Grant no. BHTPP202023).
Author information
Authors and Affiliations
Contributions
Professor MX carried out the research design and article revision. PX was responsible for the specific implementation of the experiment, data collection, statistical analysis and article writing. LM, GJ, and WY participated in the writing process. The data is interpreted by all authors who participated in the writing and revision of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Peng, X., Liu, M., Gang, J. et al. Use of oral glucose tolerance testing and HbA1c at 6–14 gestational weeks to predict gestational diabetes mellitus in high-risk women. Arch Gynecol Obstet 307, 1451–1457 (2023). https://doi.org/10.1007/s00404-022-06637-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-022-06637-7