Abstract
Purpose
This study aimed to estimate the incidence of fatal amniotic fluid embolism, describe its risk factors, and analyze perinatal outcomes.
Methods
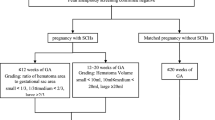
Maternity cases and newborn records of amniotic fluid embolism were collected from the Zhejiang Maternal Surveillance System from October 2006 to October 2019. This study strictly limited the diagnostic criteria for AFE and excluded suspicious cases in order to minimize false-positive AFE cases. The risk factors of fatal amniotic fluid embolism and the relationship between perinatal prognosis and AFE were investigated using logistic regression analysis, estimating the adjusted odds ratios (aORs) and 95% confidence intervals (CIs).
Results
149 cases of amniotic fluid embolism were registered, of which 80 cases were fatal. The estimated fatal AFE incidence was 0.99 per 100,000. The occurrence of fatal AFE was significantly correlated with spontaneous vaginal delivery (aOR 12.3, 95% CI 3.3–39.2) and cardiac arrest (aOR 64.8, 95% CI 14.6–287.8). The average diagnosis time of fatal AFE is 85.51 min, and the peak period of female death is 1–12 h after the onset of the disease, accounting for 60% (48/80) of cases. Fatal amniotic embolism is a cause of intrauterine fetal death and fetal death during delivery (aOR 11.957, 95% CI 1.457–96.919; aOR 13.152, 95% CI 1.636–105.723). Of the 149 confirmed AFE cases, 11 cases of stillbirth occurred, 12 cases were stillborn, and 7 cases of neonatal death were reported. The perinatal mortality rate was 202 per 1000.
Conclusions
Early detection, diagnosis, and treatment of amniotic fluid embolism are essential to avoiding fatal AFE. Clinicians should fully evaluate the pros and cons of choosing the delivery method for pregnant women. When cardiac arrest occurs in women with amniotic fluid embolism, obstetricians should be particularly careful and provide timely and effective treatment to minimize the fatality rate. The outcome of AFE is not only related to maternal survival but also plays a decisive role in the prognosis of the infant over the perinatal period.


Similar content being viewed by others
References
Wakasa T, Ishibashi-Ueda H, Takeuchi M (2021) Maternal death analysis based on data from the nationwide registration system in Japan (2010–2018). Pathol Int 71:223–231. https://doi.org/10.1111/pin.13076
Bonnet MP, Zlotnik D, Saucedo M, Chassard D, Bouvier-Colle MH, Deneux-Tharaux C (2018) Maternal death due to amniotic fluid embolism: a national study in France. Anesth Analg 126:175–182. https://doi.org/10.1213/ANE.0000000000002511
Kanayama N, Inori J, Ishibashi-Ueda H, Takeuchi M, Nakayama M, Kimura S, Matsuda Y, Yoshimatsu J, Ikeda T (2011) Maternal death analysis from the Japanese autopsy registry for recent 16 years: significance of amniotic fluid embolism. J Obstet Gynaecol Res 37:58–63. https://doi.org/10.1111/j.1447-0756.2010.01319.x
Steiner PE, Lushbaugh CC, Frank HA (1949) Fatal obstetric shock from pulmonary emboli of amniotic fluid. Am J Obstet Gynecol 58:802–805. https://doi.org/10.1016/s0002-9378(16)39241-9
Clark SL (2014) Amniotic fluid embolism. Obstet Gynecol 123:337–348. https://doi.org/10.1097/AOG.0000000000000107
Hiroshi KM (2015) Amniotic fluid embolism: anaphylactic reactions with idiosyncratic adverse response. Obstet Gynecol Survey 70:511–517
Kanayama N, Tamura N (2014) Amniotic fluid embolism: pathophysiology and new strategies for management. J Obstet Gynaecol Res 40:1507–1517. https://doi.org/10.1111/jog.12428
Kramer MS, Rouleau J, Liu S, Bartholomew S, Joseph KS (2012) Amniotic fluid embolism: incidence, risk factors, and impact on perinatal outcome. BJOG 119:874–879. https://doi.org/10.1111/j.1471-0528.2012.03323.x
Tamura N, Farhana M, Oda T, Itoh H, Kanayama N (2017) Amniotic fluid embolism: pathophysiology from the perspective of pathology. J Obstet Gynaecol Res 43:627–632. https://doi.org/10.1111/jog.13284
Conde-Agudelo A, Romero R (2009) Amniotic fluid embolism: an evidence-based review. Am J Obstet Gynecol 201(445):e441–e413. https://doi.org/10.1016/j.ajog.2009.04.052
Shen F, Wang L, Yang W, Chen Y (2016) From appearance to essence: 10 years review of atypical amniotic fluid embolism. Arch Gynecol Obstet 293:329–334. https://doi.org/10.1007/s00404-015-3785-z
Kramer MS, Abenhaim H, Dahhou M, Rouleau J, Berg C (2013) Incidence, risk factors, and consequences of amniotic fluid embolism. Paediatr Perinat Epidemiol 27:436–441. https://doi.org/10.1111/ppe.12066
Schröder L, Hellmund A, Gembruch U, Merz WM (2020) Amniotic fluid embolism-associated coagulopathy: a single-center observational study. Arch Gynecol Obstet 301:923–929. https://doi.org/10.1007/s00404-020-05466-w
Steven L, Clark M (2010) Amniotic fluid embolism. Clin Obstet Gynecol 53:322–328
Funding
The authors have not disclosed any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
We declare that we have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhu, C., Xu, D. & Luo, Q. Fatal amniotic fluid embolism: incidence, risk factors and influence on perinatal outcome. Arch Gynecol Obstet 307, 1187–1194 (2023). https://doi.org/10.1007/s00404-022-06535-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-022-06535-y