Abstract
Purpose
This study has two aims: determine the prevalence of CIN3 + in patients with discordant cotesting, defined as negative cytology and positive human papillomavirus (HPV) testing, and identify factors (including HPV strain) associated with CIN3 + , defined as cervical intraepithelial neoplasia (CIN) 3 or cancer within this population.
Methods
We conducted a retrospective chart review of women age 30–65 with intact cervices who had discordant cotesting results between January 1, 2013 and September 1, 2018, at an academic medical center. We used the t test for continuous variables and the Chi-square test for categorical variables to compare women with and without CIN3 + . To identify factors associated with CIN3 + , we performed univariate and multivariate logistic regression.
Results
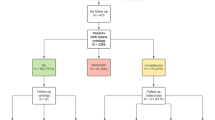
The primary outcome was the prevalence of CIN3 + based on pathologic diagnosis following biopsy or excisional procedure. Among 375 patients with discordant co-testing, the mean age was 43.8 years, 58.4% were parous, and 84.8% were white. Overall, 43/375 (12.0%) had CIN3 + and 7/375 (1.9%) had AIS. On logistic regression, only parity ≥ 1 (p = 0.04, adjusted OR = 2.23, CI = 1.06–4.68) was significantly associated with CIN3 + . HPV-18 was less likely to be associated with CIN3 + (p = 0.02, adjusted OR 0.08, CI 0.01–0.65) but was present in 43% of AIS cases. HPV16 and other HR-HPV strains were highly associated with CIN3 + .
Conclusion
Women with discordant cotesting are at significant risk for CIN3 + . We recommend that biopsy be performed at the time of indicated colposcopy for all patients with discordant cotesting to assess for high-grade dysplasia.

Similar content being viewed by others
Data availability
Data can be made available upon request.
Code availability
Not applicable.
Abbreviations
- AIS:
-
Adenocarcinoma in situ
- ASCCP:
-
American Society for Colposcopy and Cervical Pathology
- ASCUS:
-
Atypical squamous cells of undetermined significance
- ASC:
-
Atypical squamous cells
- BMI:
-
Body mass index
- CIN:
-
Cervical intraepithelial neoplasia
- CKC:
-
Cold knife conization
- CPT:
-
Current Procedural Terminology
- HPV:
-
Human papillomavirus
- HR-HPV:
-
High-risk Human papillomavirus (HPV-16/18)
- HSIL:
-
High-grade squamous intraepithelial lesion
- LEEP:
-
Loop electrocautery excisional procedure
- LSIL:
-
Low-grade squamous intraepithelial lesion
- NILM:
-
Negative for intraepithelial lesion or malignancy
- SCC:
-
Squamous cell carcinoma
References
American Society for Colposcopy and Cervical Pathology. Updated consensus guidelines for managing abnormal cervical cancer screening tests and cancer precursors. https://www.asccp.org/Assets/51b17a58-7af9-4667-879a-3ff48472d6dc/635912165077730000/asccp-management-guidelines-august-2014-pdf. Reprinted August 2014. (Accessed 12 Dec 2019).
Choi JW, Kim Y, Lee JH, Kim YS (2016) The clinical performance of primary HPV screening, primary HPV screening plus cytology cotesting, and cytology alone at a tertiary care hospital. Cancer Cytopathol 124(2):144–152
Schiffman M, Kinney WK, Cheung LC et al (2018) Relative performance of HPV and cytology components of cotesting in cervical screening. Int Natl Cancer Inst 110(5):501–508
Bogani G, Taverna F, Lombardo C et al (2017) Retrospective study of the influence of HPV persistence on outcomes among women with high-risk HPV infections and negative cytology. Int J Gynaecol Obstet 138(1):62–68
Polman NJ, Veldhuijzen NJ, Heideman DAM, Snijders PJF, Meijer CJLM, Berkhof J (2019) Management of HPV-positive women in cervical screening using results from two consecutive screening rounds. Int J Cancer 144(9):2339–2346
Massad LS, Collins YC, Meyer PM (2001) Biopsy correlates of abnormal cervical cytology classified using the Bethesda system. Gynecol Oncol 82(3):516–522
Stoler MH, Schiffman M (2001) Interobserver reproducibility of cervical cytologic and histologic interpretations. JAMA 285(11):1500–1505
Castle PE, Aslam S, Behrens C (2016) Cervical precancer and cancer risk by human papillomavirus status and cytologic interpretation: Implications for risk-based management. Cancer Epidemiol Biomarkers Prev 25(12):1595–1599
Vallapapan A, Chandeying N, Srijaipracharoen S, Uthagethaworn K (2019) The role of random cervical biopsies in addition to colposcopy-directed biopsies in detection of CIN2. J Obstet Gynaecol 39(2):184–189
Huh WK, Sideri M, Stoler M, Zhang G, Feldman R, Behrens CM (2014) Relevance of random biopsy at the transformation zone when colposcopy is negative. Obstet Gynecol 124(4):670–678
Tainio K, Athanasiou A, Tikkinen KAO, Aaltonen R, Cardenas J, Glazer-Livson S, Jakobsson M, Joronen K, Kiviharju M, Louvanto K, Oksjoki S, Tahtinen R, Virtanen S, Nieminen MK, Kalliala I (2018) Clinical course of untreated cervical intraepithelial neoplasia grade 2 under active surveillance: systematic review and meta-analyiss. BMI 360-499.
Zhang J, Lu C-X (2019) Spontaneous regression of cervical intraepithelial neoplasia 2: a meta-analysis. Gynecol Obstet Invest 84(6):562–567
Cleveland AA, Gargano JW, Park IU, Griffin MR, Niccolai LM, Powell M, Bennett NM, Saadeh K, Pemmaraju M, Higgins K, Ehlers S, Scahill M, Johnson Jones ML, Querec T, Markowitz LE, Unger ER (2020) Cervical adenocarcinoma in situ: human papillomavirus types and incidence trends in five states, 2008–2015. Int J Cancer 146(3):810–818
Teoh D, Musa F, Salani R, Huh W, Jimenez E (2020) Diagnosis and management of adenocarcinoma in situ. Obstet Gynecol 135(4):869–878
Perkins RB, Guido RS, Castle PE, Chelmow D, Einstein MH, Garcia F, Huh WK, Kim JJ, Moscicki AB, Nayar R, Saraiya M, Sawaya G, Wentzensen N, Schiffman M (2020) 2019 ASCCP risk-based management consensus guidelines for abnormal cervical cancer screening tests and cancer precursors. J Low Genit Tract Dis 24:102–131
Wentzensen N, Walker JL, Gold MA, Smith KM, Zuna RE, Mathews C, Dunn ST, Zhang R, Moxley K, Bishop E, Tenney M, Nugent E, Graubard BI, Wacholder S, Schiffman M (2015) Multiple biopsies and detection of cervical cancer precursors at colposcopy. J Clin Oncol 33(1):83–89
Acknowledgements
The project described was supported by the Clinical and Translational Science Award (CTSA) program, through the NIH National Center for Advancing Translational Sciences (NCATS), grant UL1TR002373. The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH.
Funding
There was no external funding source for this study.
Author information
Authors and Affiliations
Contributions
SMP: Protocol development, data collection, data analysis, manuscript writing. AJJ: Protocol development, data collection, manuscript writing
Corresponding author
Ethics declarations
Conflict of interest
This study was approved by the University of Wisconsin with IRB number 2018–1135. There was no funding source for this project. Neither author has any conflicts of interest.
Informed consent
Informed consent was exempted by the IRB and therefore was not obtained.
IRB status
Approved by University of Wisconsin with IRB number 2018–1135.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Peace, S.M., Jennings, A.J. Prevalence of high-grade dysplasia in cytology-negative, HPV-positive cervical cancer screening. Arch Gynecol Obstet 305, 87–93 (2022). https://doi.org/10.1007/s00404-021-06208-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-021-06208-2