Abstract
Purpose
Aim of the study was to investigate the topical application of a eutectic mixture of lidocaine/prilocaine (EMLA®) cream after caesarean section (CS) and its effect on postoperative pain, time to mobilisation, and time to discharge.
Materials and methods
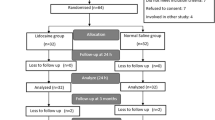
A total of 189 pregnant women were enrolled; full data sets were available for 139 of them, who were prospectively randomised to receive either placebo (control group) or EMLA® cream (study group) on the CS lesion directly as well as 24 h after surgery. Postoperative pain was assessed 24 and 48 h after surgery using the short form of the McGill Pain Questionnaire (SF-MPQ). Additional analgesic pain medication on demand was assessed in both groups.
Results
A total of 62 women were allocated randomly to the study and 77 patients to the control group before primary CS. There were no statistically significant differences regarding demographic and surgical parameters comparing both collectives. In addition, the postoperative total pain scores after 24 h [McGill total: 38.5 (0–102) vs. 50 (0–120) p = 0.0889] as well as after 48 h [24 (0–79) vs. 30.5 (0–92); p = 0.1455] showed no significant differences. Furthermore, time to mobilisation (hours) [9.68 (2.18–51.38) vs. 9.47 (4.18–41.77); p = 0.5919] and time to discharge (hours) [98.6 (54.08–170.15) vs. 98.2 (43.45–195.87); p = 0.5331] were comparable.
Conclusion
The postoperative application of EMLA® cream after CS did not reduce postoperative pain or time to mobilisation or discharge, so that its use in this context has to be seen critically.
Similar content being viewed by others
References
Wallin G, Fall O (1999) Modified Joel-Cohen technique for caesarean delivery. Br J Obstet Gynaecol 106(3):221–226
Hofmeyr GJ, Mathai M, Shah AN, Novikova N (2008) Techniques for caesarean section. Cochrane Pregnancy and Childbirth Group. The Cochrane database of systematic reviews. doi:10.1002/14651858.CD004662.pub2
Rosenberg J, Kehlet H (1999) Does effective postoperative pain management influence surgical morbidity? Eur Surg Res 31:133–137
Beake S, Bick D, Narracott C, Chang YS (2016) Interventions for women who have a caesarean birth to increase uptake and duration of breastfeeding: a systematic review. Matern Child Nutr. doi:10.1111/mcn.12390
Mkontwana N, Novikova N (2015) Oral analgesia for relieving post-caesarean pain. The Cochrane database of systematic reviews, CD010450
Stamer UM, Wiese R, Stuber F, Wulf H, Meuser T (2005) Change in anaesthetic practice for caesarean section in Germany. Acta Anaesthesiol Scand 49:170–176
Zeng AM, Nami NF, Wu CL, Murphy JD (2016) The analgesic efficacy of nonsteroidal anti-inflammatory agents (NSAIDs) in patients undergoing cesarean deliveries: a meta-analysis. Reg Anesth Pain Med 41:763–772
Adesope O, Ituk U, Habib AS (2016) Local anaesthetic wound infiltration for postcaesarean section analgesia: a systematic review and meta-analysis. Eur J Anaesthesiol 33:731–742
Fusco P, Scimia P, Paladini G, Fiorenzi M, Petrucci E, Pozone T, Vacca F, Behr A, Micaglio M, Danelli G et al (2015) Transversus abdominis plane block for analgesia after cesarean delivery. Syst Rev Minerva Anestesiol 81:195–204
Berlit S, Tuschy B, Brade J, Huttner F, Hornemann A, Sutterlin M (2015) Topical anaesthetic patches for postoperative wound pain in laparoscopic gynaecological surgery: a prospective, blinded and randomised trial. Arch Gynecol Obstet 291:585–590
Vollandt R, Horn M (1997) Evaluation of Noether’s method of sample size determination for the Wilcoxon-Mann–Whitney test. Biom J 39(7):823–829
Ismail S, Shahzad K, Shafiq F (2012) Observational study to assess the effectiveness of postoperative pain management of patients undergoing elective cesarean section. J Anaesthesiol Clin Pharmacol 28:36–40
Kainu JP, Sarvela J, Tiippana E, Halmesmaki E, Korttila KT (2010) Persistent pain after caesarean section and vaginal birth: a cohort study. Int J Obstet Anesthesia 19:4–9
Shang AB, Gan TJ (2003) Optimising postoperative pain management in the ambulatory patient. Drugs 63:855–867
McDonnell NJ, Keating ML, Muchatuta NA, Pavy TJ, Paech MJ (2009) Analgesia after caesarean delivery. Anesth Intensive Care 37:539–551
Mitra J, Reihanak T, Bita A, Zahra G (2016) A randomized controlled trial comparing the effect of intravenous, subcutaneous, and intranasal fentanyl for pain management in patients undergoing cesarean section. Adv Biomed Res 2016(5):198
Bamigboye AA, Hofmeyr GJ (2009) Local anaesthetic wound infiltration and abdominal nerves block during caesarean section for postoperative pain relief. The Cochrane database of systematic reviews, CD006954
Li Y, Li J, Yang M, Yuan H (2015) Local anaesthetic wound infiltration used for caesarean section pain relief: a meta-analysis. Int J Clin Exp Med 8(6):10213–10224
Author information
Authors and Affiliations
Contributions
TG-S: project development and manuscript writing. MK: data collection and management; BT: manuscript writing/editing; CW: statistical analysis; MS: funding the project and manuscript editing. SB: project development, supervision, and manuscript writing
Corresponding author
Ethics declarations
Funding
This study was funded by the Department of Obstetrics and Gynaecology, University Medical Centre Mannheim, Heidelberg University.
Conflict of interest
The authors declare that they do not have any conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Grosse-Steffen, T., Krämer, M., Tuschy, B. et al. Topic anaesthesia with a eutectic mixture of lidocaine/prilocaine cream after elective caesarean section: a randomised, placebo-controlled trial. Arch Gynecol Obstet 296, 771–776 (2017). https://doi.org/10.1007/s00404-017-4486-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-017-4486-6