Abstract
Introduction
There are no widely accepted algorithms for determining optimal treatment for periprosthetic joint infection (PJI). Our study aimed to confirm the validity of a previously published scoring system in a larger number of patients to support a rational surgical treatment strategy for periprosthetic hip infection.
Materials and methods
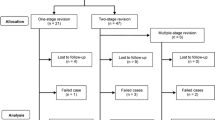
Between February 2001 and December 2020, we performed 155 consecutive revision total hip arthroplasties (THAs) for PJI, with mean follow-up of 6 years. One-stage revision THA was performed in 56 hips and two-stage revision THA in 99 hips. Prosthesis survival from recurrent infection was determined by Kaplan-Meier analysis, using implant removal as the endpoint. The pre-operative scoring system (full score of 12 points), including 6 essential elements, was retrospectively evaluated.
Results
The 10-year survival rates were 98% for one-stage (95% confidence interval [CI], 94–100) and 87% (95% CI, 79–96) for two-stage revision THA. Multivariate Cox regression analysis provided a total preoperative score as an independent risk factor for implant removal (hazard ratio, 0.17; 95% CI, 0.06–0.49; p < 0.001). The sensitivity and specificity at the cut-off of 4 points on the scoring system were 80% and 91%, respectively. The average score for one-stage revision THA in successful and failed cases were 8.9 and 6.0, and for two-stage revision THA were 6.5 and 3.9, respectively. We found significant differences between successful cases in one- and two-stage revision THA (p < 0.05).
Conclusions
The preoperative scoring system was useful for managing PJI. One-stage revision THA is recommended in patients scoring ≥ 9 points, and meticulously performed two-stage revision THA is encouraged for patients scoring ≥ 4 points.





Similar content being viewed by others
Data availability
Data available within the article.
References
Kurtz S, Ong K, Lau E, Mowat F, Halpern M (2007) Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am 89:780–785. https://doi.org/10.2106/JBJS.F.00222
Patel A, Pavlou G, Mújica-Mota RE, Toms AD (2015) The epidemiology of revision total knee and hip arthroplasty in England and Wales: a comparative analysis with projections for the United States. A study using the National Joint Registry dataset. Bone Joint J 97:1076–1081. https://doi.org/10.1302/0301-620X.97B8.35170
Gwam CU, Mistry JB, Mohamed NS, Thomas M, Bigart KC, Mont MA, Delanois RE (2017) Current epidemiology of revision total hip arthroplasty in the United States: National Inpatient Sample 2009 to 2013. J Arthroplasty 32:2088–2092. https://doi.org/10.1016/j.arth.2017.02.046
Illgen RL, Lewallen DG, Yep PJ, Mullen KJ, Bozic KJ (2021) Migration patterns for revision total hip arthroplasty in the United States as reported in the American joint replacement registry. J Arthroplasty 36:1401–1406. https://doi.org/10.1016/j.arth.2020.10.030
National Joint Registry (2020) https://reports.njrcentre.org.uk/hips-revision-procedures-patient-characteristics/H19v1NJR?reportid=AB5D4468-323C-4E54-8737-11C7DAA7B75E&defaults=DC__Reporting_Period__Date_Range=%22MAX%22,J__Filter__Calendar_Year=%22MAX%22,H__Filter__Joint=%22Hip%22
Kurtz SM, Lau EC, Son MS, Chang ET, Zimmerli W, Parvizi J (2018) Are we winning or losing the battle with periprosthetic joint infection: Trends in periprosthetic joint infection and mortality risk for the medicare population. J Arthroplasty 33:3238–3245. https://doi.org/10.1016/j.arth.2018.05.042
Ueda N, Oe K, Nakamura T, Tsuta K, Iida H, Saito T (2019) Sonication of extracted implants improves microbial detection in patients with orthopedic implant-associated infections. J Arthroplasty 34:1189–1196. https://doi.org/10.1016/j.arth.2019.02.020
Buchholz HW, Elson RA, Engelbrecht E, Lodenkämper H, Röttger J, Siegel A (1981) Management of deep infection of total hip replacement. J Bone Joint Surg Br 63:342–353. https://doi.org/10.1302/0301-620X.63B3.7021561
Colyer RA, Capello WN (1994) Surgical treatment of the infected hip implant. Two-stage reimplantation with a one-month interval. Clin Orthop Relat Res 298:75–79
Klouche S, Sariali E, Mamoudy P (2010) Total hip arthroplasty revision due to infection: a cost analysis approach. Orthop Traumatol Surg Res 96:124–132. https://doi.org/10.1016/j.rcot.2010.02.005
Osmon DR, Berbari EF, Berendt AR, Lew D, Zimmerli W, Steckelberg JM, Rao N, Hanssen A, Wilson WR, Infectious Diseases Society of America (2013) Diagnosis and management of prosthetic joint infection: clinical practice guidelines by the Infectious Diseases Society of America. Clin Infect Dis 56:e1–25. https://doi.org/10.1093/cid/cis803
Oe K, Iida H, Ueda N, Nakamura T, Okamoto N, Ueda Y (2015) Pre-operative scoring system to determine the surgical strategy for periprosthetic hip infection. Int Orthop 39:19–25. https://doi.org/10.1007/s00264-014-2493-9
Giulieri SG, Graber P, Ochsner PE, Zimmerli W (2004) Management of infection associated with total hip arthroplasty according to a treatment algorithm. Infection 32:222–228. https://doi.org/10.1007/s15010-004-4020-1
Della Valle C, Parvizi J, Bauer TW, Dicesare PE, Evans RP, Segreti J et al (2010) Diagnosis of periprosthetic joint infections of the hip and knee. J Am Acad Orthop Surg 18:760–770. https://doi.org/10.5435/00124635-201012000-00006
Jiranek WA, Hanssen AD, Greenwald AS (2006) Antibiotic-loaded bone cement for infection prophylaxis in total joint replacement. J Bone Joint Surg Am 88:2487–2500. https://doi.org/10.2106/JBJS.E.01126
Merle d’Aubigné R, Postel M (1954) Functional result of hip arthroplasty with acrylic prosthesis. J Bone Joint Surg Am 36:451–475
Zimmerli W, Trampuz A, Ochsner PE (2004) Prosthetic-joint infections. N Engl J Med 351:1645–1654. https://doi.org/10.1056/NEJMra040181
Del Pozo JL, Patel R (2009) Clinical practice. Infection associated with prosthetic joints. N Engl J Med 361:787–794. https://doi.org/10.1056/NEJMcp0905029
Carlsson AS, Josefsson G, Lindberg L (1978) Revision with gentamicin-impregnated cement for deep infections in total hip arthroplasties. J Bone Joint Surg Am 60:1059–1064
Gehrke T, Zahar A, Kendoff D (2013) One-stage exchange: it all began here. Bone Joint J 95:77–83. https://doi.org/10.1302/0301-620X.95B11.32646
Leonard HA, Liddle AD, Burke O, Murray DW, Pandit H (2014) Single- or two-stage revision for infected total hip arthroplasty? A systematic review of the literature. Clin Orthop Relat Res 472:1036–1042. https://doi.org/10.1007/s11999-013-3294-y
Callaghan JJ, Katz RP, Johnston RC (1999) One-stage revision surgery of the infected hip. A minimum 10-year followup study. Clin Orthop Relat Res 369:139–143. https://doi.org/10.1097/00003086-199912000-00014
Garvin KL, Hanssen AD (1995) Infection after total hip arthroplasty. Past, present, and future. J Bone Joint Surg Am 77:1576–1588. https://doi.org/10.2106/00004623-199510000-00015
Lange J, Troelsen A, Thomsen RW, Søballe K (2012) Chronic infections in hip arthroplasties: comparing risk of reinfection following one-stage and two-stage revision: a systematic review and meta-analysis. Clin Epidemiol 4:57–73. https://doi.org/10.2147/CLEP.S29025
Langlais F (2003) Can we improve the results of revision arthroplasty for infected total hip replacement? J Bone Joint Surg Br 85:637–640
Buchholz HW, Engelbrecht H (1970) Uber die Depotwirkung Einiger Antibiotica Bei Vermischung Mit dem Kunstharz Palacos. Chirurg 41:511–515 [in German]
Zahar A, Klaber I, Gerken AM, Gehrke T, Gebauer M, Lausmann C, Citak M (2019) Ten-year results following one-stage septic hip exchange in the management of periprosthetic joint infection. J Arthroplasty 34:1221–1226. https://doi.org/10.1016/j.arth.2019.02.021
Svensson K, Rolfson O, Kärrholm J, Mohaddes M (2019) Similar risk of Re-revision in patients after one- or two-stage Surgical revision of infected total hip arthroplasty: an analysis of revisions in the Swedish hip Arthroplasty Register 1979–2015. J Clin Med 8:485. https://doi.org/10.3390/jcm8040485
Parvizi J, Gehrke T (2014) Proceedings of the international consensus meeting on periprosthetic joint infection. J Orthop Res 32:S1–172. https://doi.org/10.1002/jor.22528
Sawada M, Oe K, Hirata M, Kawamura H, Ueda N, Nakamura T, Iida H, Saito T (2019) Linezolid versus daptomycin treatment for periprosthetic joint infections: a retrospective cohort study. J Orthop Surg Res 14:334. https://doi.org/10.1186/s13018-019-1375-7
Oe K, Sawada M, Nakamura T, Iida H, Saito T (2021) Daptomycin for the Treatment of Gram-Positive Periprosthetic Hip Infections: Can daptomycin prevent the implant removal? Cureus 2021;13:e15842. https://doi.org/10.7759/cureus.15842
Renz N, Trampuz A, Zimmerli W (2021) Controversy about the role of rifampin in biofilm infections: is it justified? Antibiot (Basel) 10:165. https://doi.org/10.3390/antibiotics10020165
Beldman M, Löwik C, Soriano A, Albiach L, Zijlstra WP, Knobben BAS et al (2021) If, when, and how to use rifampin in acute staphylococcal periprosthetic joint infections, a multicentre observational study. Clin Infect Dis 73:1634–1641. https://doi.org/10.1093/cid/ciab426
Akgün D, Trampuz A, Perka C, Renz N (2017) High failure rates in treatment of streptococcal periprosthetic joint infection: results from a seven-year retrospective cohort study. Bone Joint J 99:653–659. https://doi.org/10.1302/0301-620X.99B5.BJJ-2016-0851.R1
Shabana NS, Seeber G, Soriano A, Jutte PC, Westermann S, Mithoe G (2022) The clinical outcome of early periprosthetic joint infections caused by Staphylococcus epidermidis and managed by surgical debridement in an era of increasing resistance. Antibiot (Basel) 12:40. https://doi.org/10.3390/antibiotics12010040
Brown TS, Petis SM, Osmon DR, Mabry TM, Berry DJ, Hanssen AD, Abdel MP (2018) Periprosthetic joint infection with fungal pathogens. J Arthroplasty 33:2605–2612. https://doi.org/10.1016/j.arth.2018.03.003
Belden K, Cao L, Chen J, Deng T, Fu J, Guan H et al (2019) Hip and knee section, fungal periprosthetic joint infection, diagnosis and treatment: Proceedings of international consensus on orthopedic infections. J Arthroplasty. 2019;34(2S):S387–S391. https://doi.org/10.1016/j.arth.2018.09.023
Acknowledgements
The authors would like to all staff members working to collect the many samples. We also extend thanks to Tomomi Oe for the supervisor.
Funding
This research did not receive any specific grants from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
KO designed the study. YO, TT, FK, and SS collected and performed the analysis of the data. KO wrote the manuscript. HI, TN, and TS supervised the study. All authors gave their final approval of the version to be published.
Corresponding author
Ethics declarations
Ethics approval
This study was approved by the Ethical Committee of the Kansai Medical University (H120167).
Consent to participate
All authors have participated in the research.
Consent to publish
All authors of this paper have read and approved the final version submitted.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Oe, K., Iida, H., Otsuki, Y. et al. Validity of a preoperative scoring system for surgical management of periprosthetic hip infection: one-stage vs. two-stage revision. Arch Orthop Trauma Surg (2024). https://doi.org/10.1007/s00402-024-05279-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00402-024-05279-5